6 Management of Complications Rehabilitation of Cranial Nerve Deficits Treatment of the Eye and Disorders of the Facial Nerve Management of Postoperative Cerebrospinal Fluid Leakages Cranial nerve deficits can have a substantial impact on the patient’s quality of life. Some patients with lower cranial nerve paralyses are dependent on gastrostomy tubes and tracheostomies. Also, dysfunction of the facial nerve usually provides a significant problem to the patient’s overall quality of life. Appropriate rehabilitation is therefore necessary and is directed either toward reestablishing proper functioning or toward providing compensatory mechanisms. • The neurotologic cranial nerve examination—see p. 49 • Facial nerve—see p. 216 • Neurofibromatosis type 2—see p. 195 • Surgical management of the facial nerve—see p. 320 Injury to cranial nerves I and II is generally not remediable. Injury to cranial nerves III, IV, and VI often recovers spontaneously and dysfunction is based on stretching and compression rather than invasion or resection. Oblation of cranial nerve III results in ptosis, mydriasis, and outward displacement of the eye with diplopia. The loss of extraocular muscle function is so severe after damage to cranial nerve III that eye muscle surgery is unable to correct the deficits. However, in selected cases where only partial limitation of function has occurred, selective eye muscle surgery may be of benefit. The ptosis associated with cranial nerve III deficit occurs secondary to paralysis of the levator palpebrae muscle and is usually sufficient to completely cover the cornea and prevent diplopia. Although surgical procedures can correct the ptosis, the mydriasis and ocular displacement are often more cosmetically disturbing than the ptosis. Moreover, the protective function of the eyelid will be lost and the patient will develop diplopia in all fields of gaze unless the eye is patched. Injury to cranial nerve IV (trochlear) most commonly occurs in the cavernous sinus. The fourth cranial nerve supplies the superior oblique muscle. Loss of function results in vertical displacement of the eye. Consequently, the patient will experience vertical diplopia and cyclotorsion (image tilting). Patients with complete impairment of the fourth cranial nerve may accommodate by head tilting, which eliminates the diplopia in primary gaze. Surgical selective weakening of the antagonist muscles of the ipsilateral or the opposite eye can remediate the deficit. One should wait a minimum of 6–12 months postoperatively before undertaking surgical correction. Primary repair of cranial nerve V can result in anesthesia in the distribution of the injured branch. Anesthesia is poorly tolerated but patients generally accommodate to it over a period of many months. Dysesthesia associated with injury to the fifth nerve can be exceedingly disabling. Initial medical management is similar to that of tic douloureux. Tegretol or other anticonvulsants are employed and may be increased to maximum allowable dosages. If medical therapy fails, surgical rhizotomy of the nerve proximal to the area of injury may be performed. Unfortunately, peripheral surgical procedures are not always of benefit. In such cases, the area of abnormal or neurologic function may lie within the central nervous system, probably in the thalamus. Injury to the motor division of cranial nerve V results in paralysis of the masticatory muscles and leads to shift of the mandible to the contralateral side. This can result in malocclusion and secondary traumatic temporomandibular joint arthritis. If the motor division is divided, early postoperative management is indicated. Intermaxillary fixation at the time of the primary procedure or shortly thereafter may help in preventing the shift of the mandible to the opposite side. Physical therapy to prevent limited mouth opening should be undertaken. Occlusal adjustments should be considered when needed. Injury to cranial nerve VI results in paralysis of the ipsilateral rectus muscle and inward displacement of the eye with diplopia in all fields of gaze (Fig. 6.1B). When permanent injury occurs, several methods of surgical repair are available, including the resection of the ipsilateral medial rectus or transposition of the inferior and superior rectus muscles to the affected lateral rectus muscle. If the sixth nerve has been traumatized but not divided, recovery of function is the rule. Recovery may occur within 12 months. During this time, the unopposed action of the ipsilateral rectus muscle may cause contraction of that muscle. Therefore, despite adequate recovery of function, medial displacement of the globe and diplopia may persist, necessitating extraocular muscle surgery. To prevent contraction of the ipsilateral medial rectus muscle, some ophthalmologists recommend weakening the ipsilateral medial rectus muscle with botulinum toxin injections. Fig. 6.1 A–C If division of the facial nerve (cranial nerve VII) is necessary, it should be repaired (p. 323). Primary anastomosis should be performed whenever possible, even if rerouting of the nerve is necessary. If it is not, an interposition graft should be placed. The anastomoses must be furnished in a tension-free fashion. If the facial nerve cannot be repaired, hypoglossal facial anastomosis (XII–VII) consistently yields the best results. Return of facial function should be expected in 3–4 months. Prevention of corneal ulcerations is the most urgent consideration in postoperative facial paralysis. Injury due to corneal exposure may lead to corneal ulceration, penetration of the globe, and eventual loss of vision in the affected eye. If the patient has a fifth-nerve deficit on the same side, the resulting anesthesia can considerably increase the risk of serious ocular injury. Moistening drops should be instilled regularly, as frequently as every 30–60 minutes. If moistening drops are inadequate and discomfort persists, ophthalmologic ointments are more efficient in preventing corneal drying, although they cause blurred vision in the affected eye. The use of an eye bubble or taping of the lid can help minimize dryness and help exposure of keratitis. If the above measures fail, and especially if there are coexisting fifth-nerve deficits, more aggressive intervention is necessary. More aggressive intervention includes the use of gold weights in the eyelids and lower-lid shortening procedures to remediate lower-lid ectropion. Several ophthalmologic procedures are available to repair lower-lid ectropion. Tarsorrhaphy is a last resort and is generally only needed in patients with coexisting fifth-nerve deficits. The glossopharyngeal nerve (cranial nerve IX) provides exclusive innervation to the stylopharyngeus muscle but also helps to provide tone to the palate and the eustachian tube, and sensory innervation of the posterior and lateral pharyngeal walls and carotid body. Isolated injury to the glossopharyngeal nerve results in little disability, but when it is combined with paralysis of cranial nerve X, aspiration may become a serious problem. This is often encountered during infratemporal fossa resections for jugular foramen lesions such as a temporal bone paraganglioma. With acute surgically induced paralysis, patients may become tracheostomy- and gastrostomy tube-dependent. There is no specific remediation for cranial nerve IX injury. Isolated injury to the vagus nerve results in ipsi-lateral vocal fold paralysis, as well as pharyngeal muscle incoordination. Management should begin in the preoperative period. Patients who have existing deficits and vocal cord paralysis should consider a preoperative vocal fold injection. If a previously normally functioning cranial nerve X is injured during surgery (especially if combined with cranial nerve IX), consideration should be given to a tracheotomy to protect the airway in the immediate postoperative period. A nasogastric tube should be placed for postoperative nutrition since the combination of vocal cord paralysis and pharyngeal muscle dys-function will make aspiration and severe dysphagia inevitable. Vagal nerve injury can lead to delayed gastric emptying and may limit the amount of postoperative nutrition that can be given by naso-gastric tube feedings; in these patients, therefore, gastrostomy or ileostomy may be preferred. The value of a cricopharyngeal myotomy in eliminating dysphagia remains controversial. Permanent vocal cord paralysis can be significantly improved by a vocal cord injection or formal thyroplasty. The spinal accessory nerve (cranial nerve XI) innervates the sternocleidomastoid and trapezius muscles. Loss of muscle function results in displacement of the humeral head anteriorly and inferiorly in the glenoid fossa. Traumatic arthritis of the shoulder may subsequently occur, resulting in severe chronic pain syndrome. The problem is reasonably well managed with vigorous postoperative physical therapy. Isolated unilateral hypoglossal nerve (cranial nerve XII) function is of little consequence to most patients. However, when combined with paralysis of cranial nerve VII and its associated loss of buccinator function and/or paralysis of cranial nerves IX and X, unilateral hypoglossal injury can significantly increase problems with deglutition (Fig. 6.1C). Bilateral hypoglossal nerve paralysis results in catastrophic difficulties in swallowing. They are often irremediable and require chronic enteral nutrition. Bilateral hypoglossal paralysis results in loss of ability to produce articulated speech. Most patients with bilateral deficits are limited to communicating by writing. Currie ZI, Shipman T, Burke JP. Surgical correction of large-angle exotropia in adults. Eye (Lond) 2003; 17(3):334–339 Ing E, Kennerdell JS. The evaluation and treatment of extraocular motility deficits. Otolaryngol Clin North Am 1997;30(5):877–892 Netterville JL, Vrabec JT. Unilateral palatal adhesion for paralysis after high vagal injury. Arch Otolaryngol Head Neck Surg 1994;120(2):218–221 Pou AM, Carrau RL, Eibling DE, Murry T. Laryngeal framework surgery for the management of aspiration in high vagal lesions. Am J Otolaryngol 1998; 19(1):1–7 Vestibular rehabilitation or balance rehabilitation is frequently used in neurotologic practice. It is often bundled with posturography and the overall goal is to decrease dizziness, improve balance, and minimize the risk of falls. • Vestibular neuronitis—see p. 179 • Platform posturography—see p. 81 • Other causes of balance disturbance—see p. 185 • Vestibular schwannoma—see p. 192 Vestibular rehabilitation depends on two important characteristics of the vestibular system: redundancy and plasticity. Redundancy occurs principally at the receptor level. The vestibular system, the visual system, and proprioceptive receptors in the lower extremity and cervical area all provide information to the central nervous system that helps control balance and equilibrium. Data received from all the available sensory receptors are initially processed in the brainstem, where decisions are made on a reflex basis (see Chapter 2, p. 39). The ability of sensory receptor information to be evaluated, emphasized, deemphasized, and/or changed at the brainstem level is the principle feature of the vestibular system, allowing for progressive modification or “plasticity.” • Interventions for BPPV. Practically speaking, these exercises are considered balance physical therapy but are discussed elsewhere (see p. 182). • Unilateral or bilateral vestibular dysfunction such as rehabilitation after vestibular neuritis or status post-vestibular schwannoma resection with incomplete central compensation. • Vestibular training for fluctuating vestibular dys-function with the goal of teaching the patient strategies to manage these spells. This is important in patients with Ménière disease (see p. 188) or individuals with migraine vestibulopathy. • Central vestibular dysfunction such as vertebrobasilar insufficiency or postconcussion balance disturbance. The goal is to prevent falls and to teach strategies to manage challenging situations and everyday life. The overall goal of the evaluation process is to quantify and qualify the balance system and to identify the patient’s balance strategies by specifically eliminating certain inputs (such as visual or somatosensory inputs). The use of a foam surface, for example, is an easy method to destabilize individuals (and therefore reduce the somatosensory input). Generally, evaluation of the gait and posture response on foam is quite difficult since several central mechanisms are used to compensate. However, the foam typically provides a tool with which to quantify balance function. A “dome” is a device that partially obscures the visual field; it is often combined with the foam surface (“foam and dome”). In this way, visual dependency can be evaluated. Similarly, Frenzel goggles can be used to remove visual clues. The standard in the evaluation process is platform posturography with its sensory organization test (Fig. 6.2A, B, see Chapter 3, p. 81). Computerized platform posturography can also be used to assess treatment progress. A good vestibular rehabilitation program should both extend and accelerate the normal process of physiologic adaptation to injury. Vestibular adaptation is the ability of the vestibular system to make long-term changes in the neural response. Vestibular adaptation can frequently be accomplished using simple exercises that are designed to progressively increase the gain of the vestibular system. Substitution is designed to enhance the use of visual proprioceptive information to improve balance. Desensitization (habituation) is based on the empiric observation that constant exposure to situations that produce dizziness, nausea, or imbalance will reduce or eliminate the unpleasant response. Desensitization is accomplished by giving the patient a variety of positional exercises designed to reproduce symptoms (Fig. 6.2C, D). The simplest habituation exercises are those first used by Cawthorne, but a variety of more sophisticated techniques are also used. It is important that the patient understand that the symptoms will initially worsen following provocation exercises before they improve.
Rehabilitation of Cranial Nerve Deficits
Definition
Closely Related Topics
Cranial Nerves I and II
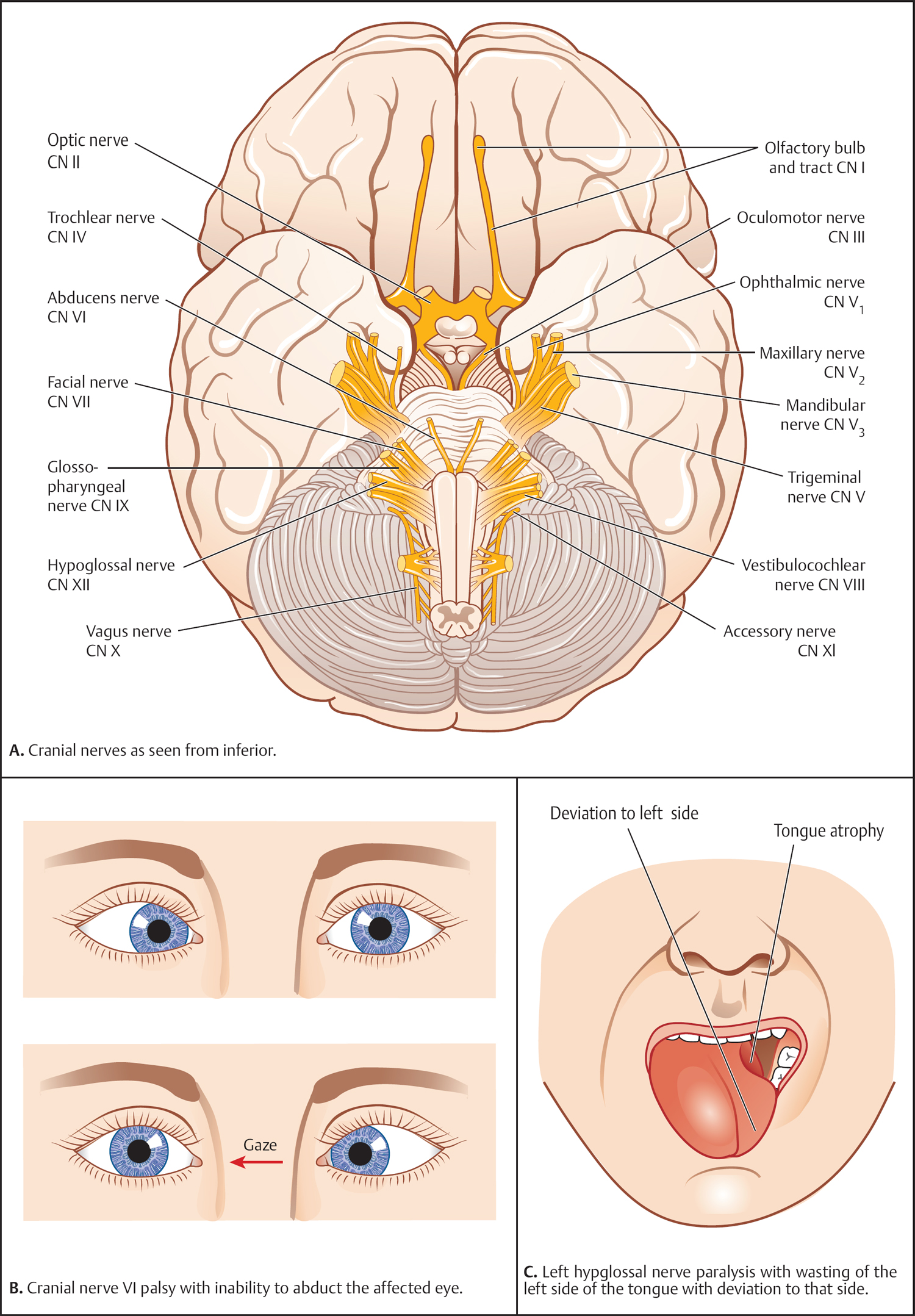
Cranial Nerves III, IV, and VI (Fig. 6.1A)
Cranial Nerve IV
Cranial Nerve V
Cranial Nerve VI (Fig. 6.1B)
Cranial Nerve VII
Cranial Nerve IX
Cranial Nerve X
Cranial Nerve XI
Cranial Nerve XII (Fig. 6.1C)
Recommended Reading
Vestibular Rehabilitation
Definition
Closely Related Topics
Introduction
Indications
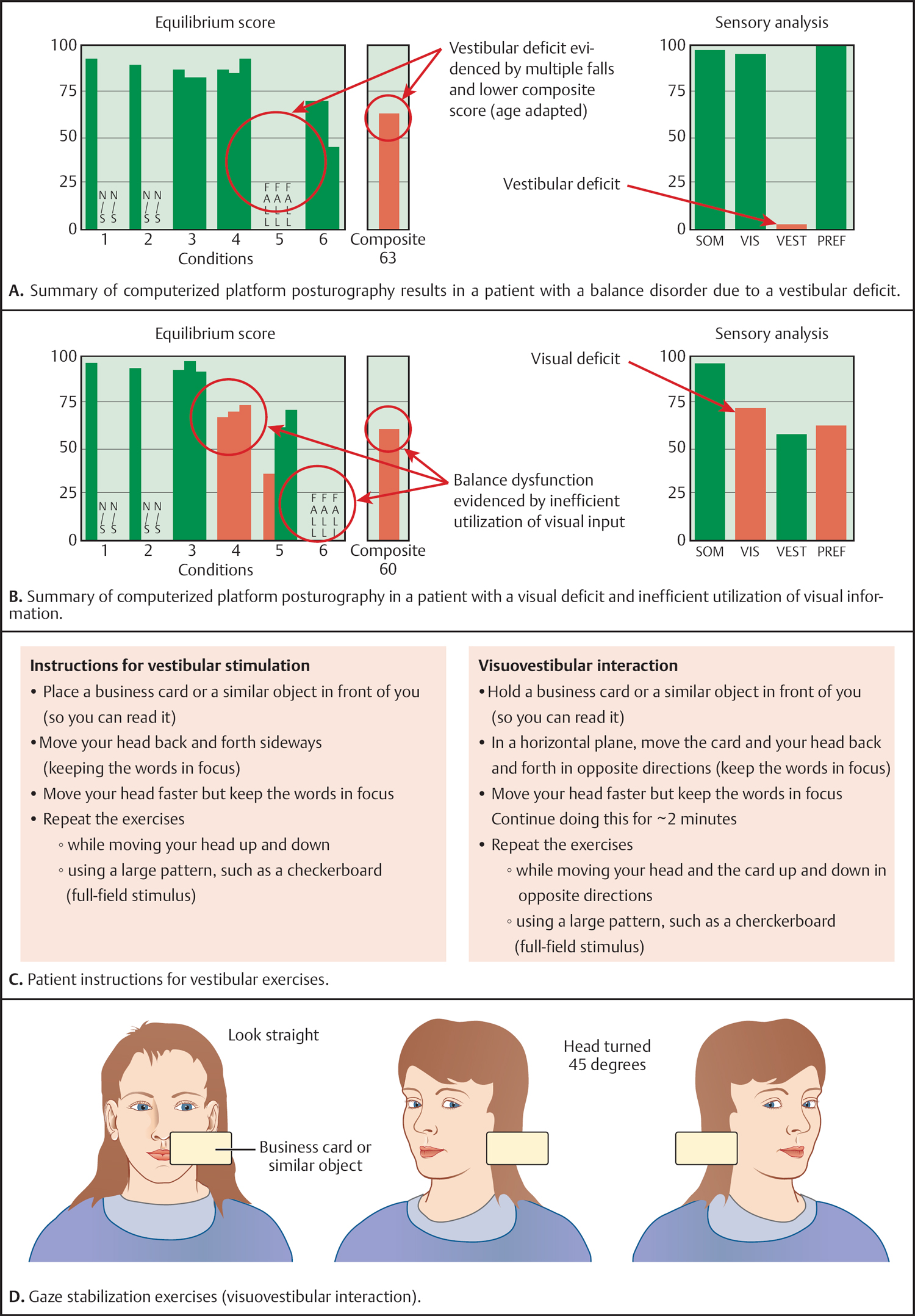
Pretreatment Evaluation (Fig. 6.2A, B)
Underlying Mechanisms and Treatments (Fig. 6.2C, D)
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


Management of Complications
Only gold members can continue reading. Log In or Register to continue






