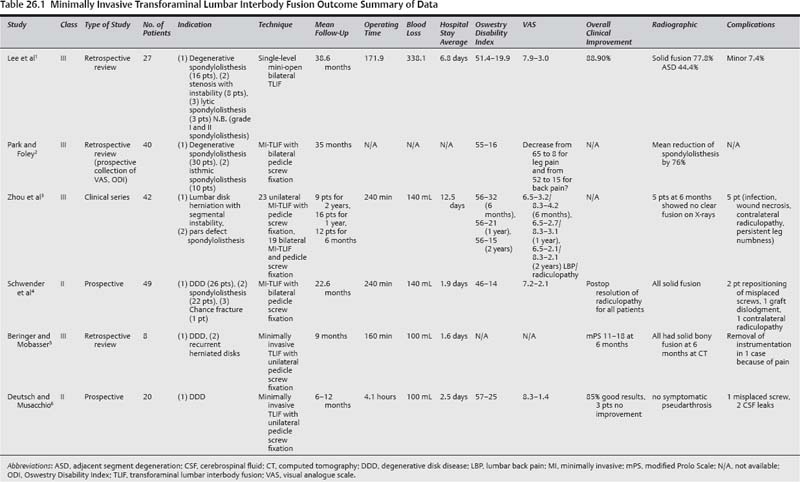
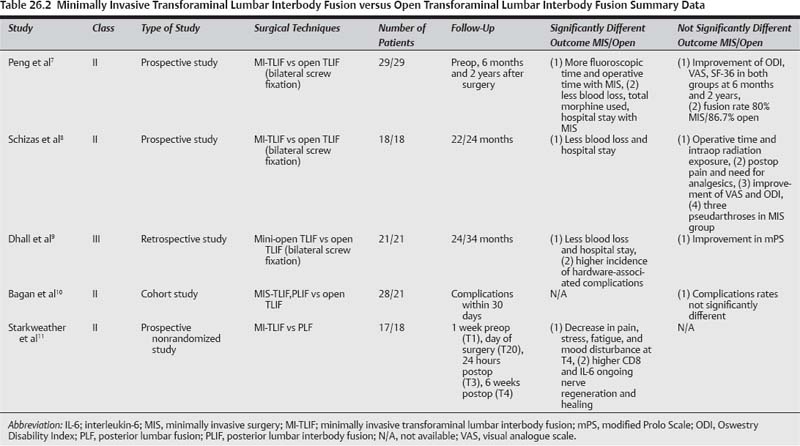
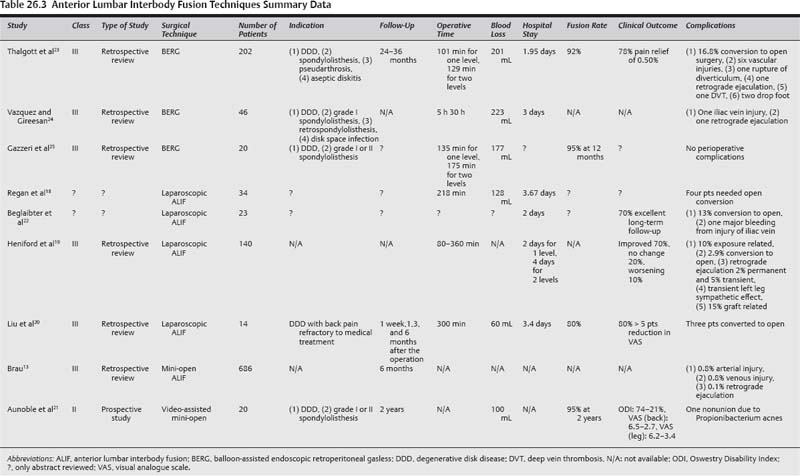
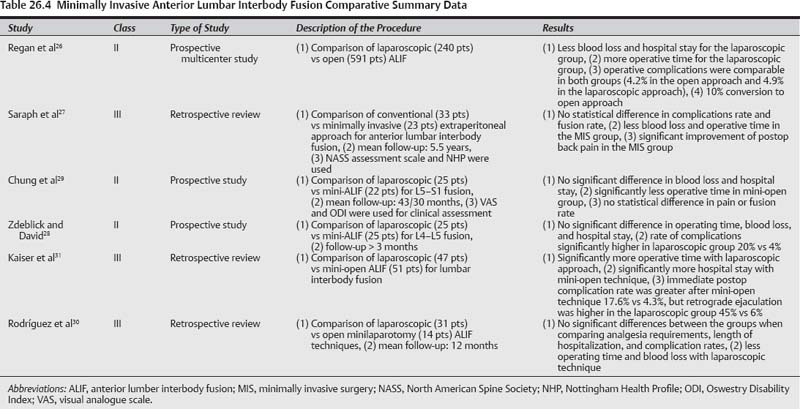
26 Lumbar spine fusions have been performed for ~100 years as a treatment modality for several lumbar spine diseases, including spondylosis, trauma, infection, neoplasm, and spinal instability. The traditional time-honored operation has been a posterolateral fusion with autologous bone graft. With the intent to improve fusion rates as well as to achieve rapid stabilization of the spine, internal fixation with instrumentation and interbody grafts were added progressively using different surgical approaches and techniques. In standard open surgical procedures, long incisions, extensive muscle dissection, and prolonged retraction can result in ischemia and denervation of the paraspinous muscles, increased blood loss, and epidural fibrosis, which can result in prolonged hospital stays and recovery. Therefore, efforts were made to develop minimally invasive techniques and instruments. Minimally invasive techniques for lumbar spine fusion include: minimally invasive transforaminal lumbar interbody fusion (TLIF), minimally invasive anterior lumbar interbody fusion (ALIF), extreme or direct lateral interbody fusion (XLIF or DLIF), transacral approach for Axial Lumbar Interbody Fusion (AxiaLIF), percutaneous pedicle screws, and minimally invasive translaminar facet screw fixation. These techniques have gained popularity over the last decades, and multiple studies have been published emphasizing their benefits, including decrease in tissue damage, preservation of anatomy, decrease in postoperative scarring, potentially shorter hospital stay, earlier patient recovery, equal clinical outcomes, and better cosmesis compared with traditionally open surgery. Over the last decade, TLIF has become a very popular technique to achieve decompression and circumferential fusion of the lumbar spine. It was developed to reduce the risk of neural element retraction and related injury of the standard posterior lumbar interbody fusion (PLIF) technique and to avoid the anterior access to the spine and its associated complications. With the advances of technology, this approach can be performed through a small paramedian incision, avoiding the surgical trauma to paraspinal muscles induced by a standard open technique. It could be done unilaterally, bilaterally, or unilaterally with contralateral percutaneous pedicle screw fixation or translaminar facet screw fixation. Its lateral surgical window access to the spinal canal allows for decompression of the contralateral side. The indications may include spondylolisthesis grade I or II, degenerative disk disease (DDD) with back pain, treatment of pseudarthrosis, and deformity. A PubMed search for “TLIF” and “minimally invasive TLIF” was performed as well as comparative studies1–11 (Tables 26.1 and 26.2). The results of these techniques have been shown to be successful and there appears to be a faster recovery with the minimally invasive technique compared with the traditional open technique. Only two studies compared directly the minimally invasive TLIF with the open TLIF. There are no level I data comparing open versus minimally invasive TLIF procedures. There are two level II studies that compared directly open versus minimally invasive TLIF procedures (Table 26.2). Peng et al published a class II study comparing clinical and radio-graphic outcomes of minimally invasive versus open TLIF.7 Twenty-nine patients in each group were included and were followed 6 months and 2 years after surgery. Operative time and fluoroscopy time were significantly longer in the minimally invasive group (p < 0.05). Blood loss, hospital stay, and morphine used postoperatively were significantly less with the minimally invasive group (p < 0.05). Long-term clinical improvement was similar in both groups, and there was no difference in fusion rates (86.7% for the open group vs 80% for the minimally invasive group). Another prospective comparative study was performed by Schizas et al.8 Thirty-six patients with symptomatic isthmic spondylolisthesis and DDD were treated either with minimally invasive (n = 18) or open (n = 18) TLIF. Blood loss and hospital stay were found to be significantly lower in the minimally invasive group (p < 0.01 and p < 0.05, respectively). There was no significant difference in length of surgery, postoperative pain, visual analogue scale (VAS), and Oswestry Disability Index (ODI) between the two groups. There are no level III data that compare directly the open with minimally invasive TLIF techniques. The literature shows that minimally invasive TLIF is associated with less blood loss, shorter hospital stay, with similar long-term clinical outcomes. Operative time, radiation exposure, and postoperative need for analgesics were controversial. Pearls • Level II and III data showed a good outcome and low complication rates for minimally invasive TLIF technique. • There are level II data comparing directly the minimally invasive versus open TLIF techniques. These showed no significant difference in outcomes and complication rates, but less blood loss and hospital stay for the minimally invasive technique. Postop pain and need for analgesics were controversial. ALIF has become an increasingly popular procedure for many spine disorders that need fusion. This is due to its ability to restore proper lordotic sagittal alignment and to allow better complete diskectomy or debridement of the intervertebral disk space, while avoiding surgical muscle trauma and neural element retraction encountered in posterior approaches. To bypass the morbidity due to long incisions and muscle splitting, minimally invasive techniques have been developed. Minimally invasive ALIF techniques include a mini-open approach, a laparoscopic approach, and a balloon-assisted endoscopic retroperitoneal gasless (BERG) technique. The indications are the same for all techniques and include back pain due to DDD, grade I or II spondylolisthesis, treatment of pseudarthrosis, and infectious diskitis. One of the first descriptions of the mini-open anterior approach was published by Mayer in 1997.12 Subsequent modifications were described after that.13–15 Obenchain was the first one to report a laparoscopic lumbar diskectomy.16 The laparoscopic approach is performed by an experienced endoscopic general surgeon to access the retroperitoneum at the spinal level needed. The BERG technique was developed to bypass the limitations of the gas insufflation of the laparoscopic approach. Thalgott et al17 first reported this technique.A lateral small incision is made laterally to get access to the retroperitoneal space. A balloon is then used to dissect the retroperitoneum, and several trochars are inserted. Then the surgery proceeds as a laparoscopic one but without need for gas insufflation of the retroperitoneum. A PubMed search for “ALIF” and “minimally invasive ALIF” was performed18–31 (Tables 26.3 and 26.4). There are no level I data comparing directly the open versus minimally invasive ALIF techniques. There is one level II study that compared laparoscopic versus open ALIF techniques. Regan et al26 reported in 1999 a large prospective, multicenter study comparing laparoscopic transperitoneal (n = 240) and open retroperitoneal (n = 305) ALIF. They reported shorter stay (p = 0.005), less blood loss (p = 0.005), and longer operative time (p < 0.001) in the laparoscopic group. Ten percent of the laparoscopic cases were converted to an open procedure. No significant difference was found in the postoperative complication rate (19.1% vs 14.1%) (p > 0.05). There are two level II studies that compared laparoscopic versus mini-open ALIF techniques. Zdeblick and David reported a prospective comparative study between laparoscopic (n = 25) and mini-open (n = 25) ALIF for L4–L5 level.28 There was no significant difference in operating time, blood loss, and hospital stay between the two groups for one-level L4–L5 fusion. For two-level fusions including L4–L5, the operative time was significantly higher in the laparoscopic group (p = 0.035). The complication rate was higher in the laparoscopic group 20% versus 4% in mini-open. Chung et al collected prospectively the data of 47 patients who underwent laparoscopic (25 patients) and mini-open (22 patients) ALIF procedures.29 The follow-up was for more than 2 years. The operative blood loss, postoperative hospital stay, and clinical outcomes (VAS, ODI, and fusion rate) were not significantly different between the two groups. The operative time was statistically higher in the laparoscopic group (p = 0.001). There is one level II study for a mini-open, video-assisted ALIF technique. Aunoble et al21 reported their series of 20 patients who underwent a mini-open, video-assisted ALIF procedure. The follow-up was 2 years. The mean operative blood loss was 100 mL. The mean Oswestry score was improved from 74% preoperative to 21% postoperative. VAS for back pain and leg pain were improved from 6.5 to 2.7 and from 6.2 to 3.4, respectively. The fusion rate was 95%. The one case of pseudarthrosis was found to be secondary to an infection of the level operated. There was no retrograde ejaculation noted for the male patients. There is one level III study that compares open versus mini-open ALIF procedures. Saraph et al27 reported a comparative retrospective study between conventional (n = 33) and minimally invasive extraperitoneal approach (n = 23) for ALIF. The mean follow-up was 5.5 years. There was no statistical difference in complications or fusion rate. Less blood loss and operative time and significant improvement of postoperative back pain were reported in the minimally invasive group (p < 0.001, p = 0.012, and p < 0.001, respectively). There are two level III studies that compare laparoscopic versus mini-open ALIF procedures. Kaiser et al31 conducted a retrospective review of 98 patients who underwent laparoscopic (47 patients) and mini-open (51 patients) ALIF procedures. Operative time was longer with the use of a laparoscopic approach, and significantly greater during L5–S1 ALIF procedures (p = 0.014). Hospital stay was significantly longer in the mini-open ALIF group (p = 0.016). The immediate postoperative complication rate was greater after mini-open ALIF procedures, 17.6 versus 4.3% (p = 0.04); however, the rate of retrograde ejaculation was higher in the laparoscopic group, 45 versus 6% (p = 0.006). Rodríguez et al30 reviewed retrospectively 45 patients who underwent L5– S1 laparoscopic (31 patients) and mini-open (14 patients) ALIF procedures. The mean follow-up was 12 months. There were no significant differences between the groups when comparing analgesia requirements, length of hospitalization, and complication rates. However, laparoscopic procedures were associated with shorter operating room times (p = 0.08) and less intraoperative blood loss (p = 0.029). The laparoscopic approach was estimated to cost $1,374 more than the open technique. Several level III studies are available in the literature for laparoscopic, BERG, and mini-open ALIF techniques. Regan et al18 published the first results for laparoscopic ALIF cases done in 34 patients in 1994. Thirty cases were successful and four were converted to an open procedure because of poor visualization (two cases) and venous injury (two cases). The average of operative time was 218 minutes, blood loss 128 mL, and hospitalization stay 3.67 days. Preliminary results showed an earlier discharge and return to work than that expected for open procedure. Heniford et al reported 140 laparoscopic ALIF cases in 2000.19 The operative time varied from 80 to 360 minutes. The average hospital stay was 2 days for one-level cases, and 4 days for two-level cases. The overall exposure-related complication rate was 10%, including four vessel injuries, one bowel injury, and one postoperative bowel obstruction. In four (2.9%) patients, surgery was converted to open ALIF, two for vessel injuries, one because of obesity, and one because of iliac vein immobility. Postoperative exposure-related complications included a permanent retrograde ejaculation rate of 2% and a transient retrograde ejaculation rate of 5% in men and a 10% prevalence of transient left leg sympathetic effect in the entire group. The cage complication rate was 15% caused by pseudarthrosis, misplacement, traction radiculopathy, and retropulsed disk material. The clinical outcomes were graded as improved in 70%, no change in 20%, and worsening of symptoms or complications in 10%. Liu et al also reported their results for 14 cases of laparoscopic ALIF.20 The average operative time was 300 minutes, blood loss 60 mL, and hospital stay 3.4 days. No intraoperative vascular or neurological injuries were observed. Three patients were converted to open procedure. Eighty percent of cases achieved a solid fusion, assessed by plain x-rays at 3 to 6 months. Thalgott et al23 reported their results of 202 patients treated by the BERG technique. Their follow-up was 24 to 36 months. The mean operative time was 101 minutes for one-level cases and 129 minutes for two-level cases. The average blood loss was 201 mL, and hospital stay was 1.95 days. There was a 16.8% rate of conversion to an open procedure. Clinical results at 2-year follow-up for the first 50 patients were 92% fusion rate, with 78% of patients reporting satisfactory pain relief. Operative complications included six vascular injuries, one ruptured diverticulum, one retrograde ejaculation, one deep vein thrombosis (DVT), and two cases of drop foot. Vazquez and Gireesan and Gazzeri et al24,25 also reported their results for the BERG technique (Table 26.3). The literature shows that minimally invasive ALIF techniques are associated with less blood loss, shorter hospital stay, and reduced pain and faster relief when compared with an open approach. Clinical outcomes were comparable. The data comparing laparoscopic and mini-open ALIF techniques were controversial. Pearls • Level II and III evidence comparing open versus minimally invasive ALIF techniques showed similar outcomes and complication rates, with less blood loss and operative time for the minimally invasive techniques. • The level II and III evidence comparing the different minimally invasive ALIF techniques is conflicting.
Minimally Invasive Lumbar Fusion: Results and Complications Compared with Open Techniques
 Minimally Invasive Transforaminal Lumbar Interbody Fusion
Minimally Invasive Transforaminal Lumbar Interbody Fusion
Level I Data
Level II Data
Level III Data
Summary of Data
 Minimally Invasive Anterior Lumbar Interbody Fusion
Minimally Invasive Anterior Lumbar Interbody Fusion
Level I Data
Level II Data
Level III Data
Summary of Data
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree