Fig. 10.1
Acute phase of deep venous thrombosis (right thalamostriate vein). The FLAIR sequence (a) shows the venous infarction with very limited hyperintensity on diffusion-weighted images (c) related to predominantly vasogenic oedema. The thrombus is visible as hypointensity on T2-weighted GE images (b black arrow) in the wall of the right lateral ventricle, with a delta sign on gadolinium-enhanced T1-weighted images (d white arrow) associated with enhancement of the vein wall without enhancement of the thrombus. The CBV (e) is slightly modified in the affected territory, with prolonged MTT (f) related to venous oedema
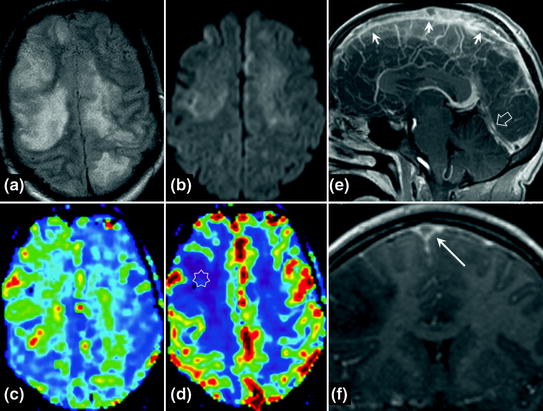
Fig. 10.2
Acute phase of cerebral venous thrombosis (superior sagittal sinus and straight sinus). Venous infarction is visible as a hyperintensity on FLAIR images (a) with variable signal on diffusion-weighted images (b ADC mainly normal or increased). Characteristic appearance of venous oedema on perfusion-weighted sequences with prolonged MTT (c green and red) compared with normal cerebral parenchyma (blue) and moderately decreased CBV (d star). On gadolinium-enhanced T1-weighted sequence sagittal section, thrombus is visible in the superior sagittal sinus (e 3 small arrows) and straight sinus (e hollow arrow). Note the delta sign on the gadolinium-enhanced T1-weighted sequence with coronal reconstruction (f long arrow)
Clinical Features
Incidence: 0.5 % of strokes.
Occurs at any age with a female predominance.
No clearly defined anatomical and clinical syndrome due to the anatomical variability of the cerebral venous system and the possible presence of collateral vessels.
Variable onset. Classical clinical presentations: isolated intracranial hypertension (25 %) with progressive headache (always present), bilateral papilloedema on funduscopy, sometimes sixth cranial nerve palsy, shifting focal neurological deficits, seizures, disturbances of consciousness, signs of encephalopathy.
Ten to 20 % of patients present signs of confusion or isolated psychiatric disorders or sometimes recent isolated headache with normal brain CT scan and CSF analysis.
Aetiologies
Multiple causes are often associated.
Local: head injury, tumours, arteriovenous malformations, developmental venous anomaly (rare).
Infections: local (ENT: sphenoid and petrous part of temporal bone) or systemic.
Systemic diseases: systemic lupus erythematosus, Behçet’s disease, congenital thrombophilias, coagulopathies, neoplasms, haematological diseases, iron deficiency, drugs.
Gynaecological and obstetric: postpartum more often than pregnancy and oral contraception.
Idiopathic.
Investigations
D-Dimers: if normal, excludes the diagnosis of recent venous thrombosis except when the patient reports isolated headache: 25 % of patients with normal D-Dimers.
Complete blood count, platelets (looking for haematological diseases), PT, APTT, CRP.
Lumbar puncture if feasible (meningitis, assessment of CSF pressure), before starting anticoagulant therapy. In the absence of an intracerebral lesion responsible for a mass effect, lumbar puncture is indicated in this context (even in the presence of intracranial hypertension).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








