and Aditya G. Shivane1
(1)
Cellular and Anatomical Pathology Level 4, Derriford Hospital, Plymouth, UK
Abstract
Injury to the brain and spinal cord remains the commonest cause of death in young adults in many regions of the world. This chapter describes the pathology of head and spinal cord injury, including the types of haemorrhage, diffuse axonal injury and effects of internal herniations. The pathological findings in inflicted head injury in children and chronic traumatic encephalopathy are also described.
Keywords
TraumaHead injuryContusionsDAIInjury to the brain and spinal cord remains an important cause of long term disability, and in Europe and North America, is the commonest cause of death in individuals under the age of 45 years. The majority of cases result from falls, road traffic accidents, assaults and contact sports. The incidence is highest in children, young adults and the elderly, and is about twice as common in males compared with females. Alcohol ingestion is often a factor in the aetiology of adult head injury.
A simple clinical assessment of the severity of head injury in adults can be undertaken using the Glasgow coma score [1]. A score of less than 9 is classified as severe head injury and is associated with a poorer outcome.
Injury to the head can be broadly classified as either missile or non-missile, with differing patterns of pathology. Non-missile, or blunt, head injury is most often caused by rapid acceleration or deceleration of the head with or without impact, and occasionally by crushing of the head. By contrast missile injuries are due to impact of the head by rapidly moving external objects such as a bullet, and may result in penetration into the cranial cavity. Blunt head injury causes both localised and diffuse brain injury, some of which develops at the time of the head injury, however secondary processes may also develop over several hours to days such as brain ischemia, hypoxia, swelling and infection. In a significant minority of patients with severe head injury, and individuals with repetitive low impact head injury, the development of chronic traumatic encephalopathy with progressive neurological deterioration years later may occur.
The outcome of head injury is related both to the severity and the nature of the initial event and patient factors such as age, co-morbidity including other injuries, sepsis and treatment. Genetic factors also play a role and, in particular, polymorphisms for the apolipoprotein E gene affect the pathological changes and clinical outcome from head injury, with individuals possessing two copies of the ε4 allele having a worse outcome than those without this allele [2, 3].
13.1 Focal Injury
13.1.1 Scalp Injury
Lacerations, abrasions and bruising to the scalp are common and are a good indicator of the site of impact. In some cases scalp injury may give an indication of the type of object that came into contact with the head. Generally scalp lacerations are not of great clinical significance, however, they can result in profuse haemorrhage and are a potential source of infection. It should be noted that bruising is not always a result of direct impact for example periorbital bruising (‘Raccoon eyes’) is commonly associated with orbital roof fracturing as a result of a contrecoup injury e.g. after falling backwards and hitting the occiput, and mastoid bruising (Battle’s sign) occurs secondary to fracture of the petrous temporal bone and tracking of blood, often a few days after the injury.
13.1.2 Skull Fractures
These indicate that significant force was involved in the injury, and may occur either as a coup injury being initiated at the point of impact, or as a contrecoup type injury. Contrecoup fractures commonly involving the roofs of the orbits following a fall backwards, landing on the back of the head resulting in a shockwave passing through the skull and shattering the relatively thin orbital bones. Linear skull fractures are common and radiate from the point of impact along lines of least resistance, and may involve both the calvarium and skull base. A deep linear fracture extending from side to side across the middle cranial fossa through the petrous ridges and pituitary fossa may result in a ‘hinge fracture’ and indicates severe side to side impact of the skull, and is usually associated with fatal head injury. A ‘ring fracture’ through the posterior middle fossa and encircling the foramen magnum indicates either severe hyperextension of the neck or a fall from a height, landing on the feet forcing the spinal column upwards. If a forceful heavy impact is spread over a wider surface area, the skull may be fractured into multiple fragments (‘comminuted fracture’), and if over a small area, may result in a ‘depressed fracture’ whereby a portion of bone is pushed inwards indenting the brain which requires surgical decompression. Fractures may follow suture lines (‘diastatic fracture’), particularly in childhood before the sutures are fully ossified.
Skull fractures are associated with an increased risk of intracranial infection, particularly ‘compound fractures’ where the overlying skin is lacerated, and also with an increased risk of intracranial haemorrhage. Fractures, particularly basal skull, may result in CSF leakage and the formation of aeroceles within the cranial cavity.
13.1.3 Brain Contusions and Lacerations
Superficial areas of bruising to the brain (‘contusion’), often associated with tearing of the pia (‘laceration’), are common after non-missile head injuries. Brain contusions (Fig. 13.1) usually follow a stereotypical pattern which is independent of the site of injury, with involvement of the crests of gyri, particularly involving the frontal poles, orbital surfaces of the frontal lobes, temporal poles, lateral and inferior surfaces of the temporal lobes and occipital poles. They occur commonly after rapid deceleration of the head (e.g. after falling backwards and hitting the back of the head), and are due to the continued movement of the relatively soft brain across the hard irregular surface of the skull. Contusions are less common in infants where the floor of the skull has a smooth outline. Contusions may also occur adjacent to a fracture (‘fracture contusion’), or in relation to brain herniation (‘herniation contusion’), such as compression of the brain against the free edge of the tentorium cerebelli or externally against the skull edge at the site of the craniectomy defect. If the area of brain contusion extends through a laceration into the subdural space then this is known as a ‘burst lobe’ and is most common in the frontal and temporal lobes. Bleeding into an area of contusion may continue for many hours after the initial injury, contributing to raised intracranial pressure. After a period of weeks or months the contusions will resorb, resulting in scarring and yellow/brown discolouration from blood breakdown products. Many contusions are asymptomatic, although they may be a trigger for chronic epilepsy.
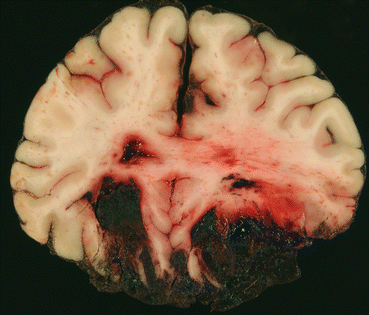

Fig. 13.1
Acute contusions, showing areas of superficial haemorrhage in the inferior frontal lobes
13.2 Traumatic Intracranial Haemorrhage
13.2.1 Extradural Haemorrhage
This commonly occurs as a result of tearing of the middle meningeal artery in association with a fracture of the squamous temporal bone as a direct result of impact. Although the bleeding is arterial, due to the dense adherence of the dura to the inner aspect of the skull, it may take several hours for significant accumulation of blood, resulting in an initial lucid interval. Extradural haemorrhage is seen in approximately 10 % of individuals with severe head injury and is not always associated with a skull fracture, particularly in children due to the greater flexibility of the skull. The accumulation of blood is classically biconvex on imaging and requires urgent surgical drainage.
13.2.2 Subdural Haemorrhage
This results from tearing of the bridging veins crossing the subdural space, particularly those adjacent to the superior sagittal sinus. This is due to rapid deceleration of the head and continued movement of the brain within the cranial cavity stretching these short veins. It is particularly common in the elderly where brain atrophy allows greater movement of the brain within the cranial cavity. Acute subdural haemorrhage presents shortly after head injury (Fig. 13.2), however, if bleeding is slow it may present in a subacute form (1–2 weeks after injury) or as a chronic subdural haemorrhage (more than 2 weeks after injury). The head injury may not be severe, particularly in the elderly, patients on anticoagulation and alcoholics. In the acute phase, haemorrhage has a ‘blackcurrant jelly’ appearance and after a period of several days separates into serous fluid with an organising membrane of granulation tissue on both the dural and pial surfaces, developing over 1–2 weeks. Re-bleeding may occur, possibly due to haemorrhage from newly formed blood vessels within the granulation tissue and fibrinolysis.