10 Kinematics of the Aging Spine: A Review of Past Knowledge and Survey of Recent Developments, with a Focus on Patient-Management Implications for the Clinical Practitioner
KEY POINTS
The Current State of the Art: Diagnostic Efficacy of Today’s Functional Testing Method
The current clinical standard of care for performing functional testing of the spine was introduced in the 1940s1 and has since been the subject of scores of published investigations. Today’s method is beset by multiple performance problems2,3 and, although many practitioners are unaware of the fact, has been proven useless in differentiating normal from abnormal spinal function.4–7 In holding true to the tenets of evidence-based medicine it is critical that, as a starting point, practitioners understand the limitations of this method so testing results are interpreted appropriately.
Range of Motion (RoM) Measurements
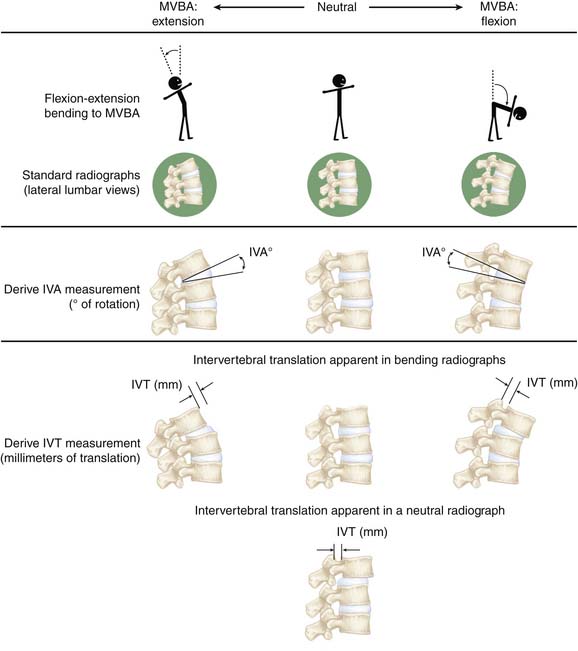
Today’s method for conducting functional testing of the spine (flexion/extension and lateral bending radiographs, which are referred to in this text as the clinical standard of care) involves capturing standard radiographs of the spine as subjects bend, and then hold their spines fixed in the extremes of motion in either the sagittal (in the case of flexion/extension) or coronal (in the case of lateral bending) planes. These studies are separate to, but often used as an adjunct with, other medical imaging studies such as plain radiographs or CT scans in the diagnostic assessment of a patient’s spine. When performing these motions, each subject bends in each direction to his or her own maximum voluntary bending angle (MVBA).
These two images taken at the extremes of trunk bending within a single plane are then interpreted — either manually using a pen, ruler, and protractor or more recently, with the advent of digital imaging, an imaging workstation — to derive range of motion (RoM) measurements. RoM measurements represent the total displacement between any two vertebrae during MVBA bending, and are expressed as both angulations, as measured in degrees and referred to in this text as the intervertebral angle (IVA) in either the coronal or sagittal plane, and translations in the sagittal plane, measured in millimeters and referred to in this text as the intervertebral translation (IVT). See Figure 10-1 for a simplified diagram showing how IVA and IVT are derived from radiographic images.
RoM is defined by the rotation of the body (IVA) and the translation of a point on the body (IVT). While the rotation is unambiguous, the translation is not. The translation is different for different points of the vertebral body and, additionally, it is subject to magnification and distortion on radiographs. This ambiguity has led to: (1) the introduction of multiple techniques for selecting points on the vertebral body and measuring IVT;2,4,8,21,22 (2) attempts to define standardized displacement thresholds for what constitutes translational instability;9 and (3) the proposal of multiple systems for scoring and classifying translational instabilities (there have been the Myerding scale,10 the Newman Scale,11 and the modified Newman scale12 for scoring translational instabilities, as well as the Wiltse13 system for classifying them).
Grade 4 is 75% to 100%; over 100% is spondyloptosis, when the vertebra completely falls off the supporting vertebra. One key advantage of the Myerding system is that it is a relative grading system, meaning that it helps to control for distortion and magnification errors that can be associated with absolute measurements of displacement (millimeters) derived from radiographic images.
IVA is used clinically to assess intervertebral articulation in either the sagittal or coronal planes, and as such should theoretically be capable of detecting six specific types of intervertebral functional presentations (see Figure 10-2):
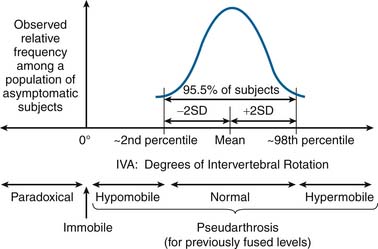
FIGURE 10-2 Theoretical framework for the detection of six functional presentations based on IVA measurements.
Measurement Variability in Range of Motion (RoM) Measurements
As with any quantitative diagnostic measurement parameter, measurement variability is the key driver of diagnostic efficacy in the application of such measurements to differentiate between the various types of patient presentations. Simply stated, measurement variability is the enemy of effective diagnosis: the higher the measurement variability, the less effective the resulting diagnosis. In the case of RoM measurements, it has been shown that measurement variability is high2,3 and diagnostic efficacy is low.4–7 The causes and effects of this measurement variability are well understood; however, the implications for the clinical practitioner have rarely been discussed in the published literature. Therefore one of the main goals of this section is to present a data-driven analysis of RoM measurement variability and how this variability should be taken into account in the interpretation of functional testing results used in the diagnosis of spine disease and management of the aging spine.
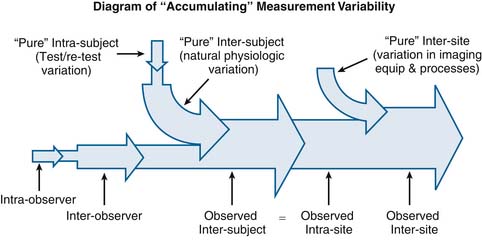
This concept of “accumulation” of variability also applies to the overall relationship between observer-related variability (interobserver and intraobserver variability) and subject-related variability (intersubject and intrasubject variability). Subject-related variation in intervertebral motion exists as an inherent property of the physiology of the spine. In other words, there is a certain amount of variation that is inherent to the way the spines of different people move, or in the way a given person’s spine moves at different points in time. For this discussion, we will refer to this inherent variation as the “pure” intrasubject and intersubject variability. However it is impossible to measure this “pure” intrasubject and intersubject variability without constructing an observational system to take measurements, and any observational system constructed to take measurements is also subject to both intraobserver and interobserver variability. Therefore any measurement of intersubject variability, for this discussion called “observed intersubject variability,” necessarily “accumulates” the combined effects of both observer-related variability and subject-related variability.
See Figure 10-3 for a simplified conceptual diagram of how selected types of RoM measurement variability interrelate through the accumulation of measurement variability.
Using Normative IVA Data to Detect Normal Motion, Hypomobility, and Hypermobility
As previously discussed, it is theoretically possible to use normative IVA data from a population of asymptomatic subjects to differentiate normal from hypomobile and hypermobile intervertebral motion (see Figure 10-2). However, with the current standard of care for conducting spinal functional testing, only hypermobility and pseudarthrosis can be detected with an acceptable level of statistical confidence. This fact, although not widely discussed, has very significant implications in terms of patient management, which are discussed later in this section. However as a starting point to this discussion, it is necessary to first re-examine the conventional wisdom regarding what is currently considered “normal healthy” intervertebral rotation.
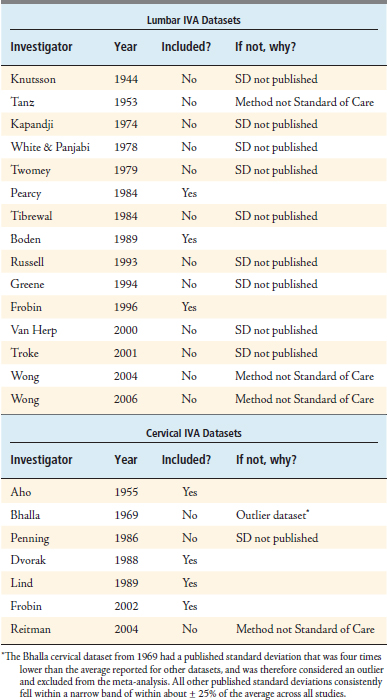
In conducting this meta-analysis, a total of 22 published IVA datasets were identified (15 lumbar and 7 cervical). Each dataset was carefully examined and screened to ensure that: (1) the method for measuring IVA was consistent with the current clinical standard of care, and (2) the variability (standard deviation, or SD) among observed IVA values was published along with the mean. After applying this screen, three lumbar datasets and four cervical datasets qualified for this meta-analysis. See Table 10-1 for a list of all 22 datasets that were considered.
After including all qualifying datasets, the following values were tabulated for the mean and standard deviation of observed IVA values taken from multiple populations of asymptomatic subjects across multiple sites (Table 10-2). The standard deviation values in the “Aggregated Across Sites” column at the far right of each table represent the standard deviation of the superset created by combining the observed values from all sites, and represents the observed intersite variability associated with the current standard of care for measuring IVA at each level, while the standard deviation values for each investigator represent that investigator’s site’s observed intersubject/intrasite variability.
TABLE 10-2 Normative IVA Data That Account for the Effects of Intersite Variability, Thereby Allowing for a More Representative Account of Mean IVA Values Than Has Ever Been Published in Any Single-Site Study
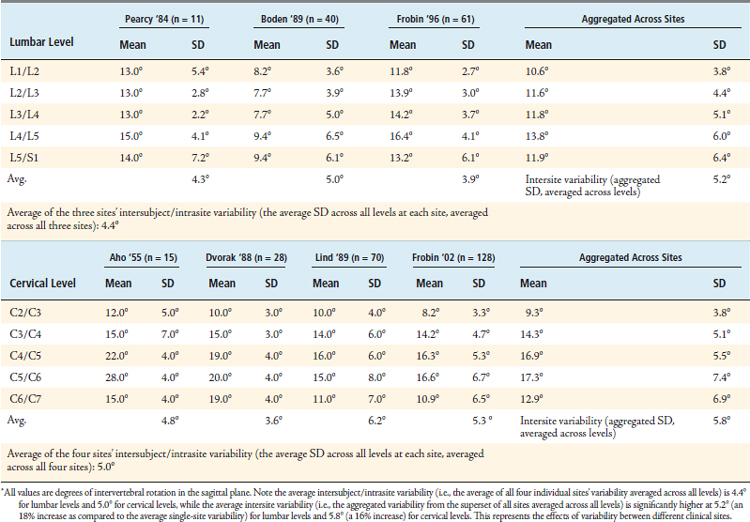
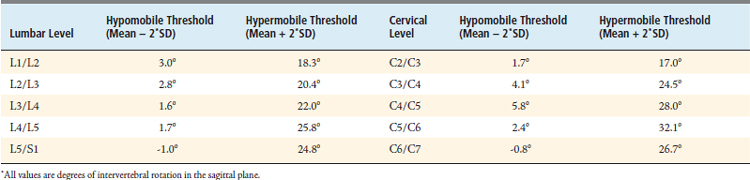
Using these normative values that account for the effects of intersite variability, it is possible to produce threshold IVA values that represent hypomobility and hypermobility, as given in Table 10-3.
Effects of IVA Measurement Variability on the Diagnostic Efficacy of Functional Testing of the Spine
To quantitatively assess the diagnostic efficacy of using IVA to detect different functional presentation (hypomobility, hypermobility, normal motion, etc.), it would be necessary to have a gold standard method for identifying true positives and true negatives for each type of functional presentation. If such a gold standard method existed, it would then be possible to quantitatively assess diagnostic efficacy with the traditional diagnostic efficacy parameters of sensitivity (Sn), Specificity (Sp), and the positive/negative likelihood ratios (+LR and −LR). however, the authors are unaware of that any such gold standard exists∗ and it is therefore impossible to measure these traditionally used diagnostic efficacy parameters. Therefore in this discussion of diagnostic efficacy associated with IVA measurements, these efficacy parameters will be described qualitatively in lieu of being able to quantitatively measure them.
As reflected in the hypomobility and hypermobility thresholds given in Table 10-3, the current standard of care for measuring IVA involves a high degree of measurement variability. This high degree of measurement variability, in turn, has disastrous consequences on the diagnostic efficacy of using IVA to detect intervertebral motion dysfunction. The first problem lies with the very low thresholds for detecting intervertebral hypomobility. Vertebral levels with IVA measurements of less than 2° to 5° are generally considered to be fused.14,15 As previously discussed, the FDA considers any IVA of up to 5° as effectively immobile for the purpose of evaluating arthrodesis status following a fusion. Therefore, because the hypomobility thresholds are all below the FDA’s 5° threshold for what is considered a fused FSU (except at C4/C5; Table 10-3), it is impossible to use IVA to differentiate hypomobile motion from a fusion, effectively rendering hypomobility an undetectable condition. A second consequence of this overlap between what is considered normal and hypomobile motion with what is considered a fused FSU is that one is guaranteed reduced specificity in detecting immobility as well as reduced sensitivity in detecting normal motion (because a “true normal” with an observed IVA of less than 5° is both a false negative in the detection of normal motion as well as a false positive in the detection of immobility).
The second problem lies with the thresholds for detecting both intervertebral hypermobility and hypomobility. The thresholds for hypermobility are so high because IVA measurement variability is so large. Having such a high threshold for hypermobility (the average threshold for lumbar levels is 22° and for cervical levels is 26°, from Table 10-3) ensures that only the grossest of rotational hypermobilities will register as being definitively hypermobile; thus subtle hypermobilities remain undetected and register as “normal.” Similarly, with hypomobility, high IVA variability makes the hypomobility thresholds so low that only the grossest of hypomobilities could register as being definitively hypomobile. As a consequence, the sensitivity of using IVA to detect hyper/hypomobility as well as the specificity of using IVA to detect normal motion are both reduced (those patients who register as normal but who have a subtle hyper/hypomobility are a false positive in the detection of normal motion as well as a false negative in the detection of hyper/hypomobility).
A third problem arises when one tries to use IVA to rule out hypomobility or hypermobility. It is theoretically possible to rule out hypomobility if observed IVA is sufficiently high. For example, if IVA is confirmed to be above the mean for any level, then it would be possible to rule out hypomobility (even the subtle hypomobilities described in the previous paragraph). It is similarly possible to rule out hypermobility if observed IVA is sufficiently low. However, one must consider the effects of interobserver variability in IVA measurements to be sure that a measurement is above or below the mean in producing threshold values to rule out hypomobility and hypermobility. In quantifying the interobserver variability at one investigational site, Lim et al.3 reported that the 95% confidence interval for the interobserver variability in lumbar IVA measurements is ±5.2°. However, as this study took place at only one site, it almost certainly underestimates the actual interobserver variability that exists across different clinical sites. Nonetheless, if one uses the Lim estimate and assumes that an IVA measurement must be 5.2 ° above/below the mean to be 95% confident that the observed IVA is actually above/below the mean, and if one further assumes that any IVA measurement above/below the mean rules out hypo/hyper-mobility, then one can produce the “rule-out” thresholds for hypomobility and hypermobility given in Table 10-4. However, there are some limitations associated with the data used to create these threshold values (as described in the caption for Table 10-4), so therefore they should be considered nondefinitive until these limitations are addressed and new thresholds can be produced.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree