Definition
Author
Total sample size
Number of pos SA
Number of non-pos SA
Prevalence of pos SA (%)
Lenient definition
Richard [8]
120
67
53
55.8
Sunwoo [9]
91
65
26
71.4
Teerapraipruk [10]
144
96
48
66.7
Gillman [4]
100
63
37
63
Oksenberg [11]
574
321
253
55.9
Strict definition
Gillman [4]
100
23
77
23
Mador [5]
258
69
189
26.7
One of the abovementioned studies was a prospective cohort trial performed in Melbourne, Australia, on 100 consecutive OSA patients, and the prevalence was measured by both definitions [4]. When positional sleep apnea was defined using the lenient definition, the prevalence was 63 %, but when they used the stricter definition for positional sleep apnea, the prevalence decreased to 23 % [4]. In our study, the prevalence using the lenient definition was 58 % and decreased to 27 % with the stricter definition [5]. It is still noteworthy that even with the strict definition, positional sleep apnea is common (Table 1). Thus, methods that can successfully eliminate supine sleep and are tolerable have the potential to be an important treatment modality.
One methodologic point that needs to be considered is the effect that the polysomnographic procedure has on promoting supine sleep in the laboratory. During a sleep study, the patient is connected to a multitude of wires. The patient may try to sleep on his/her back in the sleep laboratory because they are concerned that other postures may promote lead dislodgement. In a prospective study in 12 positional sleep apnea patients, the patients were studied for 3 nights, once with standard PSG leads attached (PSG night) and the other 2 nights without any leads attached, but position was monitored with a position sensor [12]. The time spent supine was 56 % greater during the PSG night compared to the non-PSG nights [12]. This can artifactually magnify the severity of the patients’ disease (when they have a positional component) compared to what would occur at home when supine sleep would be less.
There have also been significant differences in the AHI when tested in the right lateral compared to the left lateral position. A retrospective review performed in Turkey noted that the left lateral position had a higher AHI at 30.2 ± 32.6 per hour compared to the right lateral position at 23.6 ± 30.1 per hour that was statistically significant (p < 0.001) [13]. Another interesting study evaluated 105 sleep apnea patients in the sleep laboratory using a 9-position thoracic sensor. Positions identified were the left lateral (L), prone (P), prone left (PL), prone right (PR), right (R), supine (S), supine left (SL), supine right (SR), and upward position (UP) [14]. It was noted that the AHI gradually improved when the body position changed from the supine to prone position [14]. Thus, in this study, the AHI was worse in the supine posture, intermediate in the lateral posture, and best in the prone posture (Fig. 1). The AHI in the upright posture was similar to that observed in the prone position. The supine left or right was a position intermediate between the supine and lateral position and had an AHI that was similar to that observed in the lateral position. Similarly, the prone right and left was a position intermediate between the prone and lateral position and had an AHI similar to that observed in the prone position [14].
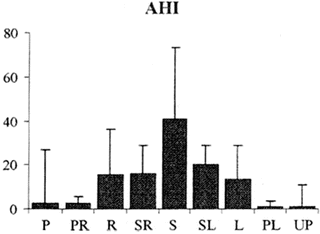

Fig. 1
AHI in different body positions. L left lateral, P prone, PL prone left, PR prone right, R right, S supine, SL supine left, SR supine right, and UP upward position. Figure adapted from Pneumologia, 2011. 60(4): p. 216–21 [14] with permission
Factors That Predict Occurrence of Positional Sleep Apnea
Multiple factors have been evaluated in the last few decades that are strongly associated or directly affect the prevalence of positional sleep apnea.
Sleep Apnea Severity
As recommended by the American Academy of Sleep Medicine, sleep apnea severity is classified into three categories based on the AHI [15]. Mild sleep apnea has an AHI between 5 and 15 events per hour; moderate sleep apnea, an AHI between 15 and 30 events per hour; and severe sleep apnea, an AHI more than 30 events per hour [15].
There have been several studies performed to evaluate the prevalence of positional sleep apnea among the different severities of sleep-disordered breathing.
A study by Mador et al. evaluated patients at two different settings: at a veterans affairs medical center with a predominantly male population and a free-standing ambulatory sleep center with equal gender proportions. They noted that positional sleep apnea prevalence (defined using the strict definition for positional sleep apnea) decreased as the sleep apnea severity increased [5]. It was 49.5 % in mild sleep apnea, 19.4 % in moderate sleep apnea, and 6.5 % in severe sleep apnea [5]. Another study by the same group evaluated 80 sequential patients who were referred to the Veterans Affairs Medical Center in Western New York and enrolled 20 patients in each of the three sleep apnea severity categories and an additional 20 patients who did not meet the definition for sleep apnea [16]. The hazard ratio for events (apneas and hypopneas) was significant in patients during supine compared to non-supine sleep in the mild and moderate sleep apnea groups at 1.25 (95 % CI 1.02–1.52) and 1.24 (95 % CI 1.04–1.47), respectively [16], meaning that events were more likely to occur in the supine posture compared to the non-supine posture in patients with mild and moderate sleep apnea but not in the normal and severe sleep apnea groups [16].
A retrospective analysis by Oksenberg et al. evaluated 574 sleep apnea patients diagnosed by a respiratory distress index (RDI) greater than 10 per hour. They were further categorized into four different RDI categories (10–19.9, 20–29.9, 30–39.9, greater than 40 per hour). It was noted that the prevalence of positional sleep apnea (defined using the more lenient definition) remained high between 65.1 and 69.0 % in the mild, moderate, severe sleep apnea categories (RDI 10–19.9, 20–29.9, and 30–39.9 per hour), but showed a statistically significant reduction to 32.4 % in the most severe category (RDI greater than 40 per hour) [11]. Chung et al. evaluated 218 positional sleep apnea patients and randomly selected 109 of these patients to be matched with non-positional sleep apnea patients by age, gender, and body mass index (BMI) [17]. It was noted that both the matched and unmatched positional sleep apnea patients had less severe AHI values compared to the non-positional sleep apnea patients [17].
Although “positionality” gets weaker as the severity of sleep apnea worsens, it should be noted that in severe sleep apnea patients, the severity of each apneic event (apnea duration, the lowest oxygen desaturation, and duration of arousals) is still worse in the supine position compared to the non-supine position [18]. A retrospective review performed by Oksenberg et al. evaluated 638 patients undergoing two diagnostic polysomnograms (PSG)s at least 6 months apart [19]. Obstructive sleep apnea was seen in 566 patients [19]. They were then divided into four groups according to whether a positional component occurred during the two recorded PSGs: “non-positional sleep apnea (NPP) who remained NPP,” “positional sleep apnea (PP) who remained PP,” “PP who became NPP,” and “NPP who became PP” [19]. The “NPP who remained NPP” group were found to have a higher AHI in their initial PSG compared to the other three groups. The group of patients that had “PP who became NPP” had a significant increase in the AHI compared to the other three groups [19]. Thus, worsening of the AHI reduces the prevalence of positional sleep apnea.
Ozeke et al. evaluated the AHI on the left side and compared it to the right side in patients with different severities of obstructive sleep apnea [13]. It was noted that on the left side, AHI was significantly higher compared to the right side in patients with moderate and severe OSA, but was not significantly different in patients with mild OSA [13].
Why is positional sleep apnea more common in patients with mild to moderate sleep apnea? Patients with positional sleep apnea might have a less collapsible upper airway that only collapses in the supine posture when gravity works against the patient. Patients with severe sleep apnea likely have a more collapsible airway that collapses in all postures, and since the AHI is already severely increased in the non-supine posture, it is difficult for that metric to substantially worsen in the supine posture. The prior study by Oksenberg et al. shows that as sleep apnea worsens, patients often will switch from a positional component to a non-positional component [19].
Anatomic/Morphological Factors
There are multiple studies performed to evaluate the anatomic factors that would determine the propensity of having positional sleep apnea.
A Belgium study evaluated the effect of changes in body position from prone to right side to supine by fast-computed tomography scanning in six awake position-dependent OSA patients and five position-nondependent OSA patients [20]. It was noted that the former (positional patients) had a larger minimum cross-sectional area than the latter and changes in body position affected the lateral but not the anteroposterior dimensions of the upper airway [20]. A study on 91 Korean patients with OSAS evaluated the level of obstruction based on video fluoroscopy [9]. The patients with soft palate obstruction had a higher chance of having positional sleep apnea compared to the patients with tongue base obstruction [9]. A Japanese study tried to evaluate the pathophysiology of positional sleep apnea [21]. They induced total muscle paralysis with general anesthesia in eight OSA patients in order to eliminate neuromuscular factors that could contribute to pharyngeal wall patency [21]. The cross-sectional area of the pharynx was measured endoscopically at different static airway pressures [21]. Then, a static pressure area plot between the positions was assessed to evaluate the influence of body position on the mechanical properties of the pharyngeal wall [21]. Static pressure area curves were higher in the lateral position compared to the supine position indicating a larger upper airway area at any given pressure in the lateral position (Fig. 2) [21]. In another small Japanese study, ten BMI-, age-, and AHI-matched positional and non-positional sleep apnea patients, respectively, underwent pharyngeal magnetic resonance imaging and cephalometric radiography during wakefulness [22]. They noted that positional sleep apnea patients have smaller volumes of the pharyngeal lateral wall soft tissues compared to non-positional sleep apnea patients [22]. They also have a larger maxilla-nasion-mandible angle and a smaller lower facial height than the latter [22]. They concluded that positional sleep apnea patients could have a wider airway laterally and a more backward position of the lower jaw compared to non-positional sleep apnea patients [22] which would lead to obstruction primarily in the supine posture. A Chinese study on 103 OSA patients revealed that the modified Mallampati (MMP) grade and the neck circumference were important morphological features that helped to predict which patients were likely to have positional sleep apnea [23]. Those with a thick neck or small airway by Mallampati score were less likely to have positional sleep apnea [23]. A Japanese study published in 2008 evaluated the upper airway morphology in positional sleep apnea compared to non-positional sleep apnea patients [24]. They noted that the horizontal distance between the tonsillar fauces was significantly greater in positional sleep apnea patients [24].
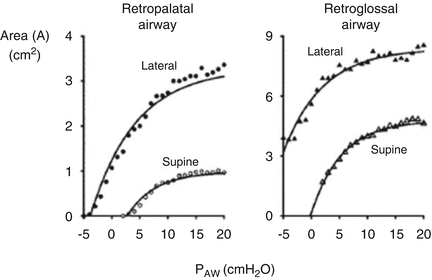

Fig. 2
Static pressure area plot in supine and lateral positions. P AW airway pressure. Figure adapted from Anesthesiology, 2002. 97(4): p. 780–5 [21] with permission
An Australian study that evaluated the critical pressure at which the pharynx collapses in 23 OSA patients noted a significant decrease in the passive pharyngeal collapsibility associated with change from supine to lateral position [25].
There is also a change of shape of the upper airway from the supine to non-supine posture. When anatomical optical coherence tomography was used to scan the upper airway in OSA patients, it was noted that the upper airway changed from a more transversely oriented elliptical shape when supine to a more circular shape in the non-supine position [26]. It was suggested that the increase in circularity has a lesser propensity for tube collapse and this may be responsible for the reduction in obstructive episodes in the non-supine position [26]. Another Chinese study noted that the distance from the velum tip to the pharyngeal wall was narrower in non-positional sleep apnea patients compared to positional sleep apnea patients [27]. Thus, changes in pharyngeal shape, size, and collapsibility all occur when patients shift from the lateral to supine posture promoting a worsening of sleep apnea in the supine posture. The less pronounced these changes are in the non-supine posture, the more likely the patient is to display a clinically significant worsening in the AHI when he/she moves to the supine posture.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree






