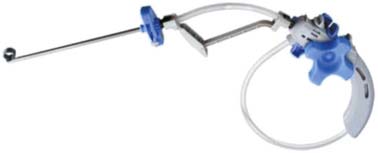
38 Kiva System in the Treatment of Vertebral Osteoporotic Compression Fractures
KEY POINTS
Introduction
Vertebral compression fractures (VCFs) have a high incidence in the elderly population and are the most common fractures in osteoporotic bones. The majority present without a history of major trauma.1 The incidence of VCF is increased in patients with a prior vertebral compression fracture, with studies indicating that nearly 20% of patients who have an osteoporotic VCF will develop a second fracture within a year of the first.2 Not only do these fractures cause significant morbidity in terms of pain, loss of mobility, and kyphosis, but the relative risk of death after a vertebral fracture is nearly nine times greater than in people without a vertebral fracture.2
Percutaneous vertebroplasty (PVP) was introduced in France in 1984 by Galibert and Deramond as a treatment for a malignant aggressive hemangioma.1 It is a therapeutic procedure performed to reduce pain and perhaps to stabilize vertebral lesions. Subsequently PVP was used to treat painful lesions such as hemangiomas, metastasis, multiple myeloma, and osteoporotic fractures. Today most patients undergoing PVP suffer from vertebral osteoporotic compression fractures. PVP is generally seen as a safe and efficient procedure for treatment of painful osteoporotic fractures.
Vertebral augmentation using balloon kyphoplasty and vertebroplasty3 is traditionally performed with polymethyl methacrylate (PMMA) cement. Clinical studies have demonstrated the efficacy of both methods in reducing fracture-related pain.2,4 However, there have also been reports of complications: extrusion of cement into surrounding tissue, vascular embolism in the corresponding vascular system, adverse systemic reactions to unpolymerized toxic monomers, and thermal damage to adjacent structures. The two latter complications are specific to PMMA. For this reason, and because PMMA does not become osseointegrated, attempts have been increasingly made in recent years to explore the possibilities of alternative cements by looking into biomaterials based on calcium phosphate (CaP). The properties of such bone cements, however, would have to fit a specific profile that takes into account the following parameters: setting behavior, mechanical fitness, and biological behavior.
Contraindications
Contraindications include the following:
Precautions
Precautions that should be taken include the following: