Fig. 1
Hunt and Kosnik grade
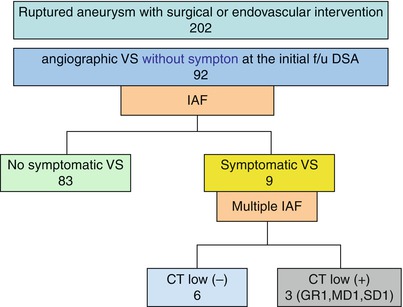
Fig. 2
GOS at discharge
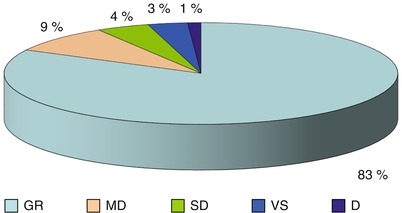
Fig. 3
Number of patients
Discussion
We previously reported the effectiveness of IAF by measuring cerebral circulatory dynamics, as determined by cerebral angiography performed before and after IAF [3]. We found that that the time to peak opacification and the time to half-peak opacification were significantly reduced in the proximal portion of the middle cerebral artery in the early arterial phase after intra-arterial administration of fasudil hydrochloride, and that the time to peak opacification was significantly reduced both in the distal portion of the middle cerebral artery in the late arterial phase and in the transverse sinus in the venous phase. IAF induced dilation of the proximal arteries and improved cerebral microcirculation in patients with vasospasm. We also reported that IAF was clinically safe and effective treatment for patients with vasospasm following SAH [4]. In this study, only three patients (3.2 %) of 92 patients treated with IAF for angiographic vasospasm without ischemic symptom had evidence of ischemic lesion caused by vasospasm on CT at discharge. IAF performed before presentation of symptomatic vasospasm could improve outcome in patients with SAH. IAF for patients with angiographic vasospasm may prevent further progression of vasospasm.
Conclusion
IAF therapy was safe and effective for patients with vasospasm following SAH. Prophylactic IAF therapy may prevent symptomatic vasospasm.
Conflict of Interest Statement
The authors have no personal financial or institutional interest in any of the drugs, materials, or devices in the article. All authors have registered online Self-reported Conflict of Disclosure Statement Forms through the website for the Japan Neurosurgical Society members.






