V 22 Seronegative Spondyloarthropathies 23 Pediatric Cervical Spine Disorders I. Evaluation A. History 1. Pain (localized versus radicular) is the most common chief complaint (85% of patients). a. Other common presenting symptoms include motor weakness (41%) and a palpable mass (16%). 2. Pain secondary to a spinal tumor is typically localized, progressive, unrelenting, nonmechanical, and worse at night. a. Patients do not have relief with rest. 3. Systemic signs and symptoms a. Fevers/chills b. Lethargy c. Unexplained weight loss 4. Neurological symptoms may be present, such as weakness, sensory changes, or bowel and bladder changes. 5. Age may help to narrow the differential diagnosis. a. In older patients, metastasis and multiple myeloma are more common. 6. A history of a primary tumor elsewhere in the body raises the concern of metastases. a. See Table 19–1 for risk factors. B. Physical examination of the spine should include palpation, range of motion, and neurological examination. 1. Neurological examination a. Detailed motor examination b. Sensory examination (1) Light touch (2) Pinprick (3) Vibration (4) Assessment of long tract findings (a) Reflexes 2. Physical examination of potential metastatic foci (Table 19–2)
Miscellaneous
19
Spinal Tumors
| Primary Tumor | Risk Factors |
| Breast cancer | First-degree relative History of increased estrogen exposure (early menarche, late menopause, nulliparity, prolonged hormone replacement therapy) Radiation exposure |
| Prostate cancer | Increased age (>45 y) Bladder outlet obstruction |
| Thyroid cancer | Iodine excess/deficiency Radiation exposure |
| Lung cancer | History of smoking |
| Renal cell carcinoma | Tobacco use |
C. Laboratory studies
1. Helpful in differentiating tumor from infection
a. White blood cell count (WBC), erythrocyte sedimentation rate, and C-reactive protein should all be elevated with infection and normal or slightly elevated with tumor.
(1) Exception is lymphoma, which is associated with an elevated WBC
2. Multiple myeloma is associated with protein spikes on serum or urine analysis.
3. Thyroid-stimulating hormone and free T4 levels are useful in identifying thyroid disease.
4. Prostate specific antigen (PSA) is useful for prostate cancer.
| Primary Tumor | Physical Exam Findings |
| Breast cancer | Hard, fixed, nontender breast mass Nipple retraction Skin erythema or edema |
| Prostate cancer | Large, hard, nodular prostate on digital rectal examination |
| Thyroid cancer | Painless, palpable thyroid |
| Lung cancer | Baseline change in cough Hemoptysis |
| Renal cell carcinoma | Classic triad of hematuria, flank pain, and abdominal mass Tobacco use |
| Imaging Study | Advantages | Disadvantages |
| Plain radiography | Simple screening method Helpful in diagnosis (benign versus malignant) | Low sensitivity (>50% of cancellous bone loss is needed for radiographic identification of bone destruction) |
| Bone scan | Most sensitive tool for metastases (osteoblastic lesions) | Low specificity (cannot differentiate fracture, infection and neoplasm) |
| CT | Best for evaluating bone destruction Important for preoperative planning | Ineffective as a screening tool |
| MRI | High sensitivity especially when used with gadolinium Provides information about soft tissue component Helpful in evaluating spinal cord compression | Extent of cord compression does not consistently correlate with symptoms or outcome |
| Myelography | Good visualization of epidural metastasis and cord compression | Invasive |
| Angiography | Selective embolization of the neoplasm may decrease bleeding during surgery | Invasive |
5. Calcium and phosphate are commonly associated electrolyte abnormalities that may need to be corrected.
6. Radiological evaluation (Table 19–3)
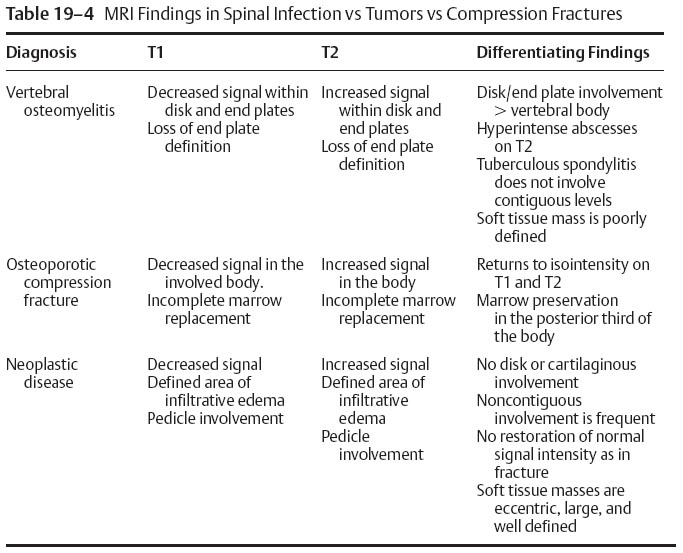
7. Magnetic resonance imaging (MRI) differentiation of infection, fracture, and tumor (Table 19–4)
D. Tumor types
1. See Tables 19–5 to 19–8
E. Staging
1. Weinstein-Boriani-Biagini system
a. Three-dimensional description of tumor invasion
(1) Anatomic zones
(a) Twelve pie-like zones starting at the spinous process and rotating clockwise
(2) Involvement of different vertebral layers
(a) Extraosseous soft-tissue
(b) Intraosseous (superficial)
(c) Intraosseous (deep)
(d) Extraosseous (extradural)
(e) Extraosseous (intradural)
(3) Specification of the spinal segment(s) involved
F. Treatment
1. Goals
a. Establishment of a definitive diagnosis
b. Maintenance of neurological function