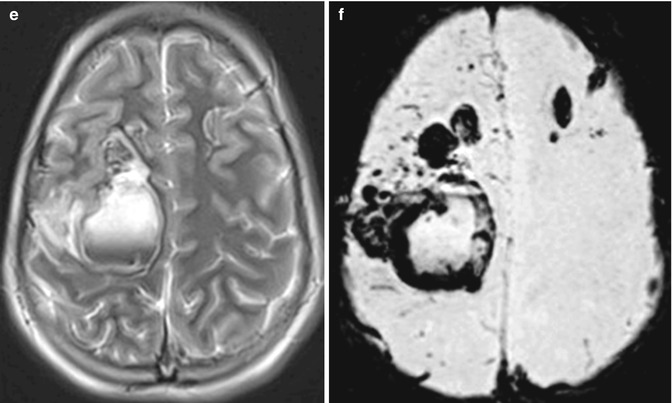
Fig. 21.1
Dural sinus thrombosis and hemorrhage associated with L-Asparaginase. A pediatric patient with newly diagnosed acute lymphoblastic leukemia presented with generalized tonic-clonic seizures and hemiparesis 14 days after treatment with L-Asp. Axial (a) and coronal (b) non-contrast CT demonstrate bilateral frontal lobe hemorrhages. T1-weighted sagittal non-contrast (c) and post-contrast fat-suppressed (d) images demonstrating thrombus within the superior sagittal sinus (arrows). Axial T2-weighted (e) and axial SWI MIP (f) images demonstrate the extensive bifrontal hemorrhages with layering blood products in the largest area of hemorrhage
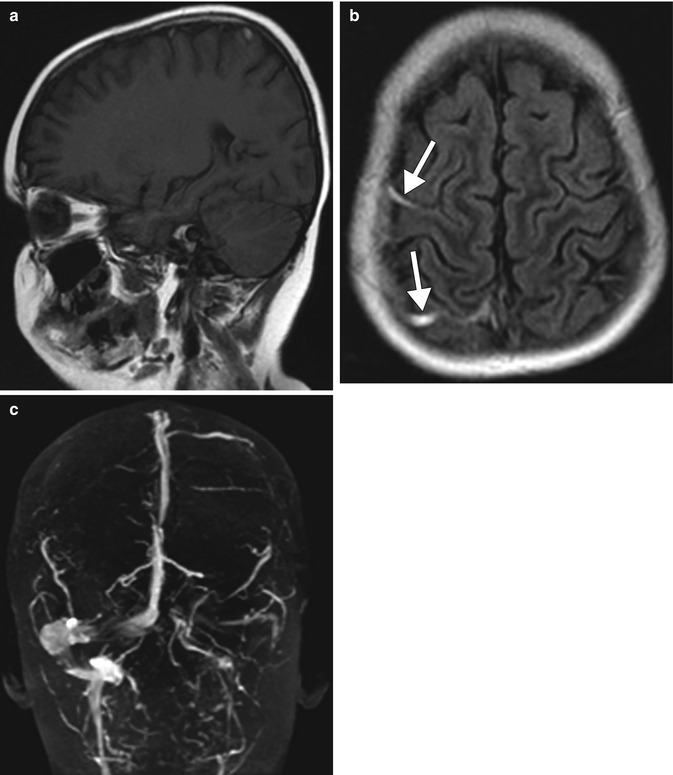
Fig. 21.2
Cortical vein trombosis associated with L-Asparaginase. A 6-year-old female with B-cell ALL presenting with right-sided weakness 1 month after L-Asp induction chemotherapy. Initial sagittal pre-contrast T1-weighted MRI (a) shows two foci of hyperintensity in cortical veins over the right cerebral convexity. Axial FLAIR image (b) shows hyperintensity in the same two cortical veins (arrows). MIP image from an MRV (c) shows absence of flow in corresponding right-sided cortical veins
The diagnostic test of choice is either CT or MR venography. Any filling defect should raise suspicion of CVT; however, this needs to be distinguished from normal intra-sinus septations, arachnoid granulations, and congenital hypoplastic/aplastic venous structures.
Treatment of L-Asp-associated thrombosis is anticoagulation and cessation of L-Asp. Long-term outcomes remain good, and L-Asp may be restarted after imaging shows thrombus stabilization or improvement.
21.4 Differential Diagnosis
A potential drug-induced etiology should be considered for every patient presenting with cerebral venous thrombosis. The most common drug associated with venous thrombosis is the oral contraceptive pill. Other drugs that have been reported to cause venous thrombosis include tamoxifen, androgens, cisplatin, thalidomide, and MDMA. Neuroimaging manifestations are similar to non-drug-induced venous thrombosis. Other conditions that predispose to venous thrombosis in children and young adults should also be considered, such as congenital or acquired prothrombotic conditions, dehydration, infection, anemia, renal disease, trauma, autoimmune disorders, congenital heart disease, central venous line placement, and malignancy.
Oral contraceptive pills (OCP) (refer to Chap. 47 ). In most developed countries, the most common risk factor for venous thrombosis is OCP use. The use of the estrogen-containing OCP is significantly associated with an increased risk of venous thrombosis, particularly in patients with hereditary prothrombotic states. OCPs containing drospirenone may be associated with higher risks of venous thrombosis than those with levonorgestrel.
Tamoxifen: A selective estrogen receptor modulator commonly used in the treatment of breast cancer. The potential mechanism for a procoagulant effect is unknown but may relate to its weak estrogenic effects.
Androgens: Androgen-induced venous thrombosis has been mainly reported in young body builders. The mechanism is unknown but may relate to increased platelet activation or an increase in coagulation factors.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








