Fig. 17.1
A schematic of the similar metabolic pathways of the 5-HT precursor tryptophan and the analogous radioisotope α-[11C]MTrp. PNS peripheral nervous system, CNS central nervous system, BBB blood-brain barrier, α-[ 11 C]MTrp α-[11C]methyl-L-tryptophan, Trp tryptophan, α–M5–HTrp α-methyl-5-hydroxytryptophan, α–M5–HT α-methylserotonin, 5–HTrp 5-hydroxytryptophan, 5–HT serotonin, MAO monoamine oxidase
17.3.2 Baseline Measurements of Serotonin Synthesis in OCD
A recent α-[11C]MTrp study of OCD patients identified a pattern of effects that was opposite to that seen in the previously tested patient groups. Berney et al. (2011) compared regional K* values of unmedicated OCD patients (n = 21) with those of age- and gender-matched healthy controls (n = 21). All patients were without current comorbid disorders and reported never having used the alleged SERT-inhibiting neurotoxic substances 3,4-methylenedioxymethamphetamine (MDMA) and 3,4-methylenedioxyamphetamine (MDA). Patients with a past history of depression secondary to OCD were included in this study, but no significant correlations were found between K* values and Beck Depression Inventory (BDI) scores, suggesting that this was not a confounding variable. Regions of interest included cortical areas such as the OFC and ACG and subcortical areas such as the caudate, based on previous implications of these regions in OCD pathology. OCD patients showed significantly higher K* values in the right hippocampus and left inferior temporal gyrus and did not show significantly lower K* values in any of the regions of interest. The larger subgroup of male patients also showed significantly higher K* values in the caudate nucleus bilaterally. Furthermore, estimates of 5-HT synthesis in the temporal cortex and right caudate correlated positively with symptom severity (Table 17.1).
Table 17.1
The demographics of both OCD patients and healthy controls in a recent study by Berney et al. (2011)
Characteristics | OCD patients (n = 21) | Controls (n = 21) |
|---|---|---|
Age in years | ||
Mean (SD) | 34.0 (8.6) | 34.0 (9.6) |
Range | 18–53 | 20–56 |
Gender | 15 M/6 F | 15 M/6 F |
Early-onset OCD | 11 | N/A |
Predominant compulsion | ||
Washing | 10 | N/A |
Checking | 11 | N/A |
History of MDE | 6 | 0 |
History of substance abuse | 1 | 0 |
Past SSRI treatment | 2 | 0 |
Mean Y-BOCS score (SD) | 23.6 (5.3) | N/A |
Mean BDI score (SD) | 13.2 (9.3) | 1.4 (2.2) |
Mean plasma free Trp | 8.4 (3.7) | 8.9 (3.8) |
Concentration, nmol/l | ||
These findings suggest that OCD patients, as a group, relative to non-symptomatic healthy volunteers, may have abnormally elevated rates of 5-HT synthesis in brain regions such as the hippocampus, temporal cortex and caudate. Although this study alone could not establish whether elevated 5-HT synthesis in limbic and striatal regions reflects a primary or secondary compensatory event, these findings connote the failed attempt by the inhibitory system to regain control. This interpretation was deemed plausible and emphasized.
17.3.3 The Effects of Treatment on Serotonin Synthesis in OCD
Extending the findings of Berney et al. (2011), a recent unpublished study by our group has investigated the change in brain regional 5-HT synthesis rates after behavioural and drug therapy for OCD. By also using PET in combination with the α-[11C]MTrp tracer, brain 5-HT synthesis was estimated before and after CBT or sertraline treatment. Participating patients were randomly assigned to 12 weeks of either biweekly CBT sessions (n = 6) or daily doses of sertraline (n = 6). CBT included cognitive therapy for symptom-related difficulties such as dysfunctional beliefs and tolerance of distress, and exposure and response prevention with therapist assistance in naturalistic environments (e.g. home, work) as needed. Sertraline doses were gradually increased to a maximum of 200 mg, and the mean daily dose received was 133 mg/day (SD = 52 mg/day). Both SPM8 and volume of interest analyses were performed, and Yale-Brown Obsessive Compulsive Scale (Y-BOCS), BDI, and Go/NoGo task scores were assessed prior to and following treatment. Although a total of 16 patients were recruited, the preliminary PET analyses presented here are limited to a subset of 12 patients. As such, the following results are preliminary, and the proposed interpretations, based upon the intriguing patterns that have emerged thus far, are provocative and must be considered speculative. Significant improvement in symptom severity was observed in both treatment modalities (see Fig. 17.2), with four patients in the sertraline group and five in the CBT group showing a minimum 30 % decrease in Y-BOCS scores, classifying them as responders to treatment (Table 17.2).
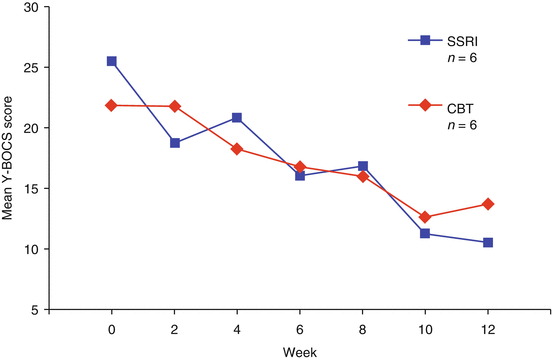

Fig. 17.2
Significant decreases in symptom severity were observed in OCD patients treated with 12 weeks of either cognitive behaviour therapy (CBT) or the selective serotonin reuptake inhibitor (SSRI) sertraline
Table 17.2
The demographics of OCD patients treated with either SSRI or CBT
Characteristics | SSRI group (n = 6) | CBT group (n = 6) | ||
Age in years | ||||
Mean (SD) | 33.5 (10.0) | 37.0 (11.1) | ||
Range | 18–45 | 26–53 | ||
Gender | 4 M/2 F | 4 M/2 F | ||
Early-onset OCD | 3 | 5 | ||
Predominant compulsion | ||||
Washing | 3 | 1 | ||
Checking | 3 | 5 | ||
History of mood disorder | 2 | 2 | ||
History of substance abuse | 0 | 0 | ||
Past SSRI treatment | 1 | 0 | ||
Pre | Post | Pre | Post | |
Mean Y-BOCS score (SD) | 25.5 (3.4) | 15.7 (9.4) | 21.8 (4.5) | 14.6 (6.0) |
Mean BDI score (SD) | 16.8 (11.8) | 8.8 (10.7) | 9.7 (5.3) | 6.4 (5.9) |
Mean plasma free Trp | 9.9 (2.1) | 10.0 (2.1) | 10.8 (2.8) | 8.6 (1.3) |
Concentration, nmol/l | ||||
Interestingly, in both treatment modalities, there was a significant positive correlation between symptom improvement and K* value change in the right striatum, right hippocampus, and cerebellum (p < .05). That is, both CBT and sertraline treatment appear to have increased α-[11C]MTrp trapping in regions previously found to have abnormally high α-[11C]MTrp trapping in unmedicated OCD patients (Berney et al. 2011). These findings suggest that a modulation of central serotonergic neurotransmission could contribute to further coping, thus providing the support needed to effectively control OC symptoms. The direction of change in K* values suggested that the response seen here was associated with a further enhancement of 5-HT synthesis, in essence allowing any inhibitory influence to achieve full potential and act effectively as a brake against obsessions and compulsions. Additionally, tracer trapping (K*) at baseline correlated positively with treatment response, independently of the nature of treatment. The higher the 5-HT synthesis in the pons before treatment, the more patients benefitted from either CBT or sertraline treatment (see Fig. 17.3). The ability of K* values at baseline to predict response to treatment is consistent with the proposed braking system hypothesis.
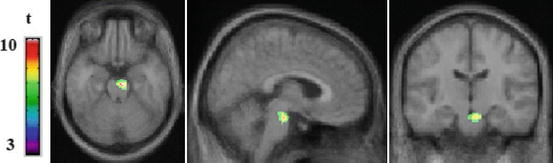

Fig. 17.3
Statistical parametric maps (SPM8) demonstrating a positive correlation between pretreatment K* values in the pons and symptom improvement after CBT or SSRI treatment
Furthermore, responders showed substantial increases in unidirectional α-[11C]MTrp trapping, suggesting that these changes were not merely a regression towards the mean, as shown in Fig. 17.4. These increases in regional 5-HT synthesis appear to be restricted to the right side of the brain; whether such asymmetry is meaningful or relevant is not known, as this effect could reflect on sample size and “disappear” with a larger sample studied for a longer time. Those responders whose baseline K* values in the temporal cortex, frontal cortex, and cerebellum were below the average control K* values in these regions of healthy controls from a study by Berney et al. (2011) showed increases in K* values well above mean control K* values. Similarly, responders whose K* values in the striatum and hippocampus were already above mean control K* values at baseline also showed a substantial increase in regional 5-HT synthesis. The marked increases in α-[11C]MTrp trapping were not observed in nonresponders, thus suggesting that dysfunction in the nonresponders may well be differentially mediated.
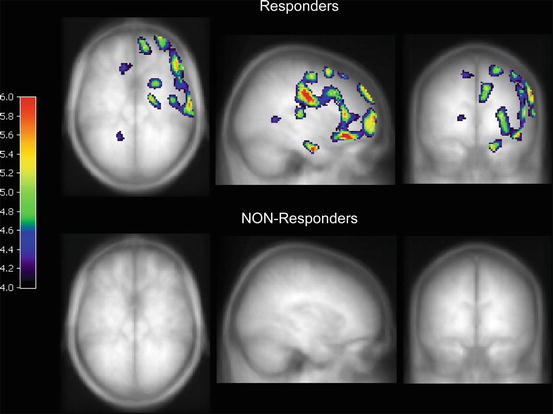

Fig. 17.4
Maximum intensity projection of the t-values (SPM8: p < 0.005 and k = 50 voxels) for the non-normalized K* difference between the post- and pretreatment conditions. TOP: OCD patients that responded to either SSRI treatment or CBT (>30 % decrease in Y-BOCS scores). Bottom: OCD patients that did not respond to either treatment (no significant voxel)
17.4 Concluding Remarks
In spite of numerous findings, some of which were reviewed herein, one must recognize that those very many contributions to our understanding of OCD cannot fully elucidate the details within the multiple OCD aetiologies. Several aetiological pathways and mechanisms, responsible for the many diverse phenotypic expressions, are likely to be encountered. Additionally, longer-term CBT is required for many patients to optimize symptom reduction (offered following this study). Further research could usefully examine results following additional treatment duration.
One intriguing observation that can be made, though, is the link between memory and OCD. In particular, it has often been speculated that OCD patients with predominantly checking compulsions (referred to as “checkers”) may have altered meta-memory (van den Hout and Kindt 2003). It has been reported that for individuals performing an experiment with disinformation distractors, those with reduced memory confidence exhibited a greater amount of checking (Alcolado and Radomsky 2011; Cuttler et al. 2013; Radomsky and Alcolado 2010). OCD checkers may exhibit dysfunctional memory self-monitoring; that is they have decreased confidence in their memory ability, yet they actually have higher standards for the reliability of their memory (Macdonald et al. 1997). Interestingly, then, OCD patients showed, at baseline, abnormal α-[11C]MTrp trapping in the temporal cortex, which is a structure with important roles in memory formation and preservation (Bayley et al. 2005).
The present research also suggests that rather than contributing to OC symptoms directly, the serotonergic system acts to control symptoms. As such, prior to treatment, it is proposed that this system is working inefficiently and therefore unable to successfully inhibit symptoms in a good portion of OCD patients. Accordingly, clinical improvement as a result of either behavioural or drug therapy may arise from a stimulation of serotonergic neurotransmission that ultimately allows this system to control symptoms effectively, thus producing a therapeutic response. As the system is progressively engaged, and further overactivity of the serotonergic system gains traction, effective inhibition may take place.
Acknowledgments
Alexandre Berney, MD; Igor Sibon, MD, PhD; Amir Barsoum, MD; Gilbert Pinard, MD; Akio Nakai, MD, PhD; Mirko Diksic, PhD
References
Baxter LR, Phelps ME, Mazziotta JC, Guze BH, Schwartz JM, Selin CE (1987) Local cerebral glucose metabolic rates in obsessive-compulsive disorder. Arch Gen Psychiatry 44:211–218PubMedCrossRef
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree





