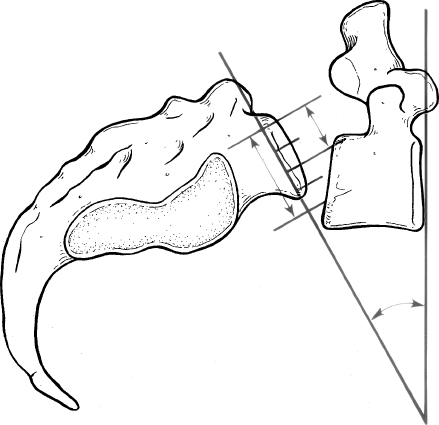
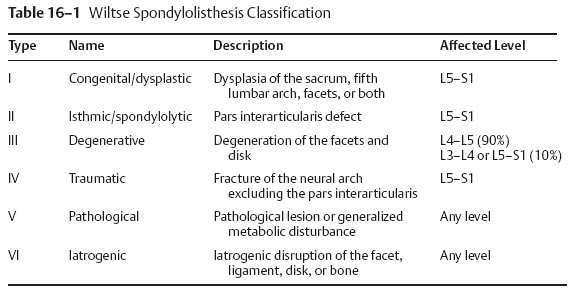
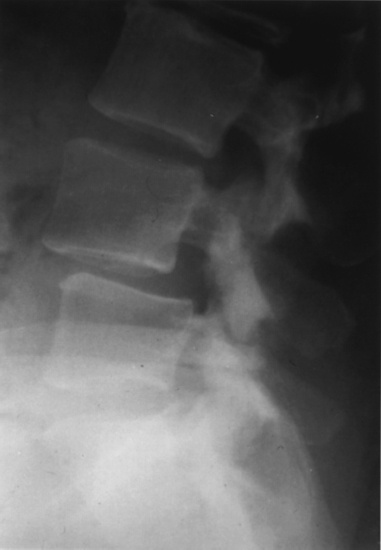
IV 18 Kyphotic Spinal Deformities in Children and Adults I. Introduction A. Definitions 1. Spondylolisthesis—displacement of one vertebra on another 2. Spondylolysis—lytic defect in the pars interarticularis a. Bone between the superior and inferior articular processes II. General considerations A. Hereditary factors 1. Familial tendency is stronger in dysplastic type (94%) compared with isthmic type (32%). 2. More common in white males (6.4%) than black females (1.1%) a. Higher incidence among Eskimo population (up to 45%) 3. Association with spina bifida of the sacrum and dysplastic changes of the bony elements in high dysplastic types B. Epidemiology 1. More common in men than women 2. Higher incidence among football players, female gymnasts, and soldiers carrying heavy backpacks 3. Lower incidence among nonambulatory patients III. Biomechanics A. Abrupt change in stiffness across the lumbosacral junction 1. Pars interarticularis is strong but susceptible to fatigue fractures a. Especially with extension injuries 2. Shear stress at the pars can be increased by flexion contractures of the hip and secondary hyperlordosis a. Pincerlike effect on L5 pars from the superior articular process of S1 and inferior articular process of L4 IV. Classifications A. Modified Wiltse (Table 16–1) B. Classification of spondylolisthesis (Marchetti—Bartolozzi) 1. Developmental a. Deficient “bony hook,” anatomic abnormalities of the L5 pedicle, pars, inferior facets (1) High dysplasia (a) Severe bony anomalies with significant kyphosis (b) Common during 7 to 20 years of age (c) Compensatory lumbar hyperlordosis (2) Low dysplasia (a) Slower progression (b) Frequently asymptomatic (c) Disk degeneration aggravates the motion segment instability. (3) Acquired (a) Traumatic (acute versus chronic stress fractures) (b) Postsurgical (c) Pathological (d) Degenerative (e) Specific entities (modified Wiltse classification) 2. Congenital or dysplastic (14%) a. Epidemiology (1) Displacement occurs early (a) Typically during the adolescent growth spurt (b) Two-to-one female:male ratio (c) Genetic component (a) Increased risk among all affected first-degree relatives b. Etiology (1) Congenital or dysplastic abnormality of the L5–S1 facet joint (a) Prevents proper articulation (b) Displacement is early but limited based on the intact posterior neural arch. (a) Increased rate of neurological symptoms (25 to 35%) (2) Pars interarticularis is intact but poorly developed or elongated. c. Clinical findings (Fig. 16–1) (1) Pain radiating into lower extremities (a) Little or no back pain (2) Cauda equina d. Treatment (1) Most congenital spondylolisthesis patients with progression of the slip require decompression and arthrodesis 3. Isthmic spondylolisthesis a. Epidemiology (a) Most common spondylolytic disorder among children and young adults (a) Common from 7 to 20 years (b) Onset usually coincides with adolescent spurt, and progression occurs between 10 and 15 years of age. (2) Most common at L5 over S1 vertebrae (95%) (3) Most often asymptomatic (a) Low back pain and radiculopathy (L5 nerve root) may develop. b. Clinical findings (1) Restricted forward flexion of the hips and back (2) Tight hamstrings (3) Flat buttock (vertical sacrum) (4) Lumbosacral kyphosis (5) Compensatory lordosis (6) Anterior protrusion of the pelvis (7) Pelvic waddle gait c. Roentgenographic findings (1) Defect at the pars interarticularis (a) Seen at neck of “Scottie dog” projection on oblique view (2) Grades (Meyerding or Taillard) and slip angle (3) Trapezoidal L5 vertebral body (a) Rounded sacral dome (i) On an anteroposterior (AP) view, this appears as the reverse “Napoleon’s hat” sign. (4) CT scan shows the pars defects and stenosis (i) Single-photon emission computed tomography (SPECT) can detect metabolic activity in the region of the pars interarticularis defect. (5) Magnetic resonance imaging (MRI) is the study of choice for as sessing spinal stenosis. (a) May demonstrate “wide canal sign” (i) Suggestive of a bilateral pars defect (6) Radiographic measurements (a) Meyerding classification (i) Grade I—0 to 25% slip (ii) Grade II—26 to 50% slip (iii) Grade III—51 to 75% slip (iv) Grade IV—76 to 100% slip (v) Grade V-Spondyloptosis or > 100% slip (b) Slip angle (Fig. 16–2) (i) Angle of kyphosis is measured as the angle between the superior end plate of L5 and a line perpendicular to the posterior border of the sacrum. (ii) Most sensitive indicator of potential instability (iii) Correction of the slip angle is the most important goal of surgical reduction. (*) Correction of slip is not important in achieving clinical success. (**) In high-grade spondylolisthesis, an interbody may help achieve reduction. (c) Lumbar index (i) Measurement of the wedging of the anterior L5 vertebral body (*) Ratio of the anterior/posterior height of the slipped vertebrae
Deformity
16
Lumbar Spondylolisthesis
Neupsy Key
Fastest Neupsy Insight Engine