Fig. 34.1
Appropriate positioning for the patient
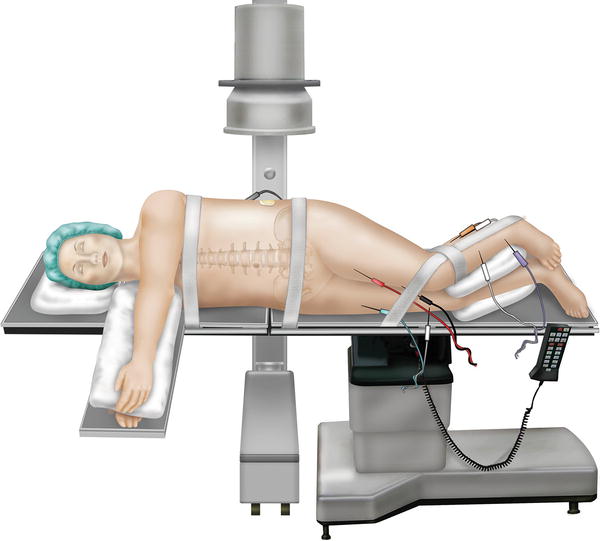
Fig. 34.2
The AP view should have parallel endplates and the spinous process should be centered between the pedicles. In the lateral view, the endplates should be parallel and the transverse processes should overlap
2.
A wide field of sterilization preparation is used in order to potentially access the posterior spine and the abdomen down to the symphysis pubis. It is possible to perform anterior and posterior instrumentation in the lateral position. Access to the abdomen is important in the advent of a visceral complication.
3.
Using fluoroscopy, the patient is positioned to maintain as true an anterior/posterior and lateral X-ray as possible for proper orientation (Fig. 34.2).
4.
Draw the line on the lateral side of the patient that connects the anterior to the posterior aspects of the disc space. This determines the incision site and, at the same time, orients the X-ray technician to the angle of the AP view and the lordosis of the disc space. The incision is approximately 3–5 cm from the mid-portion of the anterior/posterior line. The greater the distance, the more oblique the access will be. There is a range of several centimeters based on the surgeon’s desire to be more or less oblique for entry into the disc space (see Fig. 34.3a–c).
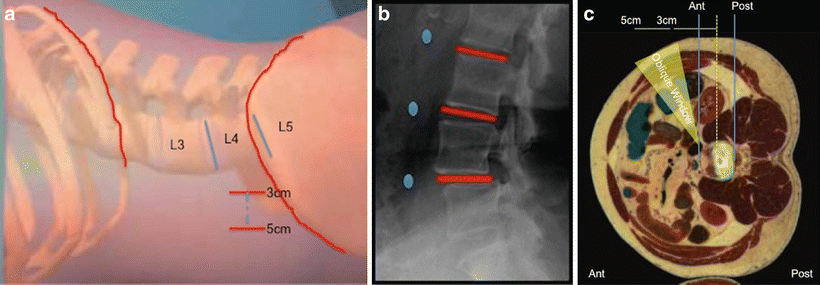

Fig. 34.3
(a, b) A view of the laterally marked skin incision and corresponding fluoroscopic view. (c) An axial cadaveric cut showing the oblique window for access to the disc space
5.
Once the anterior/posterior disc space has been identified, the incision site will be 3–5 cm anterior to the disc space and away from the ASIS (anterior superior iliac spine), and in line with the lordosis of the disc. The incision can be made in almost any orientation depending upon the surgical approach and number of levels to be done. The incision length is approximately 2–5 cm depending upon the technique preferred by surgeon to access the anterior disc (see Fig. 34.4a).
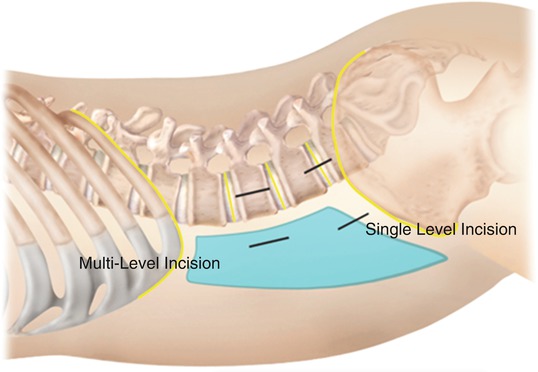

Fig. 34.4
The incision site will be 3–5 cm anterior to the disc space and away from the ASIS. For a two-level procedure, the incision is split cephalad and caudal between the two disc spaces to be treated
For a two-level procedure, the incision is split cephalad and caudal between the two disc spaces to be treated. The blunt finger dissection is done at the top of the incision and in line with each disc. At times, two disc levels can be reached through one blunt dissection. For wider spaced discs, two separate blunt dissections are needed (see Fig. 34.4b).
6.
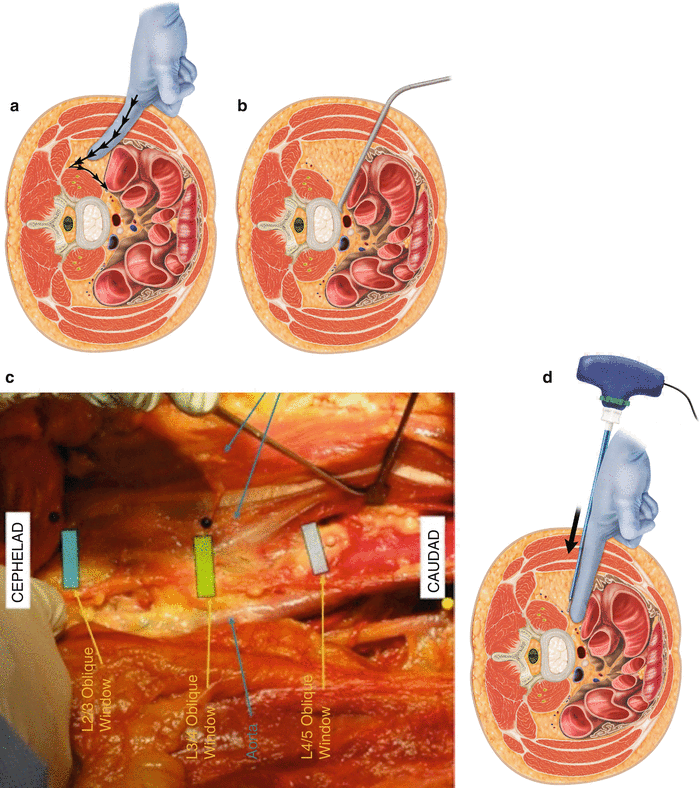
After the incision the external fascia of the external oblique muscle is opened (Fig. 34.5a). Using blunt finger dissection, the muscle fibers are split in the direction of the fibers until resistance is encountered from the almost perpendicular muscle fibers of the internal oblique muscle (see Fig 34.5b). The internal oblique muscle is finger dissected along the direction of its fibers until resistance is encountered from the smooth transversalis fascia layer beneath (see Fig. 34.5c). The direction of force from the finger is directed obliquely and posteriorly towards the Iliac crest and posterior spine. This prevents inadvertent entry into the peritoneal cavity. The goal is to feel a gentle “give way” of the transversalis fascia upon penetration from its smooth gliding surface plane as the release into the retroperitoneal space occurs with the tip of the finger. A decreased resistance should be immediately experienced as the finger slips into the retroperitoneal space. A feeling of lumpy, slippery tissue confirms entry into the retroperitoneal fat plane (see Fig. 34.6a, b).
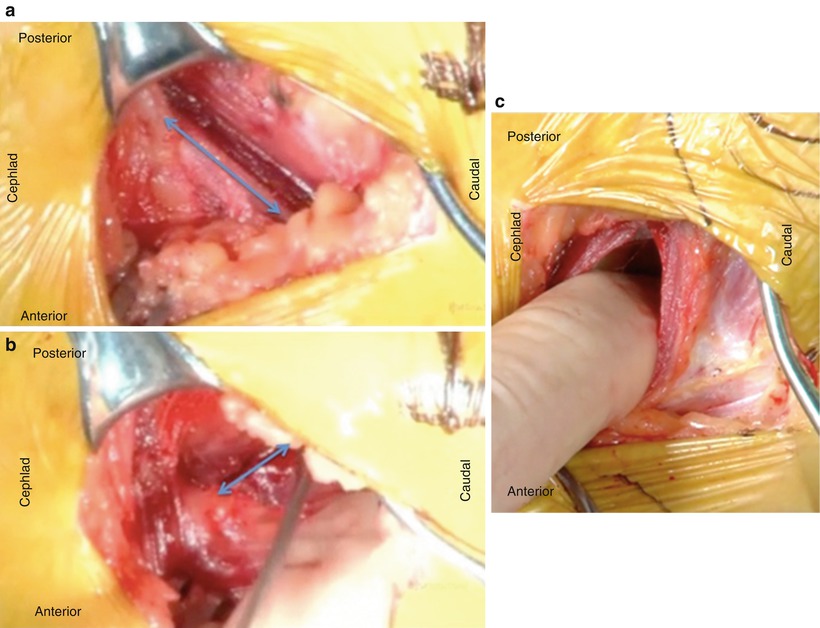
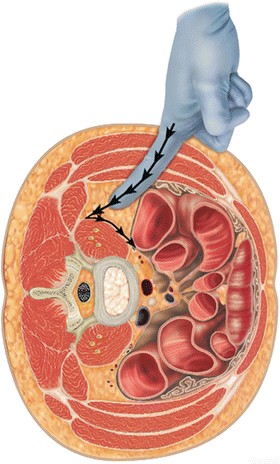

Fig. 34.5
(a–b) Views of the external oblique and the internal oblique muscles during dissection. (c) The direction of force from the finger is directed obliquely and posteriorly towards the iliac crest and posterior spine

Fig. 34.6
A decreased resistance should be immediately experienced as the finger slips into the retroperitoneal space
7.
The finger is directed more posteriorly to avoid inadvertent entry into the abdominal cavity. Once the finger is along the posterior pelvis and in the retroperitoneal space, a cephalad and caudal sweeping movement of the finger develops a wide plane in the retroperitoneal space (see Fig. 34.7a).