Chapter 143 High Cervical and Occipitocervical Plate, Rod, Wire, and Bone Techniques
Abnormalities at the craniocervical junction were first reported in the early 19th century.1 The craniocervical junction includes the occiput, atlas, and axis vertebrae. Numerous pathologic conditions can lead to instability at the craniocervical junction. Common mechanisms of injury include trauma, rheumatoid arthritis, inflammatory and infectious lesions, tumors, and congenital anomalies.
Stability of the occipitoatlantal joint is provided by the cup-shaped configuration of the occipitoatlantal joint and the thick articular capsule, along with the anterior and posterior atlanto-occipital membranes.2–4 The fibrous capsule of the occipitoatlantal joint is usually thickest laterally and posteriorly and thin if not deficient medially. The tectorial membrane, which is a continuation of the posterior longitudinal ligament, attaches to the ventral foramen magnum and laterally to the medial aspects of the occipitoatlantal joints, playing an important role in the stability of the craniovertebral junction (CVJ).5 The alar ligaments are paired and arise on either side of the dens and have two components: the atlantoalar and the occipitoalar ligaments. These two components connect the dens to the lateral mass of C1 and to the medial aspect of the ipsilateral occipital condyle, respectively.6 These ligaments together with the cruciform and apical ligaments span from the axis vertebra to the occiput, and all provide some degree of stability to the occipitoatlantal joint.7
Causes of Instability in the Upper Cervical Spine
Instability of the upper cervical spine can be caused by congenital, traumatic, inflammatory, or neoplastic involvement.8 Of the several congenital abnormalities that occur in the upper cervical spine, basilar impression (or cranial settling) is the most common. Basilar impression may be progressive and lead to cervicomedullary spinal cord compression. Congenital ligamentous laxity in the upper cervical spine (e.g., Down syndrome, Morquio syndrome) can cause instability and subluxation. Upper cervical spine involvement in patients with rheumatoid arthritis can also lead to atlantoaxial instability and cranial settling, both of which may require surgical decompression and stabilization. Trauma, however, is the most common cause of instability in the upper cervical spine. Most upper cervical spine injuries result from blows to the head (e.g., motor vehicle accidents and falls). The direction of the force vector determines the type of injury (i.e., blows to the head versus deceleration of the torso). Injuries of the occipitoatlantal junction are usually fatal and are only detected postmortem. Atlantoaxial instability, on the other hand, can result from disruption of the bony or ligamentous elements or both. Bony fractures often involve the dens. Fractures of the odontoid process of C2 are classified into three types: I, II, and III.9 Type II odontoid fractures are unstable and notorious for nonunion with conservative management. Published reports of nonunion rates for conservatively managed type II odontoid fractures range from 30% to 60%. Type I fractures are always stable, and type III fractures may be unstable in 10% to 15% of cases.
Craniocervical instability can result from destructive tumors as well as iatrogenically, following resection of such craniocervical tumors. Instability may depend on the extent of condylar destruction or resection in these cases.
Instability at the Craniocervical Junction
There is a paucity of reports in the literature regarding resection of the occipital condyle or the destruction of the condyle with tumors of the craniocervical junction causing instability and the necessity for stabilization in this group of patients. The recommendations to date have been to stabilize the occipitocervical junction when greater than 70% of the occipital condyle has been removed.4,10
Management of Instability in the Upper Cervical Spine
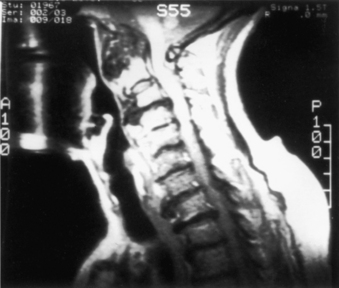
Patients with rheumatoid arthritis should have an MRI to ascertain the presence of inflammatory pannus and/or bony encroachment of the neural elements (Fig. 143-1). Patients who have evidence of neural compromise with occipitocervical instability should be considered for a ventral decompressive procedure before undergoing dorsal stabilization.11
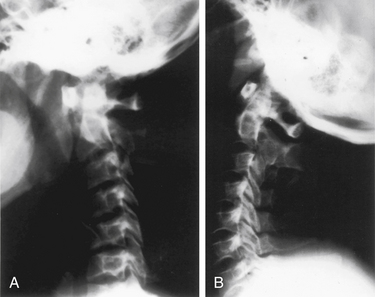
Patients with radiologic evidence of subluxation on neutral radiographs should also be evaluated with dynamic, lateral flexion-extension radiographs to assess the reducibility of the subluxation. Patients with nonreduced subluxations should undergo a trial of cervical traction to reduce the dislocation before a decision is made about the appropriate surgical treatment. Patients with chronic instability should remain in traction for 4 to 5 days with muscle relaxation before being considered for surgical treatment. Patients with a reducible subluxation, reduction achieved with flexion-extension, or with axial traction (Fig. 143-2) and without compromise of the cervicomedullary cord, may be safely stabilized by a dorsal approach.12 In contrast, patients who have a ventral spinal cord compression with a nonreducible subluxation may require a ventral transfacial decompression before undergoing occipitocervical stabilization. Usually, patients with instability related to rheumatoid arthritis or with pannus, but without neurologic deficit, can be stabilized from a dorsal approach without undergoing an initial ventral decompression.13 The pannus typically resolves in 6 to 12 months after abnormal movement has been eliminated.
Indications for Instrumentation in Occipitoatlantal Instability
The majority of traumatic occipitoatlantal dislocations are fatal. Some patients who arrive in the emergency department are treated effectively in cervical traction followed by occipitocervical instrumentation and fusion. Chronic instability at the occipitoatlantal junction occurs with rheumatoid arthritis, with tumors, and following tumor resection.14 Chronic instability at the craniocervical junction has been described as “glacial” instability in patients with chronic instability erosion of the occipitoatlantal articulation. This instability may result in cranial settling with associated rotary subluxation. In patients presenting with cranial settling with minimal or no neurologic deficits, reduction with cervical traction may be attempted, and if successful, dorsal occipitocervical instrumentation and fusion can be performed.15,16 In patients with significant neurologic deficits, a ventral decompression may be necessary before dorsal stabilization and fusion. Patients with rheumatoid arthritis, atlantoaxial subluxation, and associated cranial settling are candidates for occipitocervical instrumentation and fusion.
The only scientific evidence for the assessment of instability at the craniocervical junction following tumor surgery comes from the biomechanical study by Shin et al.17 Based on our clinical series, the biomechanical studies available, and new concepts of instability applied to the CVJ,18 we recommend that occipitocervical stabilization and fusion be performed when 50% or more of one condyle is resected or noted to have been destroyed by the tumor. A strong argument supporting this guideline can be made when using the extreme lateral transcondylar approach18 for the resection of these tumors. This approach removes the thickest parts of the capsule of the occipitoatlantal joint, and therefore renders the joint unstable (glacial instability). Thus, patients who have the condyle resected for surgical access and patients with tumor destruction of the condyle equal to or greater than 50% (but <70%) who do not undergo stabilization and fusion may progress to a glacial instability and eventually to overt instability with severe neck pain and torticollis.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree