ANI
HIV-associated asymptomatic neurocognitive impairment
Cognitive impairment involving at least two cognitive domains (performance of at least 1 SD below the mean for norms on neuropsychological tests)
1. The cognitive impairment does not interfere with everyday functioning
2. The cognitive impairment does not meet criteria for delirium or dementia
3. There is no evidence of another pre-existing cause (like depression or substance abuse)
MND
HIV-1-associated mild neurocognitive disorder
Cognitive impairment involving at least two cognitive domains (performance of at least 1 SD below the mean for norms on neuropsychological tests)
1. The cognitive impairment produces at least mild interference in daily functioning (at least one of the following):
i. Self-report of reduced mental acuity, inefficiency in work, homemaking, or social functioning
ii. Observation by knowledgeable others that the individual has undergone at least mild decline in mental acuity with resultant inefficiency in work, homemaking, or social functioning
2. The cognitive impairment does not meet criteria for delirium or dementia
3. There is no evidence of another pre-existing cause for the MND
HAD
HIV-1-associated dementia
Marked cognitive impairment involving at least two cognitive domains (performance of at least 2 SD below the mean for norms on neuropsychological tests)
1. The cognitive impairment produces marked interference with day-to-day functioning in work, home and social activities
2. The marked cognitive impairment has been present for at least 1 month
3. The pattern of cognitive impairment does not meet criteria for delirium (e.g., clouding of consciousness is not a prominent feature); or, if delirium is present, criteria for dementia need to have been met on a prior examination when delirium was not present
4. There is no evidence of another, pre-existing cause for the dementia (e.g., other CNS infection, CNS neoplasm, cerebrovascular disease, pre-existing neurological disease, or severe substance abuse compatible with CNS disorder)
Concerns on the above classification are pointed towards the category of asymptomatic neurocognitive impairment (ANI) in which only one test is required to fulfil the diagnostic criteria even though two tests are recommended for assessing each cognitive domain. This translates to 20 % of cognitively normal HIV-positive individuals being misclassified as having ANI as a result of many confounding factors; a major one being the definition of functional impairment. Gisslén et al. [16], have cautioned on the applicability of this classification and argued its modification as being warranted. For patients with HAD there is marked acquired impairment in cognitive functioning, involving at least two ability domains. Typically the impairment is in multiple domains, especially in learning of new information, slowed information processing, and defective attention/concentration [10, 17]. Table 4.1 summarizes the criteria for HAND classification.
Pathogenesis of HIV-Associated Neurocognitive Disorders, HAND
The direct effect of the HIV virus on the body is on the cellular immune system through depletion of infected CD4 lymphocytes [18]. The effects on the neurological system are through a similar mechanism of attack of brain macrophages and the production of neurotoxins which subsequently damage the brain neurons. Among untreated patients with HIV dementia, there is a close association with the inflammatory response and CSF viral load [19]. Figure 4.1 summarizes the pathogenesis for HAND [20].
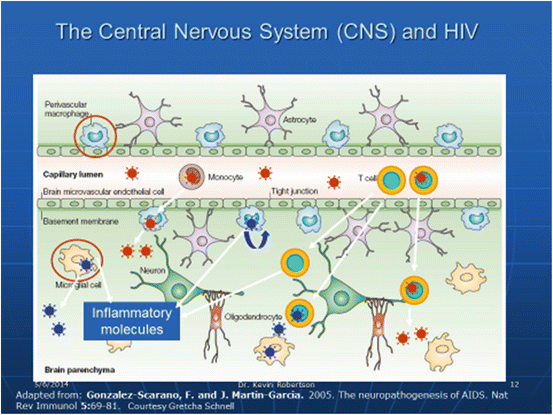

Fig. 4.1
HIV infection of CNS cells
HIV-Associated Cognitive Impairment: Evidence from Studies in Uganda
The prevalence of neurocognitive impairment associated with HIV has been considerably researched in Uganda. The initial prevalence among ART naïve individuals found at 31 % has increased to 41 % in more recent years in the population with higher CD4 counts [3, 14]. The greatest risk for the impairment has been older age and female gender [2, 11]. When tested over time, the initiation of cART contributed significantly to improvement in neurocognitive function in the short term though when followed up over a longer period of time there seems to be no difference among individuals who are on cART versus those who are not especially if they had moderate immunosuppression [2, 6]. Significantly noted in longitudinal studies among HIV positive individuals with cognitive impairment are the persistent high scores for depression symptoms even after an improvement in the neuropsychological functions tests of research participants. This underscores the importance of HIV effects on the brain and the need to have such conditions appropriately screened and treated once identified [21].
There are mainly two common subtypes of HIV clades in Uganda i.e. clade A and clade D. Among patients with advanced immunosuppression, clade D subtype showed an association for neurocognitive impairment [22]. However, there was no difference in the frequency of HIV dementia by clade subtype among those with moderate immunosuppression [3] and no association with compartmentalization between the cerebrospinal fluid and peripheral blood [3].
The double jeopardy of having HIV and psychosis or other opportunistic infections have been confirmed by Nakasujja et al. [7] who found that HIV positive individuals were almost three times more likely to be cognitively impaired on the Mini Mental State Examination (MMSE) as well as on the following cognitive tests: WHO-UCLA Auditory Verbal Learning Test, Verbal Fluency, Color Trails 1 and Color Trails 2. Even when the psychosis cleared the impairment remained higher for the HIV positive group [23]. Similarly, patients that had opportunistic infections like cryptococcal meningitis and had significant short-term neurocognitive impairment improved markedly on treatment with cART over the first 12 months [24].
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree





