 15
15 
What Is the Optimal Hematocrit and Hemoglobin for Head-Injured Patients?
BRIEF ANSWER
A hematocrit between 30 and 35% is widely believed to be optimal for head-injured patients. This number has been derived from experimental studies of blood viscosity and oxygen-carrying capacity. When cerebral autoregulation is intact, viscosity has little effect on cerebral blood flow (CBF), which is determined primarily by vessel diameter. With loss of autoregulation, vessels are maximally dilated, and viscosity becomes an important determinant of CBF. Halving the blood viscosity by reducing the hematocrit from 45–50% to 30–35% results in a doubling of CBF. Reducing the hematocrit to less than 30% is generally believed to result in only a slight decrease in viscosity at the expense of a greater decrease in oxygen-carrying capacity. However, no direct clinical studies exist to support this practice.
Background
The optimal hematocrit for head-injured patients has been the subject of intense study by physiologists and neurosurgeons for several decades. Initial theories involved the classical description of fluid dynamics as expressed by the Hagen-Poiseuille equation:
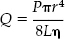
where Qis blood flow, Pis the pressure gradient, ris the vessel radius, L is the vessel length, and ŋ is the viscosity. Under normal conditions, vessel radius is the most important determinant of blood flow. Autoregulation of CBF functions by adjusting blood vessel radius to compensate for changes in pressure gradients and blood viscosity. In situations where autoregulation is lost and vessel radius is maximal, viscosity becomes an important determinant of CBF. According to the Hagen-Poiseuille equation, halving the blood viscosity doubles the CBF.
Pearl
When autoregulation is lost and vessel radius is maximal, viscosity becomes an important determinant of CBF.
The hematocrit is a major determinant of blood viscosity. The viscosity of plasma is 1.2 times that of water, whereas blood with a normal hematocrit of 45% has an apparent viscosity 2.4 times that of plasma. Reducing the hematocrit from 45 to 30% will halve the measured viscosity and therefore theoretically double the CBF. A linear relationship exists between hematocrit and the logarithm of blood viscosity at a given shear rate.1 Further hematocrit reduction will increase CBF, but at a substantial cost in terms of diminished oxygen delivery capacity. The oxygen delivery capacity is a function of hemoglobin and is calculated as:
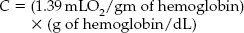
This equation assumes 100% hemoglobin saturation and disregards the very small amount of O2 dissolved in plasma. Based on these calculations, the optimal hematocrit for head-injured patients has been classically quoted to be between 30 and 35%.2
Pearl
Reducing the hematocrit from 45 to 30% will halve the measured viscosity and therefore theoretically double the CBF while decreasing oxygen-carrying capacity by only a third.
Further research has revealed that these calculations may not be accurate because the cerebral microcirculation has been found to be more complex than initially believed.3 Poiseuille’s equation only applies to ideal, or Newtonian, fluids. Blood is a non-Newtonian fluid, the viscosity of which changes with vessel diameter. Most suspensions of rigid particles display increasing viscosity as they flow through progressively narrower tubes. Fahraeus discovered that blood viscosity, however, actually decreases when the tube diameter becomes less than 0.3 mm. The Fahraeus effect is attributed to accumulation of red blood cells in the faster axial stream, whereas plasma tends to flow in the slower marginal layers. By contributing to shear thinning, that is, the decreased tendency for erythrocytes to aggregate as flow velocity increases, faster axial flow rates act to reduce viscosity. As the capillary size decreases to less than 7 µm, viscosity greatly increases because the vessel diameter is close to the erythrocyte size, an effect known as the inversion phenomenon. The erythrocytes travel through the capillaries faster than the plasma, resulting in a decreased apparent hematocrit in the capillaries. In a 300 µm or larger tube, the hematocrit is close to the hematocrit in larger vessels, but below 300 µm, the hematocrit steadily decreases. At 30 µm, the hematocrit is 40% less than in the larger blood vessels. The effects of the microcirculation on the optimal hematocrit are uncertain, but they do cast doubt on the validity of previous calculations based on Poiseuille’s equation.
Literature Review
Many animal studies have demonstrated increased CBF and decreased ischemia as a result of hemodilution and reduced hematocrit.4–6 When autoregulation is intact, lowered viscosity results in cerebral vessel narrowing and constant CBF. With loss of autoregulation in ischemic conditions, a reduction in blood viscosity results in an increase in CBF.7
Administration of whole blood to induce nondilutional hypervolemia has been shown not to improve collateral perfusion to ischemic regions or to reduce infarct size in experimental models of focal cerebral ischemia, despite significant augmentation of cardiac output.8 Analogous observations have been made in patients with idiopathic erythrocytosis (class III data). The strokes are attributed to elevated blood viscosity.9
Recent animal experiments have tried to address the role of the microcirculation in defining an optimal hematocrit. Experiments using in vivo red blood cell fluorescence videomicroscopy in intracortical capillaries have demonstrated an increasing red blood cell supply as hematocrit is lowered from 44 to 15%.10 Theoretically, hematocrits below 30% may be desirable in head trauma patients, but convincing experimental data are lacking.
Clinical studies examining optimal hematocrit after head trauma do not exist. Clinical data concerning the relationship between hematocrit and CBF are sparse. Class III data include a study by Harrison et al11 that found a correlation between elevated hematocrit and size of cerebral infarction after occlusive carotid disease. Thomas et al12 (class II data) measured CBF with an intravenous 133 Xe isotopic clearance technique in two groups of patients, one with hematocrits between 47 and 53% and another in whom those values ranged from 36 to 46%. The group with the higher values had an average CBF of 46.1 mL/100 g/min, whereas the group with the lower hematocrits had an average CBF of 65.0 mL/100 g/min (p > .001). Venesection was performed on 19 patients, reducing their hematocrit from 49.3 to 42.6%, with a resulting 50% increase in CBF from 41.4 mL/100 g/min to 62.1 mL/100 g/min. Oxygen-carrying capacity was calculated to fall by 13% in the venesection group but was accompanied by a 50% increase in CBF.12
Pearl



