Although there are concerns that one of the drivers of costs in the USA is that Americans are unhealthier (e.g., due to higher rates of obesity, diabetes, coronary problems) it is unclear what factors contribute how much to this. There is some evidence that there is a higher disease burden in the United States (Mackay & Mensah, 2004; World Health Organization, 2009), and that the medical system in the USA expends more on treatments for these diseases (Cutler, 2005). A key question is to what extent are these costs driven by higher incomes (wealthier individuals can afford more health care), higher disease burden, more expensive treatments and technology, inefficiencies such as administrative costs and defensive medicine, or to problematic incentives (called moral hazards by economists) producing overtreatment.
One cause of the high per capita costs is that the United States spends six times more per capita on the administration of the health care system than its peer Western European nations. An analysis of how money is spent revealed that high costs are due to a “failure of the intermediation system to (a) provide sufficient incentives to patients and consumers to be value-conscious in their demand decisions, and (b) establish the necessary incentives or mandates to promote rational supply by providers and their suppliers” (Angrisano et al., 2007, p. 8). Findings point to an array of unnecessary costs specific to the United States due to its present structure. For example, Danzon and Furukawa (2008) found that foreign prices on pharmaceutical drugs are 20–40 % lower than manufacturer’s prices in the USA and 10–30 % lower than public prices in the USA. However, some of this may be a segmenting marketing strategy by pharmaceutical companies to reclaim research and development costs in richer countries.
How Is Money Spent on Health Care in the United States?
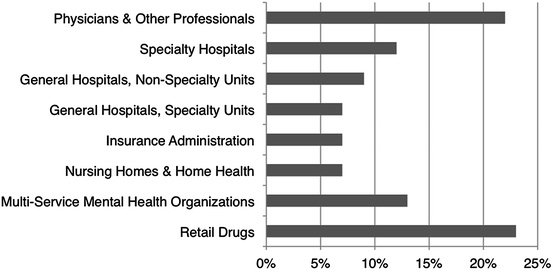
According to the Centers for Medicare and Medicaid Services (2009), total health care expenditures jumped from 253.4 billion in 1980 to 2.2 trillion in 2007. A comparison of health expenditures for 1980 versus those for 2007 (Fig. 2) reveal several notable trends: (1) expenditures on prescription drugs saw the biggest increase over the time period as they increased from 5 % of total health care expenditures in 1980 to 11 % in 2007 and (2) a shift in spending away from hospital care towards professional services and prescription drugs. As services shifted to outpatient settings, expenditures on hospital care decreased significantly from 43 % of total expenditures in 1980 to 33 % in 2007.
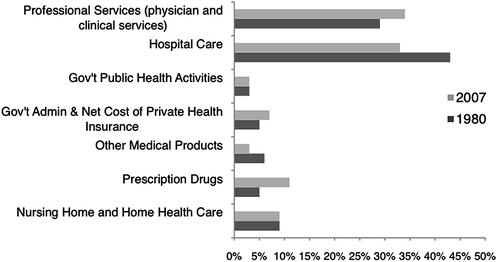

Fig. 2
National health expenditures as a percentage of total spending for 1980 and 2007 (CMS, 2009). Total health care expenditures in 1980 = $253.4 billion, 2007 = $2,241 billion
Over the past 40 years a trend towards increased public spending and decreased private spending on health care expenditures has been observed (CMS, 2008). Government expenditures (paid through taxes and borrowing) accounted for close to 50 % of all health-care expenditures in 2006, up from 30.0 % in 1966 (CMS, 2008).
Behavioral Health Care Spending
Behavioral health care spending makes up a minority of total health care spending in the USA. According to the Substance Abuse and Mental Health Services Administration (Mark et al., 2007), national expenditures for the treatment of mental health ($100 billion) and substance abuse ($21 billion) amounted to $121 billion in 2003 accounting for only 7.5 % of the total health care expenditures. Broken down further, mental health expenditures account for 6.2 % of total health care expenditures and substance abuse spending accounts for 1.3 %.
Trends in Direct Spending on Mental Health
The allocation of mental health spending has shifted over the last three decades. The trend of decreased inpatient services continued with inpatient expenditures dropping from 36 % of total mental health spending to only 24 % between 1993 and 2003 (Mark et al., 2007). The decrease in spending on inpatient services was picked up by prescription drug purchases, which increased from 8 % of total mental health spending to 23 % during the same time period (for a breakdown of mental health spending see Fig. 3). In 2003, close to 1 in 4 dollars spent on mental health services was spent on prescription medications (Mark et al., 2007). The rapid rise in the prescription of psychotropic medications has been well documented (Olfson, Marcus, Druss, & Pincus, 2002; Zuvekas, 2003). In an analysis of results from the Medical Expenditure Panel Survey, Zuvekas (2005) found that an increasing number of individuals take prescription medications without an accompanying visit to a mental health professional (40 % in 1996 and 45 % in 2001). The sharp increase in out-of-pocket spending on mental health seen between 1998 and 2003 may have largely been the result of increased spending on prescription medications. It is important for psychologist to realize that the major competitor in the marketplace—with an increasing share of the market—is the physician (most often a primary care doctor) with a prescription pad.
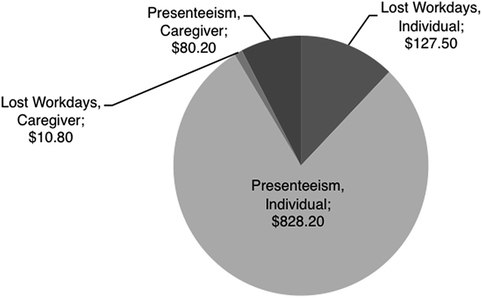
Individuals with mental health disorders rely on public sources of spending to a greater extent than people with other chronic diseases (Mark, et al., 2007). Public sources of funding account for 58 % of total mental health spending, while only 45 % of total health care spending comes from public sources. The largest portion of mental health expenditures is covered by state and local funding while private insurance accounts for only 4.0 %. The full economic costs of mental illness are not captured by the above breakdown of expenditures. Indirect costs such as reduced labor supply, public income support payments, high rates of homelessness among the seriously mentally ill (SMI), and incarceration often overshadow other indirect costs such as the high rates of medical complications, the high prevalence of pulmonary disease (individuals with mental illness smoke 44 % of all cigarettes in the USA), and early mortality (Colton & Manderscheid, 2006; Insel, 2008). While exact figures of indirect costs are difficult to quantify, a recent analysis by Kessler et al. (2008) estimated that serious mental illness is associated with an annual loss of earnings totaling $193.2 billion (Fig. 4).
The Major Drivers of Health Care Spending
Chronic Disease and Unhealthy Lifestyles
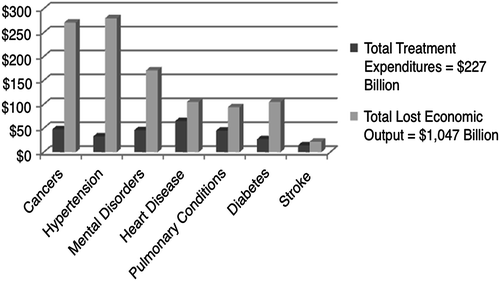
Advances in medical care and prevention efforts have resulted in an epidemiological shift in the leading cause of death from infectious disease and acute illness to chronic disease, defined by the Centers for Disease Control and Prevention as noncommunicable illnesses that are prolonged in duration, do not resolve spontaneously, and are rarely cured completely (2009; CDC, 2003). Currently, 7 of 10 deaths in the USA are caused by chronic disease (CDC, 2009). Nearly half of all Americans (133 million) suffer from one or more chronic disease and a quarter of those who do experience significant limitations in daily activities (CDC, 2009). The increase in the prevalence of chronic diseases has spread across the lifespan with chronic diseases affecting 1.8 % of children and adolescents in the 1960s to more than 7 % in 2004 (CDC, 2009). Recent analysis reveals that the seven most common chronic diseases (cancer, diabetes, hypertension, stroke, heart disease, pulmonary conditions, and mental disorders) cost the economy more than $1 trillion annually in 2003 (see Fig. 5, DeVol & Bedroussian, 2007). Currently, more than 75 % of health care costs are due to chronic conditions (CDC, 2009). Costs go beyond health care expenditures for each chronic disease and capture a host of indirect costs including sick days, low performance rates, output loss, and losses incurred by the caregiver, such as finances (DeVol & Bedroussian, 2007). The costs to the economy are projected to continue to grow and may reach close to $6 trillion by 2050 (DeVol & Bedroussian, 2007). An analysis of the modifiable behavioral risk factors that can lead to the nation’s leading chronic diseases found that close to 35 % of US deaths in 2000 were due to tobacco use, poor diet, and physical inactivity (Mokdad, Marks, Stroup, & Gerberding, 2004). In an examination of the effects of obesity, smoking, and drinking on medical problems and costs, Strum (2002) found that obesity far outranks the negative effects of drinking and smoking. Obesity was associated with a 36 % increase in outpatient and inpatient spending and a 77 % increase in medications while current smokers were associated with a 21 % increase in inpatient and outpatient spending and a 28 % increase in medications and even smaller effects for problem drinkers (Strum, 2002). Obesity has become an epidemic among children and adolescents (O’Donohue, Moore, & Scott, 2009) (Fig. 6).
Comorbid Conditions
A review of the literature reveals that individuals with mental illnesses tend to be high utilizers of medical care, as they routinely present to their primary care physicians with a high number of comorbid illnesses and incur longer hospital stays (Chiles, Lambert, & Hatch, 1999). Schizophrenia in particular is associated with substantial direct and indirect costs in excess of those incurred by matched controls (Wu et al., 2005). Wu et al. (2005) found that the overall cost of schizophrenia in the USA in 2002 was estimated to be $62.7 billion with $22.7 billion in direct health care costs. Treatment for comorbidity has been found to add 20–90 % to the annual spending among patients with schizophrenia (McDonald, Hertz, Lustik, & Unger, 2005).
Comorbid depression has been associated with higher health-care costs for patients with chronic medical disorders such as diabetes mellitus (Ciechanowski, Katon, & Russo, 2000; Gilmer et al., 2005) and congestive heart failure (Sullivan et al., 2005). In a population-based cross-sectional survey of 130,880 Canadians, Stein et al. (2006) found that the presence of comorbid major depressive disorder and a chronic physical illness was associated with approximately double the likelihood of health care utilization, increased functional disability, and work absence compared to a chronic physical illness without the comorbid depression. The increase in health care costs is particularly notable in older adults with comorbid depression (Himelhoch et al., 2004; Katon, 2003). In recent analysis of health care costs for close to 15,000 Medicare recipients with diabetes and/or congestive heart failure found that individuals with depression had significantly higher total health care costs over a 12-month period than those without depression ($20,046 vs. $11,956) (Unutzer et al., 2009). Interestingly, depressed individuals had higher health care costs across all cost categories except specialty mental health services, which accounted for less than 1 % of total costs.
A possible driver of increased costs for individuals with chronic disease and comorbid depression is the higher rates of adverse health-risk behaviors that depressed individuals have been shown to experience, such as smoking, maintaining a high-fat diet, sedentariness, drinking, and obesity (Goodman & Whitaker, 2002; Rosal et al., 2001). A meta-analysis of the effects of anxiety and depression on patient treatment adherence found that depressed individuals are three times more likely to be noncompliant with medical treatment recommendations than nondepressed patients (DiMatteo Lepper, & Croghan, 2000). The relationship between anxiety disorders and comorbid medical illnesses is less well studied, but Roy-Byrne et al. (2008) argue that anxiety and anxiety disorders may have as great a negative impact on physical illness as depression does. In a review of the literature, the authors found that anxiety disorders amplify symptoms of some medical illnesses and appear to worsen outcomes. Thus, it has increasingly become recognized that some of the key drivers of health care expenditures are behavioral: poor diet, insufficient exercise, smoking, poor treatment adherence, anxiety, and depression. These are factors that psychologists have something to offer.
The Importance of Adolescent Health Care Consumers
Adolescents are of particular importance when examining the current health care crisis in the United States. First, this population is a driver of high health care costs, at least in part due to the fact that adolescents underuse office visits and overuse emergency department care when compared with persons in other age groups (Newacheck, Wong, Galbraith, & Hung, 2003). Second, during the transition from childhood to adulthood, adolescents establish patterns of behavior and make lifestyle choices that affect both their current and future health (Centers for Disease Control and Prevention, 2011; O’Donohue & Tolle, 2009). Third, adolescence has been identified as a particularly important phase to address health behavior and it is a significant intervention point for behavior change (O’Donohue & Tolle, 2009). Adolescents are unique consumers of health care and must be considered when examining the current health care reform.
The financial burdens of preventable health problems in adolescence are large and include the long-term costs of chronic diseases that are a result of a pattern of behavior initiated during adolescence. Alarmingly, national surveys report that 70 % of adolescents engage in one or more health-risk behaviors (Klein & Matos Auerbach, 2002, as cited by Olson, Gaffney, Lee, & Starr, 2008). These behavioral problems are an important cause of adolescent morbidity and mortality (Catalano, et al., 2012). For example, the annual health-related financial burden of adult cigarette smoking, which usually starts by age 18, is $193 billion (Health People.gov, 2012). Unfortunately, adolescents have seemed to be neglected by health care providers and researchers, and as a result, adolescence health has improved far less than that of younger children over the past 50 years (Sawyer, et al., 2012). As the nation’s spending in health care continually increases it is important to target adolescences in order to improve health behaviors early in life to prevent long-term problems, reduce health care costs, and most importantly, improve quality of life.
Adolescents engage in risk behaviors that may create problems both in the short and long term for not only the individual but also society as a whole. Adolescents engage in risky driving, dieting, substance use, and sexual activity. In 2005, teen birthrates went up for the first time since 1990 (Mulye et al., 2009). We see that teen pregnancy not only influences the quality of life of the teen, but that the health of the baby is usually compromised due to the higher likelihood of the mother engaging in unhealthy behaviors (Sawyer, et al., 2012). Obesity in adolescence is projected to increase coronary heart disease 5–16 % in adults by 2035 (Bibbins-Domingo, Coxson, Pletcher, Lightwood, & Goldman, 2007). To confound these behavioral problems, one in seven adolescents lacks full-year medical coverage, making access to care difficult if not financially impossible (Mulye et al., 2009).
Because adolescence is a developmental transition, teens are particularly sensitive to environmental (or contextual) influences such as family and societal cues (Health People.gov, 2012). Adolescence is a critical transitional period that includes the biological changes of puberty and the need to negotiate key developmental tasks, such as increasing independence and normative experimentation (Health People.gov, 2012). Specifically, adolescents begin to take more personal responsibility for managing their own health (O’Donohue & Tolle, 2009). Some adolescents struggle to adopt behaviors that could decrease their risk of developing chronic diseases in adulthood, such as eating nutritiously, engaging in physical activity, and choosing to not use tobacco (Centers for Disease Control and Prevention, 2011; National Institute of Child Health and Human Development, 2007). Fortunately, adolescences view health care providers as a credible source of information, and wish to discuss their issues with health-care providers (Klein, Graff, Santelli, Hedberg, Allan, Elster, 1999, as cited by Olson, Gaffney, Lee, & Starr, 2008). If adolescents can be influenced to visit health care providers, there is a good chance of guiding adolsence behavior towards positive outcomes.
Adolescence as the Origin of Chronic Disease and Unhealthy Lifestyles
As aforementioned, chronic disease is now the leading cause of death and the origin of lifestyle choices that increase the likelihood of developing chronic disease often begins in adolescence (O’Donohue & Tolle, 2009). Obesity, diabetes, and smoking are of particular concern during this developmental phase.
The incidence of youth obesity is rising sharply and has significant health implications. It is reported that 18 % of adolescents in the United States are overweight, a number that has more than tripled from 1980 to 2008 (Centers for Disease Control, 2011a, 2011b). Obesity at this age has both immediate and long-term health effects. Of those adolescents who were considered obese, 70 % had at least one risk factor for cardiovascular disease (Li, Ford, Zhao, & Mokdad, 2009, as cited by Centers for Disease Control, 2011a, 2011b). Obese adolescents are also more likely to suffer from prediabetes, bone and joint problems, and social and psychological problems (Li, Ford, Zhao, & Mokdad, 2009 as cited by Centers for Disease Control, 2011a, 2011b). Also, obese adolescents are more likely to be considered obese as adults, which is associated with health problems such as certain types of cancer, heart disease, diabetes, stroke, and osteoarthritis (Centers for Disease Control, 2011a, 2011b).
Related to the problem of obesity, the prevalence of type 2 diabetes has increased dramatically in the recent years and in most studies all youth diagnosed with type 2 diabetes were also obese (Delamater, Jacquez, & Patino-Fernandez, 2009). In the United States, approximately 176,500 individuals under the age of 20 years have diabetes (LaGreca & Mackey, 2009). Prior to the mid-1990s, only 1–2 % of children met the criteria for type 2 diabetes and in the recent years the incidence has increased to 8–45 % of youth. In addition, 1 out of every 400–600 children has type 1 diabetes. The annual cost for diabetes management is determined to be $174 billion (LaGreca & Mackey, 2009). Diabetes is a lifelong chronic illness that requires management across the lifespan and is often diagnosed in adolescence (O’Donohue & Tolle, 2009).
In 2009, 25.6 % of high school students and 9.5 % of middle school students reported using tobacco products (Centers for Disease Control, 2011a, 2011b). While these numbers are steadily declining (34.5 % of high school students and 15.1 % of middle school students reported using tobacco products in 2000), there are still many health implications associated with smoking. Those adolescents that do smoke are more likely to engage in high-risk sexual behavior and use alcohol and other illicit drugs (Centers for Disease Control 2012). Adolescents that begin smoking will likely continue to smoke regularly throughout their adulthood (WHO, 2012). Smoking is associated with short-term health consequences that include respiratory problems, decreased lung functioning, and addiction to nicotine. Long-term effects include increase risk of heart disease, stroke, and certain forms of cancer (WHO, 2012).
Comorbid Conditions
Individuals with mental illnesses tend to be high utilizers of medical care and comorbid conditions in adolescence, such as depression, can have lifelong health implications. In 2009, about 8 % of adolescents suffered at least one major depressive episode over the course of 1 year (Childstats.gov 2011). Rates of depressive disorders peak in mid-adolescence, particularly in females (Street & Garber, 2009). Of those adolescents that experienced a major depressive episode only 35 % received some kind of treatment, either talking to a medical or mental health professional about their problem and/or taking prescription medications (Childstats.gov 2011). Not only does depression affect school and social relationships, but it also exacerbates health conditions such as obesity, asthma, migraine headaches, and allergies (Street & Garber, 2009). Adolescences that experience depression are more likely to engage in alcohol and drug use and are more likely to smoke on a daily basis Childstats.gov 2011. Additionally, depressive symptoms in adolescence have been shown to predict not only the likelihood of recurrent depressive episodes in adult life but also the onset of subsequent clinical disorders (Street & Garber, 2009). Depression can also increase the risk for other medical problems through the occurrence of sleep problems, lack of exercise, and poor eating habits (Street & Garber, 2009).
The Problem of the Uninsured
Although the United States spends more on health care than other industrialized nations nearly 46 million individuals living in the USA do not have health insurance (Carey, Herring & Lenain, 2009). The number of uninsured individuals has increased significantly in the last decade, from 38 million (14 % of the population) in 2000 to 46 million (16 % of the population) in 2007 (Carey et al., 2009). The uninsured are a heterogeneous group, including about 10 million illegal immigrants (Gruber, 2008). The increase in the uninsured is due in part to a decline in the percent of employees with employer-sponsored insurance (80.4 % in 2000–2001 to 75.7 % in 2007 (Cunningham, Artiga, & Schwartz, 2008). The largest declines (53.0–40.8 %) have been seen among low-income employees, whose family incomes are less than 200 % of poverty. Employers, particularly small businesses, have struggled to provide health insurance as a benefit due to the increases in employers’ health care costs (up to 7.3 % in 2009; Thomson Reuters, 2010).
The recently signed Patient Protection and Affordable Care Act (H.R. 3590) is focused on decreasing the number of uninsured by expanding coverage for 32 million Americans. The legislation will establish among other things a mandate for most Americans to obtain health insurance, significantly expand eligibility for Medicaid, set up insurance exchanges through which individuals can receive federal subsidies to reduce the cost of purchasing coverage, substantially reduce the growth of Medicare’s payment rates for most services, and impose an excise tax on insurance plans with high premiums (Congressional Budget Office, 2010). As detailed above, the health care reform legislature will increase the government’s role in providing health to its citizens. An analysis of the bill by the Congressional Budget Office (2010) found that health care costs will be lowered over time although this point continues to be debated.
Due to the high rate of uninsured children and adolescence and the poor quality of care associated with being uninsured the Children’s Health Insurance Program (CHIP) was enacted by Congress in 1997 to provide insurance for children and improve access to care for low-income families (Szilagyi, et al., 2004). Originally, Congress had set aside 40 billion dollars to provide states with grants to create and provide their own CHIP. However, due to budget cuts some of this original money was taken away, and in 2007, former President George W. Bush vetoed two bills to renew and expand CHIP. Due to these vetoes Congress passed a bill that extended the fund of CHIP until 2009, but fell far short of the original two bills to expand the program. In 2009, Congress passed another bill to renew and expand CHIP that was signed by President Barack Obama.
Though it has had a turbulent finically and political history, CHIP has proved to be beneficial for adolescents. One third of the individuals enrolled in CHIP are adolescences (Klein, Shone, Szilagyi, Bajorska, & Wilson, 2007). The program has been effective in reducing the amount of uninsured adolescents from 15.2 to 12.2 % since its inception (Newacheck, Park, Brindis, Biehl, & Irwin, 2004). Through CHIP, adolescences have improved access, continuity, and quality of care and this care is delivered within the usual primary care source (Szilagyi, et al., 2004). Those who have CHIP use more preventative care and have fewer unmet medical needs (Klein et al., 2007). Also, enrollment in CHIP also is associated with eliminating racial disparities in access to medical services (Klein et al., 2007).
While some improvements have been made through programs like CHIP, there is still much progress to be made. Adolescents’ access to health care is among the worst of all age groups, and relatively few interventions have shown to be effective in improving their access to care (Klein et al., 2007, p. 891). Adolescents that would qualify for programs like CHIP make up for one third of the total adolescent population but account for two thirds of the uninsured population (Newacheck et al., 2004). Since health and health behaviors are of utmost importance for this age group, it is important that we continue to target and improve access to care for these individuals.
Cost vs. Value
Cutler (2005) makes the important point that examining increasing costs misses an important part of the issue, i.e., do these incremental costs bring increased value? Cutler answers that for the most part they do. He suggests, for example, that no one would want to revert to 1950s medicine with its lower costs but also with its decreased effectiveness. Thus, a significant part of the increased costs over time is driven by actual improvements in the technology of health care, e.g., cures for cancer, more surgical options (e.g., bypass surgery and hip replacements), additional prescriptions (e.g., HAART treatments for HIV), and improved imaging. Cutler examined in detail the technological improvements in care for low birth weight babies and argues that each additional $1 spent produces $5 of derived benefit. This raises an important point: we need to realize that often improvements in medical technology translate into increased costs. Part of the increased costs in the USA may be due to the increased technology developed and used in the USA. Some improvements are very cheap (e.g., aspirin to decrease heart attacks), but these tend to be the exception. Cutler suggests that the key is not finding a lower cost health care but a more efficient health care system. He suggests that too much emphasis has been placed on high-cost, high-tech, medicine and not enough on lower cost, lower technology medicine which can produce this higher value proposition. But still the question remains what expenditures in the current system fail to represent good value?
Focus on Understanding Incentives and Moral Hazards in Payment Systems
Health care economists examine how reimbursement systems (e.g., direct consumer payment vs. third-party payments, prepaid capitated payments vs. fee for service insurance, various managed care arrangements, pay for performance, etc.) affect the behavior—and hence the overall costs—of consumers, providers, and third-party reimbursers. The assumption is that none of these stakeholders should be expected to behave as “economic eunuchs” but rather respond to whatever incentives and disincentives—perverse or constructive—the system contains. The supply and demand of health care is determined by these incentives. For example, prepaid capitated plans provide disincentives for health care professionals to provide care: fee for service has the opposite effect—it provides incentives to provide more care.
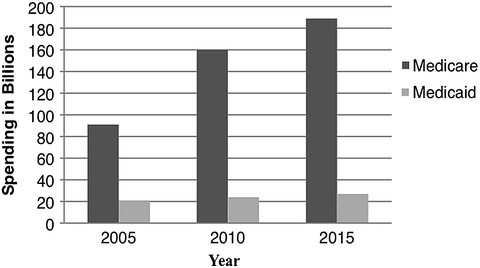
Wennberg et al. (2002) found that, for Medicare spending there was a twofold variation among regions, and the variations persist even after differences in health are corrected for. The study found that “higher levels of Medicare spending are due largely to increased use of supply sensitive services—physician visits, specialist consultations, and hospitalizations, particularly for those with chronic illness or in their last 6 months of life (p. 11).” Specifically, he found that the difference between lifetime Medicare spending for a typical 65-year-old Medicare recipient in Miami vs. one in Minnesota was $50,000. One of the ways health care is somewhat unique is that the supply of health care has a major role in determining the demand for health care.
“Free” care—either because it is paid by the government or because the consumer directly pays nothing and a third-party insurer pays everything—provides a huge incentive (by removing the normal disincentive of direct consumer payment) for consumers to demand a lot of care; hence the demand created by free care is often rationed by policy or by lines. More expensive care generally reduces demand, if demand is not perfectly inelastic—a point professionals may not completely understand as they argue for higher fees.
Properly aligning the incentives on all stakeholders is perhaps the key and most difficult question in health-care reform. Goldhill (2009) states:
…I suspect that our collective search for villains—for someone to blame—has distracted us and our political leaders from addressing the fundamental cause of our nation’s health-care crisis. All of the actors in health care—from doctors to insurers to pharmaceutical companies—work in a heavily regulated, massively subsidized industry full of structural distortions. They all want to serve patients well. But they also all behave rationally in response to the economic incentives those distortions create. Accidentally, but relentlessly, America has built a health-care system with incentives that inexorably generate terrible and perverse results. Incentives that emphasize health care over any other aspect of health and well-being. That emphasize treatment over prevention. That disguise true costs. That favor complexity, and discourage transparent competition based on price or quality. That result in a generational pyramid scheme rather than sustainable financing. And that—most important—remove consumers from our irreplaceable role as the ultimate ensurer of value (p. 40).
A major part of properly aligning incentives in the health care system is to ask basic questions about the proper role of health care insurance. No one has asked more probing questions about this topic than the late Nobel laureate, Milton Friedman. First, Friedman (2001) suggested that the health care system is distorted by the fact that most individuals receive health-care insurance from their employers. Interestingly this happened due to a historical accident: During WWII there were federal wage and price controls so that employers could not attract employees by higher wages. However employers could offer benefit packages as the government did not prohibit this. So employers offered health insurance and the government decided not to tax this (this is often criticized as it is also regressive taxation—the relatively wealthier are more likely to have a job with health care benefits than the poor, and thus more of the relatively wealthy avoid taxes on this income, while the poor do not). Friedman pointed out that the employer paying for health care distorts usual market mechanisms as the employee is not shopping with their own dollars.
What health care expenses ought to be insured? According to Friedman (2001), part of the concern is that the current system is too insurance centric. Insurance is generally regarded as reasonable for expenditures that are rare but are not affordable (a $200,000 house burning down or tens or hundreds of thousands of dollars for some cancer treatments, for example). Friedman has long argued that we spend other people’s money (i.e., the third-party insurer’s) differently than we spend our own. Thus, third-party payments for expenses we can actually afford (but would like to not pay directly) are considered moral hazards as they distort normal consumer spending. As Goldhill (2009) has stated it, “ we can’t imagine paying for gas with our auto-insurance policy, or for our electric bills with our homeowners insurance, but we all assume that our regular checkups and dental cleanings will be covered at least partially by insurance” (p. 42). This gives rise to the saying, “If you are concerned with how much healthcare costs now, just wait until it is free.” Price is a mechanism for rationing. Insurers in benefit design use co-pays and deductibles to disincent and incent consumer demand. Followers of Friedman’s arguments argue for the use of medical savings accounts—tax free accounts that can only be used for medical expenses and that can roll over each year—so that consumers experience the normal disincentive of price for their first few thousand of their health care purchases.
Psychology’s Role in Health Care Reform
The final section will discuss new opportunities for psychologists arising from the recent health care reform bill and ten suggested major reforms for the health care system. Psychology has the potential to be a major player in health care reform given the large and diverse roles that behavioral pathways play in medical presentations (Cucciare & O’Donohue, 2003). However, to take on this role, and not to be relegated to the sidelines, psychology needs to reform itself. It can no longer be business as usual.
The Patient Protection and Affordable Care Act: What Does It Mean for Psychology?
The American Psychological Association’s Public Interest Government Relations Office (2010) reviewed the 2,400 pages of the Patient Protection and Affordable Care Act and found numerous legislative provisions that are favorable for the field of psychology. The provisions sited focused on increasing integrated health care and mental and behavioral health parity, enhancing prevention and wellness, developing the psychology workforce, elimination of health disparities support for psychological research, and increasing involvement with consumers, families, and caregivers (APA, 2010). Table 1 highlights several key provisions.
Table 1




Patient protection and affordable care act: key provisions for psychology
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree