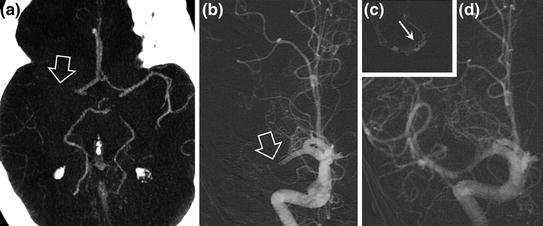
Fig. 14.1
22-year-old female patient with left middle cerebral artery infarction and right hemiplegia and aphasia. The NIHSS score was 20. MRI performed 3 h after onset of symptoms shows abnormalities on diffusion-weighted images in the left superficial middle cerebral artery territory (a diffusion-weighted sequence) with occlusion of the left middle cerebral artery bifurcation (b TOF sequence, hollow arrow). Resolution of the arterial occlusion after intravenous thrombolysis on follow-up MRI (c TOF sequence) with improvement of the neurological state and recovery of hemiplegia (NIHSS = 6)
Increases the chances of recovery without sequelae or with only minor sequelae by 30 %.
Allows recovery of one in eight patients (Fig. 14.2), despite an increased incidence of symptomatic cerebral haemorrhage (6.4 % versus 0.6 % with placebo), without significantly altering the mortality.
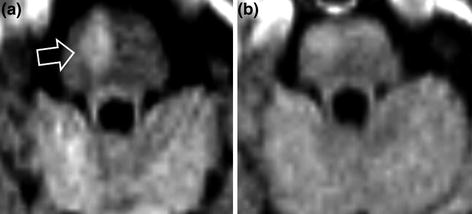

Fig. 14.2
78-year-old female patient with a right paramedian bulbar infarct with left hemiplegia. The NIHSS score was 12. MRI performed 1.5 h after the onset of symptoms shows a slightly decreased ADC with moderately hyperintense signal in the medulla oblongata (a diffusion-weighted sequence, hollow arrow). Fifteen minutes after the start of intravenous thrombolysis, complete recovery of all neurological symptoms (NIHSS = 0). Normal diffusion-weighted images on 24-hour follow-up MRI (b)
Indications
Intravenous thrombolysis should be considered for all cases of suspected infarction with onset of symptoms within the last 4.5 h. Treatment must not be administered if time of onset of symptoms cannot be determined with certainty (for example, presence of a deficit upon waking in the morning).
Strokes in diffusion-weighted images with unknown onset could be consider for thrombolysis if FLAIR sequence is normal, which means that stroke onset is probably less than 3 h (off-label indication).
Contraindications
(as defined in the SPC for Actilyse®)
Main risk factor for post-thrombolysis fatal cerebral haemorrhage is failure to comply with contraindications:
History:
cerebral infarction, severe head injury within the last three months;
diabetic patient with a history of stroke;
cerebral haemorrhage;
gastrointestinal or urinary tract haemorrhage within the last 21 days;
recent myocardial infarction;
recent puncture of a non-compressible vessel;
intercurrent disease;
bacterial endocarditis, pericarditis, pancreatitis, severe liver disease.
Clinical features:
SBP > 185 and/or DBP > 110 at the time of administration of the product;
minor or rapidly resolving neurological deficit, such as an isolated sensory deficit, isolated ataxia, isolated dysarthria or minor motor deficit (in practice when NIHSS < 5 [refer to Appendix 1]);
severe neurological deficit (NIHSS > 22), deep coma;
seizures at the time of onset of the disorders (relative IC).
Laboratory parameters:
Ongoing anticoagulant treatment or INR > 1.7;
Heparin within the last 24 h and prolonged APTT;
Platelet count <100,000/mm3;
Blood glucose <0.50 g/L or >4 g/L.
Radiology:
Early signs of ischaemia involving more than one-third of the middle cerebral artery territory demonstrated on brain CT scan.
Thrombolysis and Brain MRI
Brain CT scan is sufficient, especially when it is performed very soon after the onset of symptoms (recommendations based on CT scan). CT eliminates cerebral haemorrhage or another non-vascular cause for the symptoms.
No validated MRI criteria to define the indications for intravenous thrombolysis, but MRI should be preferred when it is available as first-line imaging procedure.
Advantages of MRI compared to CT:
positive diagnosis of definite infarction;
precise visualization of the extent of ischaemia and possibly the ischaemic “penumbra”;
visualization of the arterial occlusion.
Disadvantages:
longer acquisition time;
contraindications;
absence of validated criteria for contraindications (apart from recent or old cerebral haemorrhage). It sometimes makes treatment decisions more difficult (micro bleeds, absence of visible arterial occlusion).
Special Cases
Pregnant women, children less than 18 years old: no recommendation as excluded from clinical trials. Case by case assessment.
Patients over the age of 80: IV thrombolysis can be considered within the first 3 h (HAS guideline—off-label).
Seizure: does not constitute a real contraindication when ischaemia is documented (value of diffusion-weighted MRI).
Cervical artery dissection without intracranial extension is not a contraindication.
Procedure
rt-PA (alteplase: Actilyse®) must be prescribed by a neurologist or a physician with a specialist diploma in Neurovascular Disease. Treatment must be administered in a unit allowing continuous monitoring of the patient’s neurological status and blood pressure, preferably in a neurovascular unit.
Discuss the risk/benefit balance of thrombolysis with the family and the patient prior to initiation of treatment.
The patient’s general condition must be assessed, including respiratory, cardiac and haemodynamic conditions. Meningitis or endocarditis must be excluded in the presence of fever.
Neurological assessment is essential to assess severity (NIHSS).
Emergency laboratory tests to exclude contraindications to thrombolysis, CT scan or MRI.
Emergency CT scan or MRI (positive diagnosis; eliminate contraindications to thrombolysis).
After obtaining consent from the patient or his/her next of kin, rt-PA may be administered: 0.9 mg/kg (10 % of dose by IV bolus injection, then the rest by slow IV injection over 1 h, not exceeding 90 mg). Blood pressure must be monitored regularly, every 15 min for 3 h, then every 30 min for 6 h and finally every 60 min for 24 h.
Antiplatelet and heparin therapies are contraindicated within the first 24 h following the injection.
Complications
Cerebral haemorrhage (symptomatic in 6–8 % of cases) (Figs. 14.3, 14.4, and 14.5).
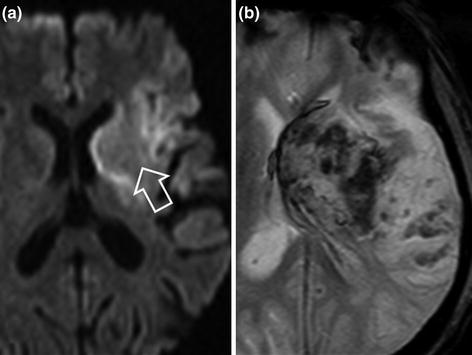
Fig. 14.3
Early complication of intravenous thrombolysis. Patient with infarction in the deep middle cerebral artery territory (a diffusion-weighted sequence, hollow arrow). Deterioration of neurological deficit following intravenous thrombolysis associated with reperfusion haematoma of the infarcted territory, hypointense on the T2*-weighted sequence (b)
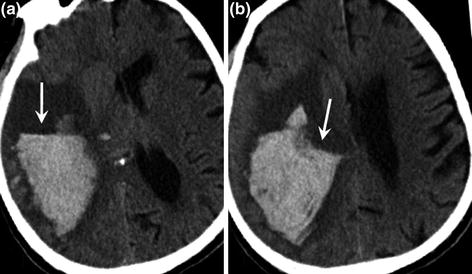
Fig. 14.4
Right parieto-occipital haematoma on CT scan in a patient after IV thrombolysis. Note the characteristic appearance of the haematoma with a fluid level (a and b arrow) related to hypodense noncoagulated blood lying on top of the hyperdense coagulated blood
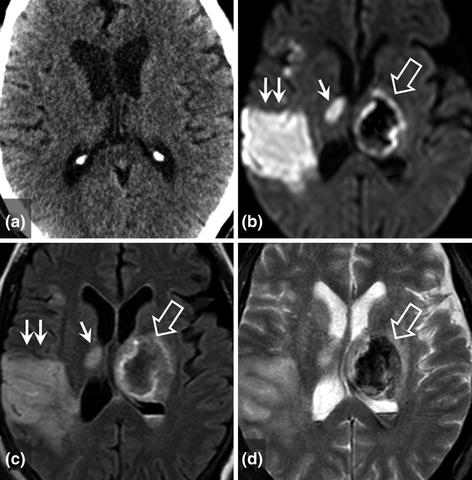
Fig. 14.5
Early complication of intravenous thrombolysis. Patient with superficial middle cerebral artery infarction with normal early imaging less than 3 h after onset of symptoms (a CT). Deterioration of neurological deficit after intravenous thrombolysis associated with contralateral thalamic haematoma, hypointense on diffusion-weighted and T2*-weighted sequences (b and d hollow arrows) and isointense on FLAIR images (c hollow arrow). The superficial middle cerebral artery infarction is clearly visible on the follow-up MRI (b and c double arrows) with focal deep involvement (b and c simple arrows)
Risk factors: severe neurological deficit, early CT signs involving more than one-third of the middle cerebral artery territory, lesion on diffusion-weighted images >100 ml, mass effect, age >80 years, high blood pressure, diabetes and/or hypoglycaemia, platelet count <150,000/mm3, protocol violation, other causes of haemorrhage: microbleeds, very low ADC, atrial fibrillation, heart failure, prior platelet antiaggregant therapy.
Systemic haemorrhage.
Allergy.
Angioneurotic oedema.
Intra-Arterial Thrombolysis and Mechanical Thrombectomy (Figs. 14.6 and 14.7)
The clinical outcome after IV thrombolysis is less favourable in the case of proximal occlusion of a cerebral artery than in the case of more distal occlusion. The early recanalisation rate after IV thrombolysis is lower when the clot is situated in a large proximal artery.