Fig. 1
An emergency CT on admission showed SAH mainly distributing in the interpeduncular and prepontine cistern
His initial clinical condition was Hunt and Hess grade IV. Three-dimensional CT and diagnostic angiography showed an upper basilar trunk fusiform-shaped aneurysm located distal to the anterior inferior cerebellar artery (Fig. 2). Original source images of multidetector computerized tomography (Multi-detector-CT) and magnetic resonance imaging (MRI) (T2-weighted images) showed a dysmorphic wall of the aneurysm with the double lumen sign. Since the preservation of the basilar trunk was not feasible because of its anatomical configuration, EC-IC bypass [superficial temporal artery (STA)–superior cerebellar artery (SCA)] and endovascular trapping were performed 14 days after the onset of SAH.
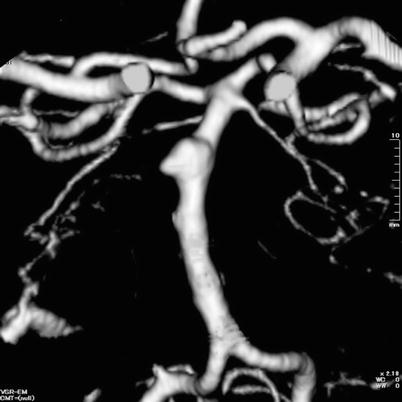

Fig. 2
A 3D-CT showed a dysmorphic fusiform aneurysm located in the upper basilar trunk
Bypass operation: Under general anesthesia, a 10-cm segment of parietal branch of the superficial temporal artery (STA) was anastomosed to a hemispheric branch of the superior cerebellar artery (SCA) through a right subtemporal approach (Figs. 3 and 4).
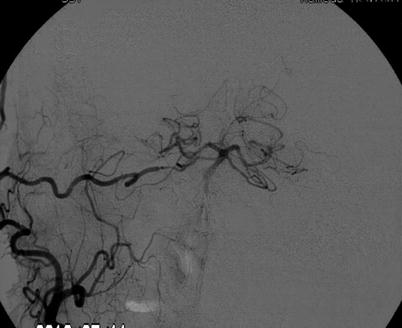
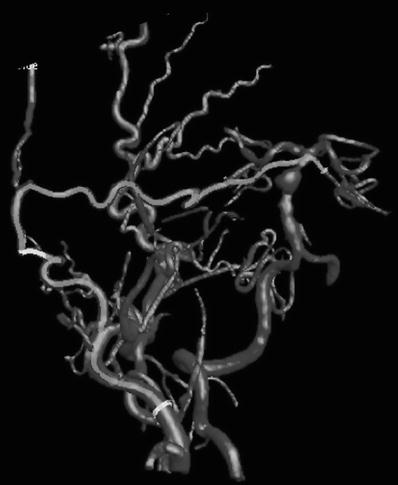

Fig. 3
Right external carotid angiography under the balloon occlusion of basilar trunk is showing bilateral PCA supplied from the STA-SCA bypass

Fig. 4
A 3D rotation angiography delineates the distribution of revascularization through the STA-SCA bypass
Endovascular procedure: Immediately after this STA-SCA bypass surgery, the patient was moved to an angiography suite. A selective balloon occlusion test was performed at the mid-basilar artery just proximal to this aneurysm with a microballoon catheter. Under this balloon occlusion, right external carotid angiography showed sufficient revascularization through this bypass and enough flow to the bilateral posterior cerebral artery, and SCA cortical territory was confirmed angiographically. Subsequently, embolization of aneurysmal lumen, including parent artery (internal trapping), was achieved (Fig. 5).
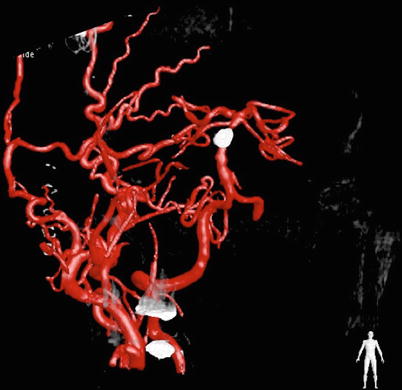

Fig. 5
Complete obliteration of fusiform aneurysm is seen, while bilateral distal PCA territory is supplied through the STA-SCA bypass
Postoperative course: He gradually regained consciousness and became alert and well oriented at 4 days post-surgery. However, his left hemiparesis remained. A postoperative MRI showed an infarction of the right paramedian nuclei of pons that was associated with the pontine perforators originating from the dissecting lesion. He went to the regional hospital for further physiotherapy with modified Rankin scale 3 at 60 days from the onset.
Case 2
A 54-year-old female presented with sudden onset of headache. An emergency CT showed an abnormally high density area of a round shape that was measured around 10 mm in diameter, localizing at the left quadrigeminal cistern and pulvinar thalamus. Initially this was diagnosed as a thalamic hemorrhage; however, an MRI and three-dimensional computerized tomography (3D-CT) images revealed a fusiform aneurysm locating left distal posterior cerebral artery (P3-P4 segment). Since the subarachnoid hemorrhage was negative on FLAIR images of the MRI, this was diagnosed as an impending ruptured aneurysm. Cerebral angiography showed a dysmorphic fusiform aneurysm at the left P3-P4 segment (Fig. 6a). Because the localization of this aneurysm was close to the tentorial notch, this was considered to be a dissecting aneurysm.
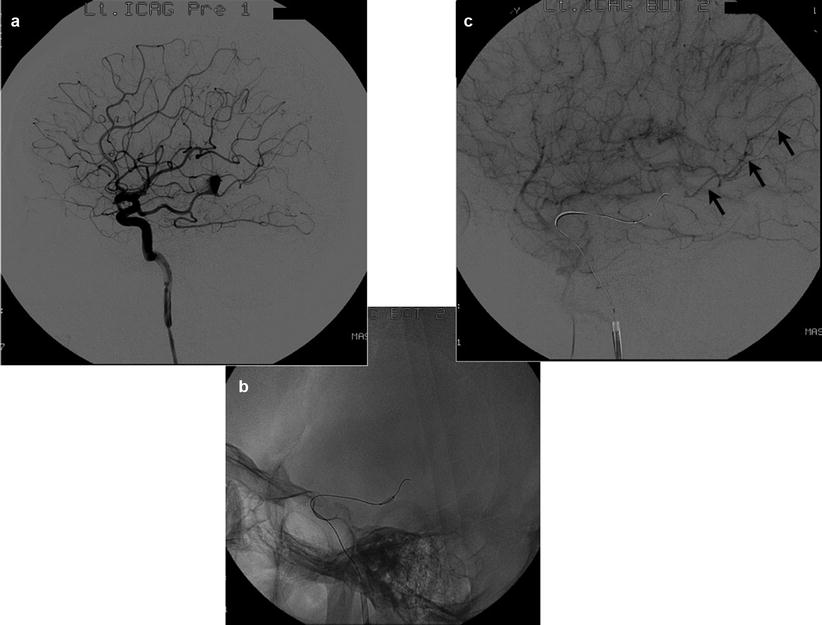

Fig. 6
(a) Left internal carotid angiography shows fusiform aneurysm locating distal PCA (P3-P4 segment). (b) Through the fetal type of posterior communicating artery, a microballoon catheter was navigated and inflated at the P3 segment that is just proximal to the aneurysm. (c) Left internal carotid angiography under balloon occlusion revealed a retrograde filling of P4 segment through the parieto-occipital branch of PCA. This functional test indicated sufficient collateral circulation through the leptomeningeal anastomosis from MCA cortical territory. It enables the trapping of the pathological lesion without hemodynamic compromise in the territory of PCA
Endovascular procedure: Under general anesthesia in the angiography suite, a microballoon was navigated into the P2 segment that was just proximal to this aneurysmal lumen (Fig. 6b). Under inflation of this microballoon, the ipsilateral internal carotid angiography showed a sufficient collateral supply with retrograde filling of the parieto-occipital branch of the posterior cerebral artery (PCA) (Fig. 6c). Because of this, enough retrograde flow distributing to the distal lumen of the aneurysm, bypass surgery was not indicated in this case.
A 3D-rotational angiography (3D-RA) confirmed that this leptomeningeal anastomosis was mainly supplied from the angular artery of the middle cerebral artery (MCA) cortical territory (Fig. 7).
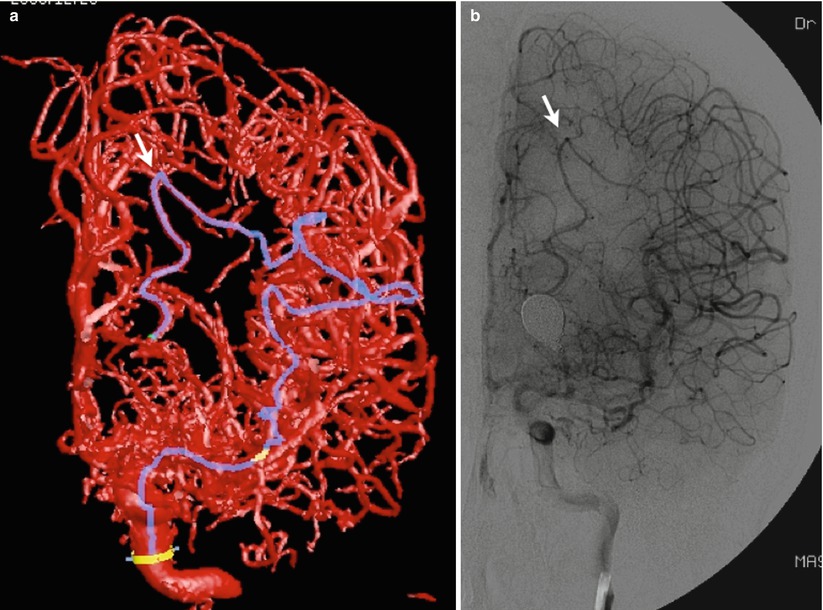

Fig. 7




(a, b) 3D-RA frontal view corresponding to the DSA showing retrograde filling to the parieto-occipital artery (arrow). Note the blue color line on 3D-RA. It delineates the collateral pathway of leptomeningeal anastomosis through the angular artery of MCA
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








