14 Fascicular Nerve Transfers to Restore Elbow Flexion A 25-year-old, right-handed man was riding a mountain bike down a hill when he struck a tree with his right shoulder. He was thrown from his bike and immediately noticed that he was unable to move his right arm. He was transferred to a level I trauma center and underwent a comprehensive trauma assessment. On examination, the patient had complete paralysis of the supraspinatus, infraspinatus, deltoid, biceps, brachialis, and supinator muscles (Medical Research Council [MRC] grade 0). He therefore completely lacked shoulder abduction, elbow flexion, and forearm supination. The remaining muscle groups of the right arm had MRC grade 4 to 5 power. Deep tendon reflexes were absent at biceps (0/4), difficult to elicit at brachioradialis (1+/4), and normal at triceps (2+/4). There was decreased sensation over the right lateral arm and forearm. Horner syndrome was not present. Plain radiographs and computed tomographic (CT) scan demonstrated right transverse process fractures at C5, C6, and C7. Magnetic resonance imaging (MRI) demonstrated left-sided deviation of the spinal cord within the spinal canal at the C5–6 level, which was interpreted to be a result of avulsion of right-sided nerve roots at this level. The patient was treated conservatively in a hard collar and discharged from hospital on postadmission day 3. Four weeks later, the patient was reassessed and underwent electromyographic (EMG) and nerve conduction studies (NCSs). On examination, there was now wasting of the supraspinatus, infraspinatus, deltoid, and biceps muscles and no motor recovery. Sensory examination demonstrated persistent numbness corresponding to the C5 and C6 dermatomes. EMG demonstrated denervation-related changes in the deltoid and biceps muscles. Sensory nerve action potentials (SNAPs) were present from the median nerve on NCS. The latter findings were consistent with preganglionic C5 and C6 nerve root avulsion injuries. The patient elected to undergo surgical intervention for rein-nervation of shoulder abduction and elbow flexion. Shoulder abduction and elbow flexion paralysis from upper trunk brachial plexus injury Erb palsy involves an avulsion or stretch injury of the C5, C6, and sometimes the C7 nerve roots. This type of injury results in a deficit to the muscles innervated by the nerves of the upper trunk. The dorsal scapular nerve arises from the C5 (C4 contribution minor) spinal nerve root and innervates the rhomboids. The long thoracic nerve arises off C5–7 spinal nerves and innervates the serratus anterior. The upper trunk of the brachial plexus is formed by the C5 and C6 spinal nerves. Just proximal to the level of the clavicle, the upper trunk forms a trident and gives rise to the suprascapular nerve before dividing into its anterior and posterior divisions to the lateral and posterior cords, respectively. The suprascapular nerve courses laterally, parallel to the course of the omohyoid muscle, entering the supraspinous fossa and sending motor branches to the supraspinatus (shoulder abduction < 90 degrees) and infraspinatus (external rotation of the shoulder) muscles. The lateral cord gives rise to the musculocutaneous nerve and, along with a portion of the medial cord, to the median nerve. The musculocutaneous nerve pierces the coracobrachialis muscle then runs in the medial aspect of the arm between the coracobrachialis and the biceps brachii muscles. Midway through its course it gives branches to the long and short heads of the biceps muscle, then within a few centimeters, gives a branch to the brachialis muscle. Beyond this point, it becomes a pure sensory nerve, providing innervation to the lateral aspect of the forearm. Musculocutaneous innervated muscles contribute to elbow flexion and supination. The posterior cord gives off the upper and lower sub-scapular nerves and the thoracodorsal nerve before dividing into the axillary and radial nerves. The only significant components of C5 and C6 contribution at this level are in the axillary and subscapular nerves, which innervate the deltoid muscle (shoulder abduction > 90 degrees), teres major (shoulder adduction), and teres minor (external rotation) muscles, and components to the radial nerve distributed to the brachioradialis and supination muscles. Traction injuries on the upper brachial plexus are particularly common when the shoulder and arm are forced awayfrom their attachments to the axial skeleton. In adults, this mechanism is most commonly seen in motorcycle injuries and falls at high speed where the shoulder absorbs the majority of the force. This type of traction is also seen in birth dystocia, where there is a need for assisted vaginal delivery. The injury to the brachial plexus is seldom limited to just one trunk or cord. The nerve roots may be avulsed from the spinal cord, there may be injury to the spinal cord itself, or there may be damage to individual nerves that arise from the plexus. Erb palsy is characterized by injury to elements of the upper and middle trunks. This type of injury results in a pattern of weakness and atrophy of the muscles indicated in Table 14–1. In addition, there is a sensory deficit in the C5, C6, and sometimes C7 dermatomes. Importantly, these patients may also have multiple other injuries, which may confound the assessment of the brachial plexus, such as multiple fractures, spinal cord injuries, and closed head injuries. In addition to traction injuries to the brachial plexus from trauma, other causes must be considered for a flaccid arm. These include laceration, compression and ischemia, and thermal and electrical injuries to the plexus or nerves. Central cord syndrome in the setting of preexisting cervical stenosis may also cause flaccidity of the upper limbs; however, the pattern of weakness is usually more severe in the distal upper limb. In addition, bony, muscular, tendinous, and ligamentous injuries may also result in a flaccid arm. The most important investigation in the setting of a brachial plexus injury is a detailed and thorough neurological examination. This is essential to determine the exact muscle groups involved and to assess the extent of loss of motor function. This exam should be performed in both the acute and the delayed settings to determine the degree of spontaneous recovery. Imaging studies are useful for detecting nerve root avulsions. They are well shown on thin-section CT myelography and MRI. When a root is avulsed, the meninges are pulled away from the spinal cord, forming a small pseudomeningocele. In addition, the spinal cord may be asymmetrically located within the spinal canal away from the avulsed root(s). A more direct sign is the absence of intradural nerve roots attached to the spinal cord on the involved side and levels.
 Case Presentation
Case Presentation
 Diagnosis
Diagnosis
 Anatomy
Anatomy
 Characteristic Clinical Presentation
Characteristic Clinical Presentation
 Differential Diagnosis
Differential Diagnosis
 Diagnostic Tests
Diagnostic Tests
| Site | Muscles |
|---|---|
| Trunks | |
| Upper | |
| Suprascapular | Supraspinatus, infraspinatus |
| Lateral pectoral | Upper part of pectoralis major |
| Musculocutaneous | Biceps and brachialis |
| Lateral half of median | Pronator teres, flexor carpi radialis (rare, usually only sensory loss seen in median distribution) |
| Part of radial | Brachioradialis and supinator |
| Axillary | Deltoid |
| Middle | |
| Thoracodorsal | Latissimus dorsi |
| Subscapular | Teres major |
| Radial | Triceps, variably other radial innervated muscles (except brachioradialis) with possible wrist drop |
| Lateral half of median | Pronator teres, flexor carpi radialis |
Source: Stewart JD. Focal Peripheral Neuropathies. 3rd ed. Philadelphia: Lippincott, Williams and Wilkins; 2000:122, Chapter 7. Adapted with permission.
Delayed EMG and nerve conduction studies are useful to confirm the findings of the neurological exam and to assess for the presence of SNAPs. These should be performed at least 2 to 3 weeks after the injury so that Wallerian degeneration of the distal parts of the injured nerves reaches its nadir. With a root avulsion, the damage to the sensory fibers is proximal to the dorsal root ganglia, so the distal sensory fibers are not separated from their cell bodies and remain viable. Thus the SNAPs are paradoxically normal,62even though the patient has no feeling in the distribution of the avulsed root.
 Management Options
Management Options
Many brachial plexus injuries will go on to spontaneous recovery and will not require surgical intervention. Three essential factors for predicting spontaneous recovery are (1) the site of damage in the plexus, (2) the severity of nerve damage (neurapraxia, axonotmesis, or neurotmesis), and (3) the presence or absence of root avulsions.
Injuries that occur far away from the target muscle have a lesser chance of spontaneous recovery. Furthermore, it takes longer for this reinnervation to occur because of the greater distance the growing nerve has to travel. It is therefore essential to consider a surgical option if no spontaneous recovery has occurred within the first 3 to 4 months. Neurapraxic injuries will typically recover far more quickly than this. This type of injury is expected when the mechanism of trauma is trivial, and confirmed when the clinical scenario demonstrates good recovery at a rate faster than that of spontaneous regrowth of a nerve (1 mm/d). Root avulsions are the strongest predictors of poor spontaneous recovery. These injuries should be treated surgically at an early stage so that reinnervation of the denervated muscles occurs before too much atrophy and deconditioning has occurred.
 Surgical Treatment
Surgical Treatment
The principles of the double transfer are illustrated in Fig. 14–1.
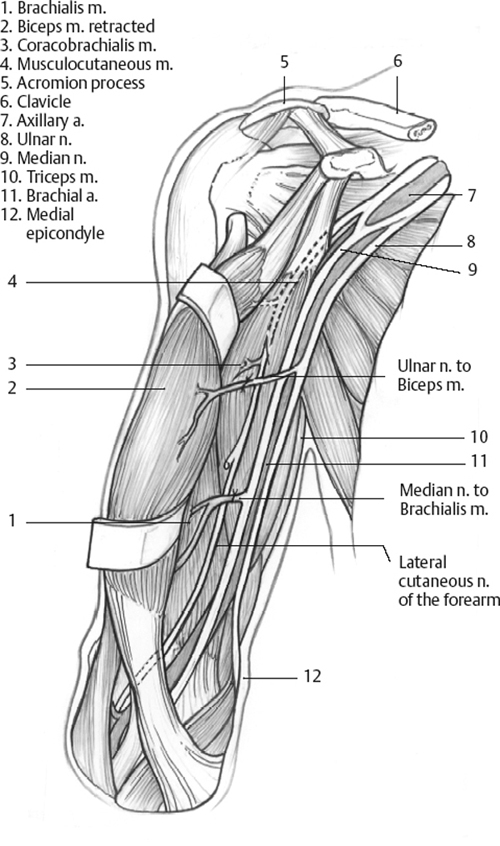
The musculocutaneous nerve is approached medially between the biceps and the coracobrachialis muscles, and the nerve to the biceps is identified. One must be aware of the numerous variations of the origin and distribution of the musculocutaneous nerve. Among these variations, the direct origin of the nerve to the biceps from the median nerve is not uncommon. The ulnar nerve is approached at the same level. Its identification is formally assessed by means of electrical stimulation. Further dissection is performed under microscopic magnification.
The branches of the musculocutaneous nerve destined to the biceps are identified. Usually, the vascular pedicle to the biceps has a more transverse orientation and does not interfere with the dissection of the nerve. The branches to the biceps muscle are split proximally from the musculocutaneous nerve for approximately 2 cm and transected. The distal part is then rotated medially toward the previously dissected ulnar nerve. The epineurium of the ulnar nerve is incised. One fascicle with an adequate size is selected, routinely anteriorly and medially situated. The fascicle is subjected to low-intensity electrical stimulation to confirm its motor capacity. The electrical stimulator device used by the anesthetists for plexus block anesthesia is per fectly suitable (intensity from 0 to 1 mA), or alternatively a Medtronic Xomed (MedtronicENT, Inc., Jacksonville, FL) disposable nerve stimulator (which stimulates at 0.5, 1, or 2 mA).
The chosen fascicle is separated from the rest of the ulnar nerve over 2 cm and divided distally. The fascicle is turned laterally and sutured to the nerve to the biceps with 11–0 nylon and fibrin glue.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


