Examples of criminal justice and behavioral health collaborative strategies using a Sequential Intercept Mapping Framework [18,20].
Police-based interventions
At the front-end early intercepts, there are evolving trends for police and community mental health providers to work together to achieve better outcomes, given that over many years it has been increasingly recognized that police may be first responders to increasing numbers of individuals with mental illness. Early research in this area referred to police as “street corner psychiatrists” [21], and noted that police were often faced with problem solving and management decisions, or an option to arrest, during these encounters.
Specialized training for police, through Crisis Intervention Team (CIT) development, for example, has expanded to numerous communities across the United States. Available data suggest that when police are specifically trained to work with individuals with mental illness through Crisis Intervention Teams, fewer injuries result to those involved [22]. Although not specifically identified as a violence-prevention strategy, CIT was developed in Memphis, Tennessee, in the late 1980s after an individual with mental illness was shot and killed during an encounter with police [23]. As these CIT programs have developed, more research is demonstrating that police are better able to respond to individuals in crisis, and consider alternative dispositions [24], since part of the training involves gaining familiarity with local programs and services. Separate from CIT, other types of law enforcement and behavioral health partnerships, including co-response to scenes and protocols that provide for tight hand-off of case referrals, similarly work to avoid arrest and direct individuals into treatment.
Court-involved interventions
Specialty court sessions and other alternatives to incarceration (sometimes referred to as court-level jail diversion) have been expanding over recent years. The wave of specialty courts began with the first drug court, which was established in Miami-Dade County, Florida, in 1989, after local stakeholders began to feel that a remedy for the revolving door for individuals with substance use disorders could benefit from creative solutions [25]. As of 2012, over 2734 drug courts have been established [26]. Enthusiasm about the effectiveness of drug courts [27] spawned interest in a host of other specialty courts, including mental health courts, veterans courts, re-entry courts, co-occurring courts, courts for drunk driving offenses, homelessness courts, and the like.
The premise of each of these specialty courts is that a judicial leader partners with a “treatment team” composed of probation, usually adversarial parties (such as defense and prosecuting attorneys), plus treatment providers to bring together shared goals and common solutions for individuals before the court. The individual participant generally must agree to participate in the specialty court on a voluntary basis, recognizing that participation involves mandated activities, regular court appearances before the judge, with rewards and sanctions for adherence and non-adherence, respectively. Data continue to emerge demonstrating that these programs result in fewer jail days and improved outcomes [28,29].
In addition to specialty court sessions, court-based programs to provide alternative pathways out of traditional criminal case processing for individuals with co-occurring disorders have expanded (also referred to as jail-diversion programs or alternatives to incarceration). As more of these programs evolve, programs are targeting special populations, such as veterans [30]. The ability to work with these groups brings together a host of resources for those involved in the justice system that can help target public safety, behavioral health, and improved functioning.
Programs linked to re-entry and community correctional supervision
Specialized programs also bring together resources for individuals with co-occurring disorders who are re-entering communities after a period of incarceration in jails and prisons [31]. Critical Time Intervention, for example, is a time-limited, staged intervention that is designed to help link individuals with mental illness to services and enhance their engagement in community programs. Early studies showed promise with working with individuals with mental illness upon re-entry from jails and prisons [32]. Forensic Assertive Community Treatment is another type of program in which justice-involved individuals with mental illness are provided intensive wrap-around, community-based services that integrate criminal justice personnel and often receive referrals from criminal justice programs. Although more research is needed, this intervention has shown some positive results in preventing arrest and incarceration [33]. A more recent study examined these two types of programs and found that both represented differing strategies that worked to enhance engagement, though each has unique components that may link to different resources over time [34].
Integration of Conceptual Models into Programs to Reduce Violence and Criminal Risks
Collaborative behavioral health and justice programs and services will likely continue to be refined with their ongoing expansion as part of the fabric of community-based services. In order to utilize these interventions most beneficially, targeted populations and approaches continue to be developed. Steadman et al. [35], for example, noted that mental health courts reduce jail days and re-incarceration, but may be inherently more expensive overall, and thus from a fiscal perspective argued that it is critical to target the “right” services for the “right” people. With that in mind, this review turns next to specific guidance related to conceptual models that address criminal offender rehabilitation on an individualized level to achieve risk mitigation and decreased recidivism.
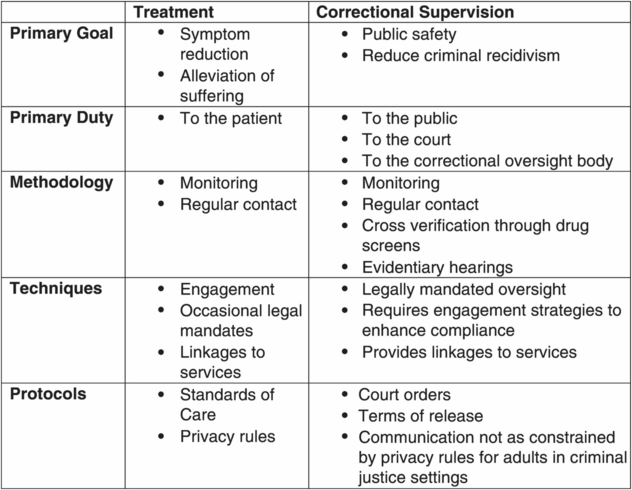
To begin with, it is important to note that criminal justice personnel view their roles from a different perspective than behavioral health treatment providers. In particular, criminal justice personnel see their primary mission as enhancing public safety outcomes and adhering to court orders, whereas traditional behavioral health services have focused their overall mission on symptom reduction, recovery, and improved psychosocial functioning (see Figure 30.2). Indeed, actions related to treatment interventions and correctional supervision can be applied synergistically for justice-involved behavioral health populations in order to achieve the overarching goal of public safety [10].
Evolving concepts therefore involve taking apart an individual’s risks and putting together treatment planning and correctional supervision planning that can enhance engagement and maximize benefit of treatment services, while focusing on mitigating public safety risks.
In the early 1990s, Andrews et al. [36] wrote about the classification of individuals for focused and effective criminal offender rehabilitation. Other models have also been promulgated, such as the Good Lives Model (see http://www.goodlivesmodel.com), to address offender rehabilitation [37]. For the purpose of this review, however, the model by Andrews et al. [36] is delineated. This model is quite commonly seen now in criminal justice programs. In this “risk–need–responsivity” (RNR) framework, individuals should be identified in accordance with their level of risk for reoffending, and with prioritization of treatments and specific interventions targeting those at highest risk [10,36]. Studies examining factors that lead to the greatest risk of criminal recidivism point to the “big 8” factors (with the first 4 being the most associated with risk):
1. Antisocial behavior
2. Antisocial personality patterns
3. Antisocial cognition
4. Antisocial associates
5. Family or marital relational disruptions
6. School and/or work difficulties
7. Leisure and/or recreation deficits
According to the RNR model, for each individual, criminogenic needs should also be targeted as the dynamic factors that can be modified to reduce the risk of reoffending. Finally, factors that create barriers to learning or to achieving success with the targeted intervention, or so-called “responsivity” factors, are important to consider in aiming toward recidivism reduction. For example, an individual’s cognitive deficits or ongoing depression might make it more difficult for him or her to adhere to probation terms, make appointments, and generally comply with court orders. An individual with these factors is at greater risk for difficulties, such as technical violations that can include new charges. A lack of system and provider awareness of and ability to accommodate the individual’s responsivity can further compound the problem.
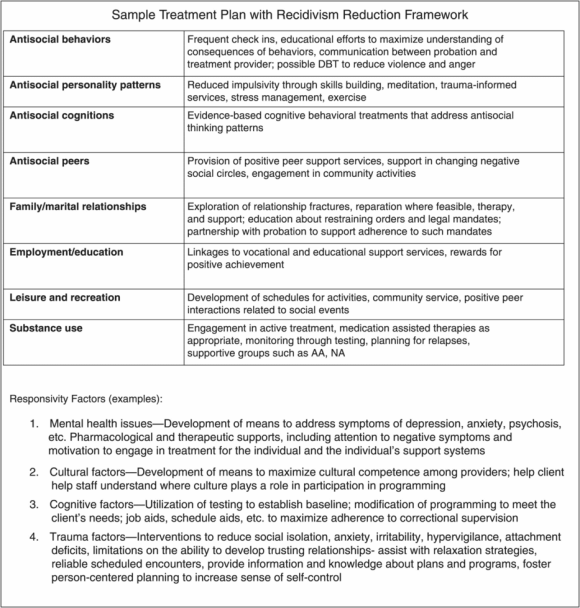
Treatment planning that addresses the central 8 risk/need factors and that also takes into account responsivity factors shows promise in reducing criminal recidivism. Figure 30.3 shows an example of a hypothetical treatment plan framed around RNR principles. This approach reflects desirable policy-level problem-solving efforts, given the aforementioned studies that point to the fact that recidivism among persons with mental illness may not be related as much to mental illness as to many of these other criminogenic risk factors [12,14,15]. Thus, although there remain countless questions that await further research, this area of treatment seems to offer an opportunity for augmentation of traditional behavioral health constructs to help address the problems of aggression and criminality among behavioral health populations.
Treatment and correctional supervision: similarities and differences.
Recidivism and Violence Risk Reduction in Practice
Traditional clinical violence risk assessment and risk management is an important practice for individuals in the behavioral health system who present concerns about public safety. Treatment planning traditionally includes a violence risk assessment approach of some type, which is targeted for the setting and for the purpose it is aiming to achieve [38]. Within an RNR framework, identification of the criminogenic risks and needs is a starting point that is focused on risk of criminal recidivism. There is a vast literature regarding instruments that might be used for screening for this risk that should serve as a reference point.
Once criminal recidivism risk (which is often thought of as a general public safety risk but may or may not involve a measure of violence) is established, the assessment of criminogenic needs helps to support treatment planning. In addition to focusing strongly on substance use treatment, practices related to psychotherapeutic techniques within correctional settings that have some evidence of efficacy could be helpful to consider [39]. Therapies, such as dialectical behavioral therapy, which is designed originally for individuals who engaged in frequent self-injury, have also shown positive results with correctional and forensic populations in reducing violence and criminal behavior [40]. Specific treatments involving cognitive behavioral techniques to address antisocial thinking may have promise for larger populations of behavioral health clients who cycle through the criminal justice system. These types of interventions have not traditionally been a part of general behavioral health services, though are more often seen in correctional settings. Moral Reconation Therapy (MRT) [41,42] and Thinking for a Change [43], for example, have been utilized with some success in criminal justice populations. In fact, MRT began with a focus on individuals with substance use disorders who also had antisocial features.
Substance use presents as an identified criminogenic risk in and of itself. Mental illness fits into the RNR framework not as one of the big 8 risk factors, but as part of what needs to be attended to with regard to responsivity. Osher et al. [10] lay out a criminogenic risk and behavioral health needs framework that targets interventions to the level of need in three main areas: criminogenic risk, substance use, and mental health. For a person with high criminogenic needs and low-level substance use or mental health needs, correctional supervision might be more intense and balanced by less intensive behavioral health treatments. In contrast, individuals who score low in criminogenic needs, but have high substance use treatment and mental health challenges, will require more intensive treatments, and perhaps less correctional monitoring and oversight.
One emerging manualized collaborative approach to such treatment is called MISSION-Criminal Justice. This approach combines several evidence-based practices and utilizes a case management and peer support model to target substance use, mental illness, and criminal recidivism, while taking into account the role of traumatic life experiences in behavioral responses [44,45]. Earlier versions of this model showed its utility among homeless veterans with co-occurring disorders [46], and preliminary administrative data in Massachusetts demonstrated its effectiveness in reducing re-incarceration, decreasing substance use, improving social connections, and helping individuals to stay engaged with mental health services.
In another innovative example, interventions have been developed that attend to the “culture of incarceration” [47]. A program designed to help individuals learn how to de-culturate from correctional settings, called Sensitizing Providers to the Effects of Correctional Incarceration on Treatment and Risk Management (SPECTRM), attempts to address staff readiness and client engagement as part of targeting responsivity factors in care [48]. Reentry After Prison (RAP) groups help clients learn about behaviors that may be adaptive in prison but are maladaptive upon re-entry, by using trauma-informed practices and cultural competence [47]. The application of these types of tools may be increasingly helpful in addressing the shared populations between criminal justice and behavioral health systems.
Recovery and Trauma-Informed Services
There is increased recognition of the critical importance of recovery concepts driving treatment that can help enhance engagement, improve individual lives, and potentially even impact recidivism. The concept of recovery is one that has grown exponentially from substance use delivery to mental health services.
The Substance Abuse and Mental Health Services Administration (SAMHSA) defines recovery as “a process of change through which individuals improve their health and wellness, live a self-directed life, and strive to reach their full potential” [49]. SAMHSA’s principles of recovery include 10 factors:
1. Hope
2. Person-driven
3. Many pathways
4. Holistic
5. Peer support
6. Relational
7. Culture
8. Addresses trauma
9. Strengths/responsibility
10. Respect
These principles provide anchors that can each be examined in relation to how an individual may achieve positive outcomes and maintain a life with minimal criminal justice involvement. Principles of recovery do not offer excuses for misconduct, or lessen personal responsibility for violent or antisocial behavior. Some individuals receiving mental health services will have impaired mental capacities impacting cognition and conduct in specific circumstances, challenging notions of personal accountability. Nevertheless, if we frame our view of the majority of individuals with behavioral health conditions as responsible, productive individuals, it is important to keep in the forefront their strengths and resiliency factors to maximize positive outcomes.
Services that are trauma-informed and trauma-responsive provide the needed sensitivity to the realities of behavioral health and criminal justice populations. It is widely recognized that the prevalence of trauma in criminal justice populations is high [50]. Trauma can be a major factor in mental health [51], and this includes witnessing prior violence and experiencing physical and sexual abuse. Furthermore, as noted above, post-traumatic stress disorder and trauma histories can contribute to aggressive behavior [52,53]. Thus, trauma is a responsivity factor that plays a complicated multidirectional role in an individual’s behavior and symptoms.
Enhancing trauma-sensitivity across systems and within treatment and across settings is therefore good practice. Here again, SAMHSA has recently offered some guidance that includes the “4 Rs” related to developing trauma responsive organizations, including (1) realization about trauma and how it can affect individuals and groups; (2) recognition of the signs of trauma; (3) responsiveness of the program or system to all persons involved by applying trauma-informed principles throughout; and (4) resistance of re-traumatization of clients and staff [54]. Beyond recognition of the individual’s historical trauma exposure, it is also helpful to recognize how interactions across settings can themselves be traumatizing. Jails, prisons, and psychiatric hospitals, for example, are places where individuals are sent where they are less in control of aspects of their lives. Traumatizing circumstances, such as disruptions in social networks, exposure to high noise level, being surrounded by individuals with tragic life circumstances, or those with antisocial and even violent propensities, can be realities of these settings.
An individual who is receiving services but who has high levels of trauma-related anxiety, hypervigilance, and irritability, for example, may be at risk of acting out aggressively, leaving treatment providers in the difficult position of managing behavior that may pose public safety risks in the moment, and that may be frightening or jarring to staff. Behaviors that occur under stress might be reduced by de-escalation that recognizes a trauma-informed strategy to add to other prevention techniques (e.g., calm and respectful responses by staff, including responses that require setting limits, development of institutional cultures promoting respect and safety, and the development of safety and crisis intervention plans for individuals and the system). Training for staff and for persons served in the recognition of signs and symptoms of trauma-reactivity, de-escalation, and relaxation skills development, as well as referral to trauma-focused treatment when needed, can all be helpful, specific activities within “trauma-informed” services. Examination of an individual’s natural support system may also yield some information that can be addressed with a trauma-responsive lens. As awareness of these issues evolves, correctional systems, community correctional supervision, specialty courts, and behavioral health systems have begun to examine how to develop more trauma-informed approaches in their work.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree