Fig. 1
Hunt and Hess grade at hospital admission and related mortality
The patients were divided into three groups. In the first group, vasospasm did not develop during the patient’s stay in the hospital. In the second group, clinical vasospasm developed after surgery. In the early postoperative days, the CSF was hemorrhagic in these patients. After daily drainage (maximum 200 cc), the color of the CSF turned clear. The patients of the second group showed clinical benefits but there was no significant difference in mortality and morbidity when compared with the first group. The clinical improvement of the patients in group 2 may be interpreted as the effect of CSF drainage by removing the blood and blood products and cleaning the subarachnoid space. In the third group, clinical vasospasm developed after surgery and did not respond to medical and CSF drainage treatment. On daily drainage, CSF was permanently hemorrhagic and never became clear. In this group, patients developed permanent neurologic deficits. These poor neurologic consequences may be attributed to blood and blood products that cannot be removed from subarachnoid space by lumbar drainage. The mortality and the morbidity of the patients in group 3 were significantly higher when compared with group 1 (Table 1) (Fig. 2). Common complications such as hydrocephalus and increased intracranial pressure in patients with CSF drainage occurred less frequently in both groups when compared with literature values.
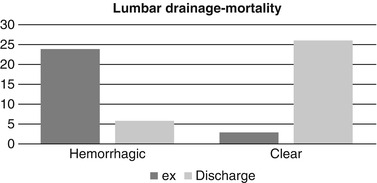
Table 1
CSF drainage and mortality
Lumbar drainage | Exitus, n (%) | Discharge, n (%) | Total (n) | Statistical count |
|---|---|---|---|---|
Hemorrhagic | 24 (80.0) | 6 (20.0) | 30 | X 2: 28.82 p: 0.000 |
Clear | 3 (10.3) | 26 (89.7) | 29 |

Fig. 2
Relationship between hemorrhagic cerebrospinal fluid and mortality
Discussion
There is currently an ongoing controversy regarding the diagnosis of vasospasm and SAH volume on initial CT scan. Although some studies show an increase in vasospasm based on initial CT scans because of SAH volume, others detect no significant difference [12, 16]. The amount of blood in the cisterns and fissures is known as an important risk factor in vasospasm [6, 9, 19, 23]. Although the Hunt and Hess classification and Glasgow Coma Scale are used for clinical staging, the Fisher Scale is used to determine the relationship between the amount of blood on CT scan and risk of vasospasm [10, 15]. The main determinant for the survey after SAH is the Fisher grade on the initial CT scan [13]. Severe neurologic status within the first 24 h after bleeding, old age, and the size of aneurysm are determining factors of mortality and morbidity after SAH. Early surgery is necessary to prevent rebleeding.
Vasospasm effects can be reduced by compensating for hypovolemia and severe anemia with hydration and blood transfusion in the postoperative period. Hypertensive therapy and calcium channel blockers may be particularly useful. Blood and blood products within the subarachnoid space play an important role in the development of cerebral vasospasm, which can be prevented by removing degrading products from the space via lumbar drainage [1, 6, 7, 9, 19]. Additionally, CSF drainage reduces the intracranial pressure and development of hydrocephalus, and a permanent shunt may be not necessary [21].
In the half of the cases, vasospasm appears as a delayed ischemic neurological deficit. These patients can be divided into two groups. In half, there is spontaneous resolution, and the remaining progress to cerebral infarction. In recent series, it has been reported that 15–20 % of these patients remain plegic or die despite all treatment options. Because symptomatic vasospasm causing delayed infarction may not present obvious symptoms in comatose patients, the smallest change in neurological examination should be approached with suspicion in this group of patients [11].
In a study of clinical and radiological vasospasm among a cohort of 921 patients, 17 % of patients had symptomatic vasospasm and 28 % had radiological vasospasm [8, 24]. Radiological vasospasm can be detected nearly 70 % of the SAH cases in DSA in the first week and only one-third of the cases were symptomatic that were proven in DSA [17].
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree





