10 Neurologic Infections
Stephen Krieger
Central nervous system (CNS) infections are significant causes of morbidity and mortality, and must be addressed with diagnostic and therapeutic urgency. CNS infections can be broadly categorized as meningitis, encephalitis, abscesses, and infections of the spinal cord.
History
- Time course of symptoms: Acute (<48 hour is often bacterial), subacute (often viral, can be anything), chronic/smoldering (often fungal, parasitic, or noninfectious)
- History of, risk factors for, and prior testing for human immunodeficiency virus (HIV)
- If HIV positive: CD4 count, highly active antiretroviral treatment (HAART) history, opportunistic infection history, and prophylaxismedication compliance
- Other immunocompromised states: malignancy, malnutrition, immunosuppressive drugs, diabetes, alcoholism, renal replacement therapy, and splenectomy
- Travel history, exposures, vaccinations/inoculations
- Time of year:
- Summer/fall: Enteroviruses, arboviruses, Lyme disease, Rocky Mountain spotted fever
- Winter: Influenza
- Winter/spring: Measles, mumps, rubella, meningococcus, lymphocytic choriomeningitis
Physical Examination
- Vitals: Full set, including accurate rectal temperature
- Head, eyes, ears, nose, and throat (HEENT): Be attentive for facial rash (trigeminal zoster); ear canal vesicles (Ramsay-Hunt); thrush (HIV); parotiditis (mumps); dentition/dental abscesses; mastoid tenderness
- Evaluate carefully for nuchal rigidity, meningismus, and range of motion.
- Brudzinski’s sign: neck flexion elicits flexion of hips and/or knees
- Kernig’s sign: flex hip and knee with thigh against abdomen, then extend knee—note pain or resistance
- Both signs have poor sensitivity and are meaningful only in their presence and not their absence.
- Dermatologic: Examine the patient for rashes: erythema migrans (Lyme disease), petechiae (Rocky Mountain spotted fever), purpura (meningococcemia with or without meningitis), vesicles (varicella zoster virus [VZV]), maculopapular rash (measles, rubella, lymphocytic choriomeningitis), Osler nodes (red-purple, slightly raised, tender lumps on the digits), and Janeway lesions (nontender, often hemorrhagic, flat lesions mostly on the palms and soles. Both Osler nodes and Janeway lesions are clues to endocarditis).
Neurologic Examination
- A full neurologic examination, including assessment of mental status, cranial nerves, motor skills, and reflexes, as well as a sensory and cerebellar exam, should be performed on all patients.
- Mental status: Assess for encephalopathy and level of attentiveness, (Can the patient do the months backward, count 20 to 1 backward?)
- Assess for aphasia, neglect, apraxia, or other cortical signs.
- Be alert for ictal or postictal states.
- Cranial nerves: Cranial neuropathies are a clue to brainstem/meningeal processes (base of skull meningitis such as tuberculosis (TB) or carcinomatous meningitis, or rhombencephalitis such as caused by Listeria), hydrocephalus (sixth nerve palsy), or herniation syndromes (third nerve palsy). Assess the funduscopic exam for papilledema or macular star (as seen in neuroretinitis due to Lyme disease, Bartonella, or syphilis).
- Motor/sensory: Assess for focal deficits (epidural/parenchymal abscess, empyema, tuberculoma).
- Cerebellar: Assess for prominent cerebellar signs (consider varicella cerebellitis).
Differential Diagnosis
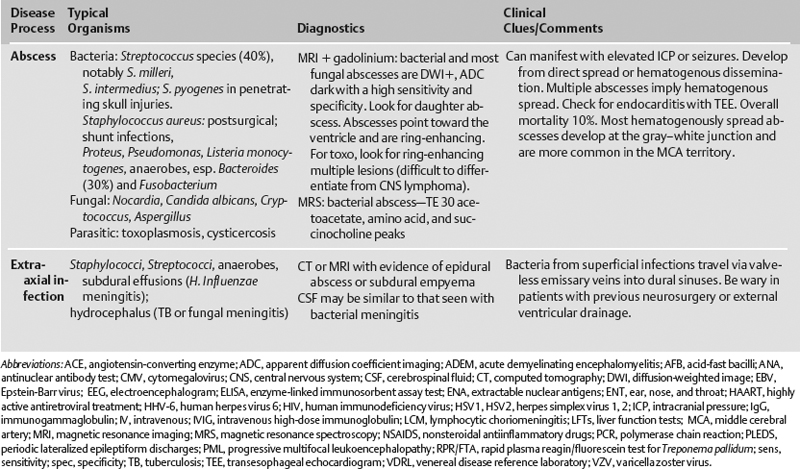
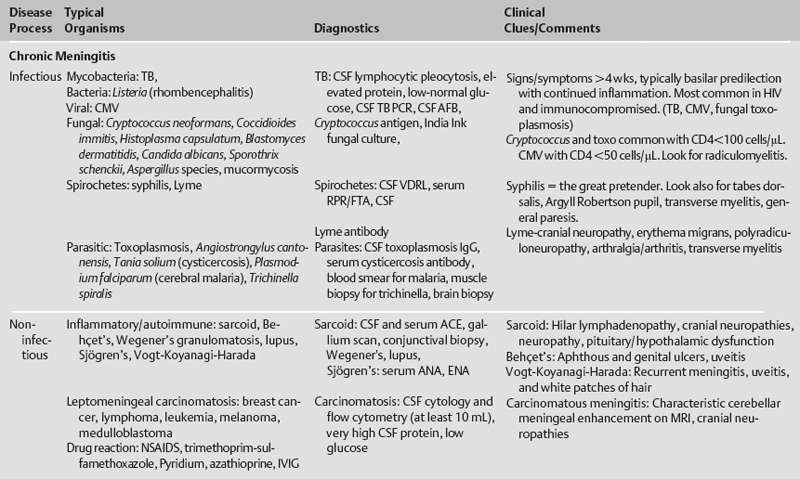
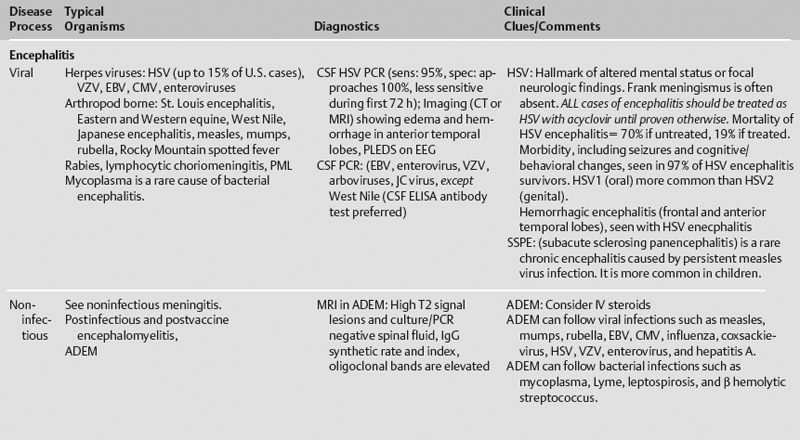
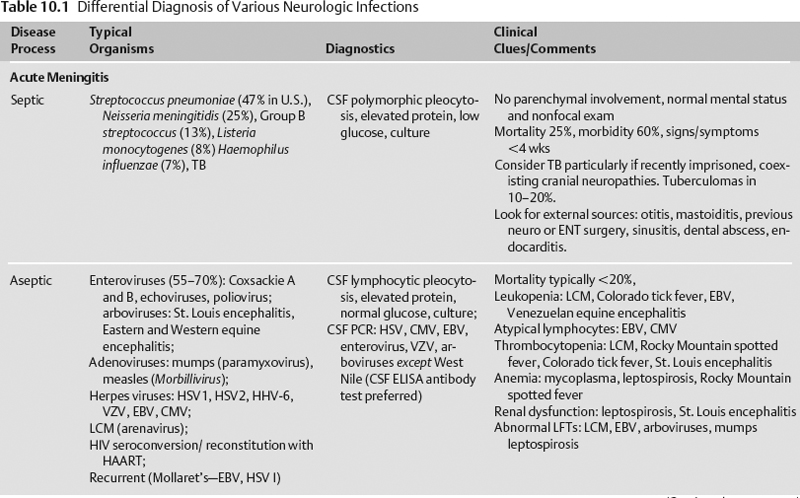
The differential diagnosis of various neurologic infections is given in Table 10.1.
Life-Threatening Diagnoses Not to Miss
- Bacterial meningitis
- Herpes simplex virus (HSV) encephalitis
- Laboratory studies
- Complete blood count (CBC), chemistry panel, liver function tests (LFTs), prothrombin time/partial prothrombin time (PT/PTT), human immunodeficiency virus (HIV), RPR/FTA, Lyme antibodies, and PPD (tuberculin skin test) placement
- Blood cultures, urinalysis (UA)/urine cultures and toxicology, sputum culture
- Chest x-ray, electrocardiogram (ECG), cardiac/hemodynamic monitoring; consider transesophageal echocardiogram (TEE)
- Lumbar puncture—make sure international normalized ratio (INR) <1.5, PTT<40, platelets >50; always check opening pressure and closing pressure (if large-volume 30 mL tap)
- Tube #1 cells and differential
- Tube #2 glucose and protein
- Tube #3 gram stain and culture
- Consider: Acid-fast and/or tuberculosis polymerase chain reaction (TB PCR), Cryptococcal antigen and India ink stains, fungal cultures, angiotensin converting enzyme (ACE), VDRL (if serum positive), Lyme antibody (if serum positive), PCR for HSV, cytomegalovirus (CMV), VZV, human herpes virus 6 (HHV-6), JC virus, and Epstein-Barr virus (EBV)
- Tube #4 cells and differential
- Traumatic tap: red blood cells/white blood cells (RBC: WBC) = 700:1, 1000 RBC account for 1 mg of cerebrospinal fluid (CSF) protein
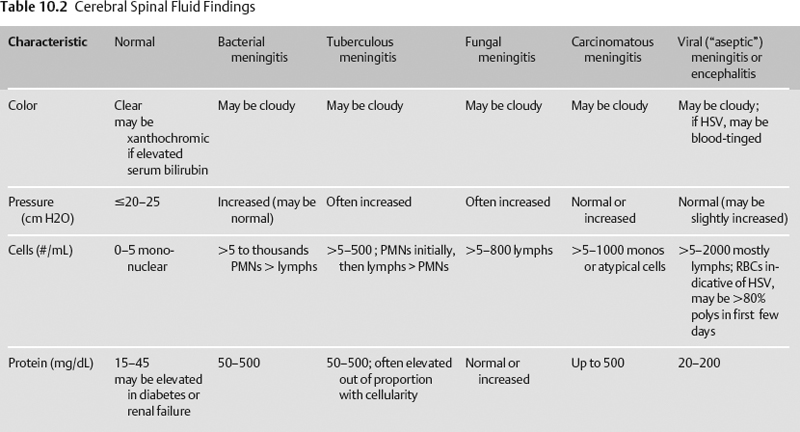
- CSF findings can be found in Table 10.2.
- Imaging studies
- Neurophysiologic testing
- EEG: Look for temporal periodic lateralized epileptiform discharges (PLEDS) with HSV. PLEDS are nonspecific and can occur with a variety of different etiologies.