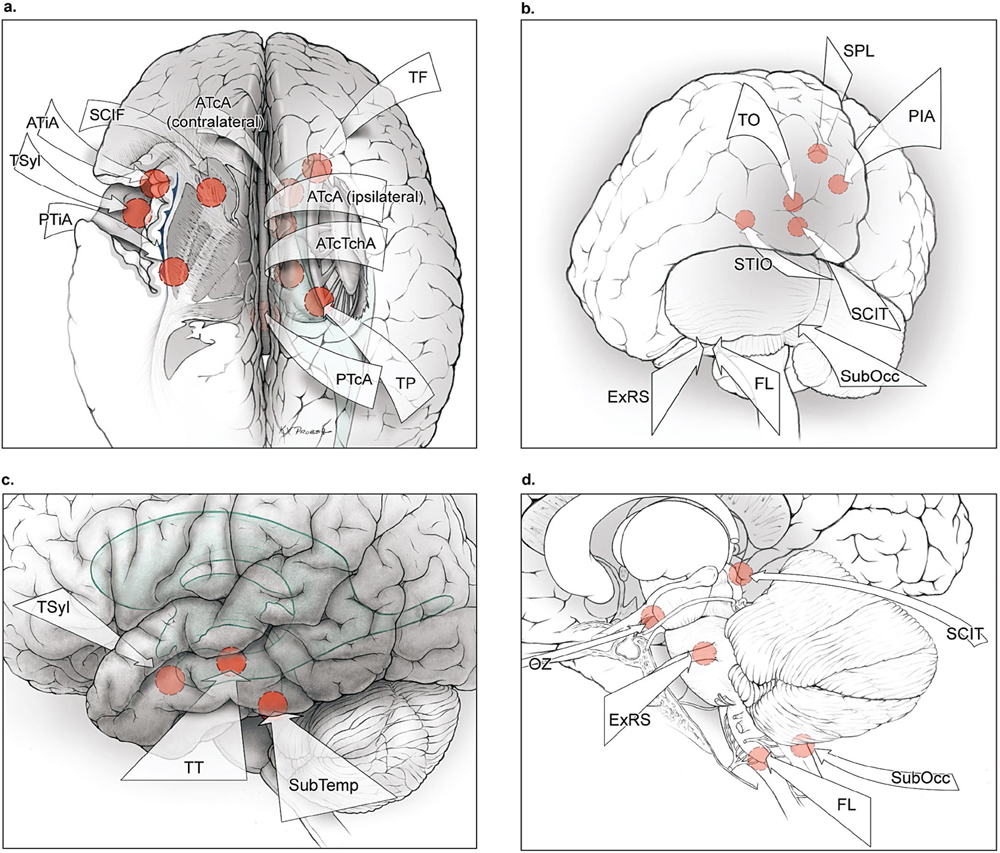
2 Subarachnoid Dissection Subarachnoid dissection is the calm before the clash, when the arteriovenous malformation (AVM) is approached, encountered, and surveyed under the microscope without salvo. The labyrinth of subarachnoid spaces around the AVM is splayed, deconstructing arachnoid membranes, disconnecting interlobular trabeculae, and intercommunicating cisternal compartments. Cerebrospinal fluid (CSF) drainage slackens and shifts the cerebral terrain. Misshapen feeding arteries and distorted draining veins are inspected, with their unusual features offering clues to their angiographic identity. Subarachnoid dissection transforms the brain’s natural landscape into the surgical field, a battlefield, with AVM surfaces laid bare, fissures opened widely, and anatomic landmarks in sight. This phase of AVM surgery is like aneurysm surgery, with microdissection that is clean and extrapial, and that can be savored as a time of reconnaissance without confrontation. The subarachnoid approach can be short with superficial AVMs on a cortical surface or long with deep AVMs in central or ependymal locations (Fig. 2.1). Superficial approaches to convexity AVMs require minimal subarachnoid dissection because the AVM is based right on the cortical surface (transfrontal, transtemporal, and transparieto-occipital approaches, Table 2.1). Intermediate approaches require more subarachnoid dissection down a fissure such as the sylvian and interhemispheric fissures or along a basal or dural plane (transsylvian, medial interhemispheric, and basal approaches, Table 2.1). Deep approaches are forays to the bottom of these fissures and beyond, through the corpus callosum, ventricles, and choroidal fissures, and along the skull base or tentorial planes (transcallosal, transchoroidal, and posterior fossa approaches, Table 2.1). Although superficial AVMs are easily localized on their free surface, they are often concealed in arachnoid thickened by microhemorrhages, chronic inflammation, radiosurgery, or prior embolization. An opaque white veil must first be opened to reveal the AVM’s anatomy. Distended veins are freed from their arachnoidal investments and peeled back to expose AVM margins. Hemorrhage, both new and old, stains adjacent surfaces with hemosiderin and presents a trail to fresh clot, liquefied hematoma, or encephalomalacia. Hemorrhage can create extra-anatomic cavities that often connect with subarachnoid spaces. Some AVM margins separate from adjacent brain as a subarachnoidal plane, often following gyral contours into a sulcus. An example is the pure sylvian AVM, which sits entirely in the sylvian fissure without invading frontal, temporal, or insular parenchyma, and can be circumdissected completely with subarachnoid dissection and without subpial invasion. Other than these cerebral and cerebellar convexity AVMs that are superficial and immediately apparent on brain surface, the rest require more dissection to expose the AVM. Transsylvian approaches expose eight lateral and deep AVM subtypes; interhemispheric approaches expose eight medial and deep subtypes; skull base approaches expose eight basal, brainstem, and cerebellar subtypes; and transtorcular approaches expose six posterior, cerebellar, and brainstem subtypes (Table 2.2). All of these AVMs have their base on a surface buried in a fissure that must be opened, or along a basal plane that does not face the axis of the approach. The initial survey of the brain after dural opening may reveal only an arterialized vein or nothing abnormal at all. Consequently, these AVMs require bilateral craniotomies, gravity retraction, or transventricular access. These buried AVMs are localized by following arterialized veins around corners and into fissures, maneuvering around and deep to these dilating veins, and separating adhesions to the falx, tentorium, or skull base. For the deepest approaches, subarachnoid dissection extends further into ventricles or deep cisterns around the brainstem to reach the AVM base and optimize the angle of attack. At such depths, the AVM axis and angle of attack are often perpendicular, and expanding the surgical corridor with extensive dissection can improve visualization and maneuverability in the working channel. Fig. 2.1 Summary of surgical approaches to brain AVMs. (a) Medial interhemispheric and lateral transsylvian approaches to supratentorial AVMs (superior view). (b) Posterior and posterolateral approaches to supra- and infratentorial AVMs (posterior oblique view). (c) Lateral approaches to temporal AVMs (lateral view). (d) Approaches to brainstem AVMs (lateral view). Medial interhemispheric approaches include the anterior interhemispheric approach (AIA); posterior interhemispheric approach (PIA); anterior transcallosal approach (ATcA, ipsilateral and contralateral); anterior transcallosal-transchoroidal approach (ATcTchA); and posterior transcallosal approach (PTcA). Lateral transsylvian approaches include the transsylvian approach (TSyl), anterior transinsular approach (ATiA), posterior transinsular approach (PTiA), and supracarotid-infrafrontal approach (SCIF). Transcortical approaches are used instead of subarachnoid and transventricular routes when hematomas or encephalomalacia create direct, nonanatomic corridors to deep AVMs and include transfrontal (TF), transtemporal (TT), transparietal (TP), transoccipital (TO), and superior parietal lobule (SPL) approaches. Brainstem approaches include the orbitozygomaticpterional approach (OZ), supracerebellar-infratentorial approach (SCIT), extended retrosigmoid approach (ExRS), far lateral approach (FL), and suboccipital-transventricular approach (SubOcc). Additional posterior approaches include the supratentorial-infraoccipital approach (STIO).
 Reconnaissance
Reconnaissance
 Approaches
Approaches
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree