(1)
Neurosurgical Department, Friederiken-Hospital, Hannover, Germany
11.1 General Considerations
Focal nerve lesions due to trauma are relatively rare diseases we have to deal with. The following chapter is therefore quite short. Most nerve trauma is associated with bone fractures or distortions of joints (Fig. 6.8). These injuries are characterized by enormous traction forces which cause long-distance damage to the nerve trunk. Elastic intraneural elements indeed allow resistance against these forces until a certain level is reached. Then the nerve disrupts, and the nerve stumps retract a few centimeters to proximal and distal. Due to axonal re-growth capacity, the proximal stump turns to develop a neuroma, whereas the distal stump gets left behind with intraneural fibrosis. However, fibrosis also occurs in the proximal nerve segment above the neuroma. Therefore, most trauma cases end in large nerve gaps after resection of the entire scar segments so that the term “focal” no longer fits. You will find supporting and detailed modern imaging findings in these cases by means of high resolution ultrasound and magnetic resonance in Sects. 6.1.6, 6.1.7, 6.1.8, 6.2.3 and 6.2.4.
It is entirely owing to Sunderland and his classification of nerve lesions in five degrees that we have an accurate impression of the possible types of structural damage and subsequent recovery potentials. For further details and references, please refer to Sect. 3.1. In addition, it is owing to Millesi that today we have an exact knowledge of the different types of intraneural soft tissue reactions which, secondarily can hinder the re-growth capabilities of nerve fibers. For further details and references concerning this field, please refer to Sect. 3.2.
In contrast to frequent and extended nerve disruptions, short distance lesions can for instance result, from a thrust with a knife, injury with a piece of broken glass, or a bite from a dog. Such injuries leave behind a circumscriptive trauma, and no physician can immediately differentiate whether the nerve remains in continuity or whether it is disrupted. Theoretically, nerve damage from grades I–V of Sunderland’s classification could have happened following one of the above-mentioned injury causes.
In previous decades, two alternative treatments were offered to patients:
1.
Subsequent exploration of the nerve lesion under general anaesthesia, neurolysis or nerve repair depending on the intra-operative findings
2.
Wait for certain period of time so that we can test the behaviour of the axon sprouts exclusively by eliciting the Tinel sign (see also Sect. 4.1)
Palpation and percussion of the affected nerve trunk at different points enables to trigger an electric current-like pain that the patient describes in the sensitive area which previously belonged to the distribution of the injured axons. The maximum trigger point will coincide with the location of the maximum number of out-growing axon sprout ends. If this point of triggering moves downward during two different investigations, axonal out-growth is proven and can be estimated as a positive prognostic factor. If such a trigger point remains at the same level, the physician has to assume that fibrosis is blocking axonal out-growth, and that a neuroma has developed. Unfortunately, the time span between nerve injury and potential or expected regeneration signs in previously paralysed muscles often lasts for several months. electrodiagnostics are consequently rather useless during this period, because re-innervation signals can only occur when axon sprouts have arrived at muscle end plates. For details please refer to Sect. 5.6.
Because of today’s abilities in high resolution ultrasound imaging demonstrated in Sects. 6.1 and 6.2, we are increasingly optimistic of improving on the time span just described. We are hopeful that new experience in these easily available techniques will help us in future to indicate neurolysis or nerve repair early enough when it is necessary, and to avoid surgery when it proves unnecessary. The timing of decision making influences the quality of regeneration. Muscle fibers which do not receive nerve signals undergo atrophy which is said to start becoming irreversible after 6–12 months, although different opinions exist today concerning this question [1, 2]. Nevertheless, the general opinion is that the prognosis for nerve regeneration and recovery essentially improves the earlier nerve repair starts.
11.2 Surgical Considerations
Even during surgical exposure with aid of magnification by microscope, it still remains difficult to determine whether or not nerve fascicles are intraneurally in continuity. In any case, our surgical goal is that remyelination and re-growth of nerve fibers start, and that this process again reaches muscle end plates. The affected nerve segment is presented as thickened and hardened (Figs. 8.8, 8.9, 8.13 and 9.9). Under magnification we can longitudinally incise the epineurium in intact and neighbouring parts of this nerve segment. After this step, the external sheath of the epineurium can be partially removed so that several groups of fascicles come into view. These fascicle groups can be slightly separated from each other, a surgical step that now facilitates an approach to the damaged nerve segment. Nerve trauma results in histo-pathologically determined reactions of the connective nerve tissue, a process called fibrosis. If epineurotomy, epineurectomy, and interfascicular neurolysis as stepwise procedures succeed in overcoming the injured nerve segment, prognosis of recovery improves significantly. Circular compressing forces due to fibrosis hinder re-growth of axons. Our efforts aim at reducing such a barrier. By means of intra-operative nerve action potentials (NAP), the surgeon can now examine possibly preserved nerve fiber function. A healthy nerve segment is stimulated proximal to the lesion, and action potentials are deduced from a nerve segment distal to the lesion. The method is entirely credited to Kline and Hudson [3]. In the meantime, quite a new additional approach exists involving applying high resolution ultrasound directly onto nerve fascicles during the operation. However, further experience of centers will be necessary to determine exactly whether fascicle continuity is preserved either in the nerve trunk, or at least in certain nerve sectors [4].
As already mentioned in Sect. 7.1, pure entrapment syndromes predominantly need slight decompression only. However, if a circumscriptive trauma has happened in the patient’s history, and if the patient then presents a pre-operative severe loss of function with deteriorated or lacking electrical conductivity, the surgeon must consider a nerve exposure which really needs microsurgical neurolysis. However, we must then take into account the plexiform structure of nerve trunks. Separation of fascicle groups destroys cross connections between them, followed by small neuroma after a period of time. This procedure can result in a painful nerve lesion in the patient’s future. The surgeon bears the whole responsibility and must decide during the operation how far to enter into the nerve and between different fascicles. The stepwise neurolysis should be stopped immediately when fascicles seem to expand under the microscope. Responsibility is high insofar as re-operations carry a high risk of making things worse. Perhaps more experience in intra-operative ultrasound will help in future to assess the type of lesion before microsurgical steps are started. For further details of this feature, please refer to Sects. 6.1.7 and 6.2.7.
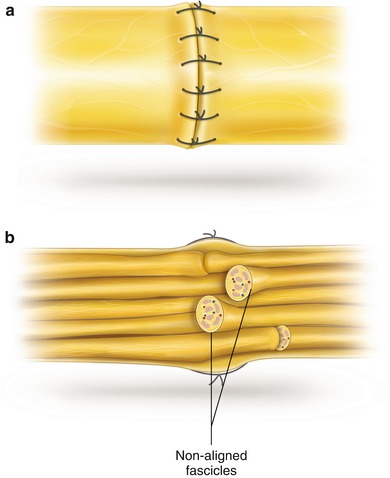
Rare focal injuries can induce such a fibrosis and, despite preserved nerve continuity, nerve fiber re-growth can end in a neuroma in continuity, in other words, in a grade IV lesion from Sunderland’s classification (see also Figs. 6.7 and 6.18). Such a situation needs the removal of the altered nerve segment or parts of it and repair of nerve continuity by means of grafts. Information on the consequences and microsurgical techniques of modern nerve repair is mainly due to the work of Millesi et al. [5, 6]. However, attention should be paid to the fact that the first nerve repair by means of autologous skin nerve grafts had already been successfully carried out in 1916 by Foester [7, 8]. Nevertheless, during a period of about 40 years, the development of nerve reconstruction unfortunately completely stagnated, despite this pioneer report. As an explanation, we have to consider that only a macro-surgical view of nerve structures was current. Surgeons tried to overcome the usual difference in caliber between the injured nerve trunk and a small nerve graft by introducing so-called “cable grafts”. In order to achieve the caliber of nerve trunks, skin grafts were glued together or wrapped in a segment of an artery or vein so that the cable turned out to have the same diameter as the nerve trunk. These cables resulted in a central necrosis because the central sector remained unnourished. Because of its unsatisfactory results, end-to-end suture of the disrupted nerve trunk stumps was more and more preferred over “cable grafts” (Fig. 11.1). Extremities were then immobilised over weeks in a flexed position. As just mentioned, it is now owing to the work of Millesi et al. that the significant disadvantages of these historical techniques have been realized, and that our theoretical concepts have completely changed. The microstructure of nerve tissue has become well known. However, even though microsurgical techniques had been introduced in peripheral nerve surgery by 1963 [9], it was more than another decade before Millesi’s results could finally prove the accuracy of these concepts (Fig. 11.2) [6]. According to them, the quality of nerve fiber growth and final recovery depends on the following basic preconditions: