Fig. 1
Two types of oral appliances used for the treatment of obstructive sleep apnea. Left panel: prefabricated “boil-and-bite” oral appliance after direct fitting in the patient. Right panel: custom-made monobloc oral appliance made on casts of the tooth arcs
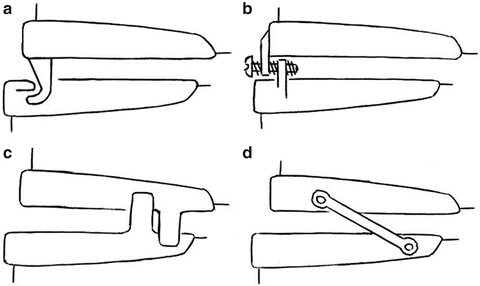
Fig. 2
Schematic overview of titratable, duo-bloc MRA designs used in current clinical practice. (a) OAm with an anteriorly articulating component. (b) OAm with attachments for adjustment of mandibular protrusion in the frontal teeth area. (c) OAm with two lateral positioning attachments for incremental protrusion of the mandible. (d) OAm with lateral telescopic rods that force the mandible into an anterior position (taken from [6])
When compared to CPAP therapy, OAm therapy has been proven to reduce the severity of sleep apnea to a lesser or similar extent than CPAP [8–11], although OAm therapy seems to have a higher acceptance rate and patient preference compared to CPAP [12, 13].
Recently, an objective compliance monitor for OAm therapy became available, allowing for calculation of the mean disease alleviation as a measure of therapeutic effectiveness [14]. This calculation showed that comparable therapeutic effectiveness between OAm therapy and the gold standard treatment for patients with OSA, being CPAP, has been reported because the superior efficacy of CPAP in alleviating OSA is offset by inferior acceptance and patient preference relative to OAm therapy [8, 14, 15].
Efficacy of Oral Appliance Therapy
OAm therapy is effective in reducing the apnea severity in some but not in all patients. In general 65 % of patients respond to the treatment with a ≥50 % reduction in apnea–hypopnea index (AHI) with the OAm in situ compared to baseline. On average 52 % of patients achieve an AHI < 10 events/h with the OAm in situ [12]. In the past, retrospective analyses of clinical, physiological, and polysomnographic variables were performed in order to identify predictors of treatment success with OAm therapy. There is evidence to support the findings that OAm therapy is more likely to be successful in younger female patients [16], with lower body mass index [17], a smaller neck circumference [11], and less severe sleep apnea [16, 18, 19].
In this chapter, we will focus on studies evaluating the effect of sleep position or the presence of supine-dependent OSA (sdOSA) on OAm efficacy. Eight [16, 20–26] studies evaluated the effect of sdOSA on the outcome of OA therapy. Six studies [16, 20–24] reported that the efficacy of OA therapy is influenced by sleep position in a way that patients with sdOSA have better treatment outcomes, where two other studies did not find a difference in success rates between non-sdOSA and sdOSA patients [25, 26].
In a study of Cartwright et al. [20], the association between the efficacy of a TRD and the factors obesity, age, supine sleep posture, and severity of sleep apnea was investigated in 16 male patients. The authors concluded that an increase in sleep apnea severity in the supine sleep position was the strongest predictor of success with a TRD.
Marklund et al. [16, 23] evaluated the effect of sdOSA on therapy outcome with success defined as AHI < 10 events/h in both the supine and non-supine sleeping positions with the OAm in situ. They reported that sdOSA was a strong predictor of successful apnea reduction with OAm therapy. In addition, it was suggested that a low AHI in the lateral position is important in predicting a successful apnea reduction with OAm therapy [23]. After subdividing the patient population according to gender, sdOSA remained the strongest predictor of OAm therapy success in men but did not relate to a successful apnea reduction in female patients [16].
Yoshida [24] assessed a significant decrease in both supine AHI and AHI in prone position under OAm therapy. The AHI increased in the lateral position, although not significantly. A successful apnea reduction under OAm therapy (AHI < 10 events/h) was achieved in 61.4, 84.6, and 0 % of patients with respiratory disturbances most frequently observed in supine, prone, and lateral position, respectively. Yoshida [24] concluded that the efficacy of OAm therapy is influenced by sleep posture.
In a study of Chung et al. [22] using Cartwright’s definition [27], the decrease in both total AHI as well as supine AHI under OAm therapy was significantly higher in sdOSA patients when compared to non-sdOSA patients. The decrease in non-supine AHI did not differ between the two groups. The complete response rate with AHI < 5 events/h under OAm therapy was higher in sdOSA patients when compared to non-sdOSA patients. Applying a multiple linear regression model, the presence of sdOSA turned out to be the only factor associated with a decrease in overall AHI or with a complete response.
Lee et al. [21] evaluated the efficacy of OAm therapy in 100 Korean patients in terms of supine dependency. The success rate, defined as a reduction in AHI of 50 % or more and an AHI under OAm of <10 events/h, was significantly higher in sdOSA compared to the non-sdOSA group.
Fransson et al. [25] subdivided their total patient population in supine-dependent ODI patients if 50 % or more of the estimated sleeping time was in supine position when desaturations were registered. In contrast with the previously described results that suggest that sdOSA is associated with a better treatment response, Fransson et al. [25] did not find a supine-dependent difference in responder rate, defined as patients with a reduction in ODI of at least 50 % or with an ODI value under OAm therapy of <5 events/h.
Sutherland et al. [26] assessed differences in treatment response among 386 patients with and without sdOSA. In this study, no difference in complete response (AHI < 5 events/h) was noted between sdOSA and non-sdOSA patients.
Several confounders must be taken into account when comparing the studies evaluating the effect of sdOSA on the outcome of OA therapy.
A first confounder is the presence of different criteria for sdOSA in the literature (Table 1). The application of three different criteria for sdOSA makes it hard to compare the prevalence of sdOSA and the effect of sdOSA among the different studies.
Table 1
Definitions supine-dependent obstructive sleep apnea
Definitions of supine-dependent OSA | Prevalence general population (%) | Prevalence population starting OAm therapy (%) | |
|---|---|---|---|
Cartwright et al. [27] | Supine AHI at least twice as high as non-supine AHI | 50–60 | 58–80 |
Mador et al. [32] | Supine AHI at least twice as high as non-supine AHI AHI < 5 events/h 15 min threshold for sleep in both postures | 20–35 | 27 |
Supine AHI ≥ 10 events/h together with non-supine AHI < 10 events/h | N/A | 46 | |
A second confounder is the lack of a consensus in literature regarding the definition of successful treatment outcome. Some studies defined success as a reduction in AHI under therapy of ≥50 % compared to baseline, while other studies used a posttreatment AHI of less than 5, 10, or 20 events/h as a successful treatment outcome. In addition, some studies used a combination of a reduction in AHI of ≥50 % compared to baseline combined with a posttreatment AHI of less than 5, 10, or 20 events/h as criteria for success. One study uses the ODI as the main outcome parameter with success defined as a reduction in ODI of at least 50 % or with an ODI value under OAm therapy of <5 events/h [25].
A third confounder is the use of different types of oral appliances in the discussed studies: one study used a TRD [20] whereas the other studies used an OAm [16, 21–26]. Furthermore, a monobloc OAm was used [16, 21, 23–25], whereas only in two studies a titratable OAm was used [22, 26]. In the studies using a monobloc OAm, four out of five studies (80 %) did find an association between the efficacy of OAm therapy and the presence of sdOSA, whereas only one out of two studies (50 %) using a titratable OAm could confirm these results.
Prevalence of Supine-Dependent Sleep Apnea Under Oral Appliance Therapy
The prevalence of sdOSA in a general population ranges from 20 to 60 %, depending on the definition used (Table 1). This prevalence was also studied in a more restricted population of patients starting OAm therapy. In order to do so, Marklund et al. [23] defined sdOSA as a supine AHI ≥ 10 events/h with a lateral AHI < 10 events/h. According to this definition, 46 % of patients were diagnosed as having sdOSA. Applying the same definition, Dieltjens et al. [28] found a comparable prevalence of 46 % prior to the start of the OAm therapy. In three studies, the prevalence of sdOSA as defined by Cartwright’s criteria was assessed before starting OAm therapy and ranged from 58 to 80 % [21, 22, 28]. In a study of Yoshida, 61 % of patients starting OAm therapy exhibited the respiratory events most frequently in supine sleeping position [24]. Overall, the prevalence of sdOSA found in patients starting OAm therapy ranged from 27 to 80 % and was comparable to the prevalence of sdOSA in the general population (Table 1). These results however do not reveal the evolution of sdOSA once OAm has started, and until recently, the prevalence of sdOSA under OAm therapy was unknown. In a recent study 183 patients with polysomnographic data before and under OAm therapy were evaluated showing a prevalence under OAm therapy ranging from 18 to 34 %, depending on the definition used. In addition, it was shown that up to one third of patients shift from non-sdOSA at baseline to sdOSA under OAm therapy [28].
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree






