, Nima Etminan1 and Daniel Hänggi1, 2
(1)
Neurochirurgische Klinik, Universitätsklinikum Düsseldorf, Düsseldorf, Germany
(2)
Medical Art Christine Opfermann-Rüngeler, Zentrum für Anatomie Heinrich Heine Universität, Düsseldorf, Germany
Peripheral aneurysms fall into three main categories:
Saccular aneurysms located at bifurcations of the postcommunicating artery segments of the anterior or posterior cerebral artery or at bifurcations of the M2 and peripheral segments of the middle cerebral artery
Mycotic or infectious aneurysms
Aneurysms associated with arteriovenous malformations (AVMs)
All distal aneurysms are rare, and knowledge is based on reports of small case series. In addition to these main categories, cases of distal perforator aneurysms, peripheral dissecting aneurysms, and peripheral aneurysms in context with moyamoya disease also have been reported.
Peripheral aneurysms are therefore etiologically a mixed bag. Nonetheless, they share common features of clinical manifestations and therapeutic problems. They often present with intracerebral hemorrhage, sometimes in combination with cerebral infarction. They often have a relatively broad and thick-walled neck, which renders preservation of arterial continuity difficult during surgical or endovascular therapy. The aneurysm commonly needs to be trapped or the parent artery, occluded by the endovascular route, hoping for sufficient collateral flow to the concerned vascular territory. A further common denominator of the peripheral aneurysms is their variable location, calling for individual approaches. Image-guided navigation is mandatory for most peripheral aneurysms.
11.1 Saccular Aneurysms Located at Distal Bifurcations
11.1.1 General Considerations
Aneurysms located at distal bifurcations of the anterior, middle, or posterior cerebral arteries or cerebellar arteries are rare. Together, they appear to account for about 1 % of all aneurysms [1]. Several authors have pointed out that the incidence of multiple aneurysms is substantially higher in patients with distal aneurysms than has been reported in patients with proximal aneurysms, in whom multiplicity is seen in some 20 %. It remains unclear, therefore, whether some of these aneurysms have an infectious embolic origin—i.e., whether some should be classified instead as mycotic aneurysms.
Most often, distal bifurcation aneurysms are relatively small. They present with subarachnoid hemorrhage or intracerebral hematoma or rarely with acute subdural hematoma.
11.1.2 Approach and Clipping
Peripheral aneurysms of the anterior and posterior cerebral arteries lie within the interhemispheric fissure, and those arising from the middle cerebral artery are situated in the Sylvian fissure. Bifurcation-related peripheral aneurysms are rarely encountered on the brain surface. Functioning CSF drainage is important for all procedures involving distal aneurysms located deeply in the interhemispheric or Sylvian fissure, as the surgical approach does not allow early access to CSF spaces to ensure sufficient brain relaxation.
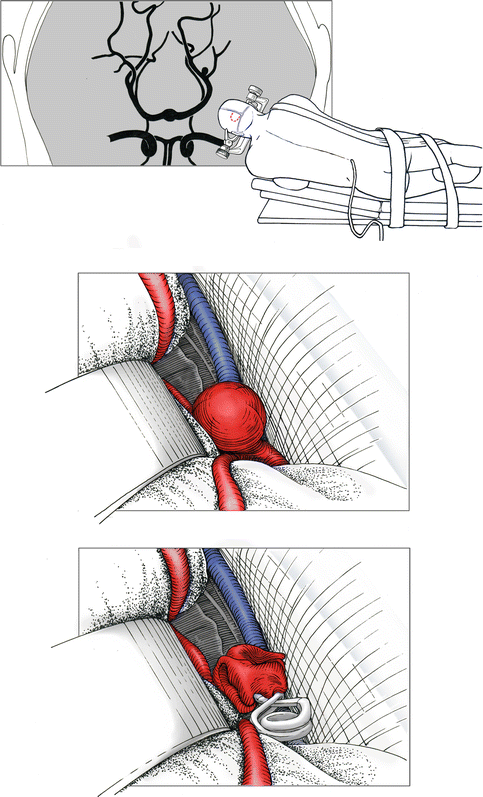
Distal aneurysms of the anterior cerebral arteries are approached via an interhemispheric route, with the patient in a supine position. Distal aneurysms of the posterior cerebral arteries are usually approached via a posterior interhemispheric approach, with the patient in park bench position (Fig. 11.1). Exceptions are aneurysms of the postcommunicating segment of the posterior cerebral artery, which cannot be approached reasonably via the interhemispheric route. We believe that these aneurysms should be approached by an endovascular route whenever possible.