Plexopathies and Myopathies
QUESTIONS
1. A patient presents after a motor vehicle accident (MVA) with right upper extremity weakness and sensory loss. On needle electromyogram (EMG), acute denervation pattern is seen in allmuscles in the shoulder region and the arm, forearm, and hand except serratus anterior and rhomboids. This pattern is seen with:
A. Upper trunk plexopathy
B. Middle trunk plexopathy
C. Lower trunk plexopathy
D. Panplexopathy
View Answer
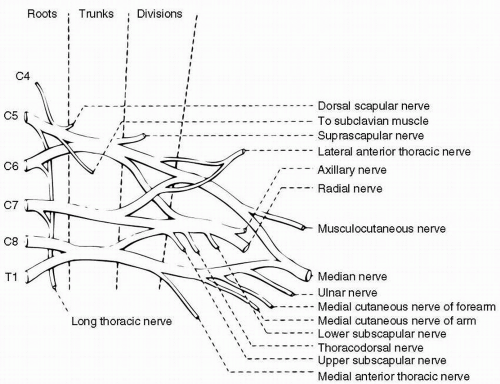
1. (D): A complete brachial plexopathy results in weakness, sensory loss, and decreased or absent reflexes in the entire arm. If the roots remain intact then serratus anterior and rhomboids are usually the only muscles spared because they are innervated by nerves arising directly from the roots. The assessment of these two muscles in often a key, both clinically and electrically, in differentiating a plexopathy from radiculopathy. Cervical root avulsion will result in a denervation pattern in the above two muscles and portends a poor prognosis. (Preston and Shapiro 1998, p. 435)
2. A patient presents after an MVA with right upper extremity weakness and sensory loss. On nerve conduction study, median and radial sensory responses are absent (recorded at thumb) while median and ulnar motor conduction studies and F-responses are normal. Needle EMG shows acute denervation in deltoid and supraspinatus muscles. This pattern is seen with:
A. Upper trunk plexopathy
B. Middle trunk plexopathy
C. Lower trunk plexopathy
D. Panplexopathy
View Answer
2. (A): In upper trunk lesions, the biceps and brachioradialis tendon reflexes are depressed or absent, but the triceps reflex is spared. In addition to nerve conduction studies, median and radial sensory responses are absent or reduced while median and ulnar motor conduction studies and F-responses are normal. Needle EMG abnormalities may involve the deltoid, biceps, brachioradialis, supraspinatus, and infraspinatus. The rhomboids, serratus anterior, and cervical paraspinal muscles are spared. (Preston and Shapiro 1998, p. 443)
3. A patient presents after an MVA with right upper extremity weakness and sensory loss. On nerve conduction study,median sensory studies recorded at themiddle finger and radial sensory responses at the wrist are absent while median and ulnar motor conduction studies and F-responses are
normal. Needle EMG shows denervation pattern in the pronator teres, triceps, and the flexor carpi radialis. This pattern is seen with:
normal. Needle EMG shows denervation pattern in the pronator teres, triceps, and the flexor carpi radialis. This pattern is seen with:
A. Upper trunk plexopathy
B. Middle trunk plexopathy
C. Lower trunk plexopathy
D. Panplexopathy
View Answer
3. (B): Middle trunk lesions are very rare but may affect the median SNAP, especially when recording the middle finger. Because the middle trunk is formed directly of C7 root, it mimics C7 radiculopathy. The radial SNAP may be absent as well. The triceps jerk is depressed or absent. On nerve conduction study, median sensory studies recorded at the middle finger and radial sensory responses at the wrist are absent or reduced, while median and ulnar motor conduction studies and F-responses are normal. The median nerve sensory result will be abnormal when recorded at the thumb or index finger. Needle EMG abnormalities involve C7 innervated muscles, for example, triceps, pronator teres, and flexor carpi radialis. The cervical paraspinal muscles are spared. (Preston and Shapiro 1998, p. 444)
4. A patient presents with a right upper extremity weakness and sensory loss after waking up from coronary bypass graft. On nerve conduction study, ulnar sensory, dorsal ulnar cutaneous and medial antebrachial cutaneous sensory nerve action potential (SNAP), and median and ulnar motor conduction studies and F-responses are absent or abnormal. Radial motor conduction studies are normal. Needle EMG shows denervation pattern in extensor indicis proprius, flexor pollicis longus, and abductor pollicis brevis. This pattern is seen with:
A. Upper trunk plexopathy
B. Middle trunk plexopathy
C. Lower trunk plexopathy
D. Panplexopathy
View Answer
4. (C): Lower trunk is formed from C8 to T1 roots. Lower trunk lesions affect the ulnar sensory, dorsal ulnar, and medial antebrachial cutaneous SNAPs (see Fig. 18.1). Because the median and ulnar innervated hand muscles are derived from the lower trunk, their respective motor conduction studies and F-responses may be abnormal. The radial SNAP and motor conduction studies are normal. The vast majority of these lesions are axonal rather than demyelinating and motor conduction studies may be normal or may show low amplitude. Needle EMG abnormalitiesmay show abnormalities in all ulnar innervated muscles as well as in the median and radial innervated muscles that contain C8-T1 fibers. In pure lower trunk plexopathies, there are no reflex abnormalities. (Preston and Shapiro 1998, p. 444)
5. A patient presents with progressive right medial hand numbness and weakness with claw-like posture of the hand. On nerve conduction study, ulnar, dorsal ulnar and medial antebrachial cutaneous SNAP are abnormal. The right ulnar and median motor conduction studies and F-responses are absent or abnormal. Radialmotor conduction studies are normal. Needle EMG shows a denervation pattern in flexor pollicis longus, flexor carp ulnaris, first dorsal interosseous, and abductor pollicis brevismuscles. This pattern is seen with:
A. Upper trunk plexopathy
B. Middle trunk plexopathy
C. Lateral cord plexopathy
D. Thoracic outlet syndrome.
View Answer
5. (D): True neurogenic thoracic outlet syndrome (TOS) is actually a lower trunk plexopathy. In this entrapment neuropathy, T1 fibers tend to be preferentially affected, leading to a distinctive pattern on nerve conductions and EMG. The median and ulnar motor distal latencies and conduction velocities may be slightly slowed. The median SNAP is normal because the median sensory fibers do not travel through the lower trunk but rather through upper and middle trunks that are not involved in neurogenic TOS. However, ulnar sensory response is abnormal because the ulnar sensory fibers travel through the lower trunk. Needle EMG abnormalities may show abnormalities in median more than ulnar innervated C8-T1 innervated muscles. In pure lower trunk plexopathies, there are no reflex abnormalities. (Preston and Shapiro 1998, p. 444)
6. A patient presents with the acute onset of severe proximal arm and shoulder pain for the last 2 days. Nerve conduction studies show normal median, ulnar, and radial sensory and motor responses. Needle EMG showed normal first dorsal interossei, abductor pollicis brevis, pronator teres, deltoid, biceps, and tricepsmuscle findings. The lesion is likely present in the:
A. Lower trunk plexopathy
B. Axillary nerve
C. Suprascapular nerve
D. Musculocutaneous nerve
View Answer
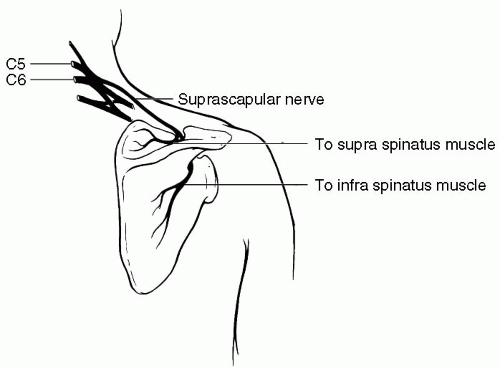
6. (C): Suprascapular nerve comes off the upper trunk of the brachial plexus (see Fig. 18.2). The nerve runs posteriorly under the trapezius, passing through suprascapular notch of the scapula to enter the supraspinus fossa. Suprascapular entrapment most commonly occurs at the suprascapular notch. The pain is typically deep and boring, occurring along the superior aspect of scapula and radiating to the shoulder. Neuralgic amyotrophy often presents with severe proximal arm and shoulder pain and later weakness. In some cases, the suprascapular nerve may be preferentially involved. In lesions at the suprascapular notch, both supraspinatus and infraspinatus are abnormal. In a spinoglenoid lesion only infraspinatus is involved. (Preston and Shapiro 1998, p. 456)
7. All statements regarding needle EMG inmyopathy are correct except:
A. Examination of proximal and distal muscle should be done
B. Muscle biopsy of the muscle, contralateral to the side sampled by the EMG should be done
C. Denervating potentials occur frequently in many myopathic disorders
D. Contractures are associated with acute denervation pattern on needle EMG
View Answer




7. (D): The needle EMG examination must be individualized based on the distribution of patient’s symptoms. Overall, examination of proximal and distal muscle should be done. Sampling the paraspinal muscles is often very useful as most myopathies affect the proximal muscles. As the needle EMG may induce transient inflammatory changes in the muscles, muscle biopsy of the muscle, contralateral to the side sampled by the EMG, should be done. Denervating potentials occur frequently in many myopathic disorders. They are likely secondary to muscle fiber necrosis, inflammation, or irritation near the site of neuromuscular junction (NMJ). The presence of denervating potentials often suggests the diagnosis of inflammatory myopathy. Contractures are associated with complete absence of any electroencephalogram (EEG). (Preston and Shapiro 1998, p. 528)
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree