Fig. 1
Overnight polysomnograms of two separate OSA patients. (a) Trunk supine position-dependent OSA: the apneas are primarily related to the position of the trunk. (b) Clusters of apnea are related to the position of the trunk, but also periods without any apnea in this position are seen
However, quite often one encounters hypnograms with a clear clustering of apnea/hypopnea events without this straightforward relationship to supine or another body position. Often, a cluster of apnea/hypopnea events may start or cease abruptly without seeing a change of body position or sleep stage (Fig. 1b).
This observation was the basis for some additional investigations in our sleep clinic. In this we looked at several aspects of current practice of measurement of body position.
Ultimately, this led to a study in 300 subjects in whom we recorded both the position of the trunk and of the head. The results of this study will be discussed to demonstrate the importance of head position, separately of trunk position, in patients with position-dependent OSA [1].
How to Measure Body Position During Polysomnography of Suspected OSA Patients?
In literature, no clear research-based guidelines are found on the technical aspects of recording body position. There are no reports on how to attach the position sensors to the body of the patient to achieve the most reliable position detection and recording. One might think that the frequently observed discrepancy between apnea/hypopnea clustering and body position is due to artifacts from the position-sensor data or is caused by sensor displacement during the night.
We set out to investigate this matter more into detail. Firstly we looked at the position sensor. The position sensor we use is an electromechanical one, mainly based on the displacement of a small mercury droplet within the sensor in different orientations due to gravity. The sensor generates five discrete output voltage levels corresponding to five different sleep positions; left, right, supine, prone and upright, with a threshold angle of ±10° from the 45° position boundary. The position sensor should reliably reflect the orientation of the sensor relative to the direction of gravity. This was assured by regularly checking and calibrating the sensors. Also position output was checked by turning over the patient when the sensors were attached. Of additional importance is that sensor characteristics remain stable throughout the night. Potential confounders are slow drifts in the output of devices based on acceleration sensors. The electromechanical type we used should not be prone to this problem. The recorded voltage levels are digitized by the polysomnographic device and stored in a raw data file on the computer as a sequence of numbers. Numerical analysis of these data files demonstrated a good reproducibility and did not show significant overnight drifts or possibly confounding spurious sensor output signals.
The second step of our investigation focused on the fixation of the position sensor on the trunk. In our center, we use a polysomnography system with a separate position sensor connected by wire to the recording device. To exclude sensor displacement, the position sensor was taped directly to the chest of the patient at the lower part of the sternum. At this location, under normal circumstances, the body surface is fairly horizontal when the patient is lying supine. Also, the lower part of the sternum has the least possible amount of subcutaneous tissue, which minimizes possible movement of the sensor relative to the rigid underlying structures of the trunk (Fig. 2). To assure a reliable readout, the surface of the bed was kept horizontal overnight.
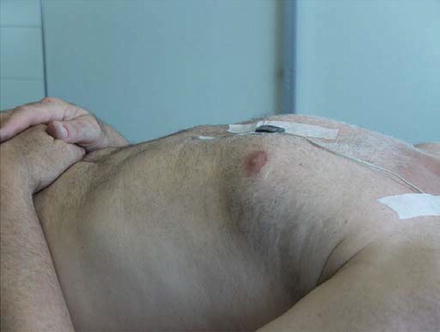

Fig. 2
Location of the trunk position sensor
All patients were also checked at the end of the overnight recording session to exclude position sensor dislocation. This procedural refinement did show a more consistent recording of trunk position. Also in a number of patients, it was verified that there was a good correspondence between position sensor indicated position and that visually observed by overnight video surveillance. With these procedural refinements, we are quite confident that the position recording faithfully reflects the position of the trunk of the patients under investigation.
However, despite our efforts at procedural optimizations, we still regularly encountered hypnograms with clusters of apnea/hypopnea, without any clear relation with the recorded body position or sleep stage.
One could hypothesize that the position of the trunk is not the only important factor for having a position-dependent OSA. The position of the head could additionally affect the appearance of respiratory events in some OSA patient. We investigated this more specifically.
How to Measure Head Position?
In literature also, no studies are found on the most reliable recording methods of head position in patients suspected of OSA. The diagnosis of position-dependent OSA is commonly related to the position of the trunk only. This is also because the vast majority of polygraph systems can record only one position parameter. To investigate head position in addition to the trunk position, we performed polysomnogram recordings with dual position sensors. The position sensor on the trunk was attached to the sternum as described previously. An identical sensor was taped directly to the skin in the middle of the forehead, just above the eyebrows (Fig. 3). This location is approximately horizontal when the head lies in supine position.
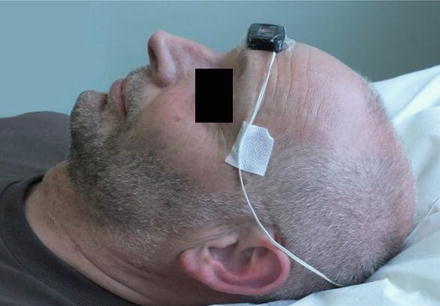

Fig. 3
Location of the head position sensor
To make sure this position readout gives the correct values, patients were asked to sleep with a single pillow (Fig. 4). It was assured that this setup could reliably detect visually observed lateral rotation of the head during sleep, with or without rotation of the trunk. A limitation is that our type of sensor does not allow a continuous recording of the exact angle of lateral rotation. It only detects rotation of more than 45° to the left or right.
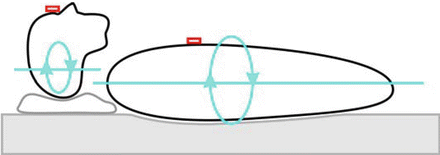

Fig. 4
Schematic representation of our dual-rotation recording setup
The electromechanical sensor on the forehead could potentially also record flexion and extension. However, because of the detection thresholds, only major flexion and extension movements may be detected. Such large flexion-extension movements are not likely to occur during sleep lying supine with the head supported by a single pillow. Recording of flexion-extension movements would require a more elaborate setup. Also, because the trunk-neck-head complex does not have a single flexion-extension rotation axis. In the most simplified form, one might use a model with two rotation axes (Fig. 5). The figure illustrates that a “neutral” head position may occur in very different postures of the neck.
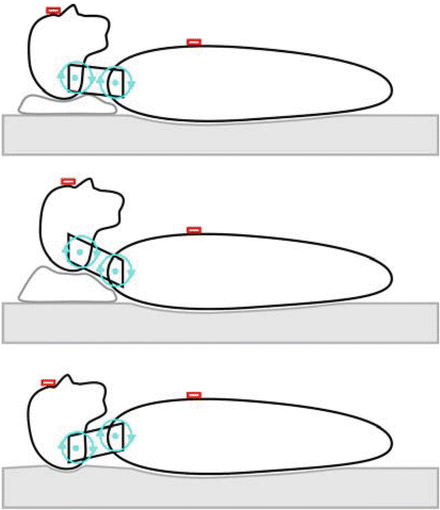

Fig. 5
Schematic representation of freedom of movement in flexion-extension
Ideally, one would also record lateroflexion of the neck and the orientation of the mandible relative to the skull.
How to Combine Head and Trunk Position Analysis?
As we were limited in our technical means, the focus of our investigation was aimed primarily at lateral rotation of the head, and not at flexion-extension. The standard software we used for generating the hypnograms from the recorder data does not allow analysis of multiple position data channels at the same time. However, the recording device did allow simultaneous recording of the output of an additional position sensor at a separate recording channel. The data from each recording channel was transferred to a separate digital computer data file. During analysis, we could choose which position data file to use. Thus, two overnight polysomnograms were constructed: one employed the data from the trunk position sensor and the other employed the data from the head position sensor. All other hypnographic data channels and parameters remained the same.
The setup described allowed us to assess two hypnograms using either head position data or trunk position data but not the interaction between the two. To achieve this, we synthesized a new position data file from the head and trunk data which reflected all possible combinations of head and trunk position. This was subsequently again entered into the standard analysis process.
Study Setup
To explore the effect of trunk and head position on the AHI, we conducted a study on 300 consecutive adult subjects (>18 years). The group consisted of 227 men (with a mean age of 50 years and an average BMI of 28.7) and 73 women (with a mean age of 49 years and an average BMI of 32.2). Subjects were referred to our department because of clinically suspected OSA and underwent overnight polysomnography. From overnight polysomnograms, the AHI in different positions was determined, and the effect of the trunk and head position on the AHI was investigated. All subjects gave informed consent for participation in this study. Respiratory events were scored according to the AASM 2007 criteria [8]. Sleep stages were scored by using the standard criteria of Rechtschaffen and Kales [9]. Automated hypnogram analysis results were manually reviewed by an experienced sleep investigator.
Firstly, the patients with an AHI > 5 were identified as having OSA.
Secondly, OSA patients who spent >5 and <95 % of the total sleeping time in supine position, based on the trunk position sensor readout, were further analyzed for position dependence. Position dependence was defined as an overnight AHI in supine position (determined for both the trunk position sensor and the head position sensor) at least twice as high as AHI in non-supine positions [1, 2, 4]. Since we used two position sensors, this led to four possible classifications: both trunk and head supine dependent, only trunk supine dependent, only head supine dependent, and not supine dependent.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree






