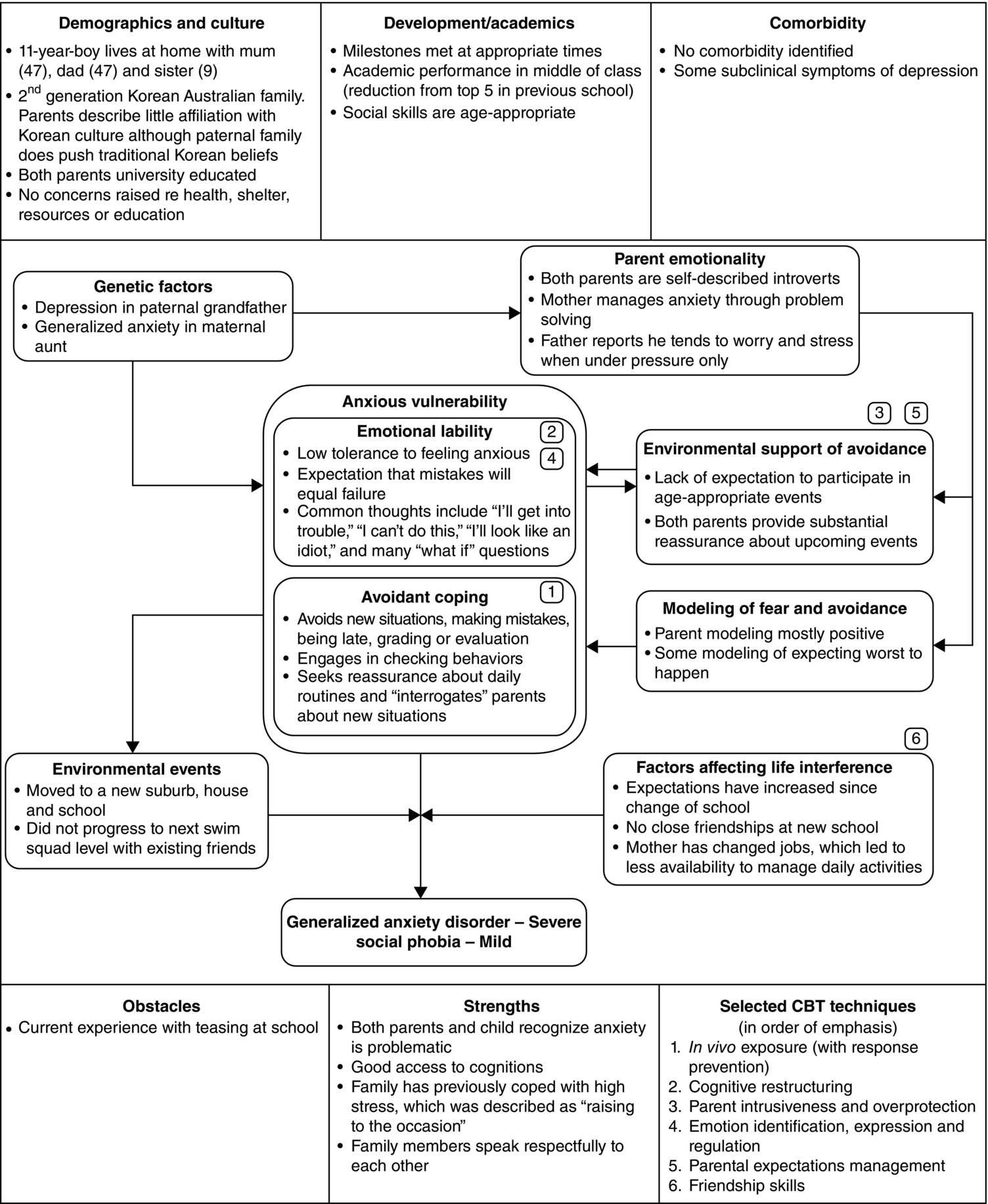
9 Heidi J. Lyneham Case formulation is the process of identifying the causes, antecedents, and maintaining factors related to a client’s emotional, interpersonal, and behavioral problems. It provides a template from which an individualized treatment plan can be derived. Importantly, case formulations are flexible. They account for all the information gathered at any point in time, and they are updated to reflect new information as it arises. The models of anxiety and depression presented in Chapter 8 are nomothetic, that is, they describe the general “laws” of how these problems arise. The purpose of the case formulation is to create an idiographic model relevant only to a specific case. Persons (1989) identifies numerous other functions of a case formulation. First, by ensuring that the therapist understands and communicates the presenting problems within the client’s personal context, it conveys hope that these problem(s) can be addressed. Second, it guides the development of a treatment plan that deliberately targets causal and maintaining factors that underlie the problems, increasing the likelihood of appropriate response to treatment. Third, it can pre-empt potential barriers that may undermine treatment progress or engagement. The treatment plan can subsequently be adjusted to proactively address these potential barriers, decreasing the likelihood that the barrier will interfere with progress. Several different approaches have been devised to guide the production of case formulations (Boschen and Oei 2008; Macneil, Hasty, Conus, and Berk 2012; Persons 1989). Surprisingly, though, there has been minimal research on the clinical utility and accuracy of case formulations and subsequent treatment plans, particularly with regard to child and adolescent populations. Inter-rater reliability of case formulations has been found to be adequate (Kuyken, Fothergill, Musa, and Chadwick 2005), the quality of case formulations improving with therapist experience and training (Eells et al. 2011). The clinical utility of case formulation as used in a community setting with adult anxiety and depression has been examined, case-formulated treatment leading to statistically and clinically significant change, comparable to that seen in randomized controlled trials of empirically supported treatments (Persons, Roberts, Zalecki, and Brechwald 2006). Direct comparison of case-formulated treatment and standardized treatment has shown slight superiority for the former (Persons and Tompkins 1997). Cognitive behavioral therapy (CBT) for child anxiety has been shown to be maximally effective when CBT interventions are matched to the specific anxiety symptoms experienced by the individual (Eisen and Silverman 1993, 1998), and long-term efficacy has been established for a majority of individuals after a CBT program for adolescent depression that incorporated use of case formulation (Treatment of Adolescent Depression [TADS] Team 2009). The case-formulation approach has also been shown to improve some aspects of the therapeutic alliance (Chadwick, Williams, and Mackenzie 2003); and client acceptance of a treatment rationale – one aspect of the case formulation – is related to good treatment outcome (see, e.g., Addis and Jacobson 2000). Despite the small amount of research to date, existing results are promising and case formulation is considered by organizations such as the APA to be fundamental to evidence-based practice (APA 2006). The distinct advantage of case formulation for the therapist in community practice is the flexibility it provides in determining a treatment plan for individuals who may or may not fit the criteria on which manual-based approaches were evaluated. For the purposes of this chapter, it will be assumed that the therapist has established, through appropriate assessment, that the targeted child or adolescent has an anxiety and/or a depressive disorder that is the basis for presentation to treatment (see Chapter 7 for more details on conducting an assessment). To devise a case formulation, a competent therapist will need to add, to the standard diagnostic and symptom severity assessment tools, a targeted assessment of the typical cognitions, behaviors, and emotions that relate to the presenting problem for the individual, as well as an evaluation of interpersonal processes between the individual and other people (e.g., parents, peers) during periods of high anxiety or low mood. This can be achieved by eliciting detailed descriptions of one or two recent events that highlight the presenting concerns and by enquiring about cognitions and behavioral choices during the chosen event(s) from both the perspective of the parent and that of the child or adolescent. Information on comorbidity, family history, current anxiety or depression in immediate family, the client’s developmental and academic functioning, and the family’s socio-demographic and cultural environment are also needed for a comprehensive case formulation. Following thorough assessment, the therapist should select the nomothetic model that is appropriate for the presenting individual, his/her family, and the organizational setting in which treatment is being offered. The chosen model will either reflect a particular manualized program or should be drawn from general models of anxiety or depression, such as those provided in Chapter 8. Once the model has been selected, the therapist should attach relevant evidence gathered during assessment to each aspect of the model. For example, Figure 9.1 applies the anxiety model presented in Chapter 8 to the case of an 11-year-old boy assessed as meeting criteria for generalized anxiety disorder and social phobia. As can be seen, a picture emerges from the idiographic model of what is causing and maintaining the presenting problem for the individual. Figure 9.1 Example of idiographic application of the anxiety model to the case of an 11-year-old boy. Chosen specific CBT skills are indicated by numerical indicators. Adapted from Figure 8.2, which was adapted from Rapee (2001) and Hudson and Rapee (2004). In addition to developing the idiographic representation of the chosen model, the potential impact that socio-demographics, culture, comorbidity, and development will have on engagement with treatment and on the likelihood of experiencing common obstacles during treatment should be considered. These influences can be described within a written case formulation or, if a visual representation of the case formulation is preferred, displayed on the idiographic model as contextual layers that surround the issues identified in the model. Finally, the formulation should consider the strengths of the individual and family, as recognition of these factors not only facilitates an optimistic view of the future, but can provide the therapist with a basis on which (s)he can build resilience (Macneil et al. 2012). These strengths should be added to any written or visual representation of the case formulation in a way that emphasizes their importance – for example they can be added to the outer layer of the contextual–idiographic model. Once an initial case formulation is established, the therapist needs to convert it into a treatment plan. Each child or adolescent will have a unique mix of factors implicated in the development of his/her anxiety and/or depressive disorder. Each factor will also vary on the strength of its association with current problems. Consequently the amount of emphasis given to a particular skill within a treatment plan must also vary. The treatment plan must therefore select the specific CBT techniques that will best address the identified problems, sequence the techniques in such a way that progress toward goals is optimized, and implement each technique at an appropriate dose, to ensure that the targeted problem is effectively overcome or managed. Each of these processes is described below. The competent therapist must ensure that (s)he has a thorough understanding of the purpose of each specific CBT technique, so that (s)he can appropriately link it to the causal or maintaining factor(s) that it is designed to address. Specific CBT techniques may focus on a single factor or may deliberately target multiple factors. Treatment manuals will provide guidance on the selection of appropriate techniques or, through design, will have made assumptions about the selection of techniques on the basis of the chosen nomothetic model and the target population. Where a therapist is using a module-based treatment manual, the clinical algorithms provided by the manual should be followed. In situations where treatment is guided by CBT theory and the therapist’s clinical judgment, the sections on clinical implication in Chapter 8 here, together with the reviews provided of each specific CBT technique in Chapters 12 through 19, should be used to guide the selection of appropriate techniques. On the basis of the case formulation, the therapist can overlay what specific CBT techniques will be used to address each component of the case formulation. (For an example of this, see Figure 9.1, where each numerical indicator provides the chosen specific CBT technique that will form the treatment plan.) The competent therapist must remain flexible throughout treatment. The initial case formulation, and consequently the treatment plan, must be updated as new information is discovered and as a result of the experience implementing each specific CBT technique with the client. For example, during the implementation of in-session exposure, it may become apparent that the parent encourages flight from challenging situations at the first sign of the child’s distress, despite having been presented with psycho-education regarding the role of overprotection in child anxiety. The flexible therapist will revise the case formulation or the treatment plan to work directly on the parent’s reactions during exposure, through one-on-one work on his/her beliefs regarding the child’s ability to cope with risk and/or by incorporating reduction of parent involvement directly into the child’s exposure hierarchy. Depending on the manual selected, the therapist may have limited or substantial control on the order of presentation of specific CBT techniques. In manuals where there is limited flexibility in the sequencing of techniques, the presented order reflects the nomothetic understanding of the targeted disorder(s). Therapist flexibility in this case focuses more on the tailoring of the technique to the specific cognitions, behaviors, or situations that the client experiences. In module-based manuals that provide greater flexibility, or in situations where the therapist is working within a general CBT framework, the sequence of selected techniques will be guided by the manual’s clinical algorithms (e.g., Chorpita 2007) or will be inferred from the direction and strength of relationships between factors identified in the case formulation. Within CBT models and at the diagnostic level, avoidance is key to all forms of anxiety. The specific CBT technique that directly targets avoidance and the only skill that appears without exception in every evidence-based treatment manual for anxiety is exposure. Consequently, after basic psycho-education, exposure would be considered the most essential technique to implement with a child or adolescent who has an anxiety disorder. In determining the sequence of skills for the treatment plan, the therapist may do best to ask him-/herself what skills will be needed prior to implementing exposure and what skills may be developed concurrently with it. For example, successful exposure to social situations in the school playground may not be possible until an underlying deficit in social skills is addressed. Therefore the treatment plan should reflect an early focus on developing basic social skills prior to exposure, as implementation of the newly learnt social skills would improve the likelihood of early success in exposure to social situations. Alternatively, the case formulation may indicate that excessive reassurance from the parent undermines the child’s ability to learn that (s)he can cope with challenging situations. In this case the treatment plan may reflect that, concurrently with the implementation of exposure, the parent would require (i) psycho-education concerning the role of excessive reassurance in his/her child’s evaluation of a situation; (ii) therapist modeling of the appropriate parent management during in-session exposure exercises; and, ultimately, (iii) parent-led in vivo exposure.
Case Formulation and Treatment Planning for Anxiety and Depression in Children and Adolescents
Introduction
Devising a Case Formulation and a Treatment Plan
Theoretically driven, context-aware case formulation
Dynamic Treatment Planning
Selecting specific CBT techniques
Sequencing selected specific CBT techniques
Sequencing selected specific CBT techniques for anxiety disorders
Sequencing selected specific CBT techniques for depressive disorders
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree





