and Anthony P. S. Guerrero1
(1)
Department of Psychiatry, John A. Burns School of Medicine, University of Hawaii, 1356 Lusitana St., 4th Floor, Honolulu, HI 96813, USA
(2)
Kapiolani Behavioral Health Services, 1319 Punahou Street, Suite 950, Honolulu, HI 96826, USA
32.2.1 Suicide Attempts
32.2.2 Eating Disorders
32.5 Summary
32.6.1 Family History
32.6.2 Social History
32.6.3 Examination
32.6.4 Questions
32.6.5 Further Questions
The field of consultation-liaison child and adolescent psychiatry is an important and vital sub-subspecialty of both child and adolescent psychiatry and psychosomatic medicine. The leading causes of morbidity and mortality among young people [e.g., accidents, homicide, malignancies, and suicide among youth aged 1–19 years (Hoyert et al. 2006)] suggest that there is much that psychiatrists can potentially contribute to general medical physicians striving to provide the best possible preventive and treatment-oriented care to children and adolescents.
This chapter is intended primarily for the benefit of consultation-liaison psychiatrists who encounter children and adolescents on a general medical service, and secondarily for the benefit of child and adolescent psychiatrists who wish to learn more about the practical aspects of working in and administering a pediatric consultation-liaison service.
32.1 General Principles Relevant to Children and Adolescents on a Consultation-Liaison Service
32.1.1 Preparing for the Pediatric Consultation-Liaison Encounter
Before seeing a pediatric patient, as with any other patient on a consultation-liaison service, it is important to discuss the case with the referring provider so as to have a clear idea of the issues to address in the consultation. Where applicable, one should get an idea of the prognosis of the general medical condition. Because children are usually not legally autonomous, it is advisable (except in unusual circumstances) to ensure that the parents have been informed about, and have agreed to, the consultation. The effectiveness of the consultation-liaison psychiatrist is limited if the initial encounter with the parents is awkward or confrontational merely because they had not been informed that a psychiatric consultation was requested. For the purposes of documenting medical necessity (and, in many cases, for billing purposes), the consultant should ensure that the referring medical team has either written an order for the consultation or documented that a consultation is necessary and therefore being requested.
In the interests of maintaining the most optimal relationships with the system of care surrounding a pediatric patient, the consultant should always remember this advice: there is no such thing as an inappropriate consultation request. Even if the identified patient were to seem fine, every consultation request suggests that someone in the system—whether a family member, health care professional, or other stakeholder—is concerned and therefore potentially able to benefit from a systems-sensitive intervention. In our institution’s consultation-liaison service, we instruct our residents that even though most of us in the consultation-liaison business operate on fixed salaries, we should nevertheless all take the perspective of bright and eager new physicians who are grateful for the privilege to work in the medical center, and who are always pleased to find work that can support their practice. We find that adopting such an attitude improves the overall quality of the consultation-liaison service and, ultimately, the care the patients and families receive.
32.1.2 The Developmental Perspective
The saying “children are not miniature adults” applies just as well to psychiatry as it does to the rest of medicine. Most prominently, children and adolescents are developing physically and cognitively, so it is very important to consider the developmental level of the patient. Although a comprehensive review of child and adolescent development is beyond the scope of this chapter, we review key aspects of development, particularly as they apply to understanding of and adaptation to general medical illnesses.
One key principle is that development is a continuous process that builds on success in earlier stages. The consultation-liaison psychiatrist working in pediatric settings should therefore recognize the potential disruption that medical illnesses may have on normal child development.
Table 32.1 summarizes the key stages of development (predominantly social and cognitive) that may be of particular clinical importance in the context of general medical illnesses. Children’s developmental levels are important to consider when discussing coping with illness (and associated treatments) and death and dying. For example, 6-year-olds may have erroneous (though developmentally age-appropriate) beliefs about human physiology, believing that they can lose all of their blood from a blood draw on injection, in spite of well-meaning reassurances that the pain will not be severe. As another example, 6-year-olds might believe that justice can emanate from inanimate objects, and thus (unknown to their parents or caregivers) blame themselves for a personal illness or otherwise be afraid of reporting symptoms. Older children, in spite of more accurate perceptions about the causation of illness, may still not be able to appreciate all of the mechanisms that lead to illness. Hence, relatively straightforward explanations about the need for certain treatments (including medications) may be most appropriate.
Table 32.1
A summary of the key stages of development
Age | Social development | Cognitive development | Clinical implications |
|---|---|---|---|
4–6 months | Increasing awareness and recognition of people, development of attachment | Potential reactive attachment disorders, failure to thrive if inadequate attention to these issues in the context of general medical illness and separation from family | |
12–15 months | Object permanence | Stranger anxiety; important to consider impact of hospitalization and separation from caregivers | |
3–6 years | Improved separation (the age when children usually start school) | Preoperational thinking; possible “magical” or otherwise erroneous beliefs | If there is ongoing severe separation anxiety, need to consider differential possibilities, for this child’s reactions and emotions are still very much connected to the family’s |
7–11 years | Generally good coping with separation | Concrete thinking | Relatively favorable age for elective surgery |
Increasing ability to be involved in explanations of illness and treatment, though need to adjust to concrete thinking | |||
11–20 years | Challenging authority | Formal operations: morals, ethics, self-control, humanitarian/global concerns | Need to anticipate/address potential impacts on compliance |
May be able to give more detailed explanations of illness and implications |
Beyond just the cognitive understanding of illness, the emotional adjustment to illness is heavily influenced by developmental level. For example, it is likely that a preadolescent who must cope with a physical deformity may be more vulnerable to emotional difficulties, compared to a younger child, who may have a less developed body image, or an older adolescent, who may be more cognitively mature.
In order for children to optimally adjust to issues related to death and dying, they need to understand that death is irreversible, final, inevitable, and causally explained. Children facing death (whether their own or in a family member) at a developmental age earlier than that when these principles are understood are vulnerable to experiencing adjustment difficulties. For example, a child who does not realize that death is inevitable or causally explained may consider death to be a punishment for wrongdoing. Therefore, parents and caregivers often benefit from briefings about how to discuss challenging topics, such as death and illness, in a developmentally appropriate manner, and are often best able to gauge their child’s cognitive development.
32.1.3 The Family and Systems Perspective
Children, both legally and developmentally, are not autonomous beings, and therefore are part of a complex system (whether explicit or not) that includes the family and other professionals involved in the child’s care. While state laws may differ somewhat on the degree to which adolescents can consent to certain aspects of medical care (e.g., related to family planning, sexually transmitted diseases treatment, and substance abuse treatment), most states require parental consent for most types of behavioral health care. Additionally, most child and adolescent psychiatrists would agree that conscientious, systems-sensitive involvement of the family in the care of a child or adolescent (or even adult), whether legally mandated or not, usually constitutes the most optimal clinical care.
Consultation-liaison psychiatrists who are not primarily child and adolescent psychiatrists often wonder what is the best way to approach child or adolescent patients and their family: should the patient be interviewed first, or should the family be interviewed first, or should the patient and family be interviewed together? In our clinical experience, we have found that there is no correct answer to this question. We recommend that (1) the patient and available family at bedside can be introduced to the context of the consultation and then asked about how they would like to proceed; (2) time may be set aside to interview the patient and parents separately (particularly if there are concerns about abuse or other sensitive issues); and (3) a solid biopsychosocial formulation with attention to family and systems perspectives should guide the titration of the amount of time spent with the patient alone, with the parents alone, and with the patient and parents together (for instance, if improving communication between the patient and parents is an important focus of the intervention).
Children and adolescents rarely request psychiatric consultations on their own. The requests for psychiatric assistance and the reporting of psychiatric symptoms are therefore often seen through the lens of the family or requesting health care providers. It is therefore of utmost importance to (1) build and maintain solid working relationships with the health care team (through rounds and other collaborative meetings with pediatric medical, nursing, social work, chaplain, and other staff); and (2) determine why the consultation is being requested, which facilitates deciding which aspects of the system warrant attention and intervention. For example, was it someone other than the child or family who requested the consultation, in which case part of an effective consultation must include directly addressing that person’s concerns. Consultation-liaison psychiatry is the perfect venue to practice the biopsychosocial formulation, which can guide the intervention on multiple levels.
Many requests for consultation arise from concerns about emotional or behavioral symptoms in a parent or other family member involved in the child’s care. These are entirely appropriate reasons to consult psychiatry, since the family is part of the whole system affecting the child’s health. Therefore, while it is certainly appropriate to clarify the intent of the consultation with the referring provider, we recommend against “hassling” the medical team about the fundamental request for help. In such situations, it is important to document the consultations from the perspective that the child is the identified patient, even though observations about the parent or other caregiver may also be included. If a parent or other family member needs follow-up as an identified patient, then this can be part of the recommendation.
Common family-related situations and the potential role for the consultation-liaison psychiatrist are summarized in Table 32.2.
Table 32.2
Common family-related situations and the potential role for the consultation-liaison psychiatrist
Consultation-liaison scenario | Potential tasks for the consultation-liaison psychiatrist | Possible pitfalls to be aware of |
|---|---|---|
Family adjustment (e.g., depression, anxiety, “denial”) to a child or adolescent’s illness | Provide family-oriented support and psychoeducation. | Providing long-term or in-depth care for a specific family member, without making it explicit to the family (or explicit in the medical record) that you have assumed this role, separate from your consultation/liaison role to the identified patient. |
Evaluate for the need for further mental health services for family members, and provide referrals as appropriate. | ||
Educate the medical team on possible emotional reactions to a child’s illness, including what may be initial “denial.” | ||
Not adequately recognizing where what may initially be adaptive “denial” may interfere with optimal medical care and possibly constitute medical neglect. | ||
History or possibility of mental illness (including substance abuse) in the parent and/or other caregiver adult | Evaluate for any acute dangerousness in the parent, or possible abuse/neglect of the child. | Providing long-term or in-depth care for a specific family member, without making it explicit to the family (or explicit in the medical record) that you have assumed this role, separate from your consultation/liaison role to the identified patient. |
Evaluate for the need for further mental health services for family members, and provide referrals as appropriate. | ||
Giving the appearance of having performed a forensic assessment of the adult’s parenting capacity, whereas such a function might better be performed by another mental health provider (using standardized assessment tools and usually affiliated with child protective services). | ||
Possible parental abuse/neglect, including Munchausen-by-proxy | Evaluate for the need for further mental health services for family members, and provide referrals as appropriate. | Providing long-term or in-depth care the parent (see above). Giving the appearance of having performed a forensic assessment of the adult’s parenting capacity, whereas such a function might better be performed by another mental health provider (using standardized assessment tools and usually affiliated with child protective services). |
Assist the team in making referrals to child protective and hospital risk management services, where indicated. | ||
Assist the team in formulating a crisis plan (e.g., with hospital security) where indicated. | ||
Angry, abusive, potentially litigious family | Listen closely to parents’ concerns (including what they are most concerned about with their child’s condition). | Not adequately helping the medical team to avoid unnecessary medicolegal risk via: |
• “Splitting” | ||
Consider all possible reasons for the family’s anger (including factors that may be within the medical team’s control). | ||
• Inappropriate documentation | ||
Evaluate for the need for further mental health services for family members, and provide referrals as appropriate. | ||
Evaluate for the need for other referrals (e.g., domestic violence help). | ||
Assist the team in making referrals to child protective and hospital risk management services, where indicated. | ||
Assist the team in formulating a crisis plan (e.g., with hospital security) where indicated. | ||
• Indiscreet conversation | ||
Failure to thrive | Provide a thorough assessment that considers child variables (e.g., temperamental and other behavioral conditions), caregiver variables, and interactional variables; encourage multidisciplinary approaches. | Failing to recognize the multifactorial nature of failure to thrive or inadequately managing general medical conditions coexisting with psychosocial conditions (see Guerrero, 2004) |
Evaluate for the need for further mental health services for the child or family members, and provide referrals as appropriate. |
32.1.4 Psychopharmacologic Principles
The consultation-liaison psychiatrist in pediatric settings should have basic knowledge of child and adolescent psychopharmacology. Once again, children are not “miniature adults” when it comes to responses to medications. It is important to note that most psychotropic medications are not approved by the Food and Drug Administration (FDA) for children and adolescents. Also, children and adolescents generally metabolize medications differently (usually faster) than adults. Finally, the responses of children and adolescents to medication are such that the risk–benefit profile (for instance, in the case of certain antidepressant medications) may not necessarily be the same as what it is for adults.
Given these differences, it is of utmost importance for psychiatrists treating children and adolescents to engage in solid psychopharmacologic practice, which includes the following:
1.
Clearly defining and monitoring target symptoms (and utilizing collateral information where appropriate)
2.
Carefully considering the existing standards of care and treatments that are best supported by evidence, whether FDA approved or not
3.
Determining and considering the patient’s and family members’ previous responses to medications
4.
“Starting low and going slow” in the titration of the medication
5.
Continuing to raise the dose until one has satisfactorily treated all symptoms, reached the recommended upper dose limit of the medication, encountered side effects that make further titration intolerable, or reached a plateau in improvement or worsening of symptoms with an increase in dose
6.
Following recommended guidelines in monitoring vital signs, other physical parameters, and laboratory values
7.
Recognizing medically ill patients’ potential sensitivity to medication side effects
Table 32.3 summarizes the usual first-line medications and recommended doses for common diagnoses and scenarios encountered in pediatric consultation-liaison psychiatry.
Table 32.3
First-line medications and recommended doses for common diagnoses and scenarios
Condition | Reasonable first-line medications | FDA approval? | Initial dose | Important precautions (should always advise patients on “rare, serious, potentially life-threatening reactions”) | Labs and other physical parameters to monitor | References |
|---|---|---|---|---|---|---|
Acute agitation | Antihistamines | No | Diphenhydramine: For infants over 20 pounds and older children: 5 mg/kg/day divided q6 h, up to 50 mg per dose (po, IM, IV) Hydroxyzine: 2 mg/kg/day divided q6 h, up to 25 mg per dose (po, IM) | Avoid diphenhydramine if there is delirium or if there is risk of anticholinergic toxicity | Allen et al. (2001) Green (1995) Johnson (1993) | |
Aggressive behavior refractory to treatment of the primary disorder, aggressive behavior in autism, and psychotic disorders | Atypical antipsychotics | Risperidone: >5k >13 for psychosis Aripiprazole >6, >13 for psychosis Olanzapine >13 for psychosis Paliperidone >12 for psychosis Quetiapine > 13 for psychosis | Olanzapine: 2.5 mg daily (po, IM) Quetiapine: 12.5 mg daily (child) 12.5 mg bid (teen) (po) Risperidone: 0.25 mg daily (<20 kg) 0.5 mg daily (≥20 kg) (po) | Weight gain, metabolic syndrome, extrapyramidal symptoms | Fasting blood sugar and lipids at baseline and every 6 months, Abnormal Involuntary Movement Scale every year Consider baseline electrocardiogram for ziprasidone | Blair et al. (2005) Janssen (2006) Pappadopulos et al. (2003) |
Attention-deficit hyperactivity disorder (ADHD) | Stimulants | Yes | Methylphenidate: 2.5–5 mg daily (po) Dextroamphetamine or amphetamine/dextroamphetamine: 2.5 mg daily (po) | Family history of tics | Tics on physical examination Pulse, blood pressure, height, weight every 3 months or with medication change | AACAP (2002) |
Bipolar disorder | Lithium or valproic acid | Lithium >12 Risperidone >10 Aripiprazole >10 Olanzapine >13 Quetiapine >10 | Lithium: 30 mg/kg/day or according to Weller protocol (po) Valproic acid: 15 mg/kg/day divided bid (po) | Weight gain, metabolic syndrome, hepatic and hematologic effects | Lithium: Baseline CBC, basic metabolic profile with renal function tests, urinalysis, thyroid function, electrocardiogram Valproic acid: Baseline CBC, comprehensive metabolic profile with hepatic function tests Both medications: Medication levels (appropriate to rate of titration) and periodic follow-up labs | Weller et al. (1986) Green (1995) |
Delirium with agitation or psychotic features | Haloperidol Risperidone Olanzapine | No | Oral: 0.01–0.1 mg/kg q12 h IV: 0.005–0.07 mg/kg every 30 min; once stable, use ½ of needed dose divided q12 h. Should not exceed 0.15 mg/kg/day. Risperidone 0.25 mg BID Olanzapine 2.5 mg BID | Vigilance to extrapyramidal symptoms, which children may be more at risk for | Rigidity, tremor, other abnormal involuntary movements Consider baseline and follow-up electrocardiogram to evaluate QTc interval | Lavid and Budner (2000) |
Major depressive disorder | Fluoxetine Escitalopram | Yes, >8 Escitalopram 12–17 | 10 mg per day (po) | Unmasking of mania, akathisia, increase in suicidal thoughts | March et al. (2004) | |
Obsessive-compulsive disorder | Sertraline fluvoxamine Fluoxetine | Yes, Sertraline >6 Fluvoxamine >8 Fluoxetine >7 | Sertraline: 25 mg per day (po) Fluvoxamine: 25 mg qhs (po) Fluoxetine 10 mg per day (po) | Unmasking of mania, akathisia, increase in suicidal thoughts | Fleming (2003) |
Because of the likelihood that patients in pediatric consultation-liaison settings will have general medical comorbidities and may be on other medications, the reader is referred to specific chapters in this book on psychopharmacology in the context of specific general medical illnesses and to tables on drug–drug interactions.
Finally, specific to the pediatric population, we recommend the following “rules”:
1.
Very carefully consider the evidence for medication safety and efficacy in children and adolescents.
2.
One medication is (generally) better than two medications, which is (generally) better than three medications, which is (generally) better than four medications, etc.
3.
Although FDA approval is not necessarily everything, pay attention to the various categories of medications:
(a)
FDA-approved for treating children/adolescents with the condition you are prescribing the medication for (e.g., stimulants for attention-deficit hyperactivity disorder, fluoxetine for major depressive disorder)
(b)
FDA-approved for treating adults with the condition but also approved for treating children/adolescents with a different condition (e.g., valproic acid for pediatric bipolar disorder)
(c)
FDA-approved for treating adults with the condition, and with some evidence for safety/efficacy for children/adolescents with the condition (e.g., certain atypical anti psychotics for pediatric psychotic disorders)
(d)
Not FDA-approved either for the condition being treated or for children/adolescents for any indication
4.
When multiple conditions amenable to psychopharmacologic treatment are possibly present, consider a rough (and potentially modifiable, depending on new evidence) hierarchy of evidence for safety and efficacy: stimulants > serotonin-selective reuptake inhibitors > mood stabilizers > antipsychotics.
5.
Finally, “it’s more than just medication.” Particularly in pediatric settings, where a complex network of people surrounds the patient, it is important to realize that good psychopharmacology depends on various other components, arranged in the form of a pyramid (Fig. 32.1).
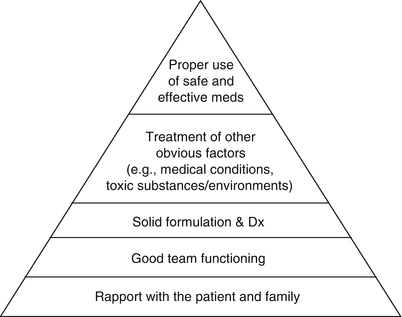

Fig. 32.1
Specific consultation-liaison scenarios that are common and/or high-risk
32.2 Specific Consultation-Liaison Scenarios That Are Common or High-Risk
32.2.1 Suicide Attempts
Suicide attempts or concerns about suicidality are likely to be among the more common concerns presented to a consultation-liaison psychiatrist on a pediatric service (Shaw et al. 2006).
First, it is important to follow whatever policies exist in the medical center regarding the management of patients who are suicidal or potentially suicidal. For many medical centers, doing so includes assigning a risk level (e.g., low, moderate, high) and implementing orders appropriate to the assigned risk level. The orders may address the following areas:
Psychiatry consultation—optional or mandatory
Whether or not the patient may leave the unit, and if so, under whose supervision
Allowed clothing (e.g., hospital clothing)
Patient/room search for dangerous articles
Allowed visitors
Need for 1:1 staff supervision
Frequency of nursing checks
Next, while keeping close contact with the referring medical team and nursing staff, the consulting psychiatrist should seek opportunities for crisis intervention where appropriate. As suggested previously, the psychiatrist, particularly when working with children and adolescents, should ask, “Why did this crisis happen now, on this day, at this time of day?” and “What are all of the biologic, psychological, and social stressors that led to this crisis?” The answers to these questions often help determine what should be done to resolve the crisis. Examples of common precipitating factors are shown in Table 32.4.
Table 32.4
Common precipitating factors of suicide attempts
Biologic | Psychological | Social | |||
|---|---|---|---|---|---|
Factors | Potential interventions | Factors | Potential interventions
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

| ||
