CHAPTER 13 DISORDERS OF SMELL AND TASTE
The “chemical” senses of smell and taste are the human organism’s means of qualitatively analyzing the chemical composition of its immediate environment. Although impairment of smell or taste is not generally perceived to be as disabling as impairment of sight or hearing, hyposmia (impaired olfaction) or hypogeusia (impaired taste) may nevertheless cause substantial loss in quality of the esthetic and hedonistic aspects of the individual’s life, may contribute to comorbid conditions such as poor nutritional intake in the elderly, and, uncommonly, may be an early sign of a serious underlying disorder.1 Unpleasant smells or tastes may trigger recognition of toxins in food or the environment not otherwise detectable by the other senses. Smell via pheromones is an important component of courtship and mating in the life cycles of other species but to a far lesser extent in Homo sapiens, which is not known to possess a vomeronasal organ or a discrete pheromonal system.2 Loss of olfaction or gustation may go relatively unnoticed by the patient; in other cases, a perceived hypersensitivity of the chemical senses or inappropriate activation of sensory pathways may be the cause of symptoms.
DISORDERS OF SMELL
Aspects of the Anatomy and Physiology of Olfaction
The primary sensory neurons of the olfactory pathway continuously die and are continuously replaced, being generated from the basal cells of the olfactory epithelium.3 The ciliated olfactory neurons have a lifespan of between 30 and 60 days3 and can be regenerated after damage or loss.4 The olfactory epithelium secretes mucus, which bathes the sensory dendritic surface of the olfactory neurons and provides a medium to dissolve odorants. Odorant signal transduction occurs through binding to G protein–coupled olfactory receptors, of which about 350 forms occur in humans. As might be expected, congenital genetically based specific anosmias (for certain odorants) have been reported, analogous to various forms of color blindness (see Hawkes, 2002). The bipolar olfactory neurons constituting the first cranial nerve pass through the cribriform plate of the ethmoid bone and synapse in the olfactory bulb, within glomeruli, with second-order afferent neurons. Considerable convergence and information processing occur within the olfactory bulb and tract.5 Significant inhibitory and interglomerular innervation occurs within the bulb3 and is believed to modulate afferent excitatory transmission even at this level. Significant bilateral communication occurs at multiple levels within the olfactory pathways, beginning from the anterior olfactory nuclei (which are collections of neuronal bodies lying posteriorly within the olfactory tracts) and extending to the thalami and cortical olfactory areas. In humans, neurons of the olfactory tracts terminate, without synapse in the thalami, in regions collectively termed the primary olfactory cortex (lateral olfactory gyrus, piriform cortex, and periamygdaloid areas). These sites subsequently project to the hypothalamus, limbic structures, entorhinal cortex, and other areas. A minority of relays project through the dorsomedial nucleus of the thalamus. Olfactory and other areas of cortex in turn project centrifugally back to the olfactory bulbs and may modulate feedback inhibition or facilitation of afferent stimuli. Finally, the trigeminal nerve is also important in the perception of smell, mediating tactile, noxious, and pain stimuli in the nasopharynx and associated structures.6
Clinical Approach to Olfactory Disorders
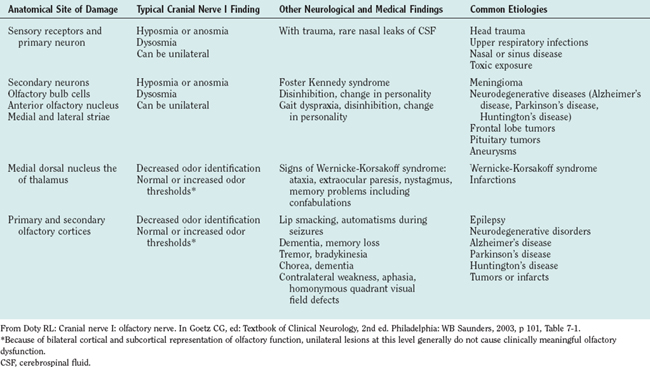
Neurological disorders of olfaction can be conveniently approached according to symptom presentation (anosmia or hyposmia; hyperosmia or dysosmia), anatomical site of dysfunction (Table 13-1), or etiology (Table 13-2).7 A careful history and examination usually allow the clinician to make a provisional diagnosis and target subsequent investigations. Upper respiratory tract infection is the most common cause of neural olfactory dysfunction, accounting for up to 33% of cases. However, in up to 40% of patients with olfactory dysfunction, no cause for their symptoms is found.8
TABLE 13-2 Causes of Olfactory Disturbance
Neurodegenerative disorders (especially Parkinson’s disease, dementia with Lewy bodies, Alzheimer’s disease) |
AIDS, acquired immunodeficiency syndrome; HIV, human immunodeficiency virus.
History
The nature of the olfactory abnormality, its temporal course, and its variation with differing stimuli should be clarified as precisely as the patient’s recall, cognitive state, and descriptive abilities allow. Dysosmia refers to a general distortion of smell sense, whereas troposmia refers to distortion in quality of a particular normal smell stimulus. Whether the smell concerned is pleasant, unpleasant, or excessively unpleasant (cacosmia) may be important. Complaints of nasal discharge or unilateral epistaxis are suggestive of an upper airway abnormality. Traumatic head injury is an important cause of smell and taste disorders and may account for up to 23% of cases of documented hyposmia.9 Intracranial surgery likewise may cause hyposmia. Any variation of intensity with a particular stimulus or scent, particular hyperosmia, should be noted. The possibility of pregnancy should be considered in the female patient of childbearing potential with hyperosmia or dysosmia.10 The medical history and drug history may reveal use of agents known to impair olfaction (Table 13-3). A history of smoking, alcohol consumption, and recreational drug use should be documented.11 The medical history may be notable for sinusitis or other rhinal disease,12 thyroid or other endocrine disease, hepatic or renal impairment, Parkinson’s disease13 or other neurodegenerative conditions,14 stroke, or features such as deafness or diabetes that are suggestive of a mitochondrial dis order. Association of a smell, particularly a strongly unpleasant or noxious one, with a period of amnesia, loss of awareness, or other suggestive symptoms, can indicate a focal seizure disorder.15 The patient may perceive an odor when no stimulus is present (phantosmia). A history from an observer can prove invaluable in this circumstance. Olfactory hallucinations are an uncommon manifestation of schizophrenia, being noted in approximately 6% of patients.16 A family history may also yield clues in regard to any of these conditions. Other important points include occupational or other exposure to toxins or fumes, past treatment with radiation, the psychiatric history, and past intracranial or systemic infection, including human immunodeficiency virus infection.17 Congenital hyposmia is known to be associated with immotility or absence of olfactory epithelial cilia, most commonly in association with hypogonadotropic hypogonadism (Kallman’s syndrome).18 Headache or other symptoms suggestive of an enlarging intracranial mass or of frontal region dysfunction may herald a progressive frontal, temporal, or anterior fossa tumor. It should be remembered that a significant decline in olfactory acuity is seen with aging, particularly in the sixth and seventh decades.19 Quality-of-life questionnaires have been developed to try to reproduce reliably the largely subjective perception of olfactory dysfunction.1
TABLE 13-3 Drugs That May Impair Olfaction or Gustation*
< div class='tao-gold-member'> Only gold members can continue reading. Log In or Register to continue
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|