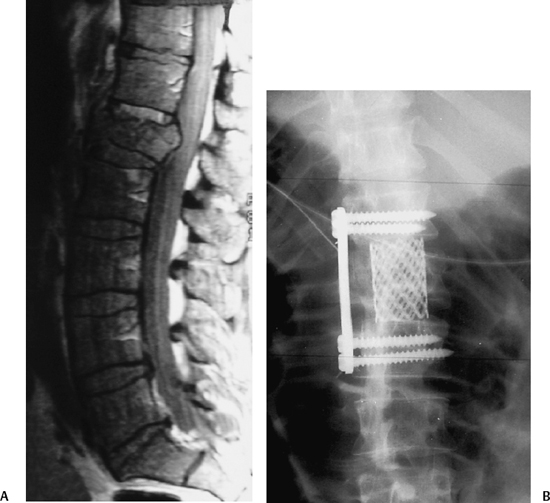
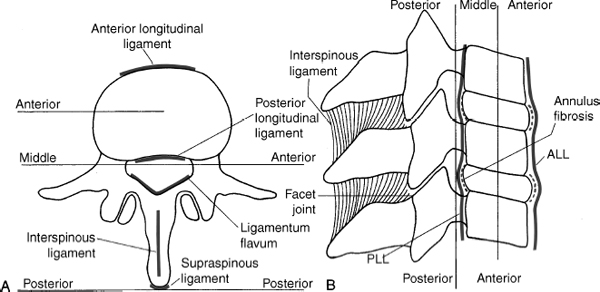
9 I. General considerations A. Thoracolumbular spine is the most common site of spinal injuries B. Most injuries occur in males (age 15 to 29), usually a result of a motor vehicle accident C. Most injuries occur between T11 and L1 (52%) 1. L1–L5 (32%) 2. T1–T10 (16%) D. Associated injuries are common and may occur in up to 50% of patients, usually the result of a distractive force. 1. Intra-abdominal bleeding from liver and splenic injuries 2. Arterial or venous vessel disruption 3. Pulmonary injuries a. Hemothorax b. Pulmonary contusion II. Patient evaluation A. General assessment 1. Respiratory, cardiothoracic, abdominal, urologic evaluation 2. Head/cervical spine status B. Neurological assessment 1. Frankel scale and American Spinal Injury Association (ASIA) motor index 2. Spinal cord, conus, cauda equina, root injuries C. Radiological evaluation 1. All patients who have injuries suspicious for spinal trauma should undergo plain radiographic imaging (anteroposterior or lateral) of all vertebral levels. 2. Plain X-ray is the initial screening modality a. Computed tomography (1) Best imaging modality for evaluation of the middle column especially with sagittal reconstructions b. Magnetic resonance imaging (MRI) (1) Most useful in evaluating the spinal cord and soft tissue disruption (disk/ligamentous injury) III. Classification methods A. Spine stability (Denis classification) (Fig. 9–1) 1. Three columns a. Anterior column (1) Anterior longitudinal ligament, anterior anulus fibrosus, and anterior half of the vertebral body b. Middle column (1) Posterior longitudinal ligament, posterior anulus fibrosis, posterior half of the vertebral body c. Posterior column (1) Pedicles, facet joints, lamina, spinous processes, and interspinous and supraspinous ligaments 2. Clinical application a. Instability is defined as a disruption of two or more of the three spinal columns. b. If the middle column is disrupted, then the spine is unstable except (1) Thoracic vertebrae above T8 (stability provided by the ribs) (2) L4–L5 where the posterior column is intact (significant weight bearing through the posterior column because of lordosis) (3) Distraction injuries where fractures occur through the cancellous bone 3. Stability is not “black and white” but gray zone (Denis) a. Stable fractures (1) Transverse process (2) Spinous process (3) Articular process (4) Pars interarticularis (5) Compression fractures B. Thoracolumbar injury classification and severity score 1. Operative treatment is based upon three factors (each subcategory has been listed with increasing severity). a. Morphology of the fracture (1) Compression (2) Burst (3) Translational/rotational (4) Distraction b. Posterior ligamentous complex (1) Intact (2) Indeterminate/suspected (3) Injured c. Neurological status (1) Intact (2) Root injury (3) Cord (a) Incomplete (b) Complete (4) Cauda equina syndrome IV. Treatment A. General considerations 1. Multifactorial a. Neurological status of the patient (1) An anterior approach is preferred in patients who are neurologically compromised. b. Posterior ligamentous complex integrity (1) If disrupted, requires reconstruction of the posterior tension band c. Fracture morphology 2. Timing of surgery a. Immediate operative intervention most likely gives the best chance for reduction and neural recovery but not clinically proven. b. Indications for acute surgical intervention (1) Progressive neurological deficit (2) Irreducible dislocations (3) Open or contaminated injuries c. Early surgery (2 to 3 days) (1) Easier reduction and decompression via ligamentotaxis (2) Earlier mobilization of the patient (3) Potential operative complications (a) Transportation issues regarding patients with severe spinal instability d. Late surgery (7 to 10 days) (1) Arguments for delayed intervention include providing a chance for the spinal cord to recover from trauma and edema (a) Skeletal traction and closed reduction and Stryker motorized rotating bed for patients with deformity or dislocations that cannot be operated on soon 3. External immobilization a. Above T5: cervico-thoracic-lumbosacral orthosis b. T6–L4: Jewet hyperextension or thoracolumbar-sacral orthosis (TLSO) braces c. L5–S1: Pantaloon cast B. Neurological status and stability 1. Neurologically intact with a stable spine a. Common in compression fractures, seat belt-type injuries and burst fractures of the lower lumbar spine b. Orthosis or body cast 2. Neurologically intact with an unstable spine a. Common in burst fractures and severe compression fractures b. Operative stabilization to prevent neurological loss c. Early rehabilitation is preferred. 3. Neurologically compromised and spine unstable a. Burst fractures or fracture dislocations of the lower thoracic spine and lumbar spine (Fig. 9–2) b. Anterior decompression with or without posterior stabilization C. Specific fracture treatment 1. Compression-flexion injuries a. Anterior column injury alone usually does not cause neurological deficits. (1) Factors suggestive of instability and disruption of the posterior ligamentous complex (a) Greater than 50% collapse (b) Thirty-degree angulation (c) Thirty-degree kyphosis b. Treatment (1) Conservative if anterior column failure alone (a) Hyperextension orthosis (2) Middle column failure (a) Operative intervention 2. Distraction flexion injuries (seat belt injury) (Fig. 9–3) a. Chance fracture without subluxation or dislocation (1) Hyperextension body cast b. Ligamentous flexion-distraction injury (1) Posteriorly instrumented arthrodesis
Thoracolumbar Spine Fractures
Neupsy Key
Fastest Neupsy Insight Engine