Fig. 3.1
Right superficial middle cerebral artery infarction: hyperintense signal on diffusion-weighted imaging (a and b) with embolic material from irregular stenosis of the right carotid artery (c, cerebral MR angiography: hollow arrow). Surgically revascularized stenosis (d)
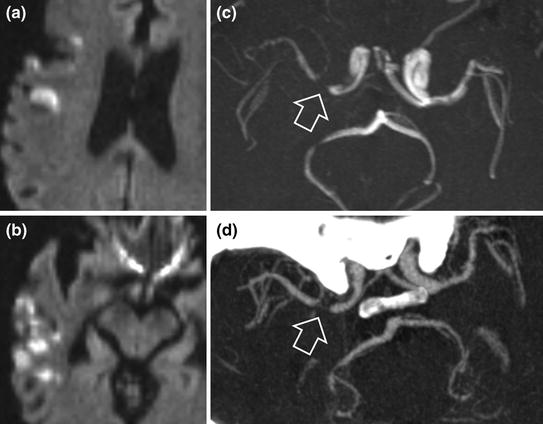
Fig. 3.2
Right superficial middle cerebral artery infarction (a and b diffusion-weighted sequences) in a subject with an intracranial atherosclerotic stenosis. Note the subocclusive stenosis of the origin of the right middle cerebral artery visualized by MRI (c TOF sequence, hollow arrow) and MR angiography (d hollow arrow)
Mechanism of infarction: most commonly thromboembolic (thrombosis [role of platelets] secondary to stenosis and/or artery-to-artery atherosclerotic embolism) or more rarely haemodynamic.
Pathology
Damage of large elastic arteries and muscular arteries (internal carotid arteries, basilar artery, subclavian arteries) by lipid and fibrin deposits, often calcified and possibly leading to ulceration, intraplaque haemorrhage or thrombosis. A classification of atherosclerotic lesions has been proposed by Stary (Table 3.1).
Table 3.1
Classification of atherosclerotic lesions according to Stary
Lesion type | Term | Description |
|---|---|---|
I | Isolated macrophage foam cells | Isolated macrophage foam cells within intima. No extracellular lipids. |
II | Fatty streak | Layers of macrophage foam cells. Lipid-laden smooth muscle cells. Scattered extracellular lipid particles. |
III | Pre-atheroma | Like type II with multiple extracellular lipid deposits forming small aggregates. |
IV | Atheroma | Like type II with multiple massive confluent extracellular lipid deposits (lipid core). |
V | Fibroatheroma | Like type IV with massive collagen deposits (fibrous cap) covering lipid core (type Va) with calcifications (type Vb). |
VI | Complicated | Like type V with disruption of fibrous cap (VIa), intraplaque haemorrhage (VIb) or thrombosis (VIc). |
VII | Fibrotic plaque | Massive intimal thickening with collagen (sclerosis); No or negligible amount of intracellular and extracellular lipids. |
Note that isolated atherosclerotic intracranial stenoses are rare in Caucasians and mainly occur in Black or Asian subjects.
Clinical Features
Often elderly subject with one or several cardiovascular risk factors.
Clinical signs depend on the arterial territory affected.
MCA/ACA junctional infarction is sometimes observed in internal carotid artery occlusion.
Imaging
CT Angiography and MR Angiography
Proximal artery stenosis (carotid bifurcation, origin of vertebral arteries). Intracranial stenosis (especially the basilar artery, 1st segment of Circle of Willis arteries). Unlike post-radiation stenoses (Fig 3.3), atherosclerotic carotid artery stenoses do not extend upstream into the common carotid arteries. Calcification of the arterial wall at the level of the stenosis is often visible on CT scan.
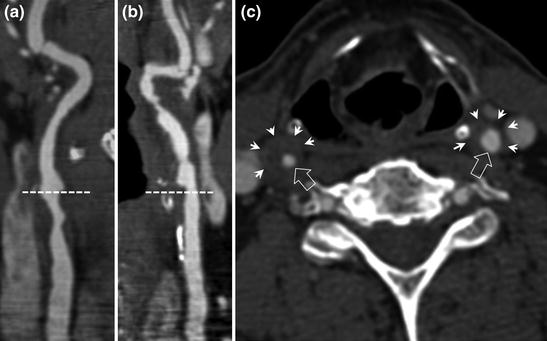

Fig. 3.3
Carotid CT angiography in a subject with a history of laryngeal cancer treated by radiotherapy. Unlike atherosclerotic stenosis, post-radiation carotid artery stenosis involves the distal third of the common carotid arteries and the origin of the internal carotid arteries in the irradiated field (a and b CT angiography: common carotid artery below the dotted line, internal carotid arteries above). Post-radiation thickening of the arterial wall is clearly visible on axial sections (c axial section through the larynx and common carotid arteries at the level of maximum stenosis), small lumen (hollow arrows) with significant thickening of carotid artery walls (small arrows).
Quantification of Carotid Artery Stenoses
Two methods are generally used:
NASCET-ACAS method (NASCET: North American Symptomatic Carotid Endarterectomy Trial; ACAS: Asymptomatic Carotid Atherosclerosis Study): minimum diameter of the stenosis divided by the diameter of the healthy cervical internal carotid artery (Fig 3.4).
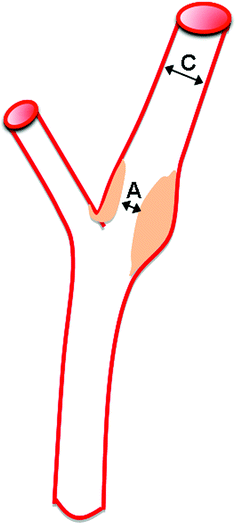
Fig. 3.4
NASCET-ACAS method for stenosis calculation: calculation with reference to the healthy cervical internal carotid artery. % stenosis = (C−A)/C × 100
ECST (European Carotid Surgery Trial) method: minimum diameter of the stenosis divided by the maximum diameter of the carotid bulb (Fig 3.5).
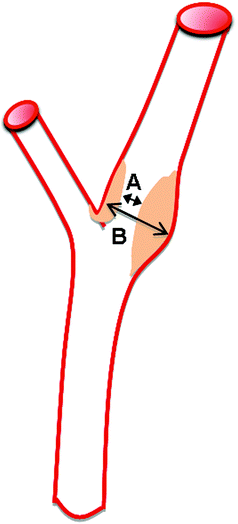
Fig. 3.5
ECST method for stenosis calculation: calculation with reference to the largest diameter of the carotid bulb. % stenosis = (B−A)/B × 100
There is a correlation between the values estimated by the two methods (Table 3.2). For tight stenoses, the values obtained by the two methods are very similar.
Table 3.2
Correlation between the percentage stenosis of arterial diameter according to the method used
NASCET–ACAS method (%) | 30 | 40 | 50 | 60 | 70 | 80 | 90 |
ECST method (%) | 65 | 70 | 75 | 80 | 85 | 91 | 97 |
Treatment of Cerebral Infarction
Emergency treatment:
Intravenous thrombolysis (sometimes intra-arterial) when indicated and in the absence of contraindications.
Aspirin (in the absence of associated haemorrhage) when thrombolysis is not possible or after thrombolysis.
Blood pressure control: maximum systolic blood pressure: 220 mmHg/maximum diastolic blood pressure: 110 mmHg, but no sudden lowering of blood pressure.
Prevention of venous thromboembolic events by low-molecular-weight heparin (high prophylactic dose) in patients with a motor deficit of a lower limb or unable to walk.
Secondary prevention:
Correction of cardiovascular risk factors.
Antiplatelet therapy.
Treatment of Atherosclerotic Stenosis
In France, the standard treatment in addition to medical treatment, is surgery.
Indications for surgical carotid endarterectomy (degree of stenosis according to NASCET method)
Symptomatic carotid artery stenosis
Major cause of stroke: risk = 14 %/year if stenosis >70 % (NASCET).
Surgery is very effective: risk = 4 %/year after endarterectomy
(10 % absolute risk reduction).
Surgical indications:
Atherosclerotic stenosis between 70 % and 99 %: surgery indicated.
For patients with a history of TIA or moderately large or resolving stroke: carotid artery surgery performed as soon as possible (<2 weeks) is more effective than delayed treatment.
Carotid artery Stenosis >70 % + Carotid TIA = EMERGENCY
between 50 % and 69 %: surgery is indicated but with decreased benefit, particularly for women.
carotid artery surgery not beneficial for stenoses less than 50 % and harmful and contraindicated for stenoses less than 30 %.
Asymptomatic carotid artery stenosis
Accounts for a low proportion of infarcts (2 %/year), but constitutes a marker of global vascular risk (risk of myocardial infarction > risk of cerebral infarction).
No surgical indication when stenosis <60 %.
For stenoses ≥60 %, studies comparing surgery and medical treatment only indicate similar results, but in favour of surgical treatment: 1 % absolute risk reduction.
The benefits of surgical treatment for asymptomatic stenoses ≥60 % are observed in the long term, after more than one year. The benefit has been much less clearly established for women.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








