CSF-like Parenchymal Lesion(s)
Anne G. Osborn, MD, FACR
James D. Eastwood, MD
DIFFERENTIAL DIAGNOSIS
Common
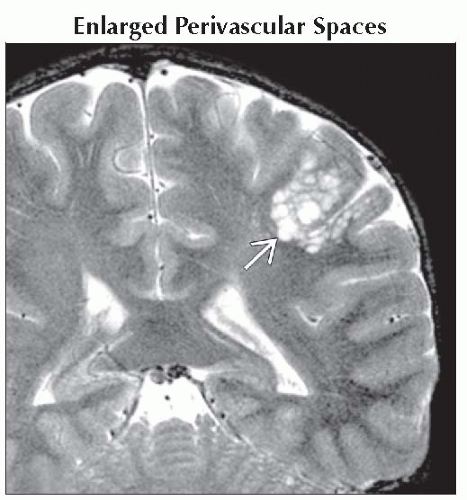
Enlarged Perivascular Spaces
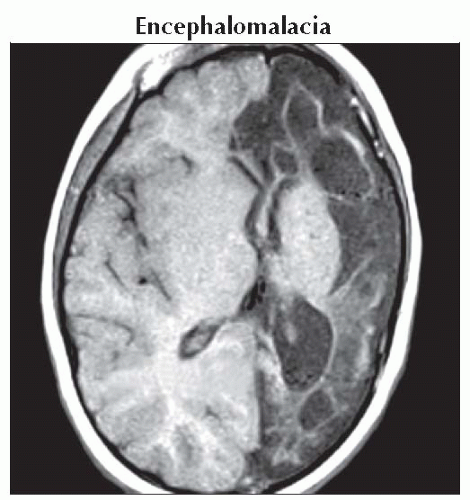
Encephalomalacia
Lacunar Infarction
Neurocysticercosis
Less Common
Porencephalic Cyst
Multiple Sclerosis
Normal Variant
Hippocampal Sulcus Remnants
Connatal Cysts
Rare but Important
Neuroglial Cyst
Cryptococcosis
Parasites, Miscellaneous
Mucopolysaccharidoses
Germinolytic Cysts
Miscellaneous Congenital Malformations
ESSENTIAL INFORMATION
Key Differential Diagnosis Issues
Key imaging questions
Does lesion follow CSF on all modalities/sequences?
Is there any mass associated effect?
Does lesion enhance?
Included
CSF-like cystic mass(es), e.g., enlarged perivascular spaces, neuroglial cysts
Excluded
Cystic neoplasms, abscess, resolving hematoma (rarely exactly like CSF)
Developmental cysts that do not behave exactly like CSF (e.g., epidermoid, neurenteric cysts)
Helpful Clues for Common Diagnoses
Enlarged Perivascular Spaces
Perivascular spaces (PVSs)
Can be seen at all ages but ↑ with age
Filled with interstitial fluid but follow CSF on all sequences
Most have no abnormality in surrounding parenchyma on PD/FLAIR
≈ 25% have thin hyperintense rim
Bilateral > unilateral
Multiple > solitary
“Clusters” of variably sized CSF-like cysts characteristic
Can occur anywhere but most common locations = basal ganglia, hemispheric white matter, midbrain, dentate nuclei
Variant (mostly in elderly) = “état criblé” (“cribriform state”) with multiple tiny cysts in basal ganglia (BG)
Encephalomalacia
Etiology varies (trauma, infarction, etc.)
Can be solitary, multifocal, multicystic
CSF-like ± adjacent FLAIR hyperintensity
Lacunar Infarction
Solitary or multiple
Typically along single long unpaired penetrating arteries &/or vascular watershed zones
BG, thalamus, white matter (WM) common
Multifocal BG infarcts + surrounding gliosis = “état lacunaire” or “lacunar state”
Neurocysticercosis
Most neurocysticercosis (NCC) cysts are actually in sulci
Cysts in vesicular stage smooth, thin-walled, with scolex generally visible as “dot” within cyst
Multiple lesions in mixed stages common
Some enhance, some do not
Ca++ (multiple = “starry sky” pattern)
Helpful Clues for Less Common Diagnoses
Porencephalic Cyst
Communicates with ventricle &/or pial surface
Does not enhance
Multiple Sclerosis
Chronic “burned-out” lesions
Appear as CSF foci with hyperintense rinds on FLAIR/PD
Look for faint hyperintensity surrounding lesions on T1WI (“lesion within a lesion”)
Do sagittal FLAIR or T2WI to look for other lesions along callososeptal interface
Hippocampal Sulcus Remnants
“String of beads” cysts medial to temporal horns of lateral ventricles
Developmental variant, incidental
Remnants of vestigial primary embryonic hippocampal sulcus
Imaging
Connatal Cysts
Single or multiple
Location
Intra- or periventricular (may actually be cysts of anterior choroid plexus)
Small cyst adjacent to tip of frontal horn may be normal anatomic variant
Lined with ependyma
Present at birth
Usually transient
Occasionally seen in older patients
No septations, no hemosiderin
Generally isolated without associated abnormalities
Helpful Clues for Rare Diagnoses
Neuroglial Cyst
Nonenhancing CSF-like cyst
No surrounding signal abnormality
Does not communicate with ventricle
Subcortical WM, choroidal fissure common sites
Cryptococcosis
Nonenhancing gelatinous pseudocysts in perivascular spaces (PVS)
Multifocal > > solitary lesions
Most patients have HIV/AIDS
Parasites, Miscellaneous
Other than NCC, parasitic brain cysts uncommon
Hydatid cyst = large nonenhancing unilocular cyst
Mucopolysaccharidoses
Multiple, bilateral
Dilated PVSs in deep periventricular WM
Germinolytic Cysts
Periventricular/subependymal cysts
Cyst(s) along caudothalamic groove probably result from germinolysis
Glial (not ependymal) lined cysts/pseudocysts resulting from germinolysis
Distinguish from “connatal” cysts (intraventricular anterior choroid plexus cysts)
Many etiologies, including inherited metabolic disorders (e.g., Zellweger, infantile Refsum), congenital infections (CMV)
CSF-like; ± septations, hemosiderin; do not enhance
Look for associated abnormalities
Leukoencephalopathy
Delayed myelination
Polymicrogyria, pachygyria, heterotopias
Miscellaneous Congenital Malformations
Several have parenchymal CSF-like cysts as part of syndrome
Van der Knaap leukoencephalopathies (megaloencephalic leukoencephalopathy with subcortical cysts, anterior temporal lobe cavitations)
Congenital muscular dystrophy (cerebellar cysts common, may represent dilated perivascular spaces)
Image Gallery
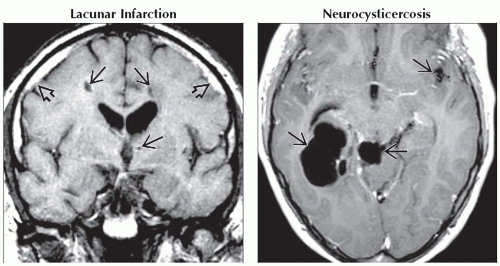 (Left) Coronal T1WI MR in an elderly patient with bilateral chronic subdural hematomas
 shows multiple lacunar infarcts shows multiple lacunar infarcts  in white matter, basal ganglia. (Right) Axial T1 C+ MR shows several nonenhancing CSF-like cysts in white matter, basal ganglia. (Right) Axial T1 C+ MR shows several nonenhancing CSF-like cysts  of variable sizes in a patient with NCC. Several may be cisternal, invaginating into brain. (Courtesy E. Bravo, MD). of variable sizes in a patient with NCC. Several may be cisternal, invaginating into brain. (Courtesy E. Bravo, MD).Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|