(1)
Mayo Clinic, Rochester, MN, USA
Several terms that reappear throughout this chapter are first defined: neural foramen, nerve root, and foraminotomy.
When two contiguous vertebrae are apposed, a lateral, somewhat cylindrical tunnel is formed that serves as an exit for segmental nerve roots. From the standpoint of surgical importance, the ventral floor is made up of the disc space and the adjacent joint of Luschka. The roof is formed by the overlapping inferior and superior zygapophyseal joints. Superiorly and inferiorly, the pedicles of the respective vertebrae form the bony limits; this constitutes the neural foramen.
The nerve root is the most important structure that passes through this foramen. It is invested by surrounding fat and accompanied by epidural veins (Fig. 41.1). This nerve root is composed of a sensory ganglion and its proximal preganglionic axons and postganglionic motor axons arising from the anterior horn cells within the spinal cord and terminating in the muscle fiber they innervate. These sensory and motor structures are bathed by cerebrospinal fluid and invested by an outpouching of the common dural sac referred to as the dural root sleeve. It is this structure that is seen at the time of surgical exposure.
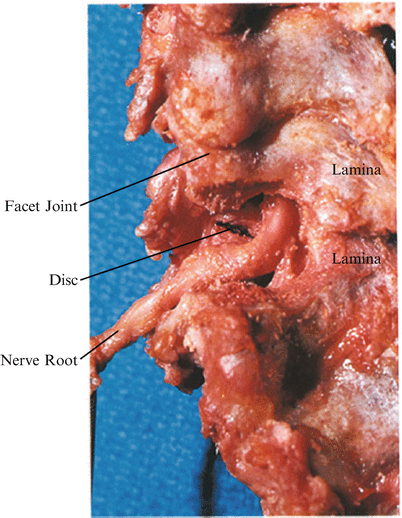

Fig. 41.1
Ventral retraction of the nerve root shows the intervertebral disc
The C5 nerve root forms a 45-degree angle with the spinal cord as it traverses its foramen, and this angle increases as one descends; so that C8 is essentially at right angles as it enters the spinal canal outlet.
Foraminotomy is decompression of a nerve root by removal of offending pathologic material within and in the proximity of a neural foramen. Ventrally, disc material or osteophytic bone may be removed. The latter is particularly true of the joint of Luschka, whose hypertrophic excrescences usually encroach on the nerve root within its axilla. Dorsally decompression is accomplished by resection of the medial aspect of the superior and inferior facets; this is performed with a high-speed drill.
It is imperative to determine preoperatively the extent of neck flexion tolerated by the patient without aggravating neurologic symptoms.
1.
In spite of the inherent dangers of air embolism, I prefer the upright position to the prone (Fig. 41.2) [1 , 2] The Mayfield headrest is used. Skeletal pin fixation remains an option, but I prefer the “horseshoe” headrest. The suboccipital scalp is shaved sufficiently to tape the head in place and to allow operative preparation of the surgical field. Flexion of the neck distracts the facets and facilitates exposure, as does slight lateral flexion contralateral to the lesion.
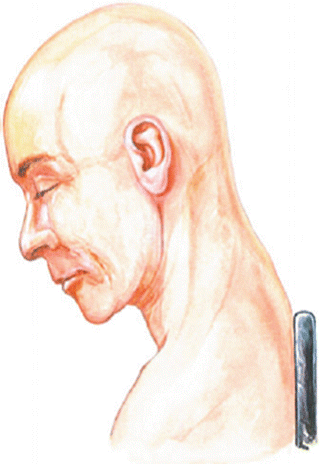

Fig. 41.2
The upright position is used in preference to the prone position. The Mayfield headrest supports the head. Skeletal pin fixation remains an option, but the horseshoe headrest is preferred. The occipital scalp is shaven sufficiently to tape the head in place and to allow operative preparation of the surgical field. Flexion of the neck distracts the facets and facilitates the exposure, as does slight lateral flexion contralateral to the lesion. There is some inherent danger of air embolus in the upright position
2.
The level and length of the midline posterior cervical incision are determined by external landmarks, for example, a prominent C7 spinous process. Meticulous attention to hemostasis is essential. To accommodate the application of hemostatic Raney clips, the subcutaneous tissue may be slightly undercut.
3.
A self-retaining retractor is placed and the trapezius fascia incised, allowing retraction of the muscle mass on the side of the lesion.
4.
Then, the splenius and semispinalis capita, the lower semispinalis cervicis, and the multifidus muscles are separated from the spinous processes and contiguous laminae by subperiosteal dissection with a periosteal elevator or Bovie “cutting” electrocautery.
5.
Get Clinical Tree app for offline access

The wound is repeatedly irrigated with a sterile saline or comparable solution to cool the operative field when the electrocautery is used; this helps prevent potential air embolism. Muscle stripping is greatly facilitated when the bony projection of a bifid spinous process is resected on the side of the exposure (Fig. 41.3).
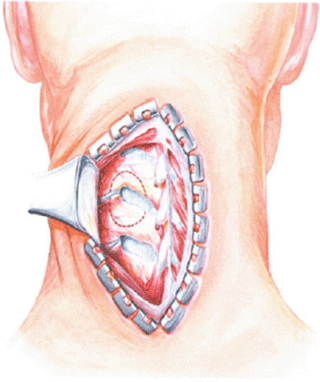

Fig. 41.3




The incision should extend two spinous processes above and two below the desired level. Open the skin and subcutaneous tissue. Slightly undercut the subcutaneous tissue and apply hemostatic Raney clips. Place the self-retaining retractor and incise the trapezius fascia. Retract the muscle mass on either side of the lesion. Use either a periosteal elevator or the cutting electrocautery to remove the paraspinous musculature from the spinous process and the lamina of the involved side. Beginning at the tip of the spinous process, obtain the subperiosteal plane before sweeping out on the lamina. Resection of the bifid spinous process may aid greatly in the muscle stripping exposure. Irrigate repeatedly with saline. Maintain meticulous hemostasis
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








