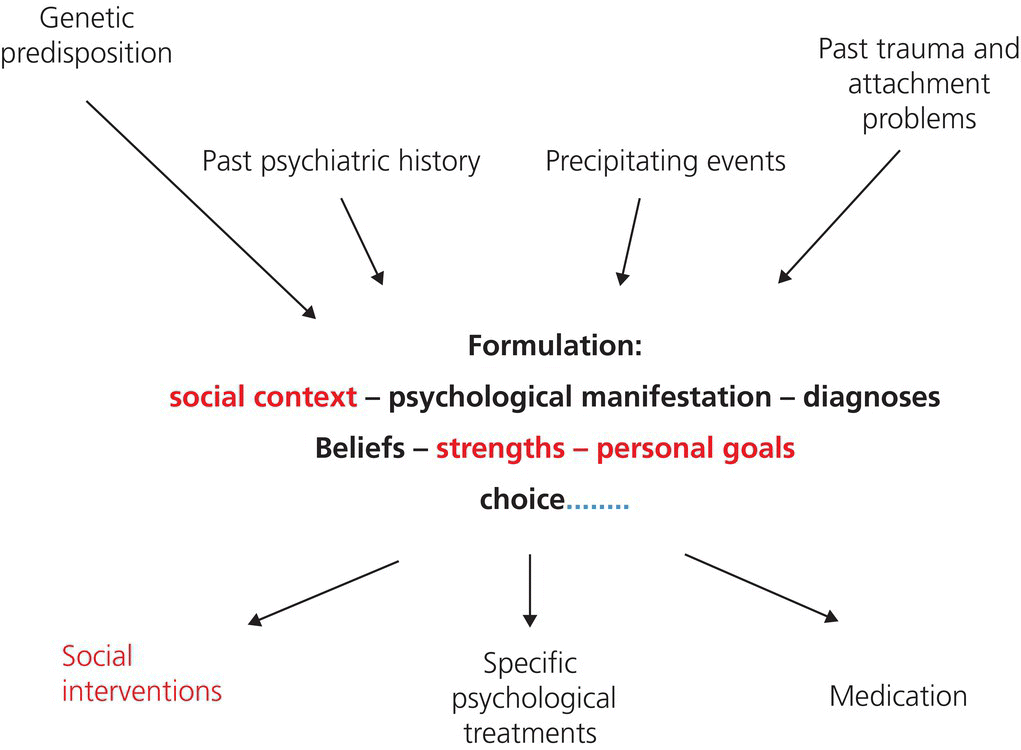
Chapter 9 Richard Byng1 and Judith Forrest2 1 Primary Care Group, Institute of Health Services Research, Plymouth University Peninsula School of Medicine and Dentistry, University of Plymouth, Plymouth, UK 2 Derbyshire Healthcare NHS Foundation Trust, UK This case exemplifies many of the characteristics of those in contact with the criminal justice system who have mental health problems. They often come from socially excluded backgrounds, have ongoing social problems and have a range of symptoms across a number of diagnostic categories, in this case substance misuse as well as anxiety and depression. Patrick’s anxiety includes both fight and flight responses, and he has been using street drugs as self-medication. He does not recognise himself as having a mental illness, or know where he might get help. His self-worth is very low and his trust in everyone, including the health service, has been minimal for many years. At 18, Patrick is probably too young for a diagnosis of personality disorder, which his troubled relationships might suggest, but later it may become a more obvious or defining problem. He would share this difficulty with many offenders. This chapter will outline how, when dealing with individuals like Patrick, either in primary care or within a justice setting, there are particular issues that need to be considered in assessment, treatment and the design of services. Each of these will be taken in turn and background contextual issues are briefly outlined below. Practitioners are often unaware that individuals have contact with the criminal justice system. Offenders may be divided into three groups: those with long prison sentences; short-stay prisoners, including those on remand, who have not been convicted and may be released at any time; and those with community sentences or contact with courts and police. In October 2013 the total prison population in England was over 84 000. While many of these individuals have long sentences, in the year ending March 2013, 57% of convictions were for sentences of 6 months or less, of whom 58.5% were likely to reoffend within 12 months of release. Twenty-six percent of offenders received a non-custodial sentence. Care received varies by setting: general practice and primary care prison services are the mainstays of care for physical health and also for mental health care, mainly in the form of antidepressant prescriptions and fit-notes. Specialist mental health care is provided by in-reach teams in most penal institutions. Substance misuse treatment, which is funded mainly via the Home Office and often provided by a third-sector organisation rather than the NHS, is available to large numbers both in prison and those on community sentences. A small but growing number of prisons have their own Improving Access to Psychological Therapies (IAPT) services, and there is anecdotal evidence to suggest that most community IAPT services are ill equipped to deal with offenders such as Patrick, with comorbid substance misuse and symptoms of anxiety, depression and personality disorder. While distrust and stigma might seem insurmountable problems to initial access, research with offenders in prison and evidence from services set up in selected areas show that in the right situation, offenders are often willing to engage with practitioners, services and treatment. There is compelling evidence to suggest that demonstrating respect, care and concern; reducing talk of mental health or diagnosis; and taking a flexible, problem-solving approach can ensure therapeutic engagement. Box-ticking and heavily protocol-based care with inflexible attitudes are less likely to be successful. We suggest that formulations need to be based on a jointly agreed psychosocial assessment. An individual’s background, including trauma, abandonment and other childhood and adolescent problems is important as is family history. An assessment of mental health symptoms is important to demonstrate whether individuals achieve the criteria for anxiety and depression, but in this group, screening for other problems such as substance and/or alcohol misuse, OCD, PTSD and personality disorder is crucial. We also find that some individuals may barely fulfil the criteria for anxiety and depression but have a range of other problems so that the total symptom load is very great. Many men express emotional turmoil as anger, so it is always key to discover whether this is masking other symptoms, such as underlying fear or feelings of inadequacy. It may be difficult to tease out whether offence-related violence is, at root, an expression of distress. Comorbidity can manifest in a number of ways. Sometimes there are two clear diagnoses that need to be treated in conjunction but with separate interventions (e.g., depression and OCD). More commonly, diagnoses are interrelated in terms of symptoms, meaning and aetiology, and the formulation needs to reflect this. Classification of individuals primarily according to disorder in order to decide a treatment plan may not be the best strategy, and would not reflect collaborative effort between practitioner and client. Furthermore, diagnosis is likely to change over time. Anxiety and PTSD can often be revealed when substance use is reduced, or anxiety might return when depressive symptoms decrease and individuals become more active. In addition, individuals may feel more anxious in the community than in prison, or vice versa: both prison and community may be depressogenic and anxiogenic. Developing a person-centred collaborative formulation should be based around an individual’s personal goals, their strengths and preferred treatment options. Significant social problems such as unemployment, housing and relationship issues are likely to be much higher priority than admitting to having mental health difficulties. Rather than focusing on potentially stigmatising diagnoses it is important to explore the connection between the individual symptoms (thinking, emotions and behaviours) and specific social problems in order to determine whether and how treatment can help a client achieve goals. Assessment of an individual’s strengths requires purposeful questioning. We are constantly surprised at how resourceful patients have been at maintaining their own mental health and any treatment needs to link with existing and potential self-care strategies. Figure 9.1 depicts the elements of a psychosocial formulation diagrammatically and emphasises the social. Figure 9.1 A psychosocial formulation. Source: Psychiatry in Primary Care. Patricia R. Casey and Richard Byng. New York, NY: Cambridge University Press, 2011. Reproduced with permission of Cambridge University Press.
Special Settings: The Criminal Justice System
Background
Assessment and formulation
Special Settings
Only gold members can continue reading. Log In or Register to continue

Full access? Get Clinical Tree




