35.1 Introduction
Antipsychotic medications are agents that are used to treat psychoses, such as that associated with schizophrenia or mania. They are used also for acute and chronic thought disorders and confusion, extreme aggressive behaviors, delirium, and dementia that accompanies conditions such as Alzheimer’s disease. Target symptoms for these drugs include disorganized speech and behavior, flat or inappropriate affect, delusions, hallucinations, and catatonic behavior.
Antipsychotic medications are divided into (a) “typical” or first-generation antipsychotic (FGA) drugs, and (b) “atypical” or second-generation antipsychotic (SGA) drugs.
The first generation of antipsychotic medications was developed based on the hypothesis that schizophrenia reflects a disorder of excess dopaminergic activity and that antagonism of the dopamine D2 receptor is most strongly associated with antipsychotic response. For many patients with schizophrenia, the widely used FGAs (phenothiazines, butyrophenones, and others), which are also referred to as “conventional,” “traditional,” or “typical” antipsychotic drugs, are effective in the treatment of positive symptoms of the illness, and also in preventing psychotic relapse. Accordingly, these agents have permitted many patients to live independently in the community.
However, there are substantial limitations with the use of FGAs. Up to 60% of patients treated with FGAs remain symptomatic and are considered either treatment refractory or only partially responsive. In particular, at best, these drugs only modestly improve negative and cognitive symptoms. FGAs also cause a variety of objective and subjective side-effects, both acutely and with long-term exposure. These side-effects, in many instances, reduce treatment adherence, which leads to relapse and re-hospitalization.
The SGAs were heralded in the 1970s with the development of clozapine. Its advantages over the FGAs included greater efficacy for treatment-refractory schizophrenia, amelioration of some of the negative, cognitive, and mood symptoms of schizophrenia, potential reduction in the likelihood of suicidal behavior, very low liability for acute and chronic extrapyramidal symptoms, and no associated induction of sustained hyperprolactinemia. In the years that followed the introduction of clozapine, concerted research and development efforts were made to replicate the drug’s therapeutic profile while avoiding the associated risk of agranulocytosis. Although this goal was never fully realized, the initiative spawned a second generation of atypical antipsychotic medications. Although none of these second-round agents have matched the singular effectiveness of clozapine, they have broadened the therapeutic repertoire available for the treatment of schizophrenia and other psychotic illnesses.
The role of dopamine systems in the pathophysiology and treatment of psychotic disorders has been a subject of intense investigative scrutiny for the past 50 years. Although other systems have since been implicated, the dopamine D2 receptor is still regarded as the primary target associated with antipsychotic effect, as well as with the induction of extrapyramidal syndrome (EPS) and prolactin elevation. All clinically approved, currently used antipsychotic drugs share D2 receptor antagonism properties to some extent.
Differences among antipsychotics in dopamine receptor activity have been proposed to account for the “atypicality” of SGAs; that is, their tendency to produce antipsychotic effects at considerably lower doses than those that induce EPS. Another hypothesized mechanism of SGA atypicality involves regionally selective dopamine receptor binding.
35.3 First-generation Antipsychotics
FGAs, as a class, are equally effective in the treatment of psychotic symptoms of schizophrenia, though they vary in potency, side-effect risks, and other pharmacologic properties (Table 35.1). Attributes common to all FGAs are a high affinity for, and full antagonist activity at, dopamine D2 receptors. In addition, all FGAs are capable of producing EPS and increasing serum prolactin concentration, to varying degrees, when used in the usual clinical dosage range. Based on their chemical structure, FGAs may be divided into three groups: butyrophenones, phenothiazines, and others. The butyrophenones, represented by haloperidol, tend to be potent D2 antagonists and to have minimal anticholinergic and autonomic effects. The phenothiazines block D2, acetylcholine, serotonin, histamine, and norepinephrine receptors, each of which is associated with certain adverse effects.
Table 35.1 First-generation antipsychotics.
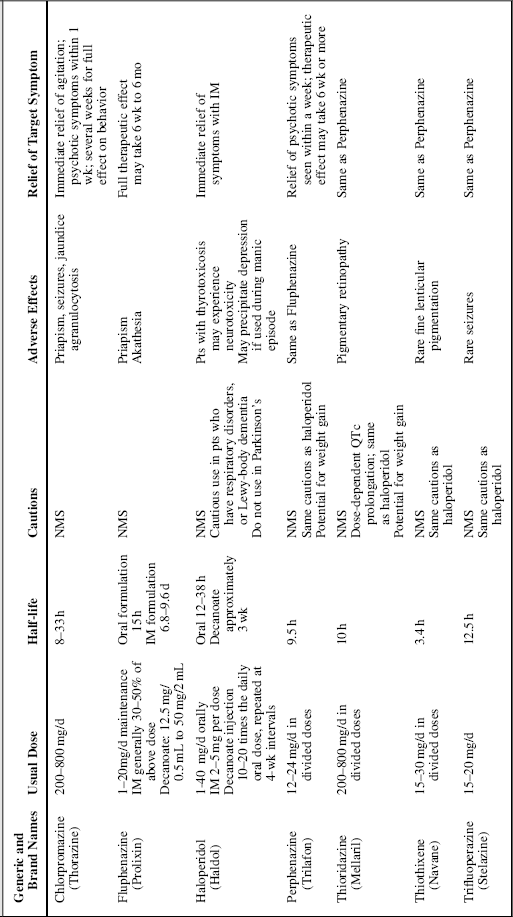
As a class, the FGAs are associated with a high degree of pseudoparkinsonism or EPS due to the blockade of the dopaminergic system, the movement disorder tardive dyskenesia, and a life-threatening condition, neuroleptic malignant syndrome (these are discussed later in the chapter). They may also have the same anticholinergic properties as TCAs, causing the same bothersome symptoms of dry mouth, constipation, blurred vision, and drowsiness.
35.4 Second-generation Antipsychotics
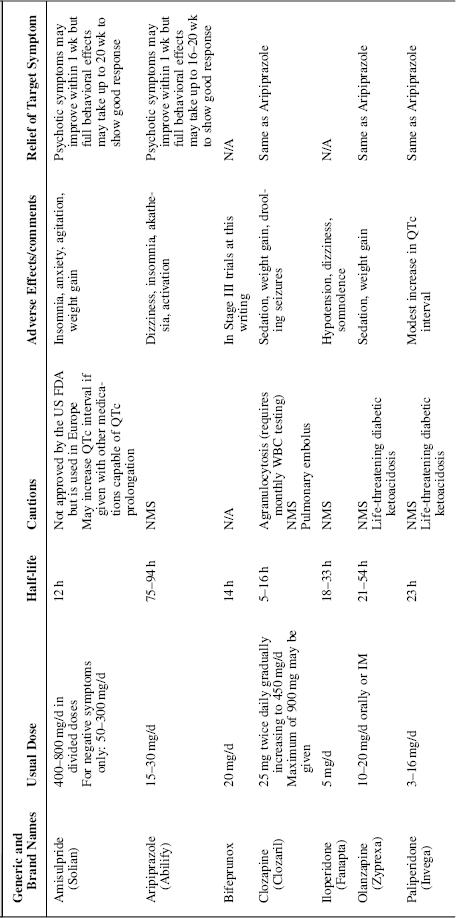
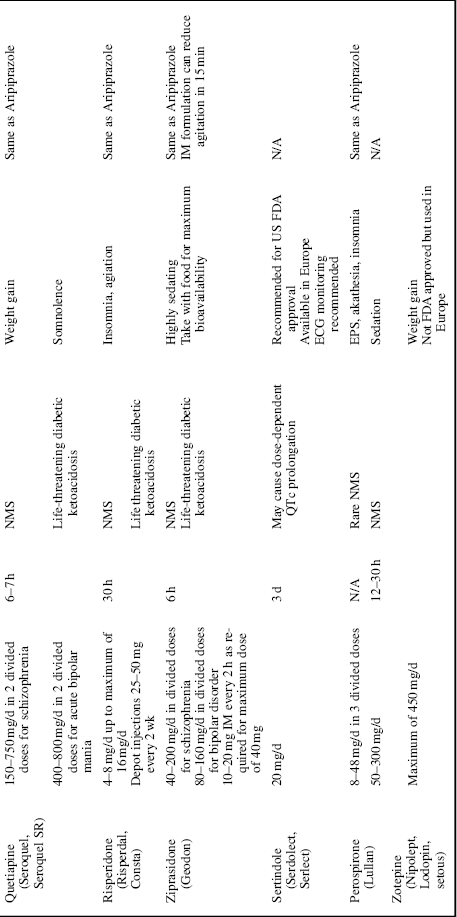
The SGAs are a group of unrelated drugs united by the fact that they work differently from the FGAs. Most share a common attribute of working on serotonin as well as dopamine receptors. Amisulpride does not have serotonergic activity, but rather is a partial dopamine agonist. Aripiprazole also displays some partial dopamine agonism, 5-HT1A partial agonism, and 5-HT2A antagonism. In this chapter, SGAs refer to clozapine, risperidone, olanzapine, quetiapine, ziprasidone, sertindole, amisulpride, perospirone, zotepine, aripiprazole, paliperidone, iloperidone, and bifeprunox (Table 35.2).
Table 35.2 Second-generation antipsychotics.
Rapid neuroleptization was proposed decades ago as a strategy for managing agitation in acutely psychotic patients. This practice involved the use of high doses of intramuscular high-potency FGAs, usually haloperidol, administered repeatedly over a 24-hour period, until the patient demonstrated obvious sedation or other effects. In the years after the introduction of rapid neuroleptization, a number of well-controlled, double-blind studies comparing high-dose strategies with standard-dosage regimens revealed no significant superiority for high dosage in either degree or rapidity of response in acutely psychotic patients. Moreover, very high doses of FGAs produced a significantly greater incidence of extrapyramidal symptoms, particularly akathisia and akinesia, which can cause significant discomfort and worsen outcome. Thus, rapid neuroleptization has been largely abandoned as a therapeutic strategy.
35.6 Conditions Treated with Antipsychotic Medications
At present, SGAs are prescribed primarily for schizophrenia; however, they are being used increasingly for other psychiatric disorders, as happened with FGAs. A proportion of these uses are empirically well supported, but only preliminary or moderate evidence exists for others. In particular, the prescription of SGAs for nonpsychotic disorders in children and adolescents has become progressively more common, despite limited data regarding the efficacy and safety of this practice.
In common practice, conditions that are treated with antipsychotic medications include adult and childhood schizophrenia, schizoaffective disorder, major depression with psychotic features, bipolar disorder, borderline personality disorder, Tourette’s disorder, substance-abuse disorder, delirium, impulse control associated with aggression and violent behavior in youth, dementia, and Huntington’s disease.
35.7 Adverse Effects of Antipsychotics
35.7.1 Neuroleptic Malignant Syndrome
The most serious and potentially fatal side-effect of the antipsychotic medications is neuroleptic malignant syndrome (NMS), which is characterized by severe muscular rigidity, altered consciousness, disorientation, dysphagia, elevated creatine phosphokinase, stupor, catatonia, hyperpyrexia, and labile pulse and blood pressure. This life-threatening condition can occur after a single dose of a neuroleptic drug, but it is more common during the first two weeks of administration or with an increase in dose. This syndrome can continue for up to two weeks after the discontinuation of medication. Treatment involves immediate cessation of the medication and hospitalization to stabilize acute symptoms.
35.7.2 Tardive Dyskenesia
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree




