Stroke
 Cerebrovascular Hemodynamics
Cerebrovascular Hemodynamics
1. Complete the following: |
| G7 p.1010:100mm |
a. Cerebral blood flow (CBF) less than_____mL per 100 g of tissue per minute is associated with ischemia. | 20 mL |
|
b. If prolonged, it will result in_____. | cell death |
|
2. Electroencephalography (EEG) becomes flat line at CBF of_____mL/100 g/min. | 16 to 18 | G7 p.1010:150mm |
3. Complete the following about strokes in general: |
| G7 p.1010:163mm |
a. What is the range of cerebral perfusion pressure in which cerebral blood flow is maintained constant despite changes in cerebrovascular resistance? | 50 to 150 mm Hg |
|
b. This is called_____. | autoregulation |
|
4. Complete the following about strokes in general: |
| G7 p.1010:175mm |
a. CMRO2 stands for_____and | cerebral metabolic rate of oxygen consumption |
|
b. averages_____. | 3.0 to 3.8 mL/100 g of tissue per minute |
|
5. Complete the following regarding abrupt onset of new focal deficit caused by: |
| G7 p.1011:60mm |
a. tumor/seizure_____% | 5% |
|
b. ischemic infarct_____% | 85% |
|
c. hemorrhagic infarct_____% | 15% |
|
d. mortality_____% | 25% |
|
e. nursing home_____% | 25% |
|
f. home_____% | 50% | |
6. True or False. The following is a cause of ischemic infarcts: |
| G7 p.1011:75mm |
a. lacune | true |
|
b. large artery embolism | true |
|
c. cardiogenic embolism | true |
|
d. aortic arch plaques | true |
|
7. Modifiable risk factors for stroke include |
| G7 p.1011:120mm |
a. c_____ | cigarettes |
|
b. a_____ | alcohol |
|
c. h_____ | hypertension |
|
d. l_____ | lipids |
|
e. a_____ | antiplatelets |
|
8. Computed tomographic (CT) scan signs of early ischemia include |
| G7 p.1012:110mm |
a. i_____ | insular ribbon lost |
|
b. s_____ | shift of midline day 1 to 25 |
|
c. c_____ | calcification almost never 1 to 2% |
|
d. h_____ | hyperdense artery sign |
|
e. e_____ | effacement of cerebral sulci |
|
f. m_____ | mass effect |
|
g. i_____ | interface of gray-white lost |
|
h. c_____ | contrast CT should be included on at least one occasion |
|
9. True or False. The following can be early CT findings of ischemic strokes: |
| G7 p.1012:125mm |
a. midline shift | true |
|
b. loss of gray-white interface | true |
|
c. hyperdensity of lentiform nucleus | false (Attenuation of the lentiform nucleus may be seen.) |
|
d. enhancement of ischemic area | true (One third of ischemic strokes may enhance early.) |
|
e. normal CT | true |
|
f. hyperdense artery sign | true (usually MCA) | G7 p.1013:40mm |
10. Is there CT enhancement with intravenous (IV) contrast in cerebrovascular accidents (CVAs) in the presence of mass effect? | no (As a rule of thumb there should not be.) | G7 p.1013:55mm |
11. MRI sequences in stroke are |
| G7 p.1013:160mm |
a._____ represents dead tissue. | DWI |
|
b._____ represents penumbra. | PWI |
|
c. Penumbra is potentially s_____tissue. | salvageable | |
12. Components of luxury perfusion are |
| G7 p.1014:35mm |
Hint: ischemia |
|
|
a. i_____ | ischemia |
|
b. “s”_____ | “s” idosis (acidosis) |
|
c. c_____ | CO2 rises |
|
d. h_____ | hyperemia |
|
e. e_____ | enlargement (dilation) of vessels |
|
f. m_____ | mechanism of luxury perfusion |
|
g. i_____ | increase blood flow |
|
h. a_____ | accelerated circulation adjacent to an infarct |
|
13. Explain the mechanism of luxury perfusion. |
| G7 p.1014:40mm |
a. Ischemia produces_____, | acidosis |
|
b. which causes an_____in PCO2. | increase |
|
c. What does this do to regulation? | loss of autoregulation |
|
d. It results in_____vessels | dilated |
|
e. and blood flow_____called _____. | excess; hyperemia |
|
f. What happens to blood flow adjacent to an infarct? | it becomes accelerated |
|
14. t-PA works by |
| G7 p.1016:145mm |
a. converting p_____ | plasminogen |
|
b. to the fibrinolytic compound_____. | plasmin |
|
c. The primary agent is a_____. | alteplase |
|
15. Complete the following regarding the use of recombinant tissue plasminogen activator (rt-PA) compared with control groups: |
| G7 p.1016:175mm |
a. reduction in stroke_____% | 30% |
|
b. recurrent stroke rate_____% | 5%—same in both groups |
|
c. mortality_____ vs_____% | 17 vs 21% |
|
d. hemorrhage (NINDS study)_____ vs _____% | 6.4 vs 0.6% |
|
e. hemorrhage ECASSII study_____ vs _____% | 8.8 vs 3.4% |
|
f. benefit at 90 days in mortality_____ _____ | no difference | |
16. Facts learned from the ECASS-3 study of t-PA include |
| G7 p.1017:16mm |
a. Extended the window of IV treatment to_____ hours | 4.5 |
|
b. Improved outcome at 90 days by_____% | 7.2% |
|
c. |
|
|
i. Incidence of hemorrhage _____% | 7.9% |
|
ii. And_____% for placebo | 3.5% |
|
d. |
|
|
i. Yet no increase in death rate t-PA _____% | 7.7% |
|
ii. Placebo_____% | 8.4% |
|
e. For every 100 patients treated with t-PA |
|
|
i._____ will benefit | 32 |
|
ii. _____ will be harmed | 3 |
|
17. True or False. The following would exclude a patient with ischemic stroke from treatment with tissue plasminogen activator (t-PA): |
| G7 p.1017:70mm |
a. systolic blood pressure (SBP) 180 mm Hg | false (SBP above 185 disqualifies.) |
|
b. gastrointestinal (GI) bleed 6 months ago requiring transfusion | false (GI bleed within 21 days disqualifies.) |
|
c. platelet count 120,000/mm3 | false (Below 100,000 disqualifies.) |
|
d. hip arthroplasty 10 days ago | true (Major surgery within 14 days of an ischemic stroke is a contraindication for t-PA treatment.) |
|
e. blood glucose 250 mg% | false (Above 400 mg% disqualifies.) |
|
18. Complete the following about the management of post-t-PA intracerebral hemorrhage: |
| G7 p.1018:15mm |
a. Stop_____. | t-PA |
|
b. Obtain stat_____. | CT |
|
c. Send labs for PT, PTT, platelet and _____. | fibrinogen |
|
d. Prepare to administer |
|
|
i. 6 to 8 units of c_____ | cryoprecipitate |
|
ii. 6 to 8 units of p_____ | platelets |
|
e. Consider use of_____ _____. | factor VII |
|
19. Intra-arterial t-PA may be used up to_____hours after stroke onset. | 6 | G7 p.1018:48mm |
20. Merci retriever |
| G7 p.1018:48mm |
a. stands for mechanical embolus removal in_____. | cerebral ischemia |
|
b. It can be used for up to_____hours. | 8 |
|
c. It has a recanalization rate of_____%. | 48% | |
21. Complete the following about strokes in general: |
| G7 p.1018:165mm |
a. After a stroke you must monitor electrocardiography (EKG) because |
|
|
i. _____% have EKG changes | 5 to 10% |
|
ii. _____% have myocardial infarction (MI) | 2 to 3% |
|
b. You must avoid hyperglycemia because hyperglycemia |
|
|
i. _____ the ischemia zone, also known as the | extends |
|
ii. _____. | penumbra |
|
22. Complete the following regarding hypertension treatment: |
| G7 p.1019:120mm |
a. If diastolic blood pressure (DBP) is above_____ it is called malignant hypertension. | 140 mm Hg |
|
b. Decreasing by_____% to DBP of_____is desirable. | 20 to 30% (112 to 98 mm Hg) |
|
c. If SBP is above 230 or DBP is above 120 decrease to SBP of_____or DBP of_____. | 180; 110 |
|
d. For SBP of 180 to 230 or DBP of 105 to 120 decrease n_____n_____e_____. | not needed emergently |
|
e. For SBP of less than_____or DBP of less than_____ antihypertensive treatment is not needed. | 180; 105 |
|
f. Approximately_____ /_____ is acceptable. | 180/100 |
|
g. Add_____if there is a history of hypertension. | 5 |
|
23. Complete the following: |
| G7 p.1020:40mm |
a. Incidence of recurrent ischemic strokes in the week following a CVA is _____%. | 2.2% |
|
b. Is it any less if you use heparin? | no |
|
i. except in_____ | cardiogenic emboli |
|
c. Complication rate of heparin |
|
|
i. symptomatic intracerebral hemorrhage (ICH) occurs in_____% | 1 to 8% |
|
ii. conversion of pale to hemorrhagic CVA_____% | 2 to 5% |
|
iii. other bleeding complications_____% | 3 to 12% |
|
d. On balance is it justified to use heparin after an ischemic CVA? | no |
|
i. The American Heart Association states that the_____decides. | doctor | |
24. Complete the following regarding the use of anticoagulants (heparin or warfarin): |
| G7 p.1020:40mm |
a. True or False. They are effective in the prevention of embolic strokes caused by cardiogenic embolism. | true |
|
b. True or False. They are effective in ischemic strokes. | false |
|
c. They have a risk of hemorrhage of_____% per year. | 1 to 8% |
|
d. They will convert pale to hemorrhagic CVA in_____%. | 2 to 5% |
|
25. CVA and anticoagulation are generally used for |
| G7 p.1020:115mm |
a. c_____ e_____. | cardiogenic emboli |
|
b. c_____ d_____. | carotid dissection |
|
c. Complications are worse if the patient has_____. | hypertension |
|
d. How do you start the drugs? (heparin/warfarin) | simultaneously |
|
i. Why? Because of initial_____. | hypercoagulability |
|
e. Stop warfarin after_____. | 6 months |
|
f. Why? | reduced benefits, increased risks |
|
26. True or False. Regarding cerebellar infarction: |
| G7 p.1021:30mm |
a. Hydrocephalus may occur. | true |
|
b. Surgery is appropriate even if patient is in coma. | true (Patient may respond even if in deep coma.) |
|
c. Steroids should be used. | true (Steroids are suggested for cerebellar stroke.) | G7 p.1020:145mm |
d. Ventricular drainage should be used. | false (Is to be avoided; it might cause upward herniation.) |
|
e. Incidence of cerebellar infarction is less than 1%. | true (It is seen on 0.6% of all CT scans.) |
|
27. Cerebellar infarction of the |
| G7 p1021:30mm |
a. tonsil implicates the_____ | PICA |
|
b. inferior vermis implicates the_____ | PICA |
|
c. superior hemisphere implicates the_____ | SCA |
|
d. superior vermis implicates the_____ | SCA |
|
28. True or False. The following may be a late finding in patients with cerebellar infarctions that may prompt surgical decompression: |
| G7 p.1021:105mm |
a. sixth nerve palsy | true |
|
b. seventh nerve palsy | true |
|
c. worsening headache | true | |
d. Horner syndrome | false (The late findings in a cerebellar infarction are from hydrocephalus or brain stem compression. Horner syndrome is typically seen with lateral medullary syndrome and is due to an intrinsic brain stem lesion and is not an indication for surgery.) |
|
e. decreased level of consciousness | true |
|
29. Surgical decompression is appropriate if patient develops: |
| G7 p.1021:105mm |
a. True or False. Coma | true |
|
b. True or False. Ataxic respiration | true |
|
c. Loss of lateral gaze implicates_____nerve. | sixth |
|
d. Paresis of face implicates_____ _____. | facial colliculus |
|
e. Confusion and somnolence implicates_____ _____. | hydrocephalus |
|
30. With MCA infarction, consider hemicraniectomy if |
| G7 p.1022:85mm |
a. distribution of infarct is in the_____territory | middle cerebral artery (MCA) |
|
b. age of the patient is_____ | under age 70 |
|
c. if CVA is on the_____side | right (nondominant) |
|
d. it may reduce mortality from_____to_____% | 80 to 30% |
|
31. Demographics of cardiogenic stroke include |
| G7 p.1022:140mm |
a. incidence of_____ | 1 in every 6 strokes (i.e., ˜17%) |
|
b. after MI_____% in 2 weeks | 2.5% |
|
c. anterior wall_____% | 6% |
|
d. inferior wall_____% | 1% |
|
e. atrial fibrillation_____% per year without treatment | 4.5% |
|
f. especially if patient has_____ventriculomegaly | left |
|
g. due to_____ _____ | atrial thrombosis | G7 p.1022:165mm |
h. heart valve prostheses with anticoagulation |
|
|
i. mitral_____% per year | 3% |
|
ii. aortic_____% | 1.5% |
|
iii. without anticoagulation_____% per year | 2 to 4% | |
32. Complete the following about paradoxical embolus: |
| G7 p.1023:55mm |
a. Population incidence of patent foramen ovale is _____%. | 10 to 18% |
|
b. In patients with unexplained CVA, the incidence is _____%. | 56% |
|
33. Complete the following about a cardiogenic brain embolism: |
| G7 p.1023:100mm |
a. Transformation from bland to hemorrhagic infarct may occur within_____. | 2 days (48 hours) |
|
b. Based on what three-step mechanism? |
|
|
i. i_____ | ischemia |
|
ii. c_____ l_____ | clot lysis |
|
iii. r_____ | reperfusion of the infarcted brain |
|
c. If transformation occurs you can surmise that indeed this large infarction can be attributed to a_____ _____. | cardiac cause |
|
34. Complete the following: |
| G7 p.1023:145mm |
a. What is the only stroke for which anticoagulation is beneficial? | cardiogenic brain embolism |
|
b. What does anticoagulation accomplish regarding further CVAs? | reduces the incidence |
|
c. The natural risk without treatment is_____%. | 12% |
|
d. If used, when should anticoagulation be instituted? | not before 48 hours |
|
e. The size of the infarct should be_____. | not a large one |
|
f. Aim for an international normalized ratio (INR) of_____. | 2 to 3 |
|
g. Coumadin reduces stroke risk in atrial fibrillation by_____%. | 66 to 86% |
|
35. True or False. Anticoagulation should be initiated immediately after detection of stroke caused by cardiogenic embolism. | false (After 48 hours is the proper time. Hemorrhagic conversion is more likely to occur with cardiogenic embolic strokes and is most likely to occur within 48 hours of the stroke. A CT scan should be obtained 48 hours after the stroke and before the initiation of anticoagulation.) | G7 p.1023:165mm |
 Strokes in Young Adults
Strokes in Young Adults
36. Complete the following about strokes in young adults: |
| G7 p.1024:45mm |
a. Incidence of all strokes |
|
|
i. Under age 40: _____% | 3 |
|
ii. Under age 55: _____% | 10 |
|
b. Etiologies |
|
|
Hint: mA3 pc3 le2 hv |
|
|
i. m_____ | migraine |
|
ii. al_____ | alcohol |
|
iii. AP_____ | APLAS |
|
iv. ar_____ | arteriosclerosis |
|
v. p_____ | peripartum |
|
vi. coa_____ | coagulopathy |
|
vii. coc_____ | cocaine |
|
viii. con_____ | contraceptives |
|
ix. l_____ | lupus |
|
x. ec_____ | ecstasy |
|
xi. em_____ | embolism |
|
xii. h_____ | homocystinuria |
|
xiii. v_____ | vasculitis |
|
c. Incidence of main etiologies |
|
|
i. arterio-sclerosis _____% | 20% |
|
ii. embolism _____% | 20% |
|
iii. vasculitis _____% | 10% |
|
iv. coagulopathy_____ % | 5% |
|
 Lacunar Strokes
Lacunar Strokes
37. Complete the following about lacunar infarcts: |
| G7 p.1026:50mm |
a. size of infarct_____ | 3 to 20 mm |
|
b. size of artery involved_____ | less than 200 μm in diameter |
|
c. due to_____ | lipohyalinosis |
|
d. related to_____ | hypertension |
|
e. L’etat Lacunaire is_____ _____. | multiple lacunae |
|
f. Small-step gait is called_____ _____ _____ _____. | marche á petits pas |
|
38. What is Dejerine-Roussy syndrome? |
| G7 p.1026:105mm |
a. The patient complains of_____ | pain |
|
b. The area of the brain involved is_____, | thalamus |
|
c. specifically the_____ _____ | posteroventral nucleus |
|
d. due to a_____ infarct. | lacunar (Rare thalamic pain syndrome develops long after a lacunar infarct in the posteroventral [sensory] thalamus.) | |
39. Name the lacunar syndrome sites. |
| G7 p.1026:115mm |
a. pure sensory_____ | posterior ventral thalamus |
|
b. pure motor_____ | posterior limb of internal capsule |
|
c. ataxia hemiparesis_____ | basis pontis |
|
d. top of the basilar_____ | mesencephalothalamic |
|
e. Weber_____ | third-nerve palsy and contralateral hemiparesis (cerebral peduncle and issuing fibers of third nerve) |
|
f. hemiballismus_____ | subthalamic nucleus of Luys |
|
g. Wallenberg_____ | posterior inferior cerebellar artery (PICA)—vertebral artery |
|
40. Concerning lacunar infarcts, give the symptoms, anatomic site, and distinguishing comment for the listed syndromes. |
| G7 p.1026:120mm |
a. pure sensory |
|
|
i. symptom: f_____, a_____, l_____ n_____ | face, arm, leg numbness |
|
ii. anatomic site: PVT | PV thalamus |
|
iii. comment: (first) | most common lacuna |
|
b. pure motor |
|
|
i. symptom: f_____, a_____, l_____ | face, arm, leg |
|
ii. anatomic site: PL-IC | posterior limb of IC |
|
iii. comment: (second) | second most common |
|
c. ataxia hemiparesis |
|
|
i. symptom: a_____ | ataxia |
|
ii. anatomic site: PL-IC | basis pontis (midbrain) |
|
iii. comment: (lips) | numb lips |
|
d. top of the basilar (mesencephalothalamic) |
|
|
i. symptoms: t_____ n_____ p_____, P_____, a_____ | third nerve palsy, Parinaud, abulia |
|
ii. anatomic site: b_____ p_____ | basis pontis (midbrain) |
|
iii comment: b_____ s_____ | butterfly shape |
|
e. Weber |
|
|
i. symptoms: t_____ n_____ p_____, m_____ w_____ | third nerve palsy, motor weakness |
|
ii. anatomic site: i_____ a_____ to the m_____ | interpeduncular arteries to the midbrain |
|
iii. comment: b_____ a_____ | basilar aneurysm | |
41. True or False. The following is part of the “top of the basilar” syndrome: |
| G7 p.1026:160mm |
a. third nerve palsy | true |
|
b. amnesia | true |
|
c. light-near dissociation | true |
|
d. vertical gaze impairment | true |
|
e. dysarthria, clumsy hand | false (Dysarthria—clumsy hand syndrome—occurs with lacunar infarction of the basis pontis or genu of the internal capsule.) |
|
42. Matchin. Match the following regarding MCA occlusion and symptoms. |
| G7 p.1028:25mm |
Area of MCA occlusion: |
|
|
|
|
|
Symptoms: |
|
|
a. homonymous hemianopsia |
|
|
b. aphasia |
|
|
c. paresis |
|
|
d. hemi-sensory loss |
|
|
43. True or False. Complete the following regarding inferior division MCA occlusion: |
| G7 p.1028:25mm |
a. Patient’s visual fields will be normal. | false |
|
b. Patient’s speech will be normal. | false |
|
c. Patient will have hemiparesis. | false |
|
d. Patient will have sensory deficit. | false |
|
 Miscellaneous CVA
Miscellaneous CVA
44. Complete the following about the Huebner artery: |
| G7 p.1028:121mm |
a. also known as the r_____ a_____ | recurrent artery |
|
b. also known as m_____ s_____ a_____ | medial striate artery |
|
i. arises from A2 in _____% of patients | 78% |
|
ii. arises from A1 in _____% of patients | 14% |
|
iii. arises from anterior communicating artery (A-comm) in_____% of patients | 8% |
|
iv. arises within_____ mm of the A-comm junction | 5 mm |
|
c. diameter is_____ mm: mean range _____ to _____ | 1 mm: mean range 0.2 to 2.9 mm |
|
d. diameter compared with diameter of A1 is_____ | one third | |
e. may be confused at surgery with the_____ artery | orbitofrontal artery (second branch of A2—arises 5 mm or more from A-comm junction) |
|
f. supplies: |
|
|
Hint: capghal |
|
|
i. ca_____ | caudate |
|
ii. p_____ | putamen |
|
iii. g_____ p_____ | globus pallidus |
|
iv. h_____ | hypothalamus |
|
v. a_____ l_____ | anterior limb of internal capsule |
|
45. Describe the syndrome of occlusion of the recurrent artery of Huebner. |
| G7 p.1028:123mm |
Hint: Huepb |
|
|
a. h_____ | hemiparesis (mild) |
|
b. u_____ | upper extremity—weaker than lower |
|
c. e_____ | expressive aphasia |
|
d. p_____ | proximal muscles—weaker than distal |
|
e. b_____ | A2 segment of origin 78% |
|
46. Complete the following: |
| G7 p.1028:125mm |
a. Occlusion of the anterior choroidal artery produces infarct in the_____ limb of the internal capsule. | posterior |
|
b. The Huebner artery produces infarct in the_____ limb of the internal capsule. | anterior |
|
47. Occlusion of the anterior choroidal artery causes |
| G7 p.1028:125mm |
a. c_____ h_____ | contralateral hemiplegia |
|
b. c_____ h_____ | contralateral hypesthesia |
|
c. c_____ h_____ h_____ | contralateral homonymous hemianopsia |
|
48. Complete the following about Wallenberg syndrome: |
| G7 p.1028:155mm |
a. also known as l_____ m_____ s_____ | lateral medullary syndrome |
|
b. also known as P_____ s_____ | PICA syndrome |
|
c. but most related to _____ artery | vertebral | |
d. Give the structure involved and the symptoms: |
|
|
i. structure: v_____ n_____ | structure: vestibular nucleus; |
|
symptoms: v_____, n_____ and v_____, n_____ | symptoms: vertigo, nausea and vomiting, nystagmus |
|
ii. structure: v_____ and g_____ n_____ | structure: vagus and glossopharyngeal nerve; |
|
symptoms: d_____, h_____ | symptoms: dysphagia, hoarseness |
|
iii. structure: n_____ of_____ | structure: nucleus of V; |
|
symptoms: f_____ p_____, p_____ | symptoms: facial pain and paresthesias |
|
iv. structure: r_____ b_____ | structure: restiform body; |
|
symptom: l_____ a_____ | symptom: limb ataxia |
|
v. structure: s_____ t_____ | structure: sympathetic tract; |
|
symptom: H_____ | symptoms: Horner |
|
vi. structure: s_____ t_____ | structure: spinothalamic tract; |
|
symptoms: c_____ p_____ and t_____ l_____ | contralateral pain and temperature loss |
|
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


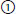 complete MI;
complete MI; 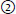 superior division;
superior division; 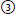 inferior division
inferior division ,
, 
 ,
, 
 ,
, 
 ,
,