Tumor
 General Information
General Information
1. True or False. The following tumor is considered to be a World Health Organization (WHO) grade IV: |
| G7 p.582:97mm |
a. anaplastic astrocytoma | false (Anaplastic astrocytoma is a grade III.) | G7 p.582:117mm |
b. gliosarcoma | true | G7 p.582:12mm |
c. fibrillary astrocytoma | false (Fibrillary astrocytoma is a grade II.) |
|
d. subependymal giant cell astrocytoma | false (Subependymal giant cell astrocytoma is a grade II.) | G7 p.582:148mm |
2. True or False. Tumors of mixed neuronal-glial origin include the following: |
| G7 p.583:45mm |
a. ganglioglioma | true |
|
b. central neurocytoma | true |
|
c. primitive neuroectodermal tumor (PNET) | false (Primitive neuroectodermal tumor [PNET] is listed under embryonal tumors. Old nomenclature is medulloblastoma—small round blue cell tumor.) |
|
d. desmoplastic infantile ganglioglioma (DIG) | true |
|
3. Complete the following about general tumor information: |
| G7 p.583:95mm |
a. Medulloblastoma is considered to be what type of tumor? | embryonal |
|
b. It is also known as_____. | PNET |
|
4. What are the two types of craniopharyngioma? |
| G7 p.584:180mm |
a. a_____ | adamantinomatous (“Adam Antinomatous”) |
|
b. p_____ | papillary | |
5. List the four most common presentations of brain tumor and their frequency. |
| G7 p.585:160mm |
a. p_____ n_____ d_____— _____% | progressive neurologic deficit—68% |
|
b. h_____—_____% | headache—54% |
|
c. m_____ w_____—_____% | motor weakness—45% |
|
d. s_____—_____% | seizure—26% |
|
6. When encountering a first-time seizure in a patient older than 20 years of age, think_____until proven otherwise. | tumor | G7 p.586:38mm |
 Infratentorial Tumors
Infratentorial Tumors
7. What is the name of the so-called vomiting center? | area postrema | G7 p.586:145mm |
8. What nerve has the longest intracranial course? | sixth nerve (abducens) | G7 p.586:160mm |
9. Matching. Match the area of cerebellum with symptoms. |
| G7 p.586:165mm |
Area of cerebellum: |
|
|
|
|
|
a. Ataxia of extremities |
|
|
b. Broad-based gait |
|
|
c. Truncal ataxia |
|
|
d. Dysmetria |
|
|
e. Intention tremor |
|
|
f. Nystagmus |
|
|
g. Cranial nerve dysfunction |
|
|
10. Complete the following concerning a > 20-year-old patient presenting with a headache: |
| G7 p.587:120mm |
a. The classical headache of brain tumor includes |
|
|
i. a.m._____ | worse |
|
ii. strain cough_____ | increases |
|
iii. bending forward_____ | increases |
|
iv. associated with n_____ and/or v_____ | nausea and/or vomiting |
|
b. Is this constellation truly suggestive of brain tumor? | no |
|
c. What percentage have these “classic” headaches? | 8% (77% had headache similar to tension headache, 9% were similar to migraine, only 8% showed classic brain tumor headache; two thirds of these had high intracranial pressure [ICP]) | |
11. Familial syndromes |
|
|
a. are associated with_____ _____ | CNS tumors | G7 p.588:40mm |
b. which are (Hint: vntLT): |
|
|
i. v_____ _____-_____ | von Hippel-Lindau |
|
ii. n_____ | neurofibromatosis |
|
iii. t_____ _____ | tuberous sclerosis |
|
iv. L_____-_____ | Li-Fraumeni |
|
v. T_____ | Turcot |
|
12. Matching. Match the familial syndromes with the associated CNS tumors. |
| G7 p.588:40mm |
Syndromes: |
|
|
|
|
|
CNS tumors: |
|
|
a. PNET |
|
|
b. glioblastoma multiforme (gbm) |
|
|
c. hemangioblastoma |
|
|
d. subependymal grant cell astrocytoma |
|
|
e. vestibular schwannoma |
|
|
13. True or False. The following central nervous system (CNS) tumors occur in neurofibromatosis (NF): |
| G7 p.588:108mm |
a. acoustic (vestibular schwannoma) | true (bilateral) |
|
b. meningioma | true |
|
c. ependymoma | true |
|
d. astrocytoma | true (otherwise known as multiple inherited schwannomas, meningiomas, and ependymomas) |
|
e. ganglioglioma | false |
|
14. True or False. The beneficial effect of steroids is greater for |
| G7 p.588:115mm |
a. metastatic tumor | true |
|
b. primary tumor | false |
|
15. What brain tumor has a generally favorable response to chemotherapy? | oligodendroglioma | G7 p.589:90 mm |
16. What tactics can be used to circumvent the blood-brain barrier (BBB)? |
|
|
Hint: lhdb |
|
|
a. l_____ | lipophilic agent nitrosoureas |
|
b. h_____ | higher doses of medications |
|
c. d_____ | disrupt BBB with mannitol |
|
d. b_____ | bypass BBB with intrathecal methotrexate for primary lymphoma |
|
17. What common medication can be used to disrupt the BBB for chemotherapy delivery? | mannitol | |
18. Complete the following about general tumors: |
| G7 p.589:160mm |
a. What is the proper time to obtain postop computed tomographic (CT) scan after brain tumor surgery? |
|
|
i. to check for bleeding use contrast immediately. True or false? | false |
|
ii. to check for residual tumor use contrast_____? | in the first 2 days postop |
|
b. What period of time would be inappropriate to obtain a postop head CT scan with contrast to assess for residual tumor? | during the period 2 days to 8 weeks after surgery is not a reliable testing time for CT or MRI |
|
c. Any exception to this timing rule of thumb? | yes |
|
i. In what case? | pituitary tumors |
|
ii. How long to wait? | 4 months’ delay is recommended |
|
19. Complete the following about general tumors: |
| G7 p.590:45mm |
a. In a pediatric patient with a posterior fossa tumor, what additional test should be done preoperatively? | MRI of lumbosacral spine with contrast |
|
b. Why? | to rule out drop metastases |
|
c. Why not do it postoperatively when you are sure the test is needed? | because postoperative blood may cause an artifact |
|
d. Artifact will last for_____. | 3 weeks |
|
20. Should we place a shunt or external ventricular drain (EVD) into a pediatric patient with a posterior fossa tumor and hydrocephalus? |
| G7 p.590:60mm |
a. pros |
|
|
i. possible lower o_____ m_____ | operative mortality |
|
b. cons |
|
|
i. l_____ shunt | lifelong |
|
ii. s_____ of peritoneum | seeding |
|
iii. u_____ _____ herniation | upward transtentorial |
|
iv. i_____ in shunt | infection |
|
v. d_____ in definitive treatment | delay |
|
 Primary Brain Tumors
Primary Brain Tumors
21. Characterize low-grade gliomas. |
| G7 p.591:58mm |
a. On T1-weighted image (T1WI), they are _____. | hypointense |
|
b. On T2WI, they are_____. | hypointense |
|
c. What percentage enhance? | 30% only |
|
d. A positron emission tomographic (PET) scan may demonstrate_____. | hypometabolism |
|
e. Can they be diagnosed radiologically? | no (Biopsy is needed for definitive diagnosis.) | |
22. Under the WHO classification an astrocytoma with necrosis is called a_____. | GBM | G7 p.594:168 mm |
23. Complete the following about astrocytoma: |
| G7 p.595:50mm |
a. grade I |
|
|
i. frequency_____% | 0.7% |
|
ii. frequency rule of thumb_____% | 1% |
|
iii. median survival_____years | 10 |
|
iv. peak age incidence_____years | 20 |
|
b. grade II |
|
|
i. frequency_____% | 16% |
|
ii. frequency rule of thumb_____% | 15% |
|
iii. median survival_____years | 4 |
|
iv. peak age incidence_____years | 30 |
|
c. grade III |
|
|
i. frequency_____% | 17% |
|
ii. frequency rule of thumb_____% | 15% |
|
iii. median survival_____years | 1.6 |
|
iv. peak age incidence_____years | 40 |
|
d. grade IV |
|
|
i. frequency_____% | 65% |
|
ii. frequency rule of thumb_____% | 65% |
|
iii. median survival_____years | 0.7 (8.5 months) |
|
iv. peak age incidence_____years | 50 |
|
24. Complete the following regarding astrocytoma: |
| G7 p.595:122mm |
a. longevity with low-grade astrocytoma |
|
|
i. aged 45 or younger_____ | ˜5 years |
|
ii. aged 45 or older_____ | ˜1½ years |
|
b. why? |
|
|
i. Because low-grade astrocytomas undergo_____ _____ | malignant transformation |
|
ii. _____-fold more rapidly after | six |
|
iii. age_____ | 45 |
|
25. List astrocytoma GBM microscopic characteristics. |
| G7 p.596:73mm |
Hint: cgppmnn |
|
|
a. c_____ | cellular |
|
b. g_____ a_____ | gemistocytic astrocytes |
|
c. p_____ | pleomorphism |
|
d. p_____ | pseudopallisading |
|
e. m_____ | mitosis |
|
f. n_____ | necrosis |
|
g. n_____ | neovascularization |
|
26. True or False. The following fluid clots: |
| G7 p.596:120mm |
a. cerebrospinal fluid (CSF) | false |
|
b. cyst fluid | true |
|
c. subdural fluid | false |
|
d. blood | true | |
27. Describe astrocytoma CT and MRI characteristics. |
| G7 p.596:165mm |
a. grade I |
|
|
i. CT | low |
|
ii. MRI | abnormal |
|
iii. mass? | no |
|
iv. enhancement? | no |
|
b. grade II |
|
|
i. CT | low |
|
ii. MRI | abnormal |
|
iii. mass? | yes |
|
iv. enhancement? | no |
|
c. grade III |
|
|
i. CT | low |
|
ii. MRI | abnormal |
|
iii. mass? | yes |
|
iv. enhancement? | yes |
|
d. grade IV |
|
|
i. CT | low |
|
ii. MRI | abnormal |
|
iii. mass? | yes |
|
iv. enhancement? | ring |
|
e. In ring enhancement the center represents |
|
|
i. n_____ and the rim is | necrosis | G7 p.597:88mm |
ii. c_____ t_____. | cellular tumor |
|
28. Meningeal gliomatosis occurs in_____% of high-grade gliomas at autopsy. | 20% | G7 p.598:52mm |
29. True or False. Treatments for low-grade gliomas should generally include |
| G7 p.598:145mm |
a. biopsy or surgery for tissue diagnosis | true |
|
b. excisional biopsy | false |
|
c. radiation | false |
|
d. chemotherapy | false |
|
e. excision of pilocytic astrocytomas | true |
|
f. removal because the more tumor removed improves longevity | false (not clearly proven) | G7:p.599:15mm |
30. Complete the following regarding stereotactic biopsy: |
| G7 p.600:20mm |
a. It underestimates the occurrence of GBM by_____%. | 25% |
|
b. Some CNS_____ mimic GBM radiographically. | lymphomas |
|
c. Yield of biopsy is highest when |
|
|
i. low density_____ and | center |
|
ii. enhancing_____ are both sampled. | rim |
|
d. If Karnosky rating is higher than_____ | 70 |
|
e. it portends a_____ prognosis. | better | |
31. Answer the following concerning malignant astrocytoma grade III or IV: |
| G7 p.600:120mm |
a. True or False. Treatment is surgical excision when possible. | true |
|
b. Prognosis from surgical excision and radiotherapy is_____ weeks in the elderly. | 30 |
|
c. Prognosis from biopsy and radiotherapy is_____ weeks in the elderly. | 17 |
|
d. Type of radiotherapy advised is_____. | focal |
|
e. Amount is_____ Gy. | 50 to 60 |
|
32. Characterize wounded glioma syndrome. |
| G7 p.600:175mm |
a. Partial resection of a GBM carries significant risk of_____ | hemorrhage |
|
b. or_____ | edema |
|
c. with resultant_____. | herniation |
|
d. The benefit of subtotal resection is_____. | dubious |
|
e. Surgical excision should be considered if total removal is_____. | feasible |
|
33. Characteristic radiation therapy for |
| G7 p.601:35mm |
a. malignant gliomas is_____ Gy. | 50 to 60 |
|
b. Is whole brain x-ray treatment (XRT) valuable? | no (It does not increase survival.) |
|
34. Considering malignant gliomas, what is the only protocol fully validated by a phase 3 study for treatment of malignant glioma? |
| G7 p.601:125mm |
a. s_____ | surgery—maximal resection |
|
b. r_____, _____ Gy | radiation, 60 Gy |
|
c. c_____ (B_____) | chemotherapy (BCNU at 6-week intervals) |
|
35. Matching. Match level of risk with patient characteristics. |
| G7 p.603:45mm |
Risk: |
|
|
|
|
|
Patient characteristics: |
|
|
a. Age under 40 |
|
|
b. Age between 40 and 65 |
|
|
c. Frontal tumor |
|
|
d. Tumor outside frontal lobe |
|
|
e. Karnofsky scale < 80 |
|
|
f. Age above 65 |
|
|
g. Subtotal resection (STR) |
|
|
h. Gross total resection (GTR) |
| |
36. What are the common locations of pilocytic astrocytoma? |
| G7 p.603:118mm |
Hint: hoc |
|
|
a. h_____ | hypothalamus |
|
b. o_____ _____ | optic chiasm |
|
c. c_____ | cerebellum |
|
37. Characterize pilocytic astrocytoma. |
| G7 p.604:110mm |
a. Appearance on CT and MRI |
|
|
i. True or False. It enhances. | true (enhancing lesion) |
|
ii. True or False. It is solid. | false (often cystic) |
|
iii. It may have a_____ nodule. | Mural |
|
iv. True or False. It is diffuse. | false (well circumscribed) |
|
b. You should resect the wall of the cyst if the wall_____. | enhances |
|
38. Characterize the radiologic appearance of pilocytic astrocytoma. |
| G7 p.604:110mm |
a. What is their shape? | well circumscribed |
|
b. Do they enhance? | yes—on MRI and CT |
|
c. Are they cystic? | yes |
|
d. Is there anything in the cyst? | mural nodule |
|
e. Are they surrounded by edema? | no |
|
f. Where are they located? | periventricular | G7 p.604:135mm |
39. Complete the following about primary brain tumor: |
| G7 p.605:15mm |
a. cystic cerebellar astrocytoma |
|
|
i. incidence in adults_____% | 10% of CNS tumors |
|
ii. percentage of childhood tumors_____% | 27 to 40% of posterior fossa |
|
b. optic glioma |
| G7 p.606:15mm |
i. incidence in adults_____% | 2% of gliomas |
|
ii. percentage of childhood tumors_____% | 7% of gliomas |
|
c. brain stem gliomas |
| G7 p.607:45mm |
i. incidence in adults_____% | 1% of CNS tumors |
|
ii. percentage of childhood tumors_____% | 10 to 20% of CNS tumors |
|
d. oligodendroglioma |
| G7 p.609:155mm |
i. incidence in adults_____% | 2 to 4% of CNS tumors and 35% of all gliomas |
|
ii. percentage of childhood tumors_____% | small% |
|
e. meningioma |
| G7 p.613:125mm |
i. incidence in adults_____% | 15 to 20% |
|
ii. percentage of childhood tumors_____% | 1.5% of CNS tumors |
|
f. vestibular schwannoma |
| G7 p.620:160mm |
i. incidence in adults_____% | 8 to 10% |
|
ii. percentage of childhood tumors_____% | 0% | |
40. According to Collins’ law, a patient’s tumor is considered cured if |
| G7 p.605:160mm |
a. it does_____ recur | not |
|
b. after a postop period equal to the patient’s_____ | age |
|
c. plus_____. | 9 months |
|
41. Consider treatments for optic glioma. |
| G7 p.606:85mm |
a. One optic nerve involved sparing chiasm, painless proptosis, gliosis of optic nerve head on funduscopy perform_____ and_____ _____. | craniotomy and orbital exploration |
|
i. Treatment should be to e_____ o_____ n_____ | excise optic nerve |
|
ii. from g_____ b_____ | globe back |
|
iii. to c_____. | Chiasm |
|
b. More posterior lesions with nonspecific visual defects, no proptosis, hypothalamic dysfunction, pituitary dysfunction, hydrocephalus, it is likely a _____ _____. | chiasmal lesion |
|
i. Treatment should be b_____ and | biopsy |
|
ii. X_____. | XRT |
|
42. Diencephalic syndrome consists of |
| G7 p.606:135mm |
Hint: diencephalic |
|
|
i. d_____ s_____ | diencephalic syndrome |
|
ii. i_____ a_____ r_____ | intraventricular appearance radiographically |
|
iii. e_____ e_____ | excessively energetic |
|
iv. n_____ | macrocephaly |
|
v. c_____ | cachexia |
|
vi. e_____ | euphoria |
|
vii. p_____ | failure to thrive |
|
viii. h_____ | hypoglycemia |
|
ix. a_____ h_____ | anterior hypothalamus |
|
x. l_____ of s_____ f_____ | loss of subcutaneous fat |
|
xi. i_____ | infiltrating |
|
xii. c_____ u_____ | children usually |
|
43. Characterize brain stem glioma. |
| G7 p.607:28mm |
a. Lower-grade tumors tend to occur in the_____ brain stem. | higher |
|
b. Higher-grade tumors tend to occur in the_____ brain stem. | lower |
|
c. They present with_____ _____ _____ _____. | multiple cranial nerve palsies |
|
d. True or False. Most are surgical candidates. | false |
|
44. How do upper brain stem gliomas present? |
| G7 p.607:65mm |
a. c_____ f_____ | cerebellar findings |
|
b. h_____ | hydrocephalus | |
45. How do lower brain stem gliomas present? |
| G7 p.607:65mm |
a. l_____ c_____ n_____ | lower cranial nerves |
|
b. l_____ t_____ f_____ | long tract findings |
|
46. Characterize four categories of brain stem gliomas. |
| G7 p.607:120mm |
a. diffuse |
|
|
i. location _____, _____, _____ | pons, medulla, cord |
|
ii. glioma grade_____ | malignant |
|
iii. percent_____% | 100% |
|
iv. treatment_____ _____ | no surgery |
|
b. cervicomedullary |
|
|
i. location_____ | cervicomedullary |
|
ii. glioma grade_____ | low |
|
iii. percent_____% | 72% |
|
iv. treatment_____ _____ _____ | surgery if exophitic |
|
c. focal |
|
|
i. location_____ | medulla |
|
ii. glioma grade_____ | low |
|
iii. percent_____% | 66% |
|
iv. treatment_____ _____ _____ | surgery if exophitic |
|
d. exophytic |
|
|
i. location _____, _____ _____ | medulla, spinal cord |
|
ii. glioma grade_____ | low |
|
iii. percent_____% | 60% |
|
iv. treatment_____ _____ _____ | surgery is okay |
|
47. How do brain stem gliomas appear on MRI? |
| G7 p.607:175mm |
a. T1_____ | hypointense |
|
b. T2_____ | increased signal |
|
c. gad_____ | gadolinium highly variable |
|
48. Complete the following about brain stem gliomas: |
| G7 p.608:140mm |
a. Prognosis of most patients is_____ months. | 6 to 12 |
|
b. Subgroup of dorsally exophytic pilocytic astrocytomas have a longer survival of up to_____ years. | 5 | G7 p.608:150mm |
49. Characterize tectal gliomas. |
| G7 p.608:165mm |
a. Pathology is usually_____-_____ _____ that | low-grade astrocytoma |
|
b. presents with_____. | hydrocephalus |
|
c. Diagnostic study of choice is_____. | MRI |
|
d. Symptoms resolve with treatment of the _____. | hydrocephalus | |
e. MRI appearance |
|
|
i. mass arising from the q_____ p_____ | quadrigeminal plate |
|
ii. on T1_____ | isointense |
|
iii. on T2_____ | iso- or hyperintense |
|
iv. gadolinium_____%_____ | 18% enhance |
|
f. Treatment |
|
|
i. s_____ or | shunt |
|
ii. t_____ v_____ | third ventriculostomy |
|
50. Characterize oligodendroglioma. |
| G7 p.609:120mm |
a. Presenting symptom is_____ in_____%. | seizure in 50 to 80% |
|
b. Calcified on |
|
|
i. _____% of skull x-rays | 30 to 60% |
|
ii. _____% of CT scan | 90% |
|
c. Oligodendroglioma cells in a tumor suggests what for the patient? | a better prognosis |
|
51. Characterize oligodendrogliomas. |
| G7 p.609:155mm |
a. They have a predilection for the f_____ l_____. | frontal lobes |
|
b. A classic description of cytoplasm is f_____ e_____. | fried egg |
|
c. The role of chemotherapy is the p_____ t_____ | primary treatment |
|
d. after s_____ r_____. | surgical resection |
|
52. What are the chemotherapy agents used for oligodendrogliomas? |
| G7 p.611:30mm |
Hint: Cvpt |
|
|
a. C_____ | CCNU |
|
b. v_____ | vincristine |
|
c. p_____ | procarbazine |
|
d. t_____ | temozolomide |
|
53. Prognosis: best, middle, worst. Relate. |
| G7 p.611:130mm |
a. Pure oligodendroglioma | best |
|
b. Mixed oligodendroglioma | middle |
|
c. Pure astrocytoma | worst |
|
54. Complete the following regarding prognosis: |
| G7 p.611:130mm |
a. An oligodendroglial component conveys a_____ prognosis. | better |
|
b. Pure oligo 10-year survival is_____%. | 10 to 30% |
|
c. Postop survival is_____ to_____ months. | 35 to 52 |
|
d. Calcification in an oligodendrogliioma (ODG) conveys a_____ prognosis. | better |
|
e. Loss of chromosome 1p conveys a_____ prognosis. | better |
|
f. Loss of chromosome 1p and 19q conveys a_____ prognosis. | better | |
55. Describe central neurocytoma. |
| G7 p.612:105mm |
a. It is located in the l_____ v_____ | lateral ventricles |
|
b. or in the s_____ p_____. | septum pellucidum |
|
c. It tends to affect y_____ a_____ | young adults |
|
d. and is curable by t_____ r_____. | total resection |
|
56. Characterize meningiomas. |
|
|
a. They arise from what cell of origin? | arachnoid cap cell | G7 p.613:90mm |
b. What percentage of meningiomas occur at the falx? (includes parasagittal) | 60 to 70% | G7 p.613:155mm |
c. With foot drop plus hypereflexia, think_____ _____. | parasagittal meningioma | G7 p.614:50mm |
d. Olfactory groove meningiomas |
| G7 p.614:68mm |
i. can produce what syndrome? | Foster Kennedy |
|
ii. consisting of a_____, i_____ o_____ a_____, and c_____ p_____ | anosmia, ipsilateral optic atrophy, and contralateral papilledema |
|
iii. What other syndrome? | frontal lobe |
|
iv. consisting of a_____, i_____ | apathy, incontinence |
|
57. Abulia is |
| G7 p.614:85mm |
a. l_____ o_____ w_____. | lack of willpower |
|
b. characteristic of damage to f_____ l_____. | frontal lobes |
|
c. can occur with a meningioma of the o_____ g_____. | olfactory groove |
|
58. Give a description of asymptomatic meningiomas. |
| G7 p.615:30mm |
a. The most common primary intracranial tumor is_____. | meningioma |
|
b. Percent of primary brain tumors that are meningiomas_____% | 32% |
|
c. Percent that are stable in size over 2½ years_____% | 66% |
|
d. Percent that increase in size when observed for 2½ years_____% | 33% |
|
e. What does calcification tell us about rate of growth? | slower |
|
f. Operative morbidity in patients under 70_____% | 3.5% |
|
g. Above 70_____% | 23% |
|
h. Classic histological finding is the p_____ b_____. | psammoma body |
|
59. Complete the following about MRI and meningioma: |
| G7 p.616:175mm |
a. Meningioma on T1W1 and T2W1 may be _____. | isodense |
|
b. With contrast most will_____. | enhance |
|
c. Accurately predicts sinus involvement in _____%. | 90% |
|
d. A common finding is a d_____ t_____. | dural tail |
|
60. What metastatic cancer can mimic meningioma in the bone on MRI? | prostate | G7 p.617:40 mm |
61. Olfactory groove meningiomas tend to be fed by the |
| G7 p.617:52mm |
a. _____arteries | ethmoidal |
|
b. which are branches of the_____ artery. | ophthalmic |
|
62. The artery of B_____and C_____is enlarged in lesions involving the tentorium (i.e., tentorial meningiomas). | Bernasconi and Cassinari (a branch of the meningohypophyseal trunk) | G7 p.617:65mm |
63. True or False. The artery most likely to be enlarged on an angiogram depicting a tentorial meningioma is the |
| G7 p.617:65mm |
a. superficial temporal artery | false |
|
b. artery of Bernasconi and Cassinari | true |
|
c. occipital artery | false |
|
d. posterior inferior cerebellar artery | false |
|
e. anterior choroidal artery | false |
|
64. Regarding meningiomas and plain x-rays, the plain x-rays may show |
| G7 p.617:110mm |
a. b_____ _____ _____ | blistering of bone |
|
b. c_____ _____ _____ | calcification in tumor 10% |
|
c. d_____ _____—_____ | density changes—hyperostosis |
|
d. e_____ _____ _____ | enlarged vascular grooves |
|
e. f_____ _____ _____ | frontal fossa hyperostosis |
|
65. Complete the following regarding sinus involvement: |
| G7 p.618:20mm |
a. Occlusion of middle third of the SSS is _____. | treacherous |
|
b. Morbidity/mortality is_____/_____%, | 8/3% |
|
c. due to v_____ i_____. | venous infarction |
|
66. Complete the following regarding sinus involvement: |
| G7 p.618:60mm |
a. The sinus may be divided safely anterior to the_____ _____. | coronal suture |
|
b. Posterior to this site the sinus_____ _____ be divided. | must not |
|
c. If tumor is attached, it is best to leave_____ _____. | residual tumor | G7 p.618:82mm |
d. True or False. It is safe to occlude the dominant transverse sinus. | false | G7 p.618:92mm |
67. Complete the following about the removal of meningiomas: |
| G7 p.619:140mm |
a. The Simpson grading system grades the degree of removal of _____. | meningiomas |
|
b. It is important because it correlates with_____ _____. | recurrence rate |
|
c. Components of the system are | In order of complexity, from minimal surgery to complete removal: |
|
i. s_____ r_____,b_____ | small removal, biopsy |
|
ii. p_____ r_____ | partial removal |
|
iii. c_____ r_____ | complete removal |
|
iv. c_____ d_____ | coagulate dura |
|
v. r_____ d_____ and b_____ ands_____ | remove dura and bone and sinus |
|
d. Correlates with grade | ||
i. _____ | V |
|
ii. _____ | IV |
|
iii. _____ | III |
|
iv. _____ | II |
|
v. _____ | I |
|
e. What is the most important factor regarding recurrence? | extent of tumor removal |
|
68. Five year survival for patients with menigioma is _____%. | 91.3% | G7 p.619:150mm |
 Vestibular Schwannoma
Vestibular Schwannoma
69. True or False. Vestibular schwannomas (VS) usually arise from which nerve? |
| G7 p.620:145mm |
a. facial nerve | false |
|
b. cochlear nerve | false |
|
c. nervus intermedius | false |
|
d. vestibular nerve, inferior division | false |
|
e. vestibular nerve, superior division | true |
|
70. Vestibular schwannomas arise from the junction of the _____and_____ myelin called the_____-_____zone. | central and peripheral; Obersteiner-Redlich | G6p.429:170mm |
71. Complete the following about primary brain tumors: |
| G6p.429:175mm |
a. What is the Obersteiner-Redlich zone? | site of junction of central and peripheral myelin |
|
b. Where is it located? | 8 to 12 mm from brain stem |
|
c. From what cells do acoustic tumors arise? | from the neurilemmal sheath |
|
d. On what structure do they arise? | the superior division of the vestibular nerve |
|
e. Therefore, are they schwannomas or neuromas? | schwannomas |
|
f. They are the result of a chromosomal defect that leads to |
| |
i. loss of a t_____ s_____gene on the | tumor suppressor on the | G7 p.620:148mm |
ii. l_____ arm of c_____ #_____. | long arm of chromosome 22 |
|
72. True or False. What is the most common chromosomal defect in vestibular schwannomas? |
| G7 p.620:150mm |
a. P53 mutation | false |
|
b. gain of function mutation on Ch 3 | false |
|
c. loss of tumor suppressor gene on Ch 22 | true |
|
d. loss of tumor suppressor gene on Ch 17 | false |
|
e. loss of heterozygosity on Ch 10 | false |
|
73. List the common triad of symptoms seen with vestibular schwannomas. |
| G7 p.621:40 mm |
a. h_____ -_____ % | hearing loss—98% |
|
b. t_____ -_____ % | tinnitus-70% |
|
c. d_____ -_____ % | dysequilibrium-67% (insidious, progressive, 70% have high-frequency loss, word discrimination difficulties) |
|
74. A patient with good hearing has an MRI study that shows a cerebellopontine angle mass. |
| G7 p.621:65mm |
a. Is this compatible with a vestibular schwannoma? | no (At the time of diagnosis virtually all VS have otologic symptoms.) |
|
b. When hearing is involved in VS, what is lost? |
| |
i. low frequencies? | no |
|
ii. high frequencies? | yes (70% have a high-frequency loss pattern.) |
|
iii. word discrimination? | yes (Most have impaired word discrimination, e.g., telephone conversation.) |
|
75. What cranial nerve deficits, other than CN VIII, occur with vestibular schwannomas? |
| G7 p.621:125mm |
a. CN_____;o_____,f_____ n_____,and t_____ c_____ | CN V; otalgia, facial numbness, and taste changes |
|
b. CN_____;f_____ w_____ | CN VII; facial weakness |
|
c. CN_____;h_____ and d_____ | CN IX, X, XII; hoarseness and dysphagia |
|
76. Answer the following about vestibular schwannoma: |
| G7 p.621:135mm |
a. As tumor increases in size the following occur in what sequence? | C, B, A (Facial numbness occurs earlier than facial |
|
A. facial weakness | weakness even though CN V |
|
B. facial numbness | is only slightly compressed, |
|
C. impaired hearing | whereas CN VII is severely distorted early—a paradox. Why? Differential resilience of motor nerves relative to sensory nerves.) |
|
b. What size tumor causes fifth and seventh nerve compression? | larger than 2 cm |
|
77. Complete the following about vestibular schwannomas: |
| G7 p.621:170mm |
a. What percentage of patients have no abnormal physical findings except for hearing loss? | 66% |
|
b. The Weber test lateralizes to the_____ side. | uninvolved (Hearing loss is sensorineural.) |
|
c. Is the Rinne test positive or negative if hearing is preserved? | positive |
|
d. What is normal for the Rinne test? | air conduction > bone conduction = positive means normal. (Note: An A is better than a B.) | |
78. Complete the following about primary brain tumors: |
| G7 p.622:75mm |
a. In VS what causes nystagmus? | vestibular involvement |
|
b. What fibers constitute VS? | ||
i. A_____ _____ n_____ e_____ b_____ f_____ | Antoni A narrow elongated bipolar fibers |
|
ii. A_____ l_____r_____f_____ | Antoni B loose reticulated fibers |
|
c. What is the growth rate for VS? | 1 to 10 mm/year |
|
d. What is the proper follow-up protocol, if no surgery is done? | repeat scan at 6-month intervals for 2 years then once each year |
|
e. Recommend surgery if what occurs? |
| |
i. size changes by_____ | > 2 mm/year |
|
ii. or symptoms_____ | progress |
|
79. Answer the following about the House and Brackmann scale: |
| G7 p.622:15mm |
a. What does the House-Brackmann scale measure? | clinical measurement of facial nerve function |
|
b. What are the categories? | normal mild moderate moderate-severe severe no movement |
|
c. Synkinesis is defined as i_____m_____ accompanying a v_____m_____. | involuntary movement accompanying a voluntary movement |
|
80. Answer the following about vestibular schwannomas: |
| G7 p.625:30mm and G6p.431:110mm |
a. What is the growth rate of vestibular schwannomas? | slow (1 to 10 mm/year) |
|
b. Do some shrink? | yes (6%) |
|
c. Can they remain stable? | yes |
|
d. Can they grow faster? | yes (2 to 3 cm/year) |
|
e. If followed most will show_____ in 3 years. | enlargement |
|
81. Describe the audiometric findings for “useful” hearing in vestibular schwannomas. | 50/50 rule | G7 p.623:90mm |
a. pure-tone audiogram threshold of_____ | ≤50% |
|
b. speech discrimination of_____ | ≥50% |
|
82. Complete the following regarding the Gardener-Robertson system: |
| G7 p.623:108mm |
a. The Gardener-Robertson system is used to grade h_____ p_____. | hearing preservation |
|
b. It consists of |
| |
i. testing patient with_____ _____ of increasing loudness. | pure tones (decibels [db]) (If patient hears dB 0 to 30—excellent hearing; 30 to 50 dB—serviceable; 50 to 90 dB—nonserviceable; 90 dB max—poor; not testable—none) |
|
ii. Evaluating patient ability to understand spoken words is called_____ _____. | speech discrimination (understands words spoken to him or her correct 100 to 70%-excellent; 70 to 50%—serviceable; 50 to 5%— nonserviceable) |
|
c. Useful hearing is judged to be present up to a cutoff point of_____. | 50/50 patient can hear at 50 dB or less and understands at least 50% of words spoken to him or her |
|
83. Name the findings for the following tests in vestibular schwannomas: |
| G7 p.622:175mm |
a. pure-tone audiogram | hearing difference between eachear>10to15dB | |
b. speech discrimination | 4 to 8% score (normal is 92 to100%) | G7 p.623:45mm |
c. brain stem auditory evoked response (BSAER) | prolonged I-III and I-V interpeak latencies | G7 p.624:45mm |
d. electronystagmography (ENG) | abnormal if one ear has ≤35% of total (Normally, 50% of response is from each ear.) | G7 p.624:20mm |
84. Complete the following concerning vestibular schwannoma: |
| G7 p.623:20mm |
a. It causes what kind of hearing loss? | sensorineural loss of high tones |
|
b. This is the same as the loss from | ||
i. _____ | old age |
|
ii. _____ | loud noise exposure |
|
c. Think tumor if the difference between the ears on audiogram is more than_____ dB. | 10to15 |
|
85. True or False. A 55-year-old male is referred for evaluation of a 4.0 cm right cerebellopontine angle (CPA) mass. You conclude it is a vestibular schwannoma. The following is least likely to be a factor in your treatment. Give rationale for each. |
| G7 p.624:65mm |
a. pure-tone audiogram score of 95 dB | false (Audiogram with hearing threshold <50 dB may allow consideration of hearing—sparing procedure, but with a score of 95 dB hearing—saving procedure is not an option.) | G7 p.622:175mm |
b. effacement of the fourth ventricle with modest ventriculomegaly | false (Evidence of hydrocephalus warrants CSF diversion—needs a shunt.) | G7 p.621:170mm |
c. stereotactic surgery 2 years previously | true (Stereotactic radiosurgery 2 years previously is long enough for SRS effect to be over. Surgery should be avoided during the interval 6 to 18 months after SRS because this is the time of maximum damage from the radiation.) |
|
d. contralateral (left) vestibular schwannoma, 1.0 cm in diameter | false (Bilateral VS unable to preserve right hearing [95 dB], will need to plan for second procedure to address the left-sided lesion. Chance of preserving left hearing— 35 to 71% for a 1 cm tumor.) |
|
e. angiogram showing absence of right transverse sinus | false (Atretic/obstructed right transverse sinus allows consideration of translabyrinthine and suboccipital approach as a combined procedure.) |
|
86. True or False. Possible treatments for vestibular schwannomas include |
| G7 p.624:120mm |
a. expectant observation, following symptons, hearing testing, serial, CT, or MRI | true |
|
b. radiation therapy, external beam radiation therapy (EBRT) | true |
|
c. radiation therapy, stereotactic radiosurgery (SRS) | true |
|
d. retrosigmoid (suboccipital) resection | true |
|
e. translabyrinthine resection | true |
|
f. extradural subtemporal (middle fossa approach) resection | true |
|
87. Complete the following about vestibular schwannoma treatment: |
| G7 p.625:115mm |
a. Under 20 mm can be_____, | observed |
|
b. Protocol is to retest at 6,12,18, 24,36, 48,60, 84,108,and 168_____ | months |
|
c. Growth of more than_____ mm between studies deserves treatment. | 2 |
|
d. Tumors larger than 15 to 20 mm should be_____. | treated |
|
e. Tumors with cysts can_____ _____. | grow dramatically | G7 p.625:103mm |
88. Matching. Match outcome with technique with microsurgery and SRS. |
| G7 p.625:170mm |
Outcome:
Technique: | ||
a. microsurgery |
|
|
b. stereotactic radiosurgery |
|
|
c. equal |
|
|
89. Classically, vestibular schwannomas push the facial nerve in which direction? Pushed_____ and_____ in_____% of cases. | forward and superiorly in 75% | G7 p.627:92mm |
90. Complete the following about vestibular schwannomas: |
| G7 p.627:145mm |
a. Small, laterally located intracanalicular vestibular schwannomas can be removed by what surgical approach? | subtemporal extradural (also known as middle fossa approach) |
|
b. A disadvantage is that the seventh nerve may be_____ at the_____ ganglion. | injured at the geniculate |
|
c. An advantage is that hearing function may be_____. | preserved |
|
91. What is the size vestibular schwannomas should be considered for hearing and CN VII preservation procedures? | < 2 to 2.5 cm | G7 p.627:80mm |
92. What are the advantages of translabyrinthine approach for resecting vestibular schwannomas? |
| G7 p.628:65mm |
a. early identification of the_____ | facial nerve |
|
b. less risk to_____ and_____ _____ _____ | cerebellum and lower cranial nerves |
|
c. best for VS that are located_____ | intracanalicular |
|
93. What are the disadvantages of a translabyrinthine approach for resecting vestibular schwannomas? |
| G7 p.628:65mm |
a. Hearing is_____. | sacrificed |
|
b. Exposure is_____. | limited |
|
c. CSFleakis_____. | more common |
|
94. Complete the following about vestibular schwannomas: |
| G7 p.628:135mm and also G6p.434:122mm |
a. What are the disadvantages of suboccipital approach (also known as retrosigmoid) for vestibular schwannomas? | ||
i. higher_____ when compared with the translabyrinthine approach | morbidity |
|
ii. small tumors_____ | difficult to remove in lateral recess of internal auditory canal (IAC) |
|
iii. facial nerve is located_____ | on blind side deep to the tumor |
|
b. The advantage is the possibility of h_____ p_____. | hearing preservation |
|
95. Complete the following about localizing the VII nerve origin: |
| G7 p.629:145mm |
a. The seventh nerve originates in the_____ sulcus, | pontomedullary |
|
b. anterior to the eighth nerve by_____ mm. | 2 |
|
c. It lies just anterior to the foramen of_____ | Lushka |
|
d. and anterior to a tuft of_____. | choroid |
|
e. It originates _____ mm cephalad to the ninth nerve. | 4 |
|
96. How do you treat postoperative facial nerve weakness after vestibular schwannoma resection? |
| G7 p.630:130mm |
a. N_____T_____ | Natural Tears (2 drops to eye every 2 hours as needed) |
|
b. L_____ | Lacrilube (to eye and tape eye at bedtime) |
|
c. t_____ | tarsorrhaphy within a few days if there is a complete CN VII palsy |
|
d. Anastomose by attaching a portion of the_____ nerve to the_____ nerve | hypoglossal facial |
|
e. When there is no CN VII function and |
| |
i. nerve is known to be divided you may anastomose in_____ | 2 months |
|
ii. nerve is known to be intact you may anastomose in_____ | 1 year |
|
97. True or False. The following symptoms of brain stem compression from a vestibular schwannoma if present postop is not likely to improve: |
| G7 p.630:155mm |
a. nausea | false (Nausea resolves with time.) |
|
b. vomiting | false (Vomiting resolves with time.) |
|
c. balance difficulties | false (Balance difficulties clear rapidly.) |
|
d. ataxia | true (Ataxia from brain stem dysfunction may be permanent.) |
|
98. True or False. The routes of CSF leakage after vestibular schwannoma resection can be via the |
| G7 p.631:20mm |
a. apical cells | true (to tympanic cavities or eustachian tube—most common) |
|
b. vestibule | true (Posterior SCC is usually entered by drilling—via the oral window.) |
|
c. perilabyrinthine cells | true (and tracks to mastoid antrum) |
|
d. mastoid air cells | true (at craniotomy site) |
|
99. True or False. The following is the most likely source of a postoperative CSF fistula after resection of a vestibular schwannoma: |
| G7 p.631:20mm |
a. mastoid air cells via craniotomy site | false |
|
b. through the vestibule of the bony labyrinth via the oval window | false |
|
c. perilabyrinthine cells to the mastoid antrum | false |
|
d. apical cells to the tympanic cavity or eustachian tube | true (All are potential routes but this is the most frequent.) |
|
100. With vestibular schwannoma, postoperative routes for rhinorrhea are |
| G7 p.631:20mm |
Hint: avam |
| |
a. a_____ | apical cells to tympanic cavity and down the eustachian tube |
|
b. v_____ | vestibule after drilling the ICA into the semicircular canal via oval window |
|
c. a_____ | to antrum of mastoid via the perilabyrinthine cells |
|
d. m_____ | mastoid air cells at site of craniotomy |
|
101. What are treatment strategies for CSF leakage after vestibular schwannoma resection? |
| G7 p.631:92mm |
a. What percent stop spontaneously? | 25 to 35% |
|
b. Do what with the head of the bed? | elevate |
|
c. Place a drain where? | lumbar |
|
d. If hydrocephalus is present place a_____. | CSF shunt |
|
e. If leak persists_____. | reexplore surgical site to pack with tissue or apply bone wax |
|
102. What are common complications of vestibular schwannoma surgery? |
| G7 p.631:175mm |
a. CSF leak in_____% | 4 to 27% |
|
b. infection in_____% | 5.7% meningitis |
|
c. stroke in_____% | 0.7% cerebrovascular accident (CVA) |
|
d. CN VII palsy in_____% | 0 to 50% |
|
e. hearing loss in_____% | 34 to 43% |
|
f. death in_____% | 1% |
|
103. Complete the following concerning hearing loss and CN VII weakness after suboccipital removal of VS: |
| G7 p.632:25mm |
a. Tumor < 1 cm |
|
|
i. CN VII preserved,_____% | 95 to 100% |
|
ii. CN VIII preserved,_____% | 57% |
|
b. Tumor 1 to 2 cm |
|
|
i. CN VII preserved,_____% | 80 to 92% |
|
ii. CN VIII preserved,_____% | 33% |
|
c. Tumor > 2 cm |
|
|
i. CN VII preserved,_____% | 50 to 76% |
|
ii. CN VIII preserved,_____% | 6% |
|
104. Complete the following concerning hearing loss after suboccipital removal of VS: |
| G7 p.632:25mm |
a. Hearing preserved_____% with tumors < 1.5 cm | 14 to 48% |
|
b. After SRS hearing preserved_____% with tumors < 3 cm | 26% |
|
105. Concerning acoustic neuroma (i.e., vestibular schwannoma), recurrence following microsurgery is |
| G7 p.633:18mm |
a. _____% after | 10 |
|
b. _____ years follow-up. | 15 |
|
106. Complete the following concerning SRS for vestibular schwannoma: |
| G7 p.633:47mm |
a. Dose recommended is_____. | 14 Gy |
|
b. Local control achieved is_____%. | 94% |
|
107. For vestibular schwannoma, what are local control rates for? |
| G7 p.633:60mm |
a. microsurgery | 97% |
|
b. SRS | 94% |
|
108. When is the time of maximal damage (possible tumor enlargement) from radiation to vestibular schwannomas? |
| G7 p.633:75mm |
a. from_____ to_____ months | 6 to 18 |
|
b. This is important to know because it can produce a false appearance of tumor_____. | enlargement (Surgery should be avoided during the interval of 6 to 18 months after SRS because of damage from radiation and the appearance of tumor enlargement.) | |
109. Most pituitary tumors are benign tumors that arise from the_____ | adenohypophysis | G7 p.634:25mm |
110. Answer the following about pituitary tumors: |
| G7 p.634:37mm |
a. By definition what is the maximal size of a pituitary microadenoma? | 1 cm |
|
b. Larger tumors are called_____ | macroadenomas |
|
c. 50% of pituitary tumors are less than_____ mm. | 5 mm |
|
111. Complete the following about pituitary carcinoma: |
| G7 p.634:48mm |
a. Occurence is_____. | rare |
|
b. They are usually i_____ | invasive |
|
c. They are usually s_____ | secretory |
|
d. The most common hormones are |
|
|
i. a_____ | adrenocorticotropic hormone (ACTH) |
|
ii. P_____ | PRL |
|
e. True or false. They can metastasize. | true |
|
f. Prognosis of 1-year mortality is_____%. | 66% |
|
112. True or False. Regarding pituitary tumors: |
| G7 p.634:67mm |
a. 10% of intracranial tumors | true |
|
b. most common in third to fourth decades | true |
|
c. affect females more often | false (Pituitary tumors affect both sexes equally.) |
|
d. higher incidence in MEN or MEA syndrome | true |
|
e. usually present due to endocrine disturbance or mass effect | true |
|
113. Complete the following about pituitary tumors: |
| G7 p.634:70mm |
a. MEN stands for_____ _____ | multiple endocrine neoplasms |
|
b. MEA stands for_____ _____ | multiple endocrine adenomatosis |
|
c. Incidence of pituitary tumors in MEN is_____. | increased |
|
114. Complete the following about clinical presentation of pituitary tumors: |
| G7 p.634:125mm |
a. Hormone hypersecretion |
|
|
i. _____% of adenomas secrete active hormone | 65% |
|
ii. prolactin_____% | 48% |
|
iii. growth hormone_____% | 10% |
|
iv. ACTH_____% | 6% |
|
v. thyroid-stimulating hormone (TSH)_____% | 1% | |
b. Growth hormone |
|
|
i. If elevated it is due to a_____ _____ | pituitary adenoma |
|
ii. More than_____% of the time. | 95% |
|
c. Corticotropin |
|
|
i. aka_____ | ACTH |
|
ii. Excess causes_____ _____ | Cushing disease |
|
iii. Nelson syndrome can develop only in patients who have had an _____ | adrenalectomy |
|
115. Complete the following about hormone hyposecretion: |
| G7 p.634:180mm |
a. Due to_____ of the normal pituitary | compression |
|
b. In order of sensitivity to compression |
|
|
Hint: go look for the adenoma |
|
|
i. G_____ | GH |
|
ii. L_____ | LH |
|
iii. F_____ | FSH |
|
iv. T_____ | TSH |
|
v. A_____ | ACTH |
|
c. Most common symptom |
| G7 p.635:52mm |
i. o_____ h_____ | orthostatic hypotension |
|
ii. e_____ f_____ | easy fatigability |
|
d. selective loss of one hormone consider_____ | hypophysitis |
|
i. A_____ | ACTH |
|
ii. A_____ | ADH |
|
e. True or False. Diabetes insipidus is seen with preop pituitary tumors. | false |
|
116. Complete the following about mass effect: |
| G7 p.635:95mm |
a. The pituitary tumor that gains the greatest size is |
|
|
i. non-secreting. (True or False) | true |
|
ii. of the secreting type is the_____ | prolactinoma |
|
b. The tumor that is usually the smallest is the_____ tumor. | ACTH |
|
117. Patient presents with sudden onset of headache, visual disturbance, ophthalmoplegia, and reduced mental status. |
| G7 p.635:155mm |
a. Consider diagnosis of p_____ a_____. | pituitary apoplexy (due to expanding mass in sella turcica resulting from hemorrhage or necrosis) |
|
b. This may occur in macroadenomas in as many as_____%. | 3 to 17% | |
118. Complete the following about primary brain tumors: |
| G7 p.636:150mm |
a. What are the indications for rapid decompression after pituitary apoplexy? |
|
|
i. s_____ c_____ | sudden constriction of visual field (VF) |
|
ii. s_____ | severe deterioration of acuity |
|
iii. mental status changes due to h_____ | hydrocephalus (complete tumor removal usually not necessary) |
|
b. What else needs to be done? | treat with corticosteroids |
|
119. Complete the following about the anatomic classification of pituitary adenoma: |
| G7 p.637:15mm |
a. Named the_____ system | Hardy |
|
b. Suprasellar extension |
|
|
i. O | none |
|
ii. A expanding into the_____ cistern | suprasellar |
|
iii. B anterior recesses of third ventricle_____ | obliterated |
|
iv. C_____ of third ventricle_____ | floor; displaced |
|
c. Floor of sella |
|
|
i. Intact or_____ _____ | focally expanded enlarged |
|
ii. Sella_____ | enlarged |
|
d. Sphenoid extension |
|
|
i. Localized_____ of sella floor | perforation |
|
ii. Diffuse_____ of sella floor | destruction |
|
120. Complete the following about functional pituitary tumors: |
| G7 p.637:135mm |
a. What is the most common functional pituitary tumor? | prolactinoma |
|
b. What are its most common symptoms? |
|
|
i. In females,_____-_____ | amenorrhea-galactorrhea |
|
ii. called the syndrome of_____-_____ | Forbes-Albright |
|
iii. causes_____ in males | impotency |
|
c. It arises from anterior pituitary l_____. | lactotrophs |
|
d. The most common cause of amenorrhea is p_____. | pregnancy |
|
121. Answer the following about Cushing syndrome: |
| G7 p.638:25mm |
a. Which hormone? | ACTH |
|
b. It is produced by a_____ tumor. | pituitary |
|
c. It is called Cushing_____. | disease (if tumor is in the pituitary hypercorticalism, it is called Cushing disease) | |
122. Complete the following about pituitary adenoma: |
| G7 p.638:25mm |
a. Adrenocorticotropic hormone (ACTH)— secreting pituitary adenoma is known as_____ _____. | Cushing disease |
|
b. Other causes of hypercortisolism are known as_____ _____ | Cushing syndrome |
|
c. Nelson disease manifests by |
|
|
i. hyper-_____ due to | hyperpigmentation | G7 p.639:30mm |
ii. cross reactivity of m_____ s_____ h_____ with_____.- | melanocyte-stimulating hormone (MSH) with ACTH |
|
123. Complete the following about Nelson syndrome: |
| G7 p.639:30mm |
a. Follows bilateral_____ | adrenalectomy |
|
b. In only_____ to_____% of cases | 10 to 30% |
|
c. Classic triad of |
|
|
i. h_____ | hyperpigmentation |
|
ii. ↑ in_____ | ACTH |
|
iii. Enlargement of the_____ | pituitary tumor |
|
iv. Usually occurs_____ to_____ years after adrenalectomy | 1 to 40 years |
|
d. |
| G7 p.639:90mm |
i. The earliest sign is the_____ _____ | linea negra |
|
ii. Midline pigmentation from the pubis to_____ | umbilicus |
|
iii. And hyperpigmentation of_____ _____ and areolae | scars, gingivae |
|
e. Have an ACTH level greater than_____ Ng/L | 200 | G7 p.639:130mm |
f. The normal being less than_____ Ng/l | 54 |
|
124. Complete the following about pituitary adenoma (Cushing syndrome): |
| G7 p.638:25mm |
a. caused by_____ | hypercortisolism—from any source |
|
b. exogenous source_____ | ingestion of steroids |
|
c. endogenous sources |
|
|
i. p_____ t_____, _____% | pituitary tumor, 60 to 80% |
|
ii. a_____ t_____, _____% | adrenal tumor, 10 to 20%, 15 to 25% |
|
iii. e_____ t_____, _____% | ectopic tumor, 1 to 10%, 5 to 10% |
|
125. Characterize the typical Nelson syndrome scenario. |
| G7 p.639:53mm |
a. patient who had_____ _____ | Cushing syndrome |
|
b. had a surgical procedure_____ | adrenalectomy |
|
c. develops_____ | hyperpigmentation |
|
d. occurs in_____% of such patients | 10 to 30% |
|
e. due to_____-_____of_____ and_____ | cross-reactivity of ACTH and MSH | |
126. To remember Cushing syndrome versus disease: |
| G7 p.638:36mm |
a. syndrome due to_____ | steroids from any source Hint: syndrome = steroids |
|
b. disease due to_____ | pituitary only |
|
127. List the findings in Cushing syndrome. |
| G7 p.638:115mm |
Hint: steroids |
|
|
a. s_____ | striae |
|
b. t_____ | thin skin |
|
c. e_____ | ecchymosis |
|
d. r_____ | reduced libido |
|
e. o_____ | obesity |
|
f. i_____ | impotence, increased blood pressure |
|
g. d_____ | diabetes |
|
h. s_____ | skin hyperpigmentation |
|
128. List the findings in Cushing syndrome. |
| G7 p.639:15mm |
Hint: Ectopic sources of acth secretions |
|
|
Hint: (a) c3 t2 h |
|
|
a. (a) |
|
|
b. c_____ | carcinoma small cell lung |
|
c. c_____ | carcinoid |
|
d. c_____ | (pheo) chromocytoma |
|
e. t_____ | thymoma |
|
f. t_____ | thyroid carcinoma |
|
g. h_____ | islet cell pancreas |
|
129. Characterize pituitary adenoma in Cushing disease. |
| G7 p.638:36mm |
a. secretion of_____ | ACTH |
|
b. most are small <_____ mm | 5 mm |
|
c. only_____% are large enough to produce mass effect | 10% |
|
d. cells produce_____ | proopiomelanocortin (POMC) |
|
e. which contains the precursors for: |
|
|
i. A_____ | ACTH |
|
ii. a_____ | alpha-MSH |
|
iii. b_____ | beta-lipotropin |
|
iv. b_____ | beta-endorphin |
|
v. e_____ | met-enkephalin |
|
130. Criteria for biochemical cure is IGF-1 level less than_____ Ng/mL. | 5 | |
131. Chart. List the effects of excess growth hormone alphabetically. |
| G7 p.640:50mm |
| arthropathy |
|
| acromegaly |
|
| bone |
|
| cartilage |
|
| cardiomyopathy |
|
| diabetes |
|
| entrapment of nerve |
|
| syndromes |
|
| frontal bossing |
|
| fatigue |
|
| glucose intolerance |
|
| gigantism |
|
| hyperhydrosis |
|
| hypertension |
|
| headaches |
|
| infection |
|
| increased hand and foot size |
|
| joint pain |
|
| macroglossia |
|
| malignancies |
|
| neoplasia |
|
| neuropathy |
|
| oily skin |
|
| polyps |
|
| paresthesias |
|
| prognathism |
|
| palmar hyperhydrosis |
|
| respiratory obstruction |
|
| rings no longer fit |
|
| shoe size enlarges |
|
| sleep apnea |
|
| skeletal changes |
|
| soft tissue swelling |
|
| thickened heel pad |
|
| thyromegaly with normal |
|
| thyroid studies |
|
132. Describe the hypothalamic pituitary axis dysfunction in acromegaly. |
| G6 p.441:55mm |
a. Hypothalamus produces_____. | GHRH |
|
b. _____ causes the pituitary to make_____. | GHRH; GH |
|
c. _____ affects the liver, which produces_____ also known as_____. | GH, somatomedin-C, IGF— 1 (hypothalamic GHRH stimulates pituitary GH secretion. Excess GH induces IGF-1 secretion from liver.) |
|
d. What medication can suppress GH release? | somatostatin (Acromegaly findings are due to IGF-1, also known as somatomedin-C.) | |
133. Complete the following about acromegaly growth hormone releasing hormone (GHRH): |
| G6 p.441:56mm |
a. produced in the_____ | hypothalamus |
|
b. causes |
|
|
ii. sy_____ | synthesis of growth hormone |
|
ii. se_____ | secretion |
|
iii. re_____ | release |
|
c. somatomedin-C |
|
|
i. produced in the_____ | liver |
|
ii. due to stimulus of_____ | GH |
|
iii. produces_____ _____ | systemic effects |
|
iv. also known as_____ _____ _____ | insulin-like growth factor (IGF- 1, also known as somatomedin-C) |
|
134. True or False. Regarding acromegaly, somatostatin suppresses growth hormone by interfering with |
| G6 p.441:60mm |
a. synthesis | false |
|
b. secretion | false |
|
c. release of the hormone | true |
|
135. Answer the following about acromegaly: |
| G7 p.640:18mm |
a. Is there any possible ectopic source of growth hormone? | yes |
|
b. If so, what? | carcinoid tumor |
|
136. Answer the following about acromegaly: |
| G7 p.640:135mm |
a. What effect on mortality does elevated GH levels have? Moratality rates are_____ to_____ times normal | 2 to 3 times |
|
b. due to |
|
|
i. c_____ | cancer |
|
ii. c_____ | cardiomyopathy |
|
iii. d_____ | diabetes |
|
iv. h_____ | hypertension |
|
v. i_____ | infection |
|
vi. n_____ _____ | neural entrapment |
|
137. Concerning growth hormone, what effects does GH have on the following? |
| G7 p.640:136mm |
a. mortality rates | ↑ |
|
b. blood pressure | ↑ |
|
c. diabetes | ↑ |
|
d. infections | ↑ |
|
e. cancer | ↑ |
|
f. cardiomyopathy | ↑ |
|
g. closure of epiphyseal plates in children | delays closure |
|
138. Which pituitary tumor is |
| G7 p.638:90mm |
a. least likely to cause mass effect? | ACTH-producing tumor |
|
b. most likely to cause mass effect? | prolactin-producing tumor | |
139. Describe the mass effects of pituitary tumors. |
| G7 p.637:80 mm |
a. What are the structures compressed? |
|
|
Hint: cop |
|
|
i. c_____ s_____ | cavernous sinus |
|
ii. o_____ c_____ | optic chiasm |
|
iii. p_____ | pituitary |
|
b. What are the mass effects usually seen in nonfunctioning pituitary tumors? |
|
|
i. p_____, f_____ p_____, d_____ | ptosis, facial pain, diplopia |
|
ii. b_____ h_____ | bitemporal hemianopsia |
|
iii. h_____ | hypopituitarism |
|
140. Describe the Hardy system of pituitary adenoma classification. |
| G7 p.637:14mm |
a. suprasellar extension of tumor |
|
|
i. _____ | no suprasellar extension |
|
ii. _____ | fills suprasellar cistern |
|
iii. _____ | anterior recess of III ventricle |
|
iv. _____ | displaces floor of III ventricle |
|
v. _____ | intracranial (intradural) |
|
vi. _____ | intracavernous sinus (extradural) |
|
b. invasion |
|
|
i. I s_____ n_____ | sella normal |
|
ii. II s_____ e_____ | sella enlarged |
|
iii. III l_____p_____ of s_____ f_____ | localized perforation of sella floor |
|
iv. IV d_____ d_____ of s_____ f_____ | diffuse destruction of sella floor |
|
v. V s_____via C_____ | spread via CSF |
|
141. What percentage of pituitary adenomas become locally invasive? | 5% | G7 p.637:15mm |
142. Cavernous sinus invasion |
| G7 p.637:60mm |
a. can be suspected if medial wall of sinus is_____ _____. | pushed laterally |
|
b. can be diagnosed if carotid artery is_____. | encased |
|
143. What is the most definite sign of cavernous sinus invasion? | carotid artery encasement | G7 p.637:70mm |
144. Matching. Match the light microscopic appearance of each of the following pituitary tumors with its most common secretory product. |
| G7 p.641:60mm |
Secretory product: |
|
|
|
|
|
Appearance: |
|
|
a. chromophobe |
|
|
b. acidophil |
|
|
c. basophil |
| |
145. What percentage of pituitary tumors are |
| G7 p.641:30mm |
a. endocrine-secretorily active? | 70% |
|
b. endocrine-secretorily inactive? | 30% |
|
146. Complete the following about tumors of the neurohypophysis and infundibulum: |
| G7 p.641:105mm |
a. Most common tumor in the posterior pituitary is_____. | metastasis |
|
b. Most common primary tumor is the_____ _____ _____ | granular cell tumor (GCT) |
|
c. If this tumor is suspected, operative approach is_____. | transcranial |
|
d. MRI appearance is identical to_____ | adenoma |
|
147. True or False. Baseline endocrinologic evaluation of patients presenting with pituitary tumors includes the following among others: |
| G7 p.642:80mm |
a. 8 a.m. cortisol (24 hours is better) | true |
|
b. serum prolactin level | true |
|
c. somatomedin-C | true |
|
d. serum thyroid-stimulating hormone (TSH) | true |
|
e. serum T3 | false |
|
148. List the baseline pituitary function tests. |
| G7 p.642:81mm |
Hint: pqrsTT |
|
|
a. p_____ | prolactin serum level |
|
b. q_____ | Q-cortisol 24 hour |
|
c. r_____ | rest FSH LH FBS (rest means the rest of the endocrine studies) (reproductive) |
|
d. s_____ | somatomedin C |
|
e. T_____ | TSH serum level |
|
f. T_____ | T4 serum level |
|
149. What is the chiasm location in relationship to the sella and the resulting visual field defect? |
| G7 p.642:80mm |
a. prefixed_____% | 5%, homonymous hemianopsia |
|
b. above_____% | 80%, bitemporal hemianopsia |
|
c. postfixed_____% | 5%, ipsilateral loss of vision, junctional scotoma contralaterally, so-called “pie in the sky,” due to compression of the anterior knee of Willebrand | |
150. Visual fields is tested using a small red stimulus because desaturation of color is an early sign of _____ compression. | chiasmal | G7 p.642:170mm |
151. Answer the following about pituitary adenoma: |
| G7 p.643:24mm |
a. What is the classic finding when a tumor compresses the optic chiasm? | bitemporal hemianopsia |
|
b. What occurs in patients with a postfixed chiasm? |
|
|
i. s_____ o_____ q_____ | superior outer (temporal) quadrantanopsia |
|
ii. j_____ s_____ | junctional scotoma |
|
c. due to compression of the k_____ of v_____ W_____ | knee of von Willebrand |
|
d. What occurs in patients with a prefixed chiasm? | homonymous hemianopsia (complete or incomplete) |
|
e. due to compression of _____ or _____ optic tracts | one or both |
|
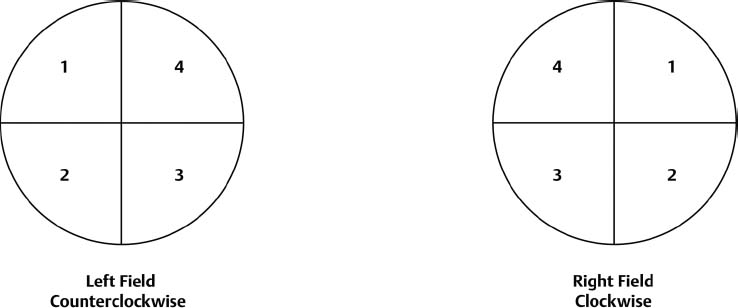
152. Characterize the pattern of progressive visual field defect caused by pituitary tumor. |
| G7 p.643:24mm |
| ||
Fig. 21.1 |
|
|
a. first | superior temporal field |
|
b. second | inferior temporal field |
|
c. third | inferior nasal field |
|
d. fourth | superior nasal field |
|
e. clockwise in the ________ field | right |
|
f. counterclockwise in the ________ field | left | |
153. Describe baseline pituitary evaluation before surgery. (*Note: Results not listed here are also not listed in the Greenberg 6th edition because results vary with age, gender, and menstrual cycle.) |
| G7 p643:70mm |
a. Hint: P8R3st2 |
|
|
i. p_____ | prolactin |
|
normal | < 30 |
|
measured in | ng/mL |
|
maybe abnormal | 25 to 150 |
|
abnormal value | > 150 |
|
ii. (sounds like q) c_____ | cortisol 8 a.m. |
|
normal | 6 to 18 |
|
measured in | μg/100 mL |
|
maybe abnormal | 5 to 10 |
|
abnormal value | > 10 |
|
iii. *(r rest) f_____-s_____ _____ | follicle-stimulating hormone (FSH) |
|
normal |
|
|
measured in |
|
|
maybe abnormal |
|
|
abnormal |
|
|
iv. *(r rest) l_____ | luteinizing hormone |
|
normal |
|
|
measured in |
|
|
maybe abnormal |
|
|
abnormal |
|
|
v. (r rest) f_____ b_____s_____ | fasting blood sugar |
|
normal | 65 to 99 |
|
measured in | mg/dL |
|
maybe abnormal |
|
|
abnormal |
|
|
vi. *s_____ | somatomedin-C |
|
normal | 0.31 to 1.4 |
|
measured in | U/mL |
|
maybe abnormal |
|
|
abnormal |
|
|
vii. *T_____ | TSH | G7 p.445:15mm |
normal | 0.4 to 5.5 mg |
|
measured in | μg |
|
maybe abnormal | peak 2× normal |
|
abnormal | if TSH stimulation test causes peak 2× normal |
|
viii. *T_____ | TH thyroid hormone |
|
normal | 0.8 to 15 |
|
measured in | free T4 index |
|
maybe abnormal |
|
|
abnormal |
| |
b. Also include diagnostic studies of |
|
|
i. f_____ v_____ f_____ | formal visual fields |
|
ii. M_____ w_____ and w_____ e_____ | MRI with and without enhancement |
|
iii. C_____-c_____ v_____ | CT-coronal views (11 tests in all) |
|
154. Thickening of the pituitary stalk and loss of a single pituitary hormone is strongly suggestive of l_____h_____. | lymphocytic hypophysitis | G7 p.643:83mm also see G7 p.1217:55mm |
155. True or False. Regarding lymphocytic hypophysitis: |
| G7 p.643:83mm also see G7 p.1217:55mm |
a. more common in men than women | false (more common in women; only 5 cases reported in men) |
|
b. associated with postpartum state | true |
|
c. affects multiple pituitary hormones | false (affects single hormone) |
|
d. rarely causes diabetes insipidus | false (often causes diabetes insipidus) |
|
156. Characterize screening for Cushing syndrome. |
| G7 p.643:92mm |
a. 8 a.m. cortisol level: normal value is _____ | 6 to 18 μg/100 mL |
|
b. 24-hour urine-free cortisol _____ | more accurate—almost 100% sensitive and specific |
|
157. True or False. Findings of primary hypothyroidism with secondary pituitary hyperplasia include the following: |
| G7 p.645:45mm |
a. prolonged and elevated TSH response to TRH stimulation | true |
|
b. low T4 | true |
|
c. hypoglycemia | false (Hypoglycemia is not part of the syndrome.) |
|
d. elevated TSH | true |
|
e. elevated prolactin | true (Enlarged pituitary causes stalk effect and prolactin increases.) |
|
f. pituitary enlarges because of hypertrophy of the _____ producing cells | thyrotropin releasing hormone (TRH) |
|
g. pituitary enlargement occurs because of the loss of _____ _____ from _____ _____ | negative feedback from thyroid hormones | |
158. Considering pituitary tumors, prolactin is under: |
| G7 p.644:35mm |
a. inhibitory control of the _____ and the infundibular stalk. | hypothalamus |
|
b. Therefore, injury to the hypothalamus or injury to the pituitary stalk causes loss of the inhibitory chemical _____. | prolactin inhibitory factor (PRIF) |
|
c. Does this lead to an increase or decrease in prolactin in the patient? | increase |
|
159. After surgery for prolactin-secreting tumor, what should you think if prolactin is still elevated |
| G7 p.644:33mm |
a. but less than 90 ng/mL _____? | injury to stalk and/or hypothalamus due to loss of prolactin inhibitory factor (PRIF), which is present in the intact stalk and hypothalamus |
|
b. but more than 150 ng/mL _____? | persistent tumor |
|
160. Answer the following about large adenomas with normal prolactin: |
| G7 p.644:160 mm |
a. What should you instruct the laboratory to do? | perform several dilutions and rerun the PRL (This may be a false negative.) |
|
b. This false negative is called the _____ effect. | hook |
|
161. True or False. Extremely high prolactin levels may produce false negatives due to the tendency for large numbers of PRL molecules to prevent formation of PRL-antibody-signal complexes in assays. | true (hook effect) | G7 p.644:160mm |
162. Complete the following about cortisol reserve insulin tolerance test: |
| G7 p.647:115mm |
a. Insulin IV will promptly lower _____ _____. | blood sugar |
|
b. Hypoglycemia is a _____. | stressor |
|
c. In response the body produces _____. | cortisol |
|
d. |
|
|
i. An increment in baseline more than _____ mg/dL | 6 |
|
ii. to a peak of _____ mg/dL is normal. | 20 |
|
e. |
|
|
i. An increment of less than _____ mg/dL | 6 |
|
ii. to a peak less than _____ mg/dL | 16 |
|
iii. indicates a need for g_____ r_____. | glucocorticoid replacement |
|
163. The most useful test for acromegaly is an _____ level. | IGF-1 | |
164. Complete the following about acromegaly and somatomedin-C: |
| G7 p.647:170mm |
a. also known as _____ | IGF-1 |
|
b. normal fasting level _____ | 0.67 U/mL (range 0.31 to 1.4 U/mL) |
|
c. in acromegalics level is _____ | 6.8 U/mL (range 2.6 to 21.7 U/mL) |
|
165. Some growth hormone-secreting pituitary tumors also secrete _____ | prolactin | G7 p.653:20mm also G6 p.447:115mm |
166. Complete the following about growth hormone: |
| G7 p.648:15mm |
a. Normal basal fasting level is _____. | less than 5 ng/mL |
|
b. Acromegalic patients have levels _____ than _____. | greater than 10 ng/mL |
|
c. Due to pulsatile secretion of GH sporadic peaks up to _____ can occur. | 50 ng/mL |
|
d. Is this a reliable test? | no |
|
167. Complete the following about the size of the pituitary gland: |
| G7 p.648:115mm |
a. Size of pituitary gland |
|
|
i. in men up to _____ mm | 10 |
|
ii. in women up to _____ mm child-bearing age up to_____ mm | 9, 11 |
|
iii. in adolescent girls up to _____ mm | 15 |
|
b. size of stalk is same size as b_____ | basilar artery |
|
c. differential diagnosis of large stalk |
|
|
i. l _____ | lymphoma |
|
ii. l_____ h_____ | lymphocytic hypophysitis |
|
iii. g_____ d_____ | granulomatous disease |
|
iv. h_____ g_____ | hypothalamic glioma |
|
168. Findings compatible with pituitary microadenoma on MRI include the following: |
| G7 p.648:145mm |
a. True or False. Lack of early (< 5 minute) gadolinium enhancement | true |
|
b. True or False. Pituitary stalk deviation | true |
|
c. True or False. Thickened pituitary stalk | false (A thickened pituitary stalk is not compatible with adenoma.) |
|
d. True or False. Late (after 30 minute) gadolinium enhancement | true |
|
e. True or False. Timing of scan after gadolinium infusion is important. | true (In early scanning, under 5 minutes, tumor will not enhance but gland will. In late scanning, after 30 minutes, tumor will enhance as well and may not be seen because the gland is also enhanced.) | |
f. The best time to scan for pituitary tumor is _____ minutes after infusion. | 5 |
|
g. At that time what enhances? | normal pituitary tissue |
|
h. Microadenoma is seen since it does _____ _____. | not enhance |
|
169. Characterize the neurohypophysis. |
| G7 p.648:160 mm |
a. normally on T1WI is _____ _____ | high signal |
|
b. possibly because it contains _____ | phospholipids |
|
c. absence of this sign suggests _____ _____ | diabetes insipidus |
|
170. For pituitary tumors, what is the benefit of coronal CT slices? |
| G7 p.649:42mm |
a. sphenoid series _____ | midline (can be identified by the anatomy of sphenoid sinus septa) |
|
b. sella floor _____ | erosion (of the sella floor to indicate presence of the tumor on one side) |
|
171. What is the medical treatment for the following? a. growth hormone-secreting tumors _____ | octreotide | G7 p.653:45mm |
b. ACTH-secreting tumors _____ | ketoconazole | G7 p.654:148mm |
c. prolactin-secreting tumors _____ | bromocriptine | G7 p.651:60mm |
172. Complete the following about nonsecreting pituitary adenomas: |
| G7 p.649:100mm |
a. Usual treatment is with _____ or _____ | S× or XRT |
|
b. |
|
|
i. Medication (bromocriptine) may reduce tumor size by _____% | 20% |
|
ii. Due to the paucity of _____ receptors | dopaminergic |
|
c. Octreotide reduces the tumor by _____% | 10% |
|
d. Follow-up by MRI at: _____, _____, _____, and _____ years | 0.5, 1, 2, and 5 |
|
173. Surgical indications are v_____ f_____ d_____. | visual field defects | G7 p.649:165mm |
174. Tumors secreting GH or ACTH |
| G7 p.650:70mm |
a. warrant _____ treatment | surgical |
|
b. because the secretion is _____ | harmful |
|
c. and there is no effective _____ _____. | medical treatment |
|
175. Complete the following about hormone replacement therapy: |
| G7 p.650:125mm |
a. corticosteroids |
|
|
i. am replacement dose is _____ mg and | 20 |
|
ii. pm replacement dose is _____ mg | 10 | |
b. thyroid hormone |
|
|
i. Do not replace if patient has _____ _____ | adrenal insufficiency |
|
ii. Synthroid _____ μ g/d | 125 |
|
176. Complete the following about primary brain tumors: |
| G7 p.651:24mm |
a. Above what level of prolactin is surgery unlikely to normalize the prolactin? | above 500 ng/mL |
|
b. In such a case what should your treatment be? | medication—dopamine agonists bromocriptine—not surgery |
|
177. Complete the following about prolactinoma as treatment with bromocriptine: |
| G7 p.651:40mm |
a. Response should be evident in _____ to _____ weeks. | 4 to 6 |
|
b. _____% will not respond. | 18% |
|
c. _____% will continue to enlarge on bromocriptine. | 1% |
|
d. Upon discontinuation tumor may _____ _____. | rapidly enlarge |
|
178. What does bromocriptine do? |
| G7 p.651:80 mm |
a. binds to r_____ | receptors |
|
b. inhibits s_____ and s_____ of _____ | synthesis and secretion of PRL |
|
c. lowers prolactin to about _____% of its elevated amount | ˜10% |
|
d. reduces tumor size by _____% in _____ | 75% in 6 to 8 weeks |
|
e. restores _____ | fertility |
|
f. harms patient by _____ | producing fibrosis |
|
g. This reduces good surgical results by _____%. | 50% |
|
h. Therefore, decide about surgery within _____ _____ of starting bromocriptine. | 6 months |
|
i. Prolactinomas may _____ _____ upon discontinuation of the drug. | enlarge rapidly |
|
179. If response to dopamine agonists is satisfactory |
| G7 p.652:90mm |
a. continue to treat for _____ to _____ years and | 1 to 4 |
|
b. check prolactin every _____. | year |
|
c. If tumor not visible on MRI may _____. | discontinue |
|
d. Recurrence rate is highest in the _____ _____. | first year |
|
180. True or False. Surgery is not indicated in elderly asymptomatic patients with GH-secreting pituitary tumors. | true | |
181. Answer the following about pituitary tumors: |
| G7 p.652:130mm |
a. best treatment for prolactinoma PRL < 500 | transsphenoidal surgery |
|
b. best treatment for prolactinoma PRL > | 500 surgery not recommended if PRL > 500 |
|
c. best treatment if prolactin is < 500 try _____ first | medical treatment |
|
d. meds will fail in _____% | 18% |
|
e. treat the failures with _____ | transsphenoidal surgery |
|
f. acromegaly best treatment is _____ | transsphenoidal surgery (Surgery is not recommended for elderly; instead use bromocriptine and/or octreotide.) |
|
g. cure for microadenoma _____% | 85% |
|
h. cure for macroadenoma _____% | 30% |
|
i. Cushing disease best treatment is _____. | transsphenoidal surgery |
|
182. In acromegaly, IGF-1 stabilizes after surgery in _____. | months | G7 p.652:185mm |
183. Complete the following about acromegaly and octreotide: |
| G7 p.652:98mm |
a. suppresses _____ _____ | growth hormone |
|
b. reduces _____, _____% to _____% become _____ | GH in 71%, 50 to 66% become normal |
|
c. reduces _____ in _____%, _____% become _____ | GF-1 in 93%, 66% become normal |
|
d. requires injection _____ | 3 times per day |
|
e. side effects can be _____ | cholelithiasis (10 to 25% of patients) |
|
f. may also be useful in _____ | thyrotropic (TSH)-secreting tumors |
|
184. True or False. Common side effects of octreotide include the following: |
| G7 p.653:120mm |
a. decreased GI motility | true |
|
b. sweating | false |
|
c. diarrhea | true |
|
d. steatorrhea | true |
|
e. bradycardia | true |
|
f. cholelithiasis | true |
|
185. Complete the following about Cushing disease and ketoconazole: |
| G7 p.654:148mm |
a. blocks _____ _____ synthesis | adrenal steroid |
|
b. normalizes _____% of patients | 75% |
|
c. normalizes _____ _____ cortisol | urinary free |
|
d. normalizes _____ steroids | hydroxycortico |
|
e. may cause |
|
|
i. adrenal _____ | insufficiency |
|
ii. hepato-_____ | hepatotoxicity | |
186. True or False. Regarding bilateral total adrenalectomy: |
| G7 p.654:90mm |
a. It is better tolerated than transsphenoidal pituitary surgery. | false |
|
b. Lifelong glucocorticoid replacement is required. | true |
|
c. Lifelong mineralocorticoid replacement is not required. | false | G7 p.654:94mm |
d. Development of Nelson syndrome is rare. | false (Not rare; it occurs in 30%.) |
|
187. Complete the following about thyrotropin-secreting adenomas: |
| G7 p.655:85mm |
a. First-line treatment is _____ _____. | transsphenoidal surgery |
|
b. The tumor may be difficult to remove and _____. | fibrous |
|
c. |
|
|
i. Medical treatment is with the same agent as for _____ | acromegaly |
|
ii. namely, _____. | octreotide |
|
188. Complete the following about pituitary tumors and radiation therapy side effects on: |
| G7 p.655:147mm |
a. cognition |
|
|
i. m_____ d_____ | memory disturbances |
|
ii. l_____ | lethargy |
|
b. vision |
|
|
i. o_____ n_____ and c_____ i_____ | optic nerve and chiasm injury |
|
ii. b_____ | blindness |
|
c. endocrine |
|
|
i. h_____ | hypocorticalism |
|
ii. h_____ | hypothyroidism |
|
d. tumor |
|
|
i. n_____ | necrosis |
|
ii. a_____ | apoplexy |
|
189. Radiation therapy should be routinely used: |
| G7 p.655:160mm |
a. True or False. Following surgical removal of pituitary adenomas | false |
|
b. True or False. If recurrence occurs | false (Repeat surgery is recommended.) |
|
c. Radiation is appropriate in the following circumstances |
| |
i. if recurrence _____ _____ _____ | can’t be removed |
|
ii. if recurrence _____ _____ _____ _____ | mass continues to grow | |
190. Answer the following about radiation for acromegaly: |
| G7 p.656:35mm |
a. True or False. It is the preferred treatment. | false |
|
b. 90% of patients reach normal growth hormone levels in _____ years. | 20 |
|
c. During this time they are exposed to _____ levels of GH | unacceptable |
|
d. and are also exposed to the risks of _____. | radiation |
|
191. True or False. Indications for pituitary surgery include |
| G7 p.649:164mm also G6 p.452:140mm |
a. prolactinomas with levels greater than 500 ng/mL not controlled with surgery | true (Medical treatment will not suffice; both are needed in 18%.) |
|
b. Cushing disease | true (Medical therapy is not adequate.) |
|
c. acromegaly | true |
|
d. macroadenoma | true (if not PRL secreting) |
|
e. visual field defect | true |
|
f. sudden visual loss | true |
|
g. to obtain tissue for diagnosis | true |
|
h. hypopituitarism | false |
|
i. Nelson syndrome | true |
|
192. What is the medical preparation for surgery? |
| G7 p656:90mm |
a. Steroids _____ _____ | stress doses |
|
b. Hypothyroid patients ideally to be treated before surgery for _____ _____ | 4 weeks |
|
193. Regarding pituitary tumors, what artery might you encounter laterally as you open the Hardy speculum and expose the keel of the sphenoid bone? | the sphenopalatine artery—a branch of the maxillary artery, which is the eighth branch of the external carotid artery | G7 p. 656:117mm |
194. Concerning the sublabial approach for pituitary adenoma, what structures can be injured? |
| G7 p.656:118mm |
a. artery g_____ p_____ | greater palatine artery branches (AKA) descending palatal arteries (They enter the incisive foramina and incisive canals.) |
|
b. nerve n_____ | nasopalatine nerves (Branch of maxillary nerve [V2] serves roof of mouth, upper lip, and teeth.) |
|
195. True or False. Regarding pituitary tumors: |
| G7 p.656:150mm |
a. Minimal enlargement of the sella and a large suprasellar mass indicate a transcranial approach. | true | |
b. The subtemporal approach provides good visualization of the optic nerves, chiasm, and carotid arteries. | false (The subfrontal approach is better to see this anatomy.) |
|
c. The subfrontal approach may be more difficult with prefixed chiasm. | true |
|
d. The transsphenoidal approach is preferred for microadenomas. | true |
|
196. Conditions indicating transsphenoidal approach that may not be appropriate for this pituitary tumor include: |
| G7 p.656:151mm |
a. sella not_____ | enlarged |
|
b. large_____ mass | suprasellar |
|
c. e_____ tumor | extrasellar |
|
d. sphenoid_____ | sinusitis |
|
197. Complete the following about transspehenoidal surgery: |
| G7 p.657:185mm |
a. Open the sella exactly in the_____. | midline |
|
b. Use the_____ _____ as your landmark. | nasal septum |
|
c. Is the sphenoid sinus septum also reliable? | no, it is unreliable |
|
198. Complete the following about intraoperative disaster: |
| G7 p.659:100mm |
a. Profuse arterial bleeding suggests_____ _____. | carotid injury |
|
b. It can usually be controlled by_____. | packing |
|
c. |
|
|
i. The operation should_____ _____ | be stopped |
|
ii. and_____ be done. | angiography |
|
d. |
|
|
i. If_____ is found | pseudoaneurysm |
|
ii. the patient is at risk for_____ _____. | lethal rupture |
|
e. |
|
|
i. It must be eliminated by_____ _____ | endovascular techniques |
|
ii. or surgical. | trapping |
|
199. True or False. Common complications of transsphenoidal pituitary surgery include |
| G7 p.659:135mm |
a. transient diabetes insipidus | true (common but lasts less than 3 months) |
|
b. basilar artery injury | false (Basilar artery injury is rare.) |
|
c. cerebrospinal fluid leakage | true (Cerebrospinal fluid leakage is common, 3.5%.) |
|
d. carotid artery rupture | false (Carotid artery rupture is rare.) | |
200. True or False. Treatment for diabetes insipidus includes the following: |
| G7 p.661:125mm |
a. desmopressin 2 to 4 mg daily (subcutaneous) | true |
|
b. vasopressin 5 U (IV) every 6 hours | true |
|
c. desmopressin 10 to 40 mg twice a day | true |
|
d. clofibrate 500 mg four times a day by mouth | true |
|
201. Complete the following regarding postoperative pituitary surgery: |
| G7 p.661:26mm |
a. diabetes insipidus |
|
|
i. can be diagnosed if urine output is more than_____ cc | 250 cc |
|
ii. for_____ | 1 to 2 hours |
|
b. ACTH (corticotropin) reserve |
|
|
i. take patient off steroids for_____ hours | 24 hours |
|
ii. check_____ a.m. cortisol level | 6 a.m. |
|
iii. normal cortisol level at 6 a.m. is_____ | above 9 μg/dL |
|
iv. suspect low cortisol is_____ | 3 to 9 μg/dL |
|
v. definitely low cortisol is_____ | below 3 μg/dL |
|
c. To assess for residual tumor don’t do CT until_____ _____ postoperative. | 4 months | G7 p.661:40mm |
202. Characterize the good outcomes of transsphenoidal surgery. |
| G7 p.662:60mm |
a. vision_____ _____ | much improved |
|
b. prolactin secreting tumors in_____% | 25% |
|
c. growth hormone secreting tumors in_____% | 20% |
|
d. Cushing disease—microadenomas in_____% | 85% |
|
e. acromegaly |
|
|
i. microadenoma in _____% | 85% |
|
ii. macroadenoma in _____% | 30% |
|
iii. all acromegalics in _____% | 50% |
|
f. recurrence _____% | 12% |
|
203. Regarding acromegaly, cure requires: |
| G7 p.662:130mm |
a. basal (morning) serum GH of less than_____ | 5 ng/mL |
|
b. suppression after ingesting glucose less than_____ | 2 ng/mL |
|
c. somatomedin-C (I-GF-1) of normal_____ acromegalics_____ | normal range—0.31 to 1.4 ng/mL; acromegalics 2.6 to 21.7 ng/mL. |
|
204. Characterize biochemical outcome acromegaly. |
| G7 p.662:120mm |
a. Recommended is a_____ serum GH level. | morning |
|
b. Cure is considered GH level of less than ng/ml. | 5 | |
c. In tumors less than 10 mm this is achieved in _____%. | 85% |
|
d. In all acrogmegalics cure is achieved in_____%. | 50% |
|
e. Macroadenomas cure is achieved in_____%. | 30% |
|
f. These patients should be seen for follow-up every_____ to_____ months. | 6 to 12 |
|
205. Answer the following about craniopharyngiomas: |
| G7 p.663:130mm |
a. Craniopharyngiomas are lined with what types of cells? | stratified squamous epithelium |
|
b. They arise from_____ _____ _____ of the pituitary. | anterior superior margin |
|
c. Show calcification |
|
|
i. on histology in _____% | 50% |
|
ii. on plain x-ray in children in_____% | 85% |
|
iii. on plain x-ray in adults in _____% | 40% |
|
d. Do they contain cysts? | yes |
|
e. Do they contain solid components also? | yes |
|
f. Do they undergo malignant degeneration? | no |
|
206. The pituitary stalk can be recognized by its pattern |
| G7 p.664:95mm |
a. of l_____ s_____ | longitudinal striations |
|
b. which are the long_____ _____. | portal veins |
|
207. Describe the Rathke cleft cyst (RCC). |
| G7 p.665:25mm |
a. Where are they located? | intrasellar—pars intermedia |
|
b. How common are they? | incidental finding in 20% of autopsies |
|
c. Do you find RCC together with pituitary adenomas? | no |
|
d. Why? | They arise from the same tissue, which goes one way or the other but not both. |
|
e. appearance on CT |
|
|
i. cystic? | yes |
|
ii. density? | low density |
|
iii. enhancement? | may have capsular enhancement |
|
208. True or False. Rathke cleft cysts arise in/at the: |
| G7 p.665:35mm |
a. anterior superior margin of pituitary | false |
|
b. neurohypophysis | false |
|
c. pars intermedia | true |
|
d. none of the above | false | |
209. Answer the following about Rathke cleft cyst: |
| G7 p.665:35mm |
a. Where is a Rathke cleft cyst located? | in the pars intermedia of pituitary |
|
b. From what does Rathke cleft cyst originate? | remnant of Rathke pouch—stomodeum |
|
210. True or False. A 14-year-old patient is found to have a 3 cm low-density lesion in the sella turcica. Surgical excision reveals a single-layer cuboidal epithelium. The most likely diagnosis is |
| G7 p.665:45mm |
a. mucocele | false |
|
b. epidermoid | false |
|
c. craniopharyngioma | false |
|
d. Rathke cleft cyst | true |
|
211. With a colloid cyst, hydrocephalus involves only the_____ _____. | lateral ventricles | G7 p.665:90mm |
212. Complete the following about primary brain tumors: |
| G7 p.665:120mm |
a. True or False. A 40-year-old male complains of intermittent headaches and gait difficulty. CT scan of head shows a cystic mass in the third ventricle. The most likely diagnosis is |
|
|
i. neurocystercercosis | false |
|
ii. meningioma | false |
|
iii. choroid plexus papilloma | false |
|
iv. colloid cyst | true |
|
b. the site of origin of this cystic mass is the |
|
|
i. d_____ e_____ of the recess of the postvelar arch called | diencephalic ependyma |
|
ii. the p_____ | paraphysis (that is, an evagination of the roof of the third ventricle) |
|
213. True or False. A 27-year-old male with a history of a colloid cyst who underwent a right frontal ventriculoperitoneal shunt 3 days ago returns to the emergency room (ER) with recurrence of severe headaches and gait difficulty. Treatment at this time could be |
| G7 p.110:110mm |
a. removal of ventriculoperitoneal shunt | false |
|
b. externalization of shunt | false |
|
c. placement of left frontal ventricular drainage | true (Colloid cysts can obstruct both foramina of Monro; thus, bilateral ventricular drainage is needed.) |
|
d. medical management and reassurance | false |
|
e. fenestration of the septum pellucidum | true |
|
f. removal of colloid cyst | true | |
214. Complete the following about colloid cyst: |
| G7 p.X:111mm |
a. shunt |
|
|
i. r_____ b_____ s_____ | requires bilateral shunts |
|
ii. or f_____ of s_____ p_____ plus o_____ s_____ | fenestration of septum pellucidum plus one shunt |
|
b. transcallosal approach complications |
|
|
i. v_____ i_____ | venous infarction |
|
ii. f_____ i_____ | fornix injury |
|
c. transcortical approach complications |
|
|
i. s_____ _____% | seizures 5% |
|
d. stereotactic aspiration |
|
|
i. f_____ —r_____ | failure—recurrence |
|
e. ventriculoscopy |
|
|
i. f_____ —r_____ | failure—recurrence |
|
215. Answer the following about hemangioblastoma: |
| G7 p.667:80mm |
a. What is the most common primary intraaxial tumor in the adult posterior fossa? | hemangioblastoma |
|
b. It can occur sporadically or as part of v_____ _____ – _____ disease. | von Hippel-Lindau |
|
c. What blood problem is associated? |
|
|
i. P_____ also known as | polycythemia |
|
ii. e_____ due to | erythropoietin |
|
iii. e_____. | erythropoitin |
|
d. Incidence of brain tumors _____% | 1 to 2% |
|
e. Characteristic appearance c_____ c_____ m_____ w_____ m_____ n_____ | mural nodule |
|
f. Should you remove the cyst wall? | no |
|
216. True or False. A 42-year-old male presents with headache, nausea, vomiting, and right-sided dysmetria. Laboratory studies revealed a hemoglobin of 17. The likely diagnosis is |
| G7 p.667:80mm |
a. metastatic lesion | false |
|
b. renal cell carcinoma | false |
|
c. hemangioblastoma | true (headache, nausea, vomiting-hydrocephalus-dysmetria-cerebellum high hemoglobin-polycythemia) |
|
d. high-grade astrocytoma | false |
|
217. Complete the following about the posterior fossa hemangioblastoma: |
| G7 p.667:80mm |
a. May be associated with |
|
|
i. p_____, e_____ | polycythemia, erythrocytosis |
|
ii. v_____ H_____ -L_____ d_____ | von Hippel-Lindau disease | |
218. Complete the following about von Hippel-Lindau disease (VHL): |
| G7 p.667:130mm |
Has hemangioblastomas tumors or cysts in the following sites: |
|
|
a. c_____ | cerebellum |
|
b. r_____ | retina |
|
c. b_____ | brain stem |
|
d. s_____ | spinal cord |
|
e. p_____ | pheochromocytomas |
|
f. c_____ | cysts in kidneys |
|
219. Complete the following about von Hippel-Lindau disease (VHL): |
| G7 p.667:135mm |
a. Most common in the_____ | cerebellum |
|
b. Second most common in the_____ | retina |
|
c. Always manifests before age_____ | 60 |
|
d. Incidence is 1 in every_____ persons | 35,000 |
|
220. True or False. The mode of inheritance of von Hippel-Lindau disease is: |
| G7 p.667:175mm |
a. autosomal recessive | false |
|
b. autosomal dominant | true |
|
c. sex linked | false |
|
d. multifactorial | false |
|
221. What is the diagnostic criteria for VHL? |
| G7 p.668:60mm |
a. |
|
|
i. One sign of VHL is needed if there is a_____ _____ | family history |
|
ii. It will be present in _____% | 80% |
|
b. Two signs of VHL if it is a_____ _____ mutation | de novo |
|
222. Complete the following about tumors associated with VHL: |
| G7 p.668:105mm |
a. Occur in younger persons if patient has_____ | VHL |
|
b. True or False. Cysts are associated with HGBs. | true |
|
c. Cerebellar HGBs are located in the |
|
|
i. s_____ | superficial |
|
ii. p_____ | posterior |
|
iii. s_____ half of the hemisphere | superior |
|
d. _____% of cerebellar HGBs were found in the_____ | 7%, vermis |
|
223. Complete the following about spinal cord hemangioblastoma: |
| G7 p.668:145mm |
a. _____% are in the cervical and thoracic cord. | 90% |
|
b. _____% are located in the posterior cord. | 96% |
|
c. _____% of spinal HGBs are associated with VHL. | 90% |
|
d. _____% symptoms are associated with syringomyelia. | 95% | |
224. The only disease with bilateral endolymphatic sac tumors is _____. | VHL | G7 p.668:180mm |
225. Complete the following about VHL: |
| G7 p.: mm |
a. Retinal hemangioblastomas occur in_____% | 50% |
|
b. Typically located in the_____ | periphery |
|
c. Frequently_____ | multiple |
|
d. Treat with laser_____ | photocoagulation |
|
226. Complete the following about renal cell carcinoma (RCC): |
| G7 p.669:130mm |
a. Which is the most common malignant tumor in VHL? | RCC |
|
b. Usually it is a_____ _____ _____. | clear cell carcinoma (CCC) |
|
c. It is the cause of death in_____ to_____% of VHL patients. | 15 to 50% |
|
227. Complete the following about surgical treatment of HGB: |
| G7 p.: mm |
a. Reserved until_____ | symptomatic |
|
b. Treatment of choice for_____ _____ HGBs | accessible cystic |
|
c. True or False. The wall must be removed. | false |
|
d. The_____ _____ must be removed. | mural nodule |
|
228. Answer the following about hemangioblastoma (HGB): |
| G7 p.671:17mm |
a. True or False. Starts at an earlier age in |
|
|
i. von Hippel-Lindau disease | true |
|
ii. sporadic cases | false |
|
b. In sporadic cases |
|
|
i. Most originate in the_____ | cerebellum |
|
ii. Next most common is the s_____ c_____ | spinal cord |
|
iii. _____% of patients with cerebellar HGB have VHL | 30% |
|
c. Erythropoitin liberated by the tumor may be responsible for the_____ | erythrocytosis | G7 p.671:53mm |
d. If one HGB is suspected we should do an |
| G7 p.671:140mm |
i. MRI scan of the _____ _____. | entire neuraxis |
|
ii. Vertebral angiography usually demonstrates _____ _____. | intense vascularity |
|
iii. CBC reveals _____. polycythemia |
| |
229. Complete the following about surgery on a solitary HGB: |
| G7 p.672:22mm |
a. It may be_____ in sporadic HGB | curative |
|
b. but not in_____. | VHL |
|
c. Preoperative _____may be helpful. | embolization | |
230. Complete the following about surgery on HGB: |
| G7 p.672:40mm |
a. They should be removed using _____ technique. | AVM |
|
b. Avoid_____ removal. | piecemeal |
|
c. Work along the_____ | margin |
|
d. and_____ the blood supply. | devascularize |
|
 CNS Lymphoma
CNS Lymphoma
231. Complete the following about CNS lymphoma: |
| G7 p.672:95mm |
a. Associated with an eye condition called_____ | uveitis |
|
b. How frequently does it occur? | 1 to 2% of all brain tumors |
|
c. What relationship does CNS lymphoma have with the ventricles? | up close to ventricles |
|
d. CT characteristics |
|
|
i. plain CT tumor is_____ | hyperdense to brain |
|
ii. contrast CT tumor_____ | enhances homogeneously |
|
iii. reminiscent of_____ _____ _____ | “fluffy cotton balls” |
|
e. reaction to steroids_____ | tumor may completely resolve |
|
f. CSF is positive for lymphoma cells in_____%. | only 10% |
|
g. What form of radiation therapy is given? | whole brain |
|
232. True or False. A 70-year-old male with a homogeneously enhancing lesion in the central gray matter and corpus callosum is suspected of having CNS lymphoma. What would make this diagnosis more likely and how is it properly diagnosed? |
| G7 p.672:107mm |
a. hydrocephalus | false |
|
b. café au lait spots | false |
|
c. uveitis | true (diagnosed with slit lamp) |
|
d. proximal muscle weakness | false |
|
233. A 73-year-old male with a history of recently diagnosed CNS lymphoma by biopsy presents to the ER with stupor and progressively deteriorating mental status. CT of the brain reveals the mass but no other abnormalities. |
| G7 p.675:55mm |
a. True or False. |
|
|
i. emergent surgical excision | false |
|
ii. radiation therapy | true (CNS lymphomas are very sensitive to radiation.) |
|
iii. chemotherapy | false |
|
iv. steroids | false |
|
b. followed by_____ | chemotherapy |
|
 Chordoma
Chordoma
234. Complete the following about chordoma: |
| G7 p.675:165mm |
a. It has a characteristic cell type called_____. | physaliphorous |
|
b. It occurs in the clivus in _____%. | 35% |
|
c. It occurs in the sacrococcygeal area in_____%. | 55% |
|
d. The recurrence rate after surgery is_____%. | 85% |
|
e. X-rays show_____ lesions with_____. | lytic lesions with calcifications |
|
f. Is there any gender predominance? | yes, male predominance for sacral chordomas |
|
g. What are the risks to bladder and bowel control |
|
|
i. from a sacrectomy between S1 and S2? | most will be impaired |
|
ii. from a sacrectomy between S2 and S3? | 50% will be impaired |
|
 Ganglioglioma
Ganglioglioma
235. True or False. Physaliphorous cells are distinctive features of |
| G7 p.675:165mm |
a. schwannomas | false |
|
b. pinealoblastomas | false |
|
c. gangliogliomas | false |
|
d. chordomas | true |
|
236. Answer the following about gangliogliomas: |
| G7 p.677:165mm |
a. True or False. Peak age of occurrence for gangliogliomas is |
|
|
i. children | true (Peak age is 11.) |
|
ii. elderly | false |
|
iii. no age predilection | false |
|
iv. unknown | false |
|
b. presenting symptom is_____ | seizure |
|
 Paraganglioma
Paraganglioma
237. Complete the following about paraganglioma: |
| G7 p.678:175mm |
a. used to be called_____ | chemodectomas |
|
b. now also called what if at |
|
|
i. carotid bifurcation: c_____ b_____ t_____ | carotid body tumor |
|
ii. jugular foramens: g_____ j_____ | glomusjugulare |
|
iii. adrenal medulla: p_____ | pheochromocytoma | |
c. may secrete |
|
|
i. e_____ | epinephrine |
|
ii. n_____ | norepinephrine |
|
iii. c_____ | catecholamines |
|
d. Resection of carotid body tumor has a |
|
|
i. morbidity of up to _____% | 50% |
|
ii. mortality of _____% | 5 to 13% |
|
238. Complete the following about pheochromocytoma: |
| G7 p.679:80mm |
a. We used to study_____ | catecholamines |
|
b. Better test now is |
|
|
i. f_____ | fractioned |
|
ii. p_____ | plasma |
|
iii. m_____ | metanephrines |
|
c. Imaging is_____ with_____ | MRI; contrast |
|
239. Carotid body tumor |
| G7 p.679:140mm |
a. and_____are the most common paraganglioma. | pheochromocytoma |
|
b. occur bilaterally in _____%. | 5% |
|
240. True or False. A 40-year-old female complains of a painless mass in her right upper neck and has deviation of the tongue to the right. The following is the most likely source of her mass: |
| G7 p.679:160mm |
a. carotid bifurcation | true (Paragangliomas present with mass in neck and CN XI and CN XII nerve palsy.) |
|
b. superior vagal ganglion | false |
|
c. inferior vagal ganglion | false |
|
d. hypoglossal nerve neuroma | false |
|
e. auricular branch of vagus | false |
|
241. Regarding carotid body tumors, treatment carries a_____ complication rate. | high | G7 p.680:25 mm |
242. Complete the following about glomus jugulare tumors: |
| G7 p.680:50mm |
a. They arise from_____ _____. | glomus bodies |
|
b. Are they vascular or avascular? | vascular |
|
c. Receives branches from the_____ _____ _____ | external carotid artery |
|
i. a_____ p_____ | ascending pharyngeal |
|
ii. p_____ a_____ | posterior auricular |
|
iii. o_____ | occipital |
|
iv. i_____ m_____ | internal maxillary |
|
d. _____ portion of the_____ _____ _____ | petrous portion of the internal carotid artery | |
243. Characterize glomus jugulare tumors. |
| G7 p.680:88mm |
a. female to male ratio | 6:1 |
|
b. Does it occur bilaterally? | no |
|
c. presenting symptoms |
|
|
i. h_____ l_____ | hearing loss |
|
ii. p_____ t_____ | pulsatile tinnitus |
|
d. clinical exam abnormalities |
|
|
i. h_____ l_____ and v_____ | hearing loss and vertigo CN VIII |
|
ii. t_____ p_____ t_____ | loss of taste posterior third of tongue CN IX |
|
iii. v_____ c_____ p_____ | vocal cord paralysis CN X |
|
iv. t_____ and SCM w_____ | trapezius and sternocleidomastoid (SCM) CN XI weakness |
|
v. t_____ a_____ and CN _____ i_____ to mass and s_____ of the hearing loss | tongue atrophy CN XII and ipsilateral to mass and side |
|
244. During surgical excision of a paraganglioma the patient is noted to have abrupt onset of hypotension and respiratory distress. This is most likely related to |
| G7 p.680:170mm |
a. intracranial pressure (ICP) changes | no |
|
b. vasovagal response | no |
|
c. inadvertent compression of airway | no |
|
d. tumor manipulation | yes |
|
e. due to r_____ of h_____ or b_____ | release of histamine or bradykinin |
|
245. Describe glomus jugulare differential diagnosis. |
| G7 p.681:15mm |
a. Distinguish from_____ _____ in the CPA | vestibular schwannoma |
|
b. True or False. By CT enhancement | false (Both enhance.) |
|
c. True or False. By presence of cystic component | true (VS may have cystic component.) |
|
d. True or False. By angiography | true (GJ [glomus jugulare] is very vascular.) |
|
e. What else will be learned by angiography? | whether the transverse sinus is occluded |
|
246. Complete the following about glomus jugulare: |
| G7 p.681:120mm |
a. What chemical should be tested for? | vanillylmandelic acid (VMA) |
|
b. If elevated, indicative of secretion of_____ | catecholamines |
|
c. similar to_____ | pheochromocytoma |
|
d. Treat medically_____ with and_____ | alpha and β blockers |
|
e. New clinical marker is_____ (NMN) | normetanephrine | G7 p.679:90mm |
 Ependymoma
Ependymoma
247. Complete the following about ependymoma: |
| G7 p.682:165mm |
a. Incidence among intracranial tumors in adults is _____%. | 5 to 6% |
|
b. Incidence among pediatric brain tumors is_____%. | 9% |
|
c. It occurs in children _____%. | 70% |
|
d. Incidence among spinal cord gliomas is_____%. | 60% |
|
e. Drop metastases occur in _____% of patients. | 11% |
|
f. What is the pathology of the distinctive type that occurs in the filum terminale? | myxopapillary | G7 p.683:190mm |
248. Characterize intracranial ependymomas. |
| G7 p.683:160mm |
a. usually occur in the_____ _____ | fourth ventricle |
|
b. dangerous to remove because they invade the_____ | floor of the fourth ventricle |
|
c. specifically they invade the_____ | obex |
|
d. current operative mortality _____% | 5 to 8% |
|
e. Is mortality higher in adults or in children? | children |
|
249. Answer the following about postop ependymoma: |
| G7 p.684:123mm |
a. What must we do? | LP |
|
b. When?_____ weeks postop | 2 |
|
c. What should be sent to lab? | 10cc CSF |
|
d. If positive follow with_____ | radiation | G7 p.684:140mm |
e. True or False. Ependymoma is sensitive to radiation. | true |
|
f. Name the tumor that is more sensitive. | medulloblastoma |
|
250. True or False. Regarding primary brain tumors: |
| G6 p.471:180mm |
a. Calcifications, although uncommon in medulloblastomas, may be seen ~20% of the time. | false (< 10%) |
|
b. The “banana sign” in the fourth ventricle refers to the medulloblastoma rather than to ependymomas. | true |
|
c. Ependymomas rank second only to medulloblastomas in radiosensitivity. | true |
|
d. Medulloblastomas arise from the roof of the fourth ventricle, the fastigium. | true |
|
e. Ependymomas arise from the floor of the fourth ventricle, the obex. | true |
|
251. What is the most common glioma of the spinal cord below the midthoracic region? | ependymoma | G7 p.685:100mm |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


 hemisphere,
hemisphere,  vermis,
vermis,  brain stem Symptoms:
brain stem Symptoms:
 von Hippel-Lindau,
von Hippel-Lindau,  neurofibromatosis,
neurofibromatosis,  tuberous sclerosis,
tuberous sclerosis,  Li-Fraumeni,
Li-Fraumeni,  Turcot
Turcot
 low risk,
low risk,  low moderate risk,
low moderate risk,  moderate high risk,
moderate high risk,  high risk
high risk
 hearing,
hearing,  facial nerve function,
facial nerve function,  trigeminal neuropathy,
trigeminal neuropathy,  tumor control
tumor control ,
, 
 growth hormone;
growth hormone;  ACTH;
ACTH;  prolactin;
prolactin;  TSH;
TSH;  nonsecretory
nonsecretory