17 First described in 1782 by a Belgian obstetrician, Georges Herbineaux, spondylolisthesis describes a slip or translational movement, either anterior or posterior, of one vertebral body upon another.1 In the adult lumbar spine, this translation can be the result of dysplastic, degenerative, traumatic, pathological, or iatrogenic etiologies.2 Numerous classification systems have been devised to describe both the types and the grades of spondylolisthesis, but the system proposed by Marchetti and Bartolozzi has emerged as the preferred system of the Scoliosis Research Society in its 2005 consensus statement.3 The Marchetti and Bartolozzi classification (Table 17.1) distinguishes between developmental and acquired etiologies leading to spondylolisthesis. When combined with the degree of translational displacement described by Meyerding, it allows for the effective communication of the type and grade of spondylolisthesis, potentially having prognostic and treatment implications.3 Low-grade spondylolisthesis in the adult is most commonly classified as acquired (degenerative and traumatic-stress fractures) by Marchetti and Bartolozzi (Table 17.1). Less commonly, it can present as the developmental (low dysplastic with lysis) subcategory. Adult patients being treated for symptoms associated with low-grade spondylolisthesis present most commonly with back pain, and/or neurological findings of neurogenic claudication or radicular leg pain. The initial management of adult low-grade spondylolisthesis sparks little controversy and includes activity modification, physical therapy, judicious use of nonsteroidal antiinflammatory drugs (NSAIDs), and steroid injections (either selective nerve roots and/or pars interarticularis injections in the case of a pars fracture) and is successful in the majority of patients. The treatment controversy arises in the management of those patients who fail the initial trial of conservative care. A comprehensive review of the English literature on adult isthmic and degenerative spondylolisthesis for therapeutic studies was performed. A search of Medline (1950 to June 2009), Embase, the Cochrane Central Registry of Controlled Trials, and a hand search of bibliographies from studies previously identified were performed to identify prospective randomized, controlled trials (PRCT) (I), prospective cohort studies (PCS) (II), and retrospective case-control studies (RCS) (III) (Table 17.2). The identified studies were then scored and assigned a level of evidence based on the merits of the study and the accepted criteria in the medical literature. Adult degenerative and adult low-grade isthmic spondylolisthesis were evaluated. A search for the terms “adult AND lumbar vertebrae AND spondylolisthesis” returned 1008 results, when combined with the term “treatment outcome” the search narrowed to 228 results. A subsearch of these results for the terms “de-compression” (36), “spinal fusion” (188), “spinal fusion AND decompression” (25), “spinal fusion AND bone screws” (62), and “spinal fusion AND decompression AND bone screws” (2) revealed the respective results. A total of 24 level I PRCTs, 3 level II PCSs, and 15 level III studies (consisting of case-controlled, retrospective cohort, systematic review, and societal summary/consensus statement studies) were evaluated and selected for this review (Table 17.2). Table 17.1 Marchetti-Bartolozzi Classification of Spondylolisthesis
Adult Low-Grade Spondylolisthesis: Surgical Approach, Role of Fusion, Role of Instrumentation
Acquired | Developmental |
|---|---|
Traumatic | High dysplastic |
-Acute fracture | -with lysis |
-Stress fracture | -with elongation |
Postsurgical | Low dysplastic |
-Direct | -with lysis |
-Indirect | -with elongation |
Pathological |
|
-Local |
|
-Systemic |
|
Degenerative |
|
-Primary |
|
-Secondary |
|
Source: Marchetti PG Bartolozzi P. Classification of spondylolisthesis as a guideline for treatment. In: Bridwell KH De Wald R, eds. Textbook of Spinal Surgery. 2nd ed. Philadelphia: Lippincott-Raven; 1997:1211–1254.
Table 17.2 Level of Evidence of Published Studies for the Management of Adult Low-Grade Spondylolisthesis
Level | Number of Studies | Study Type |
|---|---|---|
I | 24 | Prospective, randomized controlled trial (17 studies)4–7,9,17,18,24–36,38 |
II | 3 | |
III | 15 | Case-controlled study (5 studies)12,13,21,40 Retrospective cohort study (5 studies)11,20,23,39 Systematic review of level I–III studies (5 studies)14–16,22,41 Consensus summary statement (1 study)3 |
 Approach to Adult Low-Grade Spondylolisthesis
Approach to Adult Low-Grade Spondylolisthesis
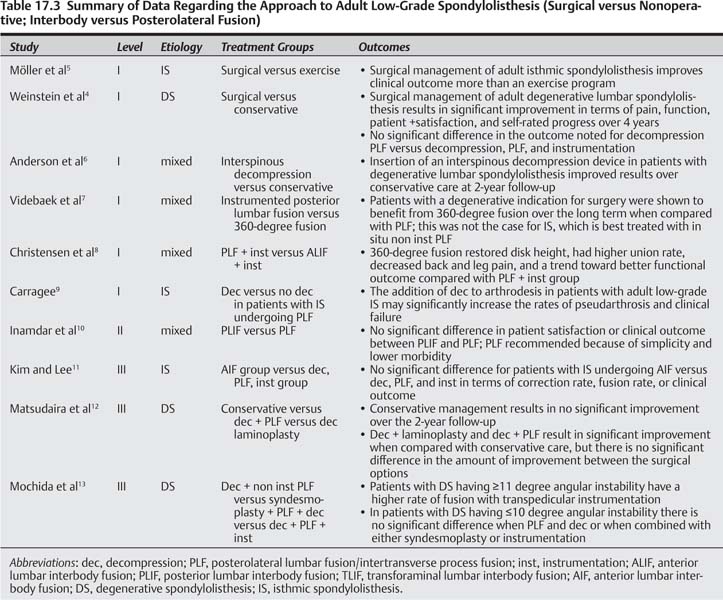
Level I Data (Table 17.3)
There are two level I studies addressing the conservative versus surgical management of adult low-grade spondylolisthesis, one for degenerative4 and one for isthmic.5
Möller’s PRCT compared surgical and conservative management in the treatment of adult isthmic spondylolisthesis.5
The study randomized 111 patients to one of three treatment arms: group I, posterior lumbar fusion (PLF); group II, posterior lumbar fusion with instrumentation; and group III, exercise program. Two-year follow-up data were available on 106 patients (93%). Part I of the study was surgical versus conservative management, and 77 patients underwent surgery versus 34 enrolled in an exercise program. Surgical management resulted in better functional outcome, assessed by the Disability Rating Index (DRI), and decreased pain (p < 0.01). The exercise group DRI showed no improvement, and pain decreased only slightly (p < 0.02).
The Spine Patient Outcomes Research Trial (SPORT) degenerative spondylolisthesis study4 compared surgical and conservative management in the treatment of adult degenerative spondylolisthesis. The study enrolled 304 patients in the PRCT arm and 303 patients who declined randomization into an observational cohort. A major limitation of the study was that there was a significant crossover of patients between treatment arms, negatively impacting the intent to treat analysis. One hundred fifty-nine patients were randomized to surgery, 105 (66%) underwent surgery and were available for 4-year follow-up. One hundred forty-five patients were randomized to conservative care, but of the 99 patients available for follow-up at 4 years, 79 (54%) had undergone surgery. The as treated analysis resulted in the most useful information, that the surgically treated cohort was found to have significant improvements with regard to neurogenic intermittent claudication (NIC) pain (p = 0.006), NIC function (PCS p = 0.047; ODI p = 0.002), patient satisfaction, and self-rated progress over 4 years when compared with the conservatively treated group. Another limitation of this study was the lack of randomization and control for the surgical group because there was heterogeneity in the treatment received.
Both the SPORT4 and the Möller5 studies provide strong evidence to support the surgical management of adult low-grade spondylolisthesis that has failed a 3-month trial of conservative care.
Interspinous process decompression (IPD) is offered as an alternative to conservative care for low-grade degenerative spondylolisthesis by Anderson et al6 in their level I PRCT comparing IPD insertion versus nonoperative management. In this study 75 patients were randomized to either X•STOP Spacer placement (n = 42), or the control group (n = 33). At the 2-year follow-up, 63.4% of the X STOP group demonstrated significant improvement in pain and function, versus 12.9% in the control group. No comparison of this form of treatment to other surgical solutions has been made.
Comparison of fusion strategies (i.e., posterolateral fusion, interbody fusion, or combined/360 degrees) was examined in a level I study with a 5- to 9-year follow-up report.7,8 The patient population was heterogeneous containing isthmic and degenerative spondylolisthesis patients, as well as degenerative disk disease and failed back syndrome patients. Christensen et al8 enrolled 148 patients in a PRCT, and randomized patients into either posterolateral fusion with instrumentation (n = 73) or circumferential fusion (n = 75). At early follow-up, there was a trend toward better functional outcome in the 360-degree fusion group compared with the posterolateral fusion and instrumentation group (p < 0.08). The 5- to 9-year follow-up7 of patients, with a diagnosis of primary or secondary degenerative instability, demonstrated a better functional score in the 360-degree fusion group compared with those in the posterolateral lumbar fusion (PLF) group (ODI and Short Form (SF)-36 p < 0.01, and back pain p < 0.05). No significant differences in functional status scores were seen with regard to leg pain and between the two groups in patients with isthmic spondylolisthesis.
Carragee9 in a PRCT evaluated single-level posterolateral fusion with or without instrumentation in adults with low-grade isthmic spondylolisthesis. Forty-two patients were randomized to posterior lumbar fusion either with decompression (n = 18) or without (n = 24). All smokers in the study were automatically assigned transpedicular instrumentation, whereas nonsmokers were assigned no instrumentation. Interestingly, the addition of decompression to posterior lumbar fusion trended toward an increase in the pseudarthrosis rate (p = 0.02), leading to poor clinical outcome (p = 0.01) when compared with patients without decompression. Limitations of this study included the lack of randomization of instrumentation, and the higher incidence of smoking in the study compared with the general population.
Level II Data (Table 17.3)
The only level II study selected for the approach to adult low-grade spondylolisthesis was a prospective cohort study (PCS) comparing posterior lumbar interbody fusion (PLIF) and posterolateral fusion (PLF) and instrumentation.10 Inamdar et al enrolled 22 patients—11 PLF and 11 PLIFs. All patients received transpedicular instrumentation. Both cohorts achieved a 100% fusion rate, and there were no significant differences in terms of outcome as assessed by the Oswestry Disability Index (ODI) (PLIF 87.5% satisfactory results vs PLF 100% satisfactory results). Inamdar et al10 concluded that PLF was recommended versus PLIF due to the simplicity and lower morbidity between the two procedures.
Level III Data (Table 17.3)
There were three level III studies reviewed for the approach to adult low-grade spondylolisthesis. Kim and Lee11 retrospectively evaluated 40 patients with adult isthmic spondylolisthesis. Patients were placed into either an anterior interbody fusion group or a posterior lumbar fusion with instrumentation group. Reported clinical outcomes were 85% and 90% satisfactory for the AIF and PLF groups, respectively. The fusion rates were 90% and 95% for the AIF and PLF groups, respectively. No significant difference in either outcome measure could be demonstrated because both groups achieved similar results.
Matsudaira et al12 reviewed 53 patients treated with laminectomy, decompression, and PLF (n = 19), laminoplasty (n = 18), and nonoperative management (n = 13) in a cohort that refused surgery. There was no improvement over the 2-year follow-up for the group treated nonoperatively. When the nonoperative group was compared with the two surgical groups a level of significance was achieved (p < 0.0001) for improvement in the decompression and PLF, and laminoplasty groups. Although deformity progression was reported in the noninstrumented groups, there were no significant differences noted between the decompression and PLF, and laminoplasty groups. Matsudaira et al12 recommended laminoplasty over decompression and PLF citing motion preservation as a potential factor to lowering the incidence of adjacent-level disease.
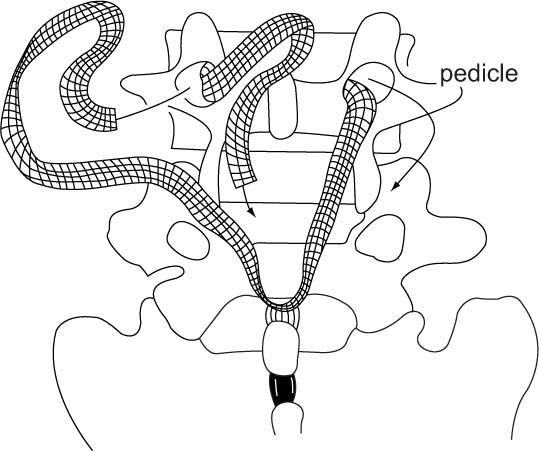
Mochida et al13 retrospectively evaluated 104 patients with degenerative spondylolisthesis enrolled in three groups: PLF and decompression (n = 35); PLF, decompression, and syndesmoplasty (Fig. 17.1) (n = 33); and decompression, PLF, with instrumentation (n = 34). There were no significant differences in outcomes between the three groups for patients with ≤ 10 degree of angular instability, but for patients with ≥ 11 degrees of angular instability transpedicular fixation resulted in a higher fusion rate (p = 0.0361 compared with noninstrumented, p = 0.0318 compared with syndesmoplasty) where the adjunctive use of instrumentation was recommended.
Fig. 17.1 Syndesmoplasty: Each end of either an artificial, allograft, or autograft ligament is passed beneath the spinous process of the caudad vertebrae then fed through the pedicles, crossed in a tunnel of the vertebral body, and pulled out to the contralateral pedicle. (From Mochida J, Suzuki K, Chiba, M. How to stabilize a single level lesion of degenerative lumbar spondylolisthesis. Clin Orthop Relat Res 1999;368:126–134. Reprinted with permission.)
Summary of Data
The majority of patients suffering from adult low-grade spondylolisthesis will respond to conservative management consisting of nonsteroidal antiinflammatory drugs (NSAIDs), activity modification, therapy, and steroid injections. Those failing a 3-month trial of conservative care are unlikely to improve and should be offered surgery because surgical management results in an improved clinical outcome compared with continued nonoperative management. The single level I study comparing the X•STOP®Spacer IPD device to conservative care reported promising early results, but no long-term data are available. X•STOP®Spacer insertion has not been compared with other forms of surgical care, thus further study is warranted.14 All studies reviewed clearly demonstrate significant improvements associated with surgery for the management of adult low-grade spondylolisthesis. Posterior lumbar fusion has been the most common procedure studied, but there is no clear advantage demonstrated for interbody fusion versus posterolateral fusion.15 There is a trend approaching significance at the long-term follow-up for circumferential fusion in patients with instability of degenerative7,8 and isthmic etiologies.16
Pearls
• In adult low-grade spondylolisthesis(isthmic and degenerative), for patients who fail initial conservative management, surgical management results in a better clinical outcome than continued nonoperative management.
• Level I evidence reports on the insertion of an interspinous process device (IPD) show an early clinical improvement when compared with nonoperative care. There is no current study comparing IPD insertion to decompression and posterolateral fusion.
• Evidence comparing interbody fusion [anterior lumbar inter-body fusion (ALIF), posterior lumbar interbody fusion(PLIF), and transforaminal lumbar interbody fusion(TLIF)] to posterolateral fusion is conflicting and demonstrates no clear advantage to one form of treatment over another.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree