Artifactual
Rhythmic, regular or paroxysmal muscle movement, ECG, or ballistocardiographic artifacts
Physiologic rhythmic patterns or patterns of nonepileptic significance
Rhythmic midtemporal theta of drowsiness
Subclinical rhythmic epileptiform discharges of adults (SREDA)
Pathologic epileptiform patterns
PLEDs [LPDs]
PLEDs plus [LPDs + F]
BiPLEDs [BIPDs]
GPEDs [GPDs]
Triphasic waves [GPDs with triphasic morphology] (e.g., in hepatic dysfunction, uremia, anoxia; hyperammonemia; toxicity/drugs)
Rhythmic delta activity
Other abnormal EEG patterns that normalize concurrently with clinical improvement after IV benzodiazepines (benzodiazepine-responsive withdrawal encephalopathy)
Classification
Prior classifications of status epilepticus have been suggested on the basis of etiology, clinical phenomenology, pathophysiology, and EEG characteristics [15]. More recently, the Commission of Classification and Terminology of the International League Against Epilepsy charged a Task Force with revising the classification of status epilepticus. This group in turn created a classification based on four axes: (i) semiology, (ii) etiology, (iii) EEG correlates, and (iv) age [16]. Various forms are differentiated along taxonomic lines into motor activity, and impairment of consciousness, producing two major groups: [1] status epilepticus with prominent motor symptoms, including all convulsive forms, and [2] those without prominent motor forms representing non-convulsive forms of status epilepticus (NCSE). Each group can be subdivided by the degree of consciousness impairment, while etiology divides into: (i) known or symptomatic (also subdivided into acute symptomatic, remote symptomatic and progressive symptomatic), and (ii) unknown or cryptogenic. Known causes of status appear as an appendix. The third axis comprises EEG correlates—more important in NCSE. Descriptors adopted (such as morphology, location, time-related features) were adopted from those developed by the American Clinical Neurophysiology Society [17]. Nonconvulsive status epilepticus (NCSE) had previously been divided into two groups, largely along electroencephalographic criteria:
- 1.
Absence status epilepticus (ASE), a form of generalized nonconvulsive status epilepticus (GNSE)
- 2.
A lateralization-related nonconvulsive state, referred to as complex partial status epilepticus (CPSE).
Each of these groups has been subdivided further. GNSE includes:
- 1.
Patients with a history of childhood absences characterized by three-per-second spike-and-waves (ASE)
- 2.
Patients with childhood-onset, secondary generalized epilepsy, usually with mental retardation, more marked confusion and myoclonus
- 3.
Elderly patients presenting de novo, usually in association with a toxic or metabolic dysfunction, psychotropic medications or benzodiazepine withdrawal, or triggered by a tonic-clonic seizure
- 4.
Generalized nonconvulsive status epilepticus from partial onset of temporal or frontal origin.
The behavioral correlates of different types of NCSE arise from—or are at least associated with—different areas of maximal involvement of seizure activity identifiable by EEG. Hence the proclivity of seizure activity for frontal, mesial temporal, neocortical temporal, and temporo-parieto-occipital junctional regions has come to be correlated with particular symptomatic or behavioral features particular to those brain regions. Additionally, such presentations are seen to occur with certain underlying associated conditions such as mental retardation, uremia, or Alzheimer disease, and therefore achieve clinical expression within the framework of the age of the patient. There are, therefore, particular clinical features typically seen in infants, small children, adults, or the elderly, although there is considerable overlap. A classification of types of NCSE based on localization-related EEG criteria as well as age of expression and particular epileptic syndromic context is provided in Table 20.2. Many of these features are superseded by the latest classification of the Task Force, but are provided, as they are familiar to many clinicians of the past two decades.
I. Generalized nonconvulsive status epilepticus (GNSE) |
A. Absence status epilepticus (ASE) |
i. Typical absence status epilepticus (TAS) occurring in idiopathic generalized epilepsies, with 3/s spike-and-wave |
ii. De novo reactive (situation-related) absence status in the elderly, usually with neuroleptic medications, or following drug withdrawal |
iii. Absence status with degenerative generalized epilepsies; progressive myoclonic epilepsies |
iv. Secondary generalized NCSE of frontal or temporal lobe origin |
B. Atypical absence status epilepticus (AASE) |
i. Seen in childhood with secondary generalized epilepsy, usually with mental retardation (cryptogenic and symptomatic) e.g., with Lennox-Gastaut syndrome. EEG shows “slow” spike-and-wave at <2.5 Hz |
IIa. Simple partial status epilepticus (also see IIb) |
i. Frontal lobe simple partial NCSE with affective/cognitive features |
ii. Parietal lobe simple partial status with somatosensory features |
iii. Temporal lobe simple partial status with autonomic features |
iv. Occipital lobe simple partial status with visual features, with or without nystagmus |
IIb. Complex partial status epilepticus (CPSE) |
i. Frontal lobe (FCPSE) Fronto polar/fronto-central NCSE, with severe confusion and major behavioral disturbances (Supplementary motor, cingular, orbito-frontal, dorsolateral frontal lobe epilepsies exist, but localized status is rarely documented) |
ii. Temporal lobe (TCPSE) |
(a) Mesial temporal lobe |
(1) Hippocampal or medial basal, limbic (experiential hallucinations; interpretative illusions) |
(2) Amygdalar or anterior polar amygdalar (nausea, fear, panic, olfactory hallucinations progressing to staring with oral/alimentary automatisms) |
(b) Lateral (neocortical) posterior temporal lobe with auditory or visual perceptual hallucinations progressing to disorientation, dysphasia and head movement (nystagmus; staring) |
(c) Opercular/insular with vestibular/autonomic hallucinations (progressing to staring and oral/alimentary automatisms) |
III. NCSE presentation by age (some overlap with IA and B) |
i. Neonatal NCSE |
ii. Myoclonic-astatic epilepsy with AASE |
iii. Electrical status epilepticus during slow sleep (ESES) |
iv. Landau-Kleffner syndrome (acquired epileptic aphasia) |
v. Minor epileptic status of Brett |
vi. Rolandic status |
vii. NCSE in the elderly (also see IAii) |
IV. NCSE presentation with learning delay and mental retardation (some overlap with IA, B, III i–v) |
i. In children |
ii. In adolescents |
iii. In adults |
V. Electrographic status in coma |
i. Subtle status, usually post convulsive status epilepticus (CSE) |
ii. With major CNS damage, often with multiorgan failure, (with facial, perioral and/or limb myoclonias), but without apparent preceding CSE |
VI. Allied ictal states |
i. Confusion, with periodic lateralized epileptiform discharges (PLEDs or LPDsa) or PLEDs plus LPDs-plusa |
ii. Confusion, with bilateral independent periodic lateralized epileptiform discharges (BiPLEDs or BIPDsa) |
iii. Confusion, with bilateral synchronous epileptiform discharges (GPEDs or GPDsa) |
iv. Epileptic encephalopathies: altered mental status with disorganized diffuse or multifocal epileptiform features [e.g., with hypsarrhythmia; interictal severe Lennox-Gastaut syndrome; borderline NCSE vs triphasic wave toxic encephalopathies (lithium, baclofen, tiagabine)] |
EEG Diagnosis of NCSE
A major challenge in definition has been the correct EEG identification of seizures. Because the determination of what represents seizures, and thus SE, on EEG depends on somewhat subjective interpretation, the art of diagnosis depends on accurate EEG interpretation. A universal EEG definition of seizure activity has been hard to pin down, as evidenced by the problems that even sophisticated, computerized seizure and spike detectors have had in correctly identifying seizures and distinguishing them from artifact. Some typical themes, however, can be noted. Seizures captured in their entirety will typically show a progression from low-voltage high-frequency spikes to high-voltage lower-frequency spike slow-wave activity before stopping abruptly and being replaced by background suppression. This progression from fast to slow components can be used to identify an isolated seizure. Problems arise, however, when the patient is in SE and activity thought to be epileptic, precedes the beginning of the tracing and continues beyond the end of the tracing. In such cases, a rhythmicity, often with variability, typically faster than one-per-second is usually seen. Rhythmic activity may contain sharply contoured or spiky components, typical spike slow-wave or polyspike-slow-wave complexes, or even rhythmic theta or delta frequencies. The major differential diagnostic confounders are epileptiform morphologies usually seen at less than one-per-second, such as periodic lateralized epileptiform discharges (PLEDs [or LPDs]), bilateral independent periodic lateralized epileptiform discharges (BiPLEDs [or BIPDs]), or even bilateral synchronous epileptiform discharges (GPEDs [or GPDs]), all of which may be seen in cortical hyperexcitable states that may follow seizures in a patient with a structural abnormality, or in patients with encephalitis (For updated terms for the types of periodic discharges (LPD, GPD, BIPD), see Hirsch and colleagues [17]). These states representing cortical “irritability,” even with a clinical correlate of diminished level of consciousness, have historically not been classified as active seizures. The electrical activity has been judged to be insufficiently fast, and to lack a more flagrant clinical correlate (such as clonic activity) to be epileptic or “ictal.” Nonetheless, this borderline is a “gray zone” because epileptic activity may not particularly originate in the motor cortex so as to produce clonic activity; conversely it may represent the end of the electroclinical continuum that follows convulsive status epilepticus [18].
Toxic, metabolic, and infectious encephalopathies, benzodiazepine withdrawal states, and neuroleptic malignant and serotonin syndromes may all be associated with altered behavior and levels of consciousness, accompanied by an abnormal EEG, often with epileptiform features such as triphasic waves (GPDs with triphasic morphology). In this way, these states resemble, and can be confused with, NCSE, even to the point of suppression of “ictal” triphasic-wave activity after IV benzodiazepines.
Differential Diagnosis
Differentiation of types of NCSE along clinical lines—for example, differentiating cases of CPSE from GNSE—can be problematic because of the marked overlap among the clinical characteristics of the different types of NCSE [15, 16, 18–77]. Such blurring of the lines can be seen in the many publications that provide clinical correlates to clearly identified focal or generalized nonconvulsive status. For example, historically, total unresponsiveness was said not to occur in the absence status, but such patients have been noted. Impaired consciousness may be common to many types of NCSE, as may be fluctuation in the level of consciousness, bradyphrenia and bradykinesia, confusion, or even simple automatisms.
Nonetheless, some generalizations can be made regarding CPSE and ASE. Fear, aggressivity, irritability, and anxiety are seen more frequently with CPSE than with ASE [42]. Similarly, stereotyped, complex automatisms are also more frequent in CPSE [42]. Lip-smacking, other oroalimentary automatisms, lateralized limb automatisms, and dystonic posturing, eye deviation, and nystagmus are typical of CPSE [38, 42–44]. In both CPSE and ASE, patients may be agitated, violent, and aggressive, and may experience hallucinations. The following sections delineate the behavioral features, emphasizing distinguishing characteristics.
Taking a step back, it may not be as important to characterize NCSE into ASE or CPSE, as it is to recognize NCSE at all. At Johns Hopkins Bayview Medical Center, where some 300+ patients with NCSE have been identified over the past 30 years, the diagnosis was frequently delayed or even missed [12, 40]. Table 20.3 describes clinical examples with such scenarios. To state the obvious, the suspicion that NCSE is present must enter the mind to trigger a request for an EEG, enabling diagnosis. Although cases of NCSE may present initially on any floor of the hospital, there are particular presentations favoring the emergency room, intensive care units, and on neurology and psychiatry services. NCSE may resemble other disorders. Examples of some of these are given in Table 20.4 (see also Chap. 2, “Types of Status Epilepticus: Definitions and Classification”).
Lethargy and confusion attributed to a postictal state |
Ictal confusion mistaken for metabolic encephalopathy |
Unresponsiveness and catalepsy presumed to be psychogenic |
Obtundation thought to be due to alcohol or drug intoxication |
Hallucinations and agitation mistaken for psychosis or delirium |
Lethargy presumed secondary to hyperglycemia |
Mutism attributed to aphasia |
Laughing and crying ascribed to emotional lability |
Neurologic |
Mitochrondrial encephalopathies |
Transient global amnesia |
Organic brain syndrome |
Posttraumatic amnesia |
Complex migraine |
Vascular compromise—ischemic; inflammatory |
Toxic/Metabolic |
Toxic/metabolic encephalopathy |
Alcohol, benzodiazepine withdrawal |
Hypoglycemia |
Hypercalcemia |
Neuroleptic malignant syndrome |
Serotonin syndrome |
Drugs: lithium, baclofen, tricyclics, tiagabine, cefepime |
Epilepsy/Seizure-related |
Typical absence status epilepticus |
Atypical absence status epilepticus |
Lennox-Gastaut syndrome with encephalopathy |
Altered mental states with PLEDs (LPDs)/GPEDs (GPDs)/BiPLEDs (BPDs) |
Prolonged postictal confusion |
Epileptic fugue states/poriomania |
Interictal/postictal psychosis |
Psychiatric |
Acute psychotic reactions |
Somatoform disorders |
Dissociative conversion reactions |
Malingering |
Clinical and Behavioral Correlates of NCSE
Typical Absence Status Epilepticus
Typical and atypical ASE have been described as petit mal status, minor epileptic status, spike-wave stupor, epileptic twilight state, prolonged epileptic twilight state, absence continue, epilepsia minoris continua, ictal psychosis, status pyknolepticus, and état de mal a l’expression confusionnelle.
Typical absence status epilepticus (TAS) may be recognized initially only in a minority of patients (19%) and is often misdiagnosed as CPSE, postictal confusion, depression, posttraumatic amnesia, hysterical behavior, schizophrenia, or toxic states [45, 47]. Three quarters of the cases appear before the age of 20 years, and in a third, TAS heralds epilepsy [47]. The typical clinical features described in the absence status epilepticus are given in Table 20.5.
Table 20.5
Clinical features described in absence status epilepticus (from Kaplan [14] with permission)
Attitude | Behavior |
Unreactivity to threat | Inappropriate for situation with preserved alertness |
Lack of initiative | Infantile behavior |
Inability to plan | Fugue states |
Withdrawal | Catatonia |
Affect | Psychiatric |
Indifference | Hallucinations |
Perplexity | Paranoid persecution |
Crying | Experiential |
Laughing | Feeling of oppression |
Aggressivity | Uncontrollable rush of thoughts |
Memory/Cognition | Desire to (but inability to) perform simple motor acts (motor apraxias) |
Variable amnesia | Dreamy state: “feels vague” |
Slow ideation | “In a different world” |
Disorientation | “Drifting away” |
Speech | “Drunk” |
Verbal perseveration | Worried; edgy |
Monosyllabic answers | Dizzy |
Lack of spontaneous speech | Missing pieces of conversation |
Interrupted speech | Central vision “vibrates” |
Clicking noises in mouth | Other |
Motor | Incontinence |
Hippus | Diarrhea |
Clumsy motor performance | Headache |
Motor perseveration | Frontal release signs |
Automatisms (chewing; compulsive handling of objects) | Babinski reflex |
Rhythmic blinking | |
Eye rolling | |
Small amplitude jerking of face or arms | |
Quivering of lips | |
Tonic neck spasms | |
Ataxic gait/pseudoataxia | |
Wandering |
Typical absence status epilepticus starts abruptly and without warning (see Chap. 15, “Status Epilepticus in the Idiopathic Generalized Epilepsies”). Typical features include perioral myoclonus, myoclonic eyelid twitching, mild to marked obtundation, bradyphrenia and bradykinesia, and confusion [47]. The change in responsiveness can be highly variable, an illustration of which is provided in Fig. 20.1 [56]. Verbal functioning is usually preserved, but there may be poverty of speech and monosyllabic answers. Amnesia is not invariably present, and many patients can describe their experiences as they go into and remain in ASE [47]. Such descriptions can be seen in the subsection “Experiential” in Table 20.5. The following are typical experiential accounts of TAS
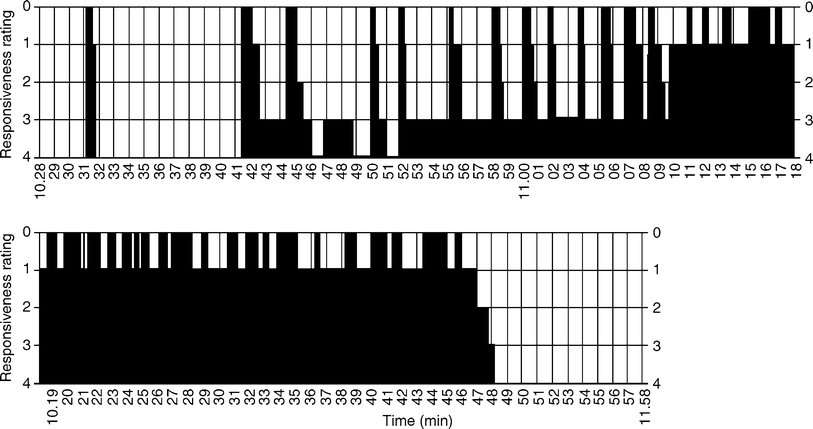

Fig. 20.1
Responsiveness during petit mal status. The patient has a brief absence attack at 10:31 AM, then a series of attacks beginning at 10:41 AM, with intervening periods of normal responsiveness. She had severe impairment of responsiveness from 11:10 to 11:48 AM, and then made a sudden recovery without postictal abnormality or complaint. The verbal responsiveness rating is as follows: 0 no response; 1 minimal response; 2 comprehension, follows simple directions, identifies receptively, cannot answer verbally, anomia may be present; 3 partial responsiveness, responds appropriately with one or two words and rote phrases, abnormal affect, some anomia; 4 accurate and immediate response, normal affect, responds to others’ comments, and initiates conversation, responds with more than one response to others’ comments, and initiates conversation, responds with more than one or two words. From Theodore and Porter [56] with permission
Mild clouding: mind slows down, understands, but delay in formulating answers; central visual field vibrates; feels drunk; perioral myoclonus; mild clouding with lip twitching so intense that could not drink coffee; marked clouding with funny feeling, lip twitching and amnesia; mild clouding with dizziness, feeling not oneself, and difficulty communicating; gradual but marked clouding with feeling edgy, uncomfortable and worrying, increasing intensity, limb jerking and wanting to withdraw to a safe place; mild clouding; feeling muzzy headed, strange, slow and “not myself”; fluctuating mild clouding—unable to look after myself, drowsy and off work; jerking of eyes [47].
Other vivid descriptions include
Mild clouding with slow communication, eyelid fluttering and spasm in neck; fluctuating mild to marked clouding with change in character, becoming extremely snappy with severe headache and frequent jerks of the arms; gradual marked clouding with tiredness, difficulty concentrating, able to hear but struggling to find the meaning; mild to marked clouding with drifting away, slowness of answers followed by amnesia; fluctuating mild to marked clouding, feeling disturbed, vague, uncooperative, slow speech with slurring, and occasional jerks with strange, disoriented behavior; marked clouding with confusion, in a trance, missing pieces of conversation and wandering; marked clouding, insomnolence with strange feeling, dizziness, increased confusion, purposeless walking around, repeating “yes” to questions and fumbling with clothes [47].
Experiential descriptions are vivid. One patient describes seeing the world through a different medium, and of “not being there,” “not being in the same world as everyone else” [47]. Other descriptions include a “feeling of uncontrollable rush of thoughts and fear of the loss of control of the mind.” One patient described it as “like sitting in a movie”; another description is “as if one were walking through the water of a swimming pool to meet somebody.” One patient was even able to look at a Walter Scott poem without turning the page and yet the next day was able to remember the entire page by heart, having never previously read the poem [47].
The patient may complain of visual hallucinations, go into a dreamy state, and interact in a vague and inappropriate way. Patients may fail to recognize familiar people, and may appear introverted or frankly disoriented. One patient described a feeling of “closeness” or “heat” [47]. Other typical behavioral aberrations include a patient who went to bed with his coat and boots on; at work he could not open his locker and while turning the key complained that he could not get his truck started. This patient put two cups into an empty dishwasher and ran it without detergent, took out a cigarette and looked at it in a puzzled fashion, and after a shower was unable to get dressed [78]. Before and after NCSE, his ability to draw a clock face changed markedly (Fig. 20.2). Another patient made coffee twice and put trousers over his pajamas, and one got up in the middle of the night to tell his wife that he was driving to work and promptly drove into a stop sign [47].
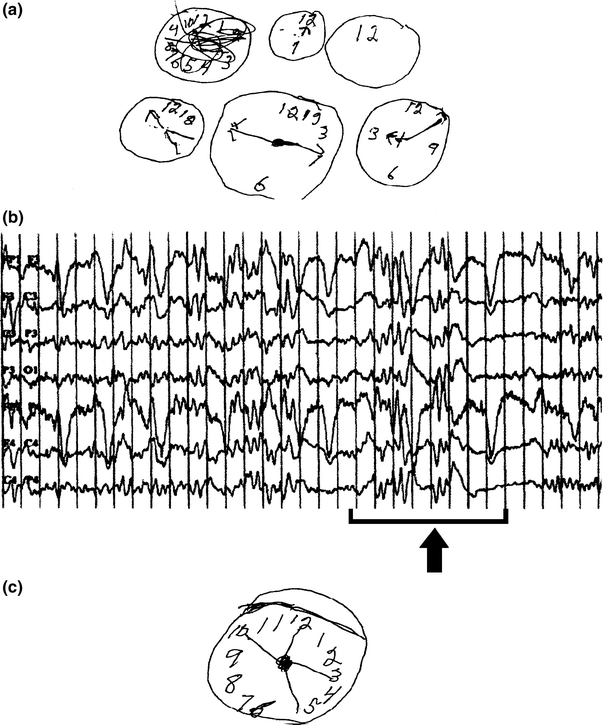

Fig. 20.2
a Patient’s effort to draw the face of a clock during nonconvulsive status epilepticus (NCSE) with EEG as seen in 2B. b EEG during NCSE showing runs of bilateral, synchronous polyspike-slow-wave complexes. c After treatment of NCSE with lorazepam, patient is able to draw a better clock. From Olnes et al. [78] with permission
TAS may present with aggression, impulsive behavior, agitation, and hostility [45, 52]. Some patients regress to infantile behavior, breaking dishes, scribbling on the walls, putting salt into coffee or milk in the sink, and insulting siblings. Some of this behavior is inappropriate rather than retrogressive [44]. One patient described by Andermann and Robb asked for a telephone number but then proceeded to give his own home address; another turned the water taps on and off [45]. Even amidst apparent confusion, some patients will retain much that takes place and be able to carry on relatively complex activities [45].
Clouding of consciousness can obscure other more typical and, therefore, diagnostic clinical features. Dunne and colleagues [41] described some patients presenting with nausea, vomiting, headache, and visual disturbance, who were later found to be in absence status. Other autonomic symptoms include changes in heart rate and sweating.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree







