Chapter 1 The biopsychosocial model
As future doctors, you will be looking forward to working face to face with patients – making sense of complex signs and symptoms, requesting and interpreting diagnostic tests, deciding on diagnoses, discussing their implications with patients and agreeing treatment and longer-term management for those who have chronic diseases that cannot be cured. You may also find yourselves involved in trying to prevent, or at least delay, the onset of disease through screening programmes, opportunistic screening and secondary prevention (see pp. 64–65 and 68–69).
This definition emphasizes psychological and social aspects of health (see pp. 38–39). Any comprehensive framework for understanding health and health care services must embrace both psychological and sociological aspects of well-being and their interactions with biological processes (see pp. 38–39). Health depends on our perceptions, beliefs and behaviour and how these interact with physical systems such as the endocrine, immunological and cardiovascular systems. At the same time our perceptions and behaviours are shaped by our social context. Understanding how social, psychological and biological processes interact to create differences in health is what is meant by adopting a biopsychosocial perspective (Schwartz, 1980), as illustrated in the case study.
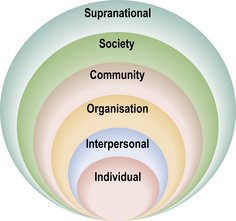
Bartholomew et al. (2006: 9) advocated a ‘social ecological’ model of health and health behaviours which includes individual and social determinants of perception and behaviour (Fig. 1). For example, in the UK, where the wealthiest 10% of the population own more than half of all wealth, the difference in life expectancy between the poorest and richest areas is about 10 years (Shaw et al., 2005). Thus just knowing where someone is born (e.g. the northern UK or even which part of a city) allows us to make useful predictions about how long they will live, illustrating how our societal context shapes our well-being and health.
Case study
Mr Brown is being interviewed by a small group of third-year medical students and telling them about his experience of heart disease (see pp. 106–107). He is 65 years old and married with two children and two grandchildren. He was born in a relatively poor part of the city and was one of four children living with their parents in a two-bedroomed third-floor tenement flat (see pp. 54–55). They ate what they regarded as good food: ‘the best: eggs, butter, meat’ as their mother worked as a cook and domestic for a local wealthy family. All six of them smoked (see pp. 84–85). He left school at 16 and went to work as bus driver and his ability led him to be promoted to operations manager – ‘quite a demanding and stressful job’ (see pp. 56–57).
Mr Brown first began to experience episodes of mild chest pain in his early 40s and when he went to see his doctor he was strongly advised to stop smoking. However, he did not stop because, as he saw it, he wasn’t that ill (see pp. 72–75, 78–79, 88–91). He had his first heart attack when he was 45, describing it as ‘crushing pain; as if a ton of bricks had landed on my chest’. In hospital, he had a second heart attack (see pp. 102–103
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree