(1)
St. Anthony’s Neurosurgery Specialists, Saint Louis, MO, USA
Posterior and posterolateral approaches for thoracic disc herniations include (a) laminotomy-facetotomy, (b) transpedicular; and (c) limited costotransversotomy (Fig. 45.1) [1 – 21].
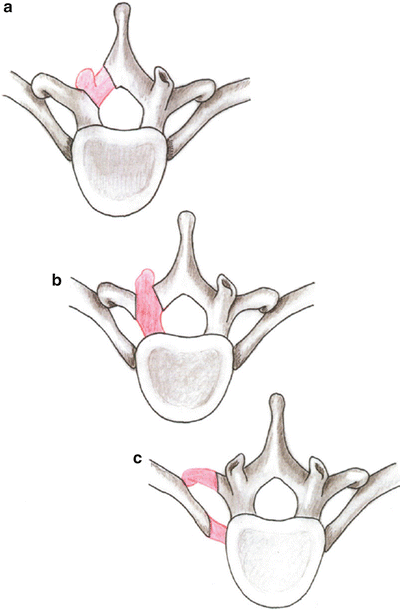

Fig. 45.1
(a) Laminotomy · facetotomy approach. (b) Transpedicular approach. (c) Limited costotransversotomy approach. The red areas represent the segments of the bony elements that are removed in each approach
Caution: Clinically significant thoracic disc herniation is a rare entity (comprising only 0.15 % to 0.8 % of all disc procedures). Degenerative thoracic discs have a tendency to protrude in the midline (or paracentrally) more often than laterally, and the displaced discal material is frequently calcified and adherent to the dura. As a consequence, symptomatic thoracic discs most often place the spinal cord at risk through a combination of acute and chronic compression, dynamic mechanical injury, and intrinsic or radicular vascular insufficiency. As a result, an approach for a specific thoracic disc herniation should be carefully planned so that it is carried out from a direction that accomplishes, for that particular anatomical setting, adequate thecal sac decompression with minimal risk of injury to the spinal cord (Fig. 45.2 ).
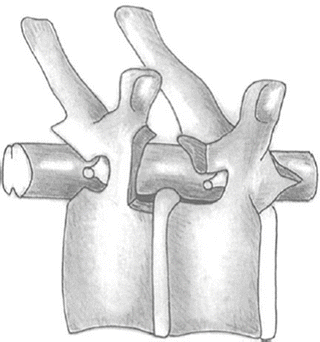

Fig. 45.2
Potential exposure of the spinal canal and disc space afforded by posterior and posterolateral approaches
Procedure
1.
Under general endotracheal anesthesia, the patient is positioned prone on padded chest rolls, rolled blanket bolsters, or a Wilson spinal frame to provide adequate cushioning for the chest and abdomen while allowing vacant space under these areas (thereby promoting epidural venous drainage and adequate pulmonary exchange). The operating table (or Wilson frame) is slightiy flexed, thereby widening the thoracic interlaminar and interpedicular spaces. The knees are placed in 30 degrees of flexion, and support stockings are used to promote venous drainage. Soft foam padding is placed at all pressure points, and special care is taken to avoid pressure on the lateral femoral cutaneous and common peroneal nerves. The head is turned sideways on a foam cushion, with special caution to prevent compression upon the globes. The arms are positioned upward in a relaxed manner with slight shoulder and elbow flexion (care is taken to avoid any traction on the brachial plexus). Padding is placed under the elbows to protect the ulnar nerves in the olecranon grooves. The breasts and genitalia are carefully checked for undue pressure points.
Caution: Appropriate additional support of the patient should be provided so that a small amount of lateral tilt in the operating table away from the surgeon may safely be applied at any point during the procedure. In addition, it is important that the anesthetist be prepared to inflate the lung should the pleura be inadvertently compromised.
2.
The spinous processes, transverse processes, and associated posterior rib tubercles provide helpful superficial landmarks for localization. Using a fingernail (or a marking pen), the surgeon gently indents (or marks) the skin to delineate the intended spinous processes and associated transverse processes and rib tubercles.
Note that heads of the 1st, 11th, and 12th ribs articulate only with their own vertebra whereas the heads of all the other ribs possess two facets and articulate with their own vertebra and the one above (i.e., the 8th rib articulates with both the T7 and T8 vertebrae and crosses the T7–T8 disc space) (Fig. 45.3).
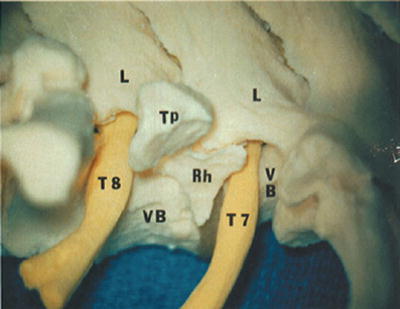

Fig. 45.3
Anatomical relationships. The 8th rib (RH) articulates with both the T7 and T8 vertebrae (VB) and crosses the T7–T8 disc space. (L, lamina; TP, transverse process
An appropriate Betadine skin prep is applied, and 1 g cephalosporin (or when indicated by hypersensitivity, 80 mg gentamicin) is administered intravenously. An 18-gauge spinal needle is inserted off the midline at the suspected appropriate interspinous space, and a lateral radiograph is obtained to confirm the deeper levels of anatomy; this permits the skin incision to be precisely located in relation to the surgical pathology and overlying bony elements. A large percentage of thoracic disc protrusions occur along the lower four thoracic disc spaces (easy to localize); the middle third of the thoracic spine ranks next in frequency; clinically relevant herniations in the upper thoracic spine (where radiographic confirmation of level is often tedious) are fortunately quite rare.
3.
A midline or paramedian incision (3–5 cm in length) centered at the level of the appropriate disc space is utilized medial to or along the paravertebral muscle mass. A symptomatic disc is approached from the side of lateralizing signs or symptoms or from the site of greatest protrusion. In the absence of such indications, a left-sided approach (for the right-handed surgeon) is employed.
Once the incision is made, hemostasis is obtained with bipolar coagulation. A small self-retaining retractor is placed, and the subcutaneous tissues are incised with electrocautery.
Laminotomy-Facetotomy Approach
4.
A curvilinear incision is made in the thoracolumbar fascia 1 cm off the midline and roughly parallel to the supraspinous ligament. A subperiosteal dissection of the paraspinous musculature and tendinous attachments is carried out using a combination of curved periosteal elevators and small Cobb elevators. An open gauze sponge is gently pushed along the spinous processes and laminae to assist in this dissection. The dissection is carried as far lateral as the facet joint. Use caution to avoid penetration of the interspinous or interlaminar ligaments or injury to the facet (especially its synovial membrane) by too vigorous and forceful dissection with periosteal elevators. A self-retaining McCulloch microdiscectomy retractor is inserted.
Caution: The medial prong of the retractor should be positioned carefully between the interspinous ligaments to promote adequate visualization of the interlaminar space.
Caution: Soft tissue remnants overlying the base of the spinous processes, the ligamentum flavum, and laminae are removed when necessary (Fig. 45.4 ).
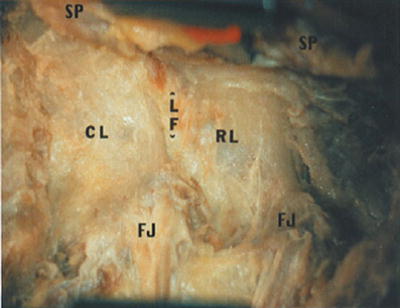

Fig. 45.4
Initial exposure of the interlaminar interval shows the ligamentum flavum (LF), rostral (RL) and caudal-bordering lamina (CL), medial spinous processes (SP), and lateral facet joint complex (FJ)
5.
The initial exposure of the spinal canal is guided by posterior spinal element landmarks, especially the laminae and their relationship to underlying structures (notably the disc space and associated nerve root of interest). The rostral bordering lamina at each level of the thoracic spine overlies the disc space for that respective motion segment. As a result, it is the rostrally bordering lamina at each interlaminar interval that requires removal for exposure of that respective disc space. Adequate exposure of the T7–T8 disc space requires partial or complete removal of the T7 hemilamina. The laminotomy is accomplished (under magnification) with a high-speed bur or rongeur (Fig. 45.5).
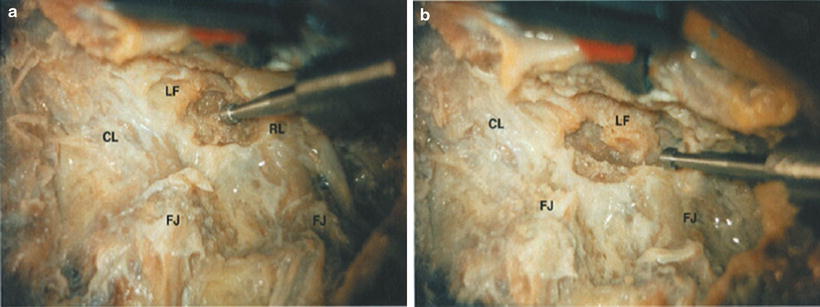

Fig. 45.5
(a) The rostrally bordering lamina (RL) is progressively removed with a high-speed bur. (b) Uncovering the underlying ligamentum flavum (LF)
Caution: Exercise care in the use of the high-speed bur to avoid the presence of any gauze or cottonoids in the wound that may inadvertently catch on the spinning bur and cause a severe whipping injury to surrounding tissues.
6.
The initial removal of the ligament is easiest along its thinner medial aspect. A scalpel can be used to incise the ligament at its apex, and an angled Kerrison rongeur can then be carefully inserted beneath the ligament for removal. On the other hand, enough lamina can be removed such that the rostral margin of the underlying ligamentum flavum is detached, a maneuver that will permit easy access into the epidural space. In this setting, an angled Kerrison rongeur (2 or 3 mm) can be simply utilized to resect the ligament from rostral to caudal (Fig. 45.6). Note that the ligamentum flavum consists of both a horizontal and vertical shelf, such that the ligament thickens as it extends from medial to lateral.
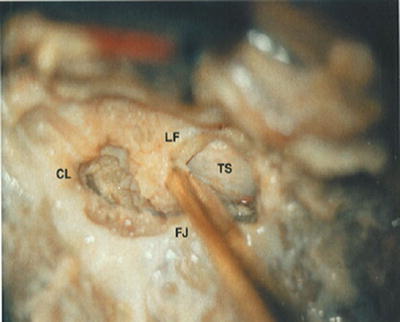

Fig. 45.6
Once the rostral end of the segmental ligamentum flavum (LF) has been unroofed, an angled Kerrison rongeur can be used to progressively resect the ligament in a rostral to caudal direction. TS, thecal sac
7.
Get Clinical Tree app for offline access

Adequate decompression of the thoracic spinal canal always involves the removal of the medial portion of the facet joint. The inferior articular facet is usually removed together with the adjoining lamina. The superior articular facet, on the other hand, is usually removed in conjunction with the vertical shelf of the ligamentum flavum (Fig. 45.7). Adequate removal of the lateral portion of the ligamentum flavum and the medial aspects of the facet joint (particularly the superior articular facet) should permit full visualization (without overhang) of the medial portion of the appropriate pedicle(s) (Fig. 45.8).
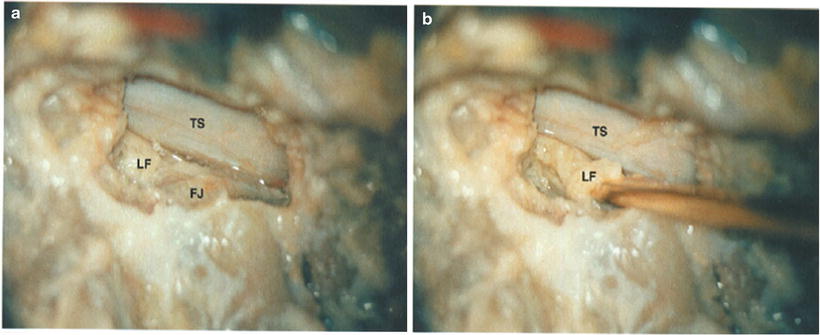
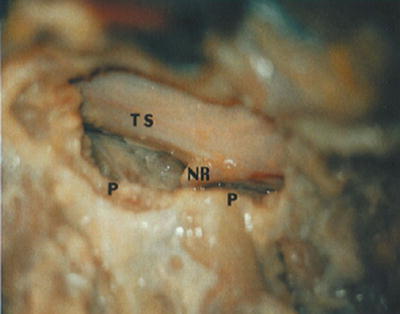

Fig. 45.7
(a) The vertical shelf of the ligamentum flavum (LF) is removed in conjunction with the medial portion of the facet joint (FJ). (b) This step can be accomplished utilizing either a high-speed bur or an angled Kerrison rongeur

Fig. 45.8




Following adequate translaminar facet resection, adequate working space lateral to the thecal sac (TS) and between adjoining pedicles (P) is created. Note the exposure of the exiting nerve root (NR)
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








