The Extradural Vertebral Arteries
Key Points
The anterior spinal artery is a major focus of concern in all vertebral artery catheterizations and embolizations.
Anastomotic connections between the vertebral arteries and the external carotid arteries are universally present, whether they are angiographically evident or not, and may become the basis for misadventurous embolization of the posterior circulation in various circumstances.
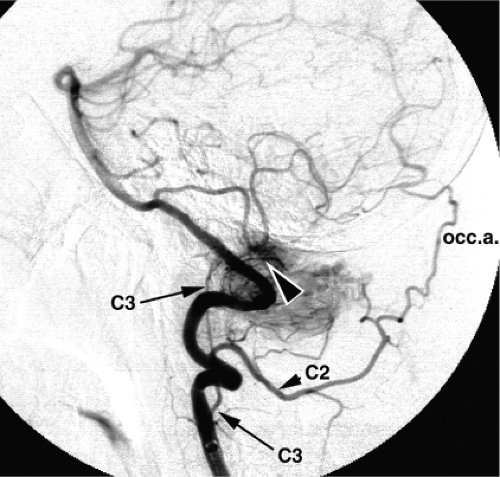
The vertebral arteries derive from eight paired segmental vessels that correspond with the embryologic cervical somites. As the vertebral bodies differentiate, the vessels become intersegmental in location and are so designated thereafter in the embryologic literature, with each numbered to correspond with the vertebral body above. In the embryologic literature, the first segmental artery is therefore displaced from the numbering scheme and is then termed the proatlantal intersegmental artery (1). However, in angiographic parlance, anastomotic branches of the vertebral artery are numbered according to the corresponding cervical nerve root. For example, the C2 branch of the vertebral artery emerges between the C1 and C2 vertebral bodies (Figs. 14-1 and 14-2).
The plexus, which is formed cranially by the segmental arteries during embryonic life, anastomoses at the level of the hypoglossal nerve with the paired longitudinal neural plexi, which form the basilar artery. The cervical vertebral artery forms from a longitudinal anastomosis between the segmental cervical arteries. A concurrent partial regression of the proximal portions of each of the upper segmental arteries takes place.
It should be theoretically possible for any of the segmental arteries to become the dominant feeder to the forming longitudinal anastomosis, which will become the ipsilateral vertebral artery. Usually the proximal vertebral trunk off the subclavian artery corresponds with the sixth intersegmental artery and enters the foramen transversarium below the C6 vertebral body. When the left vertebral artery arises directly off the aorta proximal to the subclavian artery, the vertebral artery corresponds most commonly with the fourth intersegmental vessel and enters the foramen under the C4 body. Other derivations of the intersegmental arteries such as the proatlantal intersegmental artery are rare (discussed in Chapter 10) (2).
The formation of the vertebrobasilar system from the fusion of two sets of vascular embryologic plexi explains the propensity of the vessels in this region to emerge with variable patterns. The vertebral artery itself may retain flow through two parallel channels, giving the appearance of a duplication (Figs. 14-3–14-5). Duplications can be seen at any level of the vertebral artery in 0.7% of studies (3,4,5,6,7). Alternatively, ectasia or looping in the high cervical area may result in the vertebral artery assuming an intradural course at a level as low as the C2 body. This can be an incidental finding but can also be associated with cord or root compression symptoms (8) and may be seen particularly with somal disorders affecting the cervical area such as Klippel–Feil syndrome (9). An anomalous pattern of regression of elements of the longitudinal neural plexi (in the posterior fossa) and of the cervical plexus can also explain a C1 or C2 origin of the posterior inferior cerebellar artery (Fig. 14-6).
The anatomy of the vertebral artery is sometimes described in four parts (Fig. 14-7).
The first segment extends from the subclavian artery to the foramen transversarium of the C6 vertebral body.
The second segment ascends vertically within the foramina transversaria from C6 to the atlas.
The third segment leaves the transverse foramen of the atlas and extends posteriorly and horizontally on the superior surface of the posterior arch of the atlas.
The fourth segment pierces the atlanto-occipital membrane and the dura in turn, and then enters the intracranial cavity via the foramen magnum.
Within the foramina transversaria, the vertebral artery in its usual configuration ascends surrounded by the vertebral venous plexus. It runs immediately adjacent to the uncinate processes medially and the ventral rami of the cervical nerves posteriorly. Above the axis, the artery courses laterally and posteriorly before turning sharply cephalad. It then passes through the foramen transversarium of the atlas, which is located more laterally than those below. It courses posteromedially in a horizontal direction, imprinting a groove on the superior surface of the posterior arch of the atlas. In a minority
of anatomic specimens, the rims of this groove on the superior atlantal surface become a circumferential bony ring. At the margin of the C1 posterior arch, the vertebral artery turns abruptly anteromedially and pierces the atlanto-occipital membrane to enter the dura where a waistlike impression on the contour of the vessel may be seen angiographically. The vertebral artery then fuses with its counterpart anterior to the medulla to form the basilar artery. This junction is usually at or within a few millimeters of the inferior rim of the clivus.
of anatomic specimens, the rims of this groove on the superior atlantal surface become a circumferential bony ring. At the margin of the C1 posterior arch, the vertebral artery turns abruptly anteromedially and pierces the atlanto-occipital membrane to enter the dura where a waistlike impression on the contour of the vessel may be seen angiographically. The vertebral artery then fuses with its counterpart anterior to the medulla to form the basilar artery. This junction is usually at or within a few millimeters of the inferior rim of the clivus.
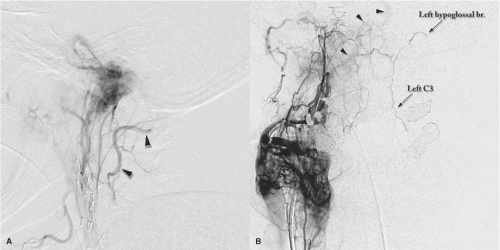 Figure 14-2. Anastomotic dangers to the vertebral artery. Lateral (A) and AP (B) views of injections in the ascending pharyngeal artery in two different patients, each with a paraganglioma of the jugular bulb and carotid body respectively. Each image shows the extreme ease with which access to the ipsilateral vertebral artery and subsequently the basilar artery (arrowheads) can be established, even when the anastomotic connections are not particularly enlarged. The C3 anastomoses to the vertebral arteries bilaterally are shown well in image (B) accessed via the hypoglossal branch of the neuromeningeal trunk on the right side, and refluxing contralaterally to the left-sided counterparts.
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|