and Srinath Samudrala2
(1)
University of Southern California Keck School of Medicine, Los Angeles, CA, USA
(2)
The Spine Institute at Glendale Adventist Medical Center, Glendale, CA, USA
1.
Preoperative otolaryngologic evaluation of upper airway anatomy and velopharyngeal competence using a flexible nasopharyngoscope is obtained. Magnetic resonance imaging (MRI) and computerized tomography (CT) scanning of the craniocervical junction (CCJ) are done to define the location and extent of the lesion as well as cervicomedullary junction compression (Fig. 3.1). Dynamic flexion and extension radiographs of the cervical spine are used to document preoperative instability. Vertebral artery angiograms are not performed routinely.
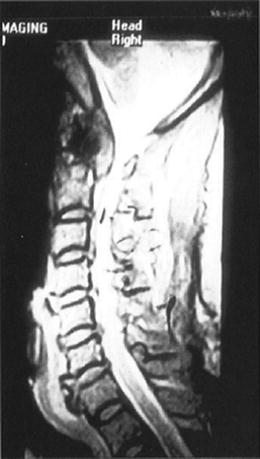

Fig. 3.1
Magnetic resonance imaging (MRI) of the cervical vertebra shows a metastatic lesion at the craniocervical junction with compression of the spinal cord
2.
The patient is placed in a supine position on the operating table with a May-field headrest with the head slightly flexed. The electrodes for somatosensory evoked potential monitoring are attached to the patient. Orotracheal intubation is performed using an oral RAE tube, which is secured in the midline. Rarely, tracheotomy is performed if oral intubation cannot be done. Nasotracheal intubation under flexible endoscopic guidance is avoided, as the nasotracheal tube compromises surgical exposure. [4 , 5]
3.
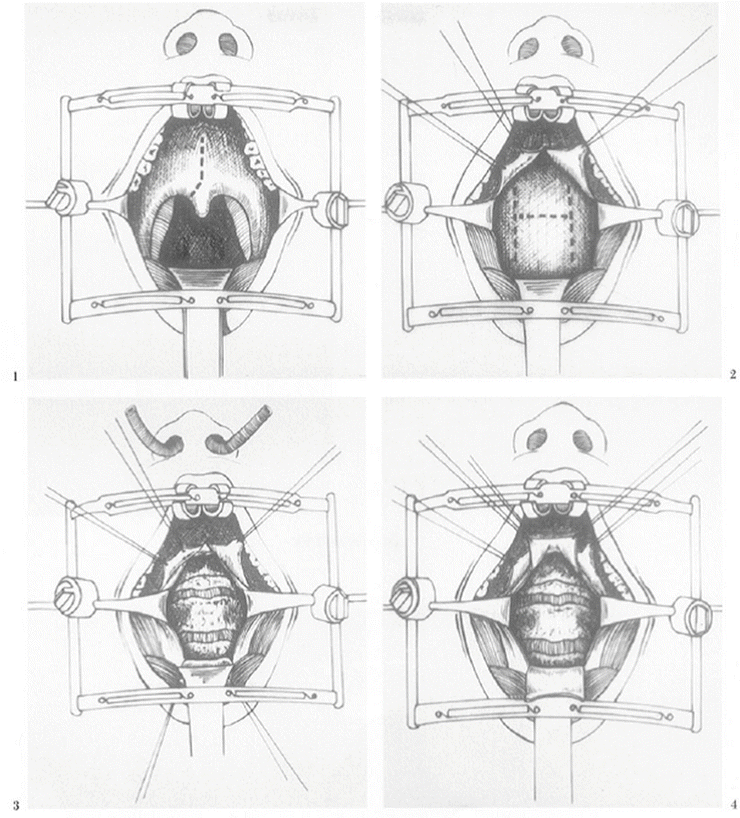
The face and neck are prepared in the usual sterile fashion. During draping no metal clamps are used because they may interfere with identification of the intervertebral spaces by intraoperative radiographic imaging. The oral cavity and oropharynx are rinsed with Peridex using a sterile toothbrush. A specially designed retractor (Spetzler/Sonntag Transoral System; Aesculap, San Francisco, CA) is used for this approach (Fig. 3.2). The ball-and-socket joint of the assembly is secured to the bedrail, near the level of the neck-shoulder interface. The two-piece vertical bar from the fixation bar assembly is attached through the ball-and-socket joint. The horizontal bar is inserted into the vertical bar. The mouth gag with ratchet is carefully inserted into the oral cavity without causing injury to the mucosa, teeth, lips, or gum (Fig. 3.3). A tongue blade of appropriate size is inserted into the mouth gag with the ratchet portion of the blade interfacing with the ratchet portion of the mouth gag. The endotracheal tube is placed in the groove of the tongue blade. The tongue blade is released every half-hour during the entire procedure to prevent ischemia and edema of the tongue. Patients receive perioperative antibiotics and decadron to reduce the chances of oropharyngeal edema. If the transoral system is not available, a Dingman mouth gag can be used for adequate exposure.
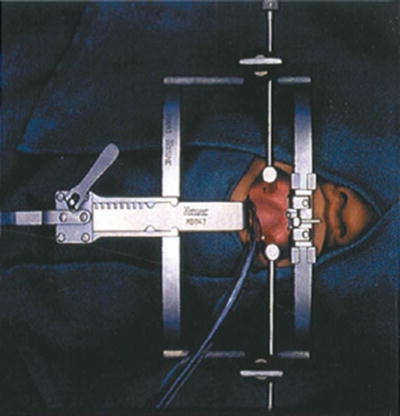
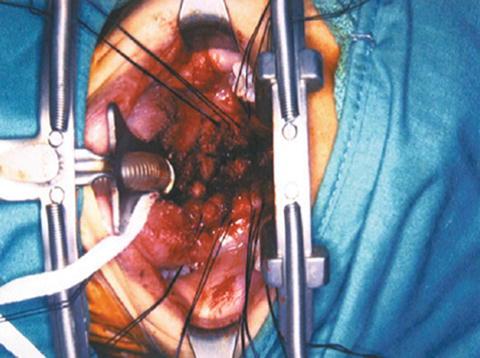

Fig. 3.2
Spetzler/SonntagTransoral System. 1 = Mouth gag with ratchet (2); 3 = tongue blade; 4 = a pair of adjustable, low-profile pharyngeal retractors; 5 = clamps on the mouth gag for holding the pharyngeal retractors in position; 6 = a portion of the mouth gag that is attached to the fixation bar (not shown) using quick-connect coupling

Fig. 3.3
The mouth gag with ratchet is carefully inserted into the oral cavity without causing injury to the mucosa, teeth, lips, or gum
4.
The soft palate, posterior portion of the hard palate, and the posterior pharyngeal wall are infiltrated with 1 % lidocaine with 1:100,000 epinephrine. Using a scalpel, the soft palate is divided in its midline extending from the hard palate to the base of the uvula, and then deviating to one side of the uvula (Fig. 3.4a). Bleeding is controlled by using bipolar cautery. Alternatively, splitting of the soft palate is done by using bipolar scissors (Ethicon; Johnson & Johnson, Somerville, NJ) [6]. Unipolar cautery is never used to split the palate as this may interfere with restoration of palatal function and may increase the chance of wound dehiscence. The split soft palate is then retracted laterally using 2–0 silk stay sutures, exposing the posterior pharyngeal wall widely.