CHAPTER 54 MANAGEMENT OF STATUS EPILEPTICUS
Known case reports of epilepsy date as far back as the 16th century, but the term status epilepticus was first noted in the English language in 1868 in Bazire’s translation of Trousseau’s Lecture on Clinical Medicine1,2: “The status epilepticus is characterized, not by a single attack, but by a series of attacks … the stupor which succeeds the convulsions lasts from ten minutes to three-quarters of an hour at most. But before the stupor has passed away another attack, exactly similar to the first, supervenes, and is confounded with it. Now, as the third stage of an epileptic fit is not usually regarded as distinct from the convulsive stage, the patient seems to be still in a fit, although his comatose condition is only an effect of the fit. He has not therefore got over the disturbances caused by the first attack before a second occurs, then a third, a fourth, a fifth; and in proportion to the recurrence of the fits the cerebral congestion increases, the apoplectic coma is prolonged, and extends over a period varying from two to twenty-four hours, and after a time the patient does not recover his senses at all …” Although the basic definition of status epilepticus has not changed significantly over time, the understanding of the pathophysiology, etiology, and particularly treatment since the initial advent of the bromides has dramatically evolved. This chapter focuses on these aforementioned concepts, with particular emphasis on the advances in treatment of status epilepticus.
DEFINITION
Status epilepticus is defined as continuous seizure activity lasting more than 30 minutes or two or more sequential seizures without full recovery of consciousness between seizures.3 However, most physicians agree that treatment should not be withheld if the manifestation does not conform to this 30-minute definition. Thus, new operational definitions, such as those by Lowenstein and colleagues, define generalized convulsive status epilepticus (GCSE) in adults and older children (>5 years old) as 5 minutes or more of continuous seizures or two or more discrete seizures between which there is incomplete recovery of consciousness.4
CLASSIFICATION
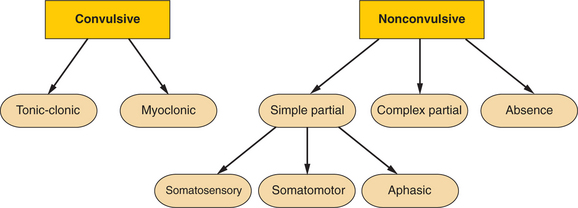
Many different complicated classification schemes for status epilepticus have been proposed. In general, status epilepticus can be defined on the basis of electrographic onset—specifically, partial versus generalized—or on clinical grounds (convulsive versus nonconvulsive) (Fig. 54-1). All forms of partial status epilepticus, such as complex partial status epilepticus, are classified clinically as nonconvulsive.
The most common form of status epilepticus is GCSE and consists of tonic and/or clonic motor activity. This motor activity may be symmetrical or asymmetrical and clinically overt or subtle. There is associated alteration of consciousness and bihemispherical, generalized, ictal discharges (which maybe asymmetrical) on the electroencephalogram (EEG).5 If GCSE is allowed to progress, convulsive activity may become less apparent and clinical manifestations more subtle. Thus, the term subtle generalized convulsive status epilepticus has been used to denote twitching movements of the face, eyelids, trunk, and distal extremities or nystagmoid movements of the eyes in association with bilateral ictal discharges on EEG.6
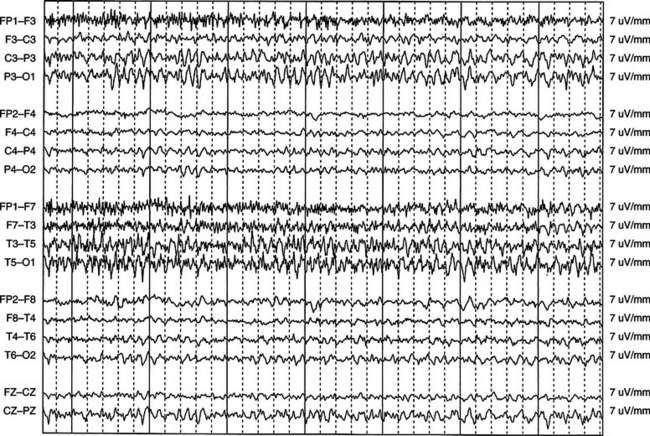
Complex partial status epilepticus (Fig. 54-2) has the most varied clinical manifestation. Although the prevailing constant is the definite impairment of consciousness and very localized electrographic seizures, the extent of the impairment can be variable, ranging from mild alteration of consciousness with or without automatisms, waxing and waning confusion, and agitation with near-psychotic behavior to complete stupor.7–10
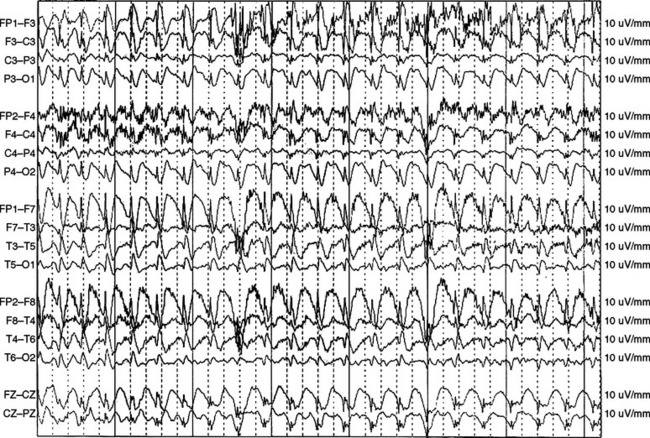
Absence status epilepticus is considered a nonconvulsive form of the condition and is often categorized as either typical or atypical absence status epilepticus. Both types are associated with paroxysms or loss of consciousness of abrupt onset and offset. However, typical absence status epilepticus is characterized by the hallmark 3-Hz spike-and-wave discharges on EEG (Fig. 54-3), a normal interictal background, and normal neurological examination findings. Atypical absence status epilepticus usually occurs in patients with underlying neurological dysfunction (Lennox-Gastaut syndrome) and is characterized by diffuse slow spike-and-wave discharges (<3 Hz) and an abnormal interictal background.11 Whatever the form, absence status epilepticus typically occurs more often in children and adolescents than in adults.
Myoclonic status epilepticus as defined by Gastaut11 is divided into two subgroups. The first group includes primary generalized epilepsy characterized by massive bilateral myoclonic jerks that occur at irregular intervals and by preservation of consciousness. This is a rare form in comparison with the second group, which occurs in secondary (symptomatic) generalized epilepsy in children and is associated with alteration of consciousness. Examples of this second group include myoclonic-astatic epilepsy, Lennox-Gastaut syndrome, and epilepsy with myoclonic absences.12 In addition, there is a separate category of myoclonic status epilepticus that occurs in nonepileptic patients with acute or subacute encephalopathies.11 This category includes degenerative encephalopathies such as dyssynergia cerebellaris myoclonica of Ramsay Hunt, progressive myoclonic epilepsy, Lafora’s disease, and various toxic and metabolic (liver, renal insufficiency) encephalopathies.12
Myoclonic status epilepticus caused by anoxic encephalopathy has not been regarded as status epilepticus in the strictest sense11; however, some authorities have argued5 that this symptomatic myoclonic syndrome should instead be considered a subtle form of GCSE.12
Simple partial status epilepticus includes somatomotor, somatosensory, and aphasic status epilepticus. Somatomotor status epilepticus can occur during or at the onset of a somatomotor partial epileptic seizure (somatomotor simple partial status epilepticus in the strictest sense)11,13 or herald the presence of a metastatic embolus or asymptomatic sylvian or suprasylvian infarction in elderly persons.11,14 Ictal discharges are usually more pronounced in the rolandic area with definite preservation of consciousness.11 A well-known type of somatomotor status epilepticus is epilepsia partialis continua (Kojewnikoff’s epilepsy), characterized by segmental myoclonus between seizures. Lastly, somatomotor simple partial status epilepticus can accompany severe brain lesions in nonepileptic persons and is characterized by proximal limb or truncal myoclonus repeated approximately once per second in conjunction with periodic lateralized epileptiform discharges (PLEDs) on EEG.8 This syndrome occurs almost exclusively in the elderly population and most often represents a watershed infarct or, less frequently, metastatic tumor or brain contusion.11,15,16
Somatosensory status epilepticus is very rare and may in fact be residual activity after surgical resection of the primary epileptogenic area in medically refractory epilepsy.13
Aphasic or dysphasic status epilepticus is less frequent than somatomotor status epilepticus, but it is well documented in the literature.17–22 This syndrome is characterized by aphasia (either receptive or expressive), sometimes in association with alexia and agraphia, lasting from seconds to days.
One special situation that deserves mention is simple partial status epilepticus in the context of hyperosmolar nonketotic hyperglycemia. Simple partial motor seizures can accompany medical symptoms such as polydipsia and loss of appetite. Osmolar values can be as high as 320 mmol, and in this situation, the use of phenytoin is contraindicated because of its inherent ability to exacerbate hyperglycemia.13
INCIDENCE, ETIOLOGY, AND MORTALITY
Multiple case series and large hospital-based retrospective studies of GCSE are noted in the literature.23–35 However, the true incidence of status epilepticus is not well defined, for multiple reasons, including clinically missed cases, variability in reporting, and inherent differences between populations. In initial hospital-based reports, Hauser31 estimated an annual incidence of 50,000 to 60,000 cases of status epilepticus in the United States. However, in a more recent prospective population-based study of status epilepticus,36 a higher U.S. incidence was estimated, approximately 100,000 to 150,000 patients with at least one episode of status epilepticus per year, according to extrapolation from community population data in Richmond, Virginia. Several retrospective and fewer prospective studies have been performed, and although methods of reporting and subpopulations of case studies are variable, a few generalizations can be drawn.
First, the incidence of status epilepticus appears to be highest at the extremes of age: the young (1 to 12 months of age) and the elderly (>60 years of age).36,37 Recurrence, however, appears most common in the pediatric population.36 The Richmond study36 revealed a recurrence rate of 35% in the pediatric population versus 7% and 10% in the adult and elderly populations, respectively. Second, the major etiology for status epilepticus in the pediatric population overall appears to be systemic non–central nervous system infections.36 In adults, low antiepileptic drug levels, temporally remote symptomatic lesions (particularly cerebrovascular accident), and acute stroke accounted for the majority of cases.38 Thus, stroke, whether acute or subacute/chronic, accounted for 61% of cases of status epilepticus in the elderly population in the Richmond study.36 Third, the overall rate of mortality from status epilepticus appears to be approximately 15% to 22% in adults25,27,28,36 but much lower in children (5% to 11%).24,26,29 Fourth, death from status epilepticus is intricately linked with etiology, age, and duration of status epilepticus. Anoxia and hypoxia were much more common causes of status epilepticus in adults than in the pediatric population and were associated with the highest rates of mortality.36 The mortality rate is higher for status epilepticus lasting longer than 60 minutes (nearly 20%) than for status epilepticus lasting 30 to 59 minutes (<5% respectively).28
PHYSIOLOGICAL CHANGES IN GENERALIZED CONVULSIVE STATUS EPILEPTICUS
Acute Systemic Complications of Generalized Convulsive Status Epilepticus
Acute systemic effects of GCSE include cardiovascular alteration, acidosis, respiratory distress, hyperthermia, and renal failure secondary to rhabdomyolysis (Table 54-1). These physiological alterations occur in essentially two phases.39 Initially, the early phase of GCSE is characterized by sympathetic overdrive,40 but after 30 minutes, failure of homeostatic mechanisms causes initial physiological alterations to normalize or even move in the exact opposite direction.39
TABLE 54-1 Systemic Physiological Changes in Generalized Convulsive Status Epilepticus
The most significant and most life-threatening changes occur within the cardiac system. Initially systemic hypertension predominates, along with tachycardia.41 Mean arterial blood pressure is elevated as a result of increased vascular resistance. However, later on, relative hypotension occurs, secondary to failure of splanchnic and renal constriction.42–44 Mortality is associated with the development of life-threatening arrhythmias in nearly 60% of patients with GCSE.45
Hyperthermia seen early on in GCSE in animal studies is not only associated with significant cerebellar damage but is also responsible for ischemic injury in outer cortical layers and hippocampus.46,47 Studies by Liu and associates48 in experimental rat models (kainic acid–induced seizures) demonstrated that decreasing temperature to 28° C decreased status epilepticus by 50%, and further reduction to 23° C abolished status epilepticus entirely. Increasing temperatures to 42° C uniformly resulted in death within 2 hours. Of most importance, decreasing temperature to 28° C prevented hippocampal cell loss, emphasizing the need to treat hyperthermia aggressively at the onset of status epilepticus.48
Derangements in blood chemistry are also seen. The natural occurrence of lactic acidosis is secondary to anaerobic metabolism in the setting of repetitive muscle activity from ongoing convulsions. Hyperglycemia occurs in the setting of increased levels of circulating catecholamines and exacerbates existing acidosis. Thus, supplemental glucose should be given only if true hypoglycemia exists.42,59
Respiratory changes include central apnea and pulmonary edema secondary to increased intravascular pressures within the pulmonary vasculature.43
Other systemic changes that may occur in GCSE include peripheral leukocytosis and possible rhabdomyolysis secondary to muscle injury from repetitive convulsions, producing subsequent acute tubular necrosis and possible renal failure.50
Central Nervous System Physiological Changes
Essentially, the central nervous system changes reflect the eventual difficulty of the brain in keeping up with the ongoing metabolic demands induced by GCSE. Initially, cerebral blood flow increases profoundly to supply the brain with the necessary glucose and oxygen.51 However, late in status epilepticus (hours after onset of seizure activity), breakdown of the body’s homeostatic mechanisms (cerebrovascular autoregulation) occurs.46 In addition, mean arterial pressure starts to fall, which causes further drop in cerebral blood flow.51,52 An eventual mismatch between elevated cerebral metabolism and insufficient cerebral blood flow (supply/demand mismatch) occurs. As lactate accumulates, brain glucose levels decline47 and, in combination with decreased oxygenation at later stages of status epilepticus, contribute to ongoing hypoxia and anoxia.53
PATHOPHYSIOLOGY OF NEURONAL INJURY
The aforementioned systemic alterations can contribute to neuronal injury, but the primary mechanisms leading to ongoing seizures and neuronal injury are at the cellular level. Although an eventual cerebral supply/demand mismatch occurs in the later stages of GCSE, neuronal injury occurs within 60 minutes.46,52 The combination of decreased γ-aminobutyric acid (GABA) neurotransmitter–mediated inhibition and abundance of glutamate excitation can lead to neuronal injury. Normal excitatory synaptic neurotransmission is essentially altered. Under normal circumstances, glutamate binds to postsynaptic non–N-methyl-D-aspartate (NMDA)–type glutamate receptors after its release from the axon terminal. This promotes sodium flow into the cell and produces depolarization, which results in further propagation down the axon. However, in the case of status epilepticus, when glutamate binds to the postsynaptic NMDA receptor, the usual self-limited depolarization does not occur. Instead, prolonged depolarization occurs, because the magnesium ion that generally blocks the NMDA channel pore is displaced.42,53 Thus, calcium ions flow into the cell, causing intracellular accumulation of calcium, which leads to cell necrosis and apoptosis.42 Because NMDA receptors are located primarily in the limbic system, neuronal cell loss thus results in hippocampal injury.42
MANAGEMENT AND TREATMENT OF STATUS EPILEPTICUS
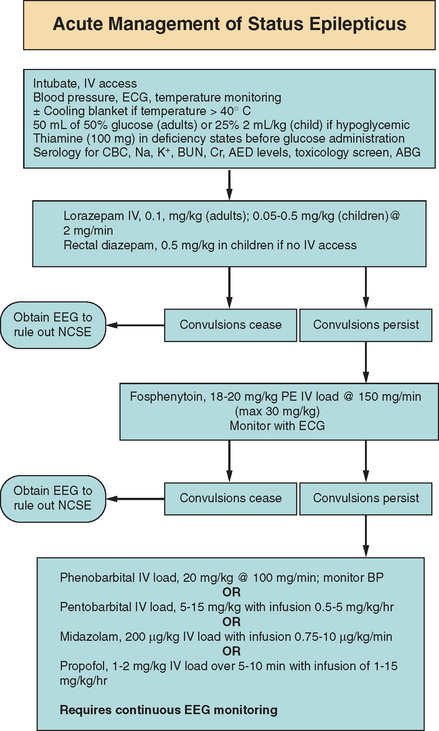
The goal with any acute medical emergency is the timely diagnosis, management, and treatment of the problem. The longer the duration of status epilepticus, the more subtle the motor manifestations,54 the later the electroencephalographic stage (impairing adequate detection of the syndrome),55 and the more refractory to pharmacological treatment the seizures will be54,56 (Fig. 54-4).
Management is essentially divided into two sections: immediate general concerns to prevent the ongoing systemic complications described previously and specific pharmacotherapy to abort ongoing seizures. In general, the ABCs (airway, breathing, and circulation) of any acute medical problem should be addressed. A clear airway for the adequate passage of air is needed with availability of immediate endotracheal intubation if required. If ongoing convulsive motor activity causes hypoventilation, a paralytic agent may be needed temporarily to support respiration and prevent the patient from injuring himself or herself. Peripheral access also needs to be addressed immediately in order to initiate intravenous medication and provide fluid resuscitation if needed. Two large-gauge intravenous catheters, or even a central catheter if peripheral access cannot be obtained, should be in place. Blood pressure, the electrocardiogram, and temperature should be monitored. Hypotension should be avoided, and agents to support blood pressure may be required temporarily. If significant hyperthermia develops (>40° C), a cooling blanket may be necessary to stabilize body temperature.57 Once the airway, breathing, and circulation are secure, blood chemistry profiles should be drawn for potentially reversible causes or exacerbating factors of status epilepticus. Fingerstick blood glucose should be tested, and 50 mL of 50% glucose bolus injection for adults and 2 mL/kg of 25% glucose for children should be administered if hypoglycemia exists. A glucose bolus should also be administered if hypoglycemia is suspected and a blood glucose level cannot be established in a timely manner. Thiamine (100-mg bolus) should be administered in individuals suspected of thiamine deficiency (e.g., alcoholic patients) before or simultaneously with glucose administration to prevent precipitating acute Wernicke’s encephalopathy. Blood samples should be analyzed for complete blood cell count, metabolic profile (sodium, potassium, blood urea nitrogen, creatinine, calcium, magnesium), antiepileptic drug levels if applicable, urine/serum toxicological levels, and arterial blood gases.
The benzodiazepines, phenytoin, and phenobarbital have been used as first-line agents for aborting status epilepticus. The rationale for use of these agents for first-line therapy is the direct result mainly of four pivotal studies.58–61
Leppik and colleagues61 compared lorazepam with diazepam for the initial treatment of status epilepticus; 78 patients received either 10 mg of diazepam or 4 mg of lorazepam. No significant difference in terminating status epilepticus (58% with diazepam versus 78% with lorazepam) or latency of action (2 minutes for diazepam and 3 minutes for lorazepam) was noted.61 In 1988, Shaner and associates,59 in a randomized clinical trial, compared the efficacy of the combination of diazepam and phenytoin with phenobarbital alone in 36 patients with GCSE. Phenytoin was added to the phenobarbital regimen if seizures persisted for 10 minutes or more after therapy was initiated. Although phenobarbital aborted status epilepticus a little more quickly than did the combination, there was no statistical significance in the success frequency between the two treatments.59 However, these two studies paved the way for the Veterans Affairs cooperative trial (randomized, double-blind study)60 in 1998 in which four different treatment protocols were compared in 384 patients with overt (presumably early) status epilepticus and 134 patients with subtle (presumably late) status epilepticus. The four treatment regimens were as follows: (1) lorazepam, 0.1 mg/kg; (2) diazepam, 0.15 mg/kg, followed by 18 mg/kg of phenytoin; (3) phenytoin alone, 18 mg/kg; and (4) phenobarbital, 15 mg/kg. In the patients with overt status epilepticus, the best response (electroencephalographic and clinical termination of seizures within 20 minutes, and no seizure recurrence within 60 minutes, of therapy initiation) occurred in 64.9% of patients who received lorazepam alone, 58.2% of those who received phenobarbital alone, 55.8% of those who received diazepam with phenytoin, and 43.6% of those who received phenytoin alone. In the patients with subtle status epilepticus, overall response was much lower than in the patients with overt status epilepticus. The response rate was highest in the patients who received phenobarbital (24.2%), followed by those who received lorazepam (17.9%) and those who received diazepam and phenytoin (8.3%), and lowest in those who received phenytoin alone (7.7%). No statistically significant difference between recurrence during the 12-hour study, incidence of adverse effects, or 30-day outcome was noted. The authors concluded that lorazepam was more effective than phenytoin as initial intravenous treatment for overt GCSE. Although lorazepam was not found to be more efficacious than phenobarbital alone or diazepam and phenytoin combined, it was found to be easier to use.60 In the most recent randomized, double-blind trial, Alldredge and colleagues58 in 2001 evaluated intravenous benzodiazepine administration by paramedics for the treatment of out-of-hospital status epilepticus. In this trial, 205 patients were randomly assigned to receive intravenous diazepam (5 mg), lorazepam (2 mg), or placebo. Status epilepticus was aborted in 59.1% of patients receiving lorazepam who arrived in the emergency department, in comparison with 42.6% of the diazepam recipients and 21.1% of the placebo recipients. The duration of status epilepticus was also shorter in the lorazepam recipients.