Flowchart of patient disposition. The exclusion of data for all 33 patients from one site was caused by concern about the integrity of data from that site. Patients who showed no hostility at baseline (hostility score = 1; N = 790) were also excluded (see text).
Primary analysis of hostility change (HLM)
The results of our primary analysis of hostility change from baseline showed a statistically significant effect of treatment group (F4,1487 = 7.78, P < 0.0001), indicating differential treatment effects on hostility.
Post-hoc treatment group contrasts for change from baseline were computed for each subsequent time point and for overall change. Olanzapine was significantly superior to perphenazine and quetiapine at months 1, 3, 6, and 9. It was also significantly superior to ziprasidone at months 1, 3, and 6, and to risperidone at months 3 and 6. Corrected P values are shown in Figure 17.2. All medications produced statistically significant improvements in comparison with baseline at all time points, except for ziprasidone, which was not significant starting from month 9, and perphenazine at month 18.
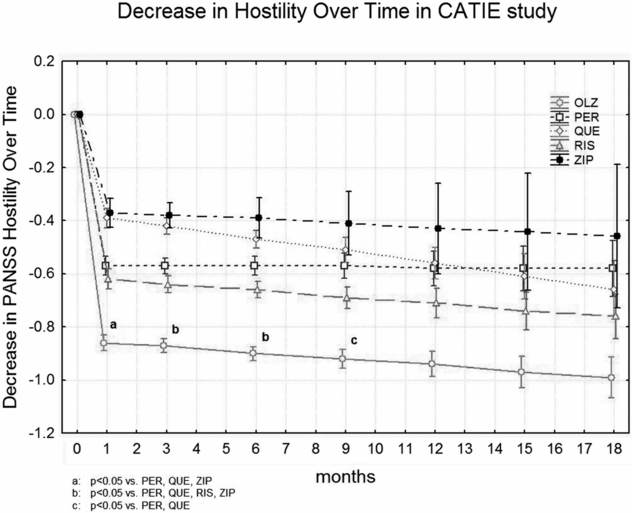
We also present the results that were not adjusted for change in positive symptoms. These results showed a statistically significant effect of treatment group (F4,1498 = 7.40, P < 0.0001). Olanzapine was significantly superior to perphenazine at months 1, 3, 6, and 9 (P ≤ 0.0161). It was also superior to quetiapine at months 1, 3, 6, 9, and 12 (P ≤ 0.0245); risperidone at months 3 and 6 (P ≤ 0.0319); and ziprasidone at months 1, 3, and 6 (P ≤ 0.0046).
The introduction of covariates for whether the participant was recruited before or after the introduction of ziprasidone, whether s/he had tardive dyskinesia at baseline, and for site effect had no substantial influence on principal results.
Sensitivity analysis (LOCF)
There was a statistically significant effect of treatment group (F = 5.48, P = 0.0002). Olanzapine was significantly superior to quetiapine (P = 0.0002) and to ziprasidone (P = 0.0048). Olanzapine’s superiority to risperidone was marginal (P = 0.0543).
The results of LOCF analysis not adjusted for change in positive symptoms showed a statistically significant effect of treatment group (F = 6.87, P > 0.0001). Olanzapine was significantly superior to quetiapine (P < 0. 0001), risperidone (P = 0.0143), and ziprasidone (P = 0.0007).
Discussion
The results supported our hypothesis that the medications would differ in their effects on hostility, and that olanzapine’s effects would be superior to those of other antipsychotics. Advantages were found for olanzapine compared with perphenazine, quetiapine, risperidone, and ziprasidone for a specific antihostility effect, independent of reduction of other positive symptoms of schizophrenia. Sensitivity analysis using LOCF was generally consistent with our primary HLM analysis.
The trajectory of response for olanzapine, as measured by a decrease in PANSS Hostility over time (Figure 17.2), is consistent with the trajectories of PANSS total score and of Clinical Global Impressions–Severity score as reported for the entire sample in the primary CATIE report [3]. Our results are also consistent with those of a similar post-hoc analysis of hostility in first-episode subjects with schizophrenia who were enrolled in the EUFEST trial [8], where olanzapine demonstrated advantages compared with haloperidol, quetiapine, and amisulpride. Our results are also consistent with those reported in a 12-week randomized double-blind clinical trial that was specifically designed to test specific antiaggressive effects of clozapine, olanzapine, and haloperidol [12]. In that study, subjects who were assigned to clozapine had statistically significant lower endpoint aggression scores than patients assigned to either olanzapine or haloperidol. Patients in the olanzapine group had statistically significant lower endpoint aggression scores than patients in the haloperidol group. However, no differences were seen among the three groups in terms of reduction of psychopathology as measured by the PANSS total score, suggesting that clozapine’s and olanzapine’s advantages were related to a specific antiaggressive effect.
In addition to this report and that from EUFEST, our methods of assessing specific antihostility effects of second-generation antipsychotics have been previously used a priori [13], as well as in a number of other post-hoc analyses [14–16]. Similar techniques have been used post-hoc by others [17–19]. Results have varied from superiority to haloperidol (compared to risperidone, olanzapine, quetiapine, and ziprasidone) to no difference from haloperidol (for aripiprazole) in terms of antihostility or antiaggressive effect. Compared with haloperidol, the second-generation antipsychotics were associated with fewer extrapyramidal effects and thus were considered more tolerable and overall more effective. Methodologies varied, however, and specific antihostility or antiaggressive effect was not always determined (for olanzapine [17]) or was inconsistently demonstrated (for quetiapine [18,19]).
The correlation of PANSS Hostility item scores and violent outcomes may not be consistent. Although we found that medications differed in their effects on hostility during Phase 1 of CATIE, there were no differences among treatments in their effects on violence during the same Phase [11]. There are several potential explanations of this apparent discrepancy.
First, hostility and violence are different constructs that are assessed using different instruments. A detailed description of the PANSS Hostility item is presented in a preceding section (“Study Populations and Interventions”).
In the study by Swanson et al. [11], the MacArthur Community Violence Interview was used to measure violent behavior and included minor violence, corresponding to battery without injury or weapon use; and serious violence, corresponding to any battery using a weapon or resulting in injury, any threat with a lethal weapon in hand, or any sexual assault. This level of violence differs qualitatively and quantitatively from the psychopathological symptom of hostility as measured by the PANSS.
Second, the time scale of the assessments of hostility in our study differed from that used in the Swanson study [11] to assess violence. We used multiple PANSS ratings that were based partly on the patient’s behavior during the rating interview and partly on the information covering the behavior in the preceding week [9]. Swanson et al. conducted two interviews: one at baseline and another at 6 months. Finally, the two studies used different subsets of CATIE patients.
Although hostility is different from violence, it can be a significant barrier to discharge from a hospital and reintegration into the community [20]; in the clinical experience of the authors, hostility is a common treatment target that is identified in individual care plans. The principal concern about hostility as a symptom is the potential for escalation of aggressive behaviors. Hostile behavior is a dynamic risk factor that is strongly associated with increased violence risk in persons who are psychotic, as demonstrated in a meta-analysis of 110 studies that reported on 45,533 individuals [7].
There are several limitations to our study. First, patients recruited for the CATIE study were not necessarily hostile, and those who were tended to display low levels of hostility. However, we note that the effect of olanzapine that was observed in the EUFEST study was very similar to the current results, although the EUFEST patients had higher baseline levels of hostility [8].
Second, with 74% of subjects discontinuing Phase 1, the attrition rate was high, although this rate is generally consistent with those previously observed [21]. The high discontinuation rate was partly due to study design, as subjects were eligible to discontinue Phase 1 and be re-randomized because of perceived lack of efficacy or tolerability with the original randomized medication.
Third, the CATIE was criticized because patients with tardive dyskinesia were not allowed to be randomized to perphenazine; because the maximal dose of olanzapine used was 30 mg per day (instead of the 20 mg per day recommended by the manufacturer), resulting in the average dose of 20 mg per day actually used; and for various other methodological problems [22].
The problem with the olanzapine dose has been somewhat mitigated by a subsequent 8-week study that compared the efficacy of olanzapine 10, 20, and 40 mg per day [23]. All dose groups showed improvement in PANSS total scores from baseline to endpoint without significant dose–response relationship. Thus, the higher dosing of olanzapine used in the CATIE is an unlikely explanation of its superior efficacy against hostility. It should be noted that similar effects of olanzapine against hostility were observed in the EUFEST study that used the recommended dose range of 5–20 mg per day.
Conclusion
Olanzapine demonstrated advantages in terms of a specific antihostility effect over the other antipsychotics tested in Phase 1 of the CATIE trial. This effect replicates, in long-term schizophrenia patients, the findings reported in patients in their first episode [8]. In general, the present findings are consistent with what is already known about olanzapine.
The use of olanzapine in these circumstances needs to be considered within the context of the multiple causes of the hostile behavior and olanzapine’s potential for weight gain and changes in metabolic variables [24].
Hostile and aggressive behavior in schizophrenia is etiologically heterogeneous [25]. Violence among adults with schizophrenia may follow at least two distinct pathways: one associated with premorbid conditions, including antisocial conduct, and another associated with the acute psychopathology of schizophrenia [26]. Schizophrenia patients who are violent may show comorbid psychopathic traits [27,28]. The effectiveness of antipsychotics in such cases merits further study.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree







