68 Guided Lumbar Interbody Fusion
KEY POINTS
Introduction
Interbody lumbar fusion techniques have become increasingly popular because of improved rates of fusion, restoration of disc and foraminal height, and promotion of lordosis.1 Accessing the anterior column of the lumbar spine lowers the incidence of pseudoarthrosis and recreates the patient’s normal sagittal alignment.2 Late results of alleviating these effects through posterior fixation techniques alone show a significant loss of disc height at the injured segment and kyphotic deformation,3 necessitating access to the anterior column of the spine for interbody fusion. Conventional methods for accessing the anterior spine use an anterior retroperitoneal approach known as an anterior lumbar interbody fusion (ALIF), whereby a surgeon must mobilize the great vessels, sympathetic plexus, and ureter. This approach is associated with considerable surgical trauma, and higher rates of morbidity. As a result, most of these techniques typically require the presence of an experienced general or vascular surgeon, due to the risk of serious complications.2
Gaining popularity are techniques that access the anterior lumbar spine from a lateral retroperitoneal approach with the patient positioned in a lateral decubitus position. These procedures allow access to the anterior spine with little risk of injuring the peritoneum or great vessels, reducing the surgical risks compared to a standard ALIF operation. Since 1973, similar retroperitoneal approaches were documented to access the lumbar spine for performing lumbar sympathectomies and, starting in 1997 and 1998, Rosenthal et al. and McAfee et al., respectively, reported on minimally invasive anterior retroperitoneal approaches to the spine for anterior lumbar fusion. Early results show these alternative lateral approaches to the lumbar spine to be safe and effective for anterior fusion of the first through the fifth lumbar vertebrae.2
Description of the Device
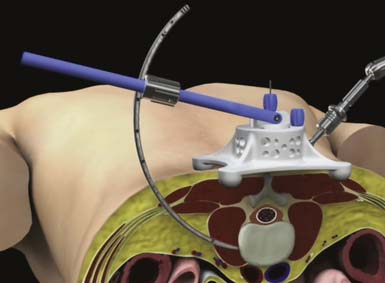
At the center of the GLIF technique is the ARC Portal System, a curvilinear lighted retractor system with a hinged top (Figure 68-1). This instrument is delivered over sequential dilators to the disc space, and the hinged top can be opened to gain direct visualization of key surgical landmarks during disc preparation. The device has proximal and distal stabilization capabilities to prevent portal migration during the procedure. In addition to the ARC Portal System, the GLIF technique utilizes specialized instrumentation to efficiently prepare the disc space for implant delivery.
Background of Scientific Testing / Clinical Outcomes
Bergey and Regan report, in a study conducted on 28 patients between 1996 and 2003, that early results show the lateral endoscopic transpsoas approach to the lumbar spine to be a safe, minimally invasive method for anterior fusion of the first through the fifth lumbar vertebrae. Their study indicates a risk of groin/thigh paresthesias and/or pain, but they report that these symptoms have proven to be transient. Of the 28 cases, eight patients experienced the transient groin/thigh numbness and/or pain; six patients experienced a small peritoneal perforation due to blunt dissection, with no bowel injuries; and two patients were converted to a mini-open lateral approach. Their report concludes that “this approach can be successfully combined with percutaneous pedicle screw fixation to provide a minimally invasive approach for circumferential fusions.”4
More recently, an extreme lateral interbody fusion technique (XLIF) has been adopted, with positive results. Pimenta indicates, in a study conducted to evaluate the XLIF technique for fixating lumbar degenerative scoliosis, that the transpsoas lateral approach has lower morbidity, does not require the use of endoscopes, avoids risks associated with anterior approaches, and avoids the invasion of the posterior spinal canal. Analyzing a consecutive series of 80 patients, Pimenta found the transpsoas approach to be a safe, reproducible, minimally invasive technique able to reconstruct sagittal balance, correct degenerative scoliosis, avoid the potential risks to the anterior approach, and promote rapid recovery.5
Wright reports similar results in a study of his first 10 patients to undergo the XLIF technique at Washington University. He reports the ability to perform a full discectomy, restore disc and foraminal height, as well as to achieve indirect canal decompression from L1 to L5. There were no vascular, visceral, or neurological complications. Nine out of ten patients ambulated on the day of surgery and were discharged on postoperative day one. One-year radiographic follow-up showed evidence of fusion. Additionally, the study indicated minimal narcotic requirement. Complications included three of 10 patients having transient pain with hip flexion that resolved by 6 weeks. His paper compared patients over 300 lb to those less than 300 lb, and found the surgical corridor to remain essentially the same length with no difference in outcomes, OR times, or blood loss. Hence, among one of the advantages of this technique he cited was that it is particularly useful in obese patients in whom anterior or posterior approaches would be more difficult.6
Operative Technique
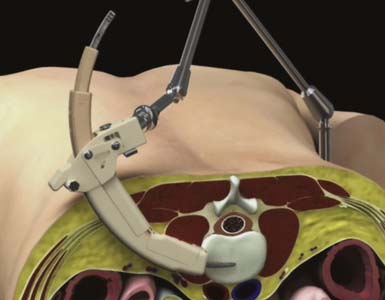
Proper patient positioning and delivery of the initial dilator are integral to the success of a GLIF technique. To facilitate proper trajectory of the instrumentation, the Calibrated Introducer was developed to repeatedly and reliably deliver the instruments to the surgical site (Figure 68-2).
Sequential dilation is performed using Dilator 2 and Dilator 3 to retract the soft tissue through the retroperitoneal space and psoas muscle in preparation for the delivery of the access portal. The ARC Portal is delivered over Dilator 3 and gently manipulated until the instrument is fully seated against the lateral wall of the anterior spinal column (Figure 68-3). Throughout the procedure, anterior-posterior fluoroscopy is used to confirm instrument placement and trajectory. Final placement of the device is maintained using a Table Fixation Arm. An Anterior Awl that retracts from the ARC Portal is deployed into the intervertebral disc space to establish distal fixation to the spine, and the dilators are removed.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree