Fig. 40.1
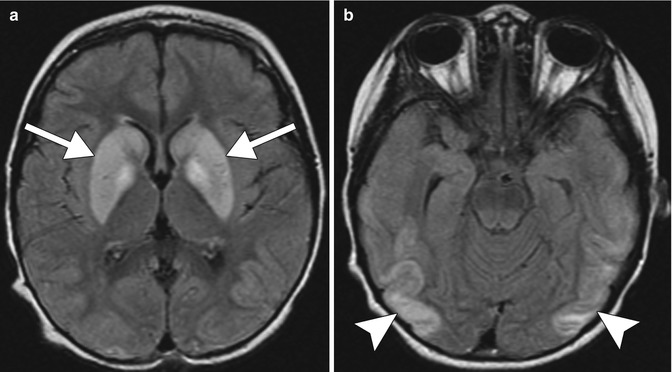
Insulin-induced hypoglycemic encephalopathy. The type 1 diabetic patient presented in coma. Axial T2-weighted (a), DWI (b), and ADC map (c) imaging reveal symmetrical corona radiata T2 hyperintensity with diffusion restriction (arrows)
Emergent management involves cardiorespiratory support in cases of coma and prompt restoration of euglycemia. The prognosis is determined by the duration and severity of hypoglycemia, which in turn impacts on the extent of brain injury. Basal ganglia and cortical involvement is generally associated with poor prognosis. Patients with poor neurological outcome who survive often eventually show generalized cerebral atrophy.
40.4 Differential diagnosis
All patients presenting with neurological symptoms, in particular seizure or coma, have measurement of their plasma glucose levels. Insulin overdose typically occurs in known diabetic patients. The history and laboratory investigations are key in making a diagnosis. Bilateral T2 hyperintensity involving the deep white matter, basal ganglia, and cerebral cortices can be seen in a variety of conditions. Symmetrical involvement favors a toxic, acquired metabolic or hypoxic process. Differential considerations include carbon monoxide, methotrexate, methanol, and cyanide toxicity, viral encephalopathy, and hypoxic ischemic injury.
Toxic-metabolic conditions and other drug toxicities, including carbon monoxide, methotrexate, methanol, and cyanide toxicity: Bilateral T2 hyperintensities involving the deep white matter, basal ganglia, and cerebral cortices can occur with all three toxins with overlapping neuroimaging appearances (Fig. 40.2). There are some specific features that can be helpful. In carbon monoxide poisoning, there is a predilection for involvement of the globus pallidus and temporal cortices. Bilateral T2 hyperintensities with diffusion restriction involving the deep white matter, in particular the centrum semiovale, are the most typical neuroimaging finding of methotrexate encephalopathy (refer to Chap. 19). Methanol toxicity typically results in bilateral hemorrhagic putaminal necrosis (refer to Chap. 3). Cyanide toxicity typically results in bilateral hemorrhagic caudate, putaminal, and sensorimotor cortex necrosis.